Intraductal Injection of LPS as a Mouse Model of Mastitis: Signaling Visualized via an NF-κB Reporter Transgenic
Summary
Described here is a technique in which lipopolysaccharide is injected into the lactating mouse mammary gland via the nipple to simulate mastitis, a condition commonly caused by bacterial infection. Lipopolysaccharide injection results in increased nuclear factor kappa B (NF-κB) signaling, visualized through bioluminescent imaging of an NF-κB luciferase reporter mouse.
Abstract
Animal models of human disease are necessary in order to rigorously study stages of disease progression and associated mechanisms, and ultimately, as pre-clinical models to test interventions. In these methods, we describe a technique in which lipopolysaccharide (LPS) is injected into the lactating mouse mammary gland via the nipple, effectively modeling mastitis, or inflammation, of the gland. This simulated infection results in increased nuclear factor kappa B (NF-κB) signaling, as visualized through bioluminescent imaging of an NF-κB luciferase reporter mouse1.
Our ultimate goal in developing these methods was to study the inflammation associated with mastitis in the lactating gland, which often includes redness, swelling, and immune cell infiltration2,3. Therefore, we were keenly aware that incision or any type of wounding of the skin, the nipple, or the gland in order to introduce the LPS could not be utilized in our methods since the approach would likely confound the read-out of inflammation. We also desired a straight-forward method that did not require specially made hand-drawn pipettes or the use of micromanipulators to hold these specialized tools in place. Thus, we determined to use a commercially available insulin syringe and to inject the agent into the mammary duct of an intact nipple. This method was successful and allowed us to study the inflammation associated with LPS injection without any additional effects overlaid by the process of injection. In addition, this method also utilized an NF-κB luciferase reporter transgenic mouse and bioluminescent imaging technology to visually and quantitatively show increased NF-κB signaling within the LPS-injected gland4.
These methods are of interest to researchers of many disciplines who wish to model disease within the lactating mammary gland, as ultimately, the technique described here could be utilized for injection of a number of substances, and is not limited to only LPS.
Protocol
All animal experiments were approved by the Vanderbilt University Institutional Animal Care and Use Committee.
1. Preparing Transgenic Mice
- Female mice, positive for the NGL (NF-κB-GFP-Luciferase) reporter transgene (described previously1) are used for this procedure. When females are at least 6 weeks of age, mate them with an FVB wild type male. Harem breeding may be used (up to 4 females in a cage with 1 male). (Please note: FVB strain mice were used for the current study. Darker strain mice such as C57Bl6 may also be used, but these mice must be shaved prior to imaging).
- Starting at 15 days post-mating, check the females regularly for signs of pregnancy (large protruding girth). Each female must be separated once pregnant and the male removed from the breeding cage once the last female becomes pregnant.
- Watch the separated females and note the date of birth when a litter appears. A litter of at least 6 pups is required for adequate lactation. Eight days after the birth of the litter, proceed with the protocol (see Figure 1 for a timeline schematic).
2. Preparation for Injection
- Dissolve the E. coli LPS in PBS to a final concentration of 0.1 μg/μl. 50 μl of this solution, or a total of 5 μg, will be injected into the mammary gland. Prepare a second tube of PBS alone to be used for control injection.
- Set-up a dissecting scope and isoflurane anesthesia equipment. A nose-cone apparatus should be secured to the stage of the dissecting scope where the mouse will be placed. A good light source, whether from the scope itself or from extra spotlights should also be prepared.
- Once the set-up is complete, start the isoflurane machine and air flow.
3. Intraductal Injection of LPS
- Load the short needle syringe with 50 μl of the LPS solution. Set this aside.
- Anesthetize the mouse to be injected by first placing the female into an isoflurane filled box and then once breathing is slowed, move her onto the stage and place her nose within the nose-cone. Use a toe pinch to confirm the mouse is fully anesthetized. Monitor the mouse’s breathing throughout the procedure and adjust the isoflurane level accordingly. The cage containing the litter of pups that the female has been taken from should be carefully set aside until the dam can be returned after the procedure.
- Use a small drop of 70% ethanol to make the coat lay flat and to help visualize the nipple attached to the right #4 inguinal mammary gland on the mouse’s lower abdomen.
- Focus the dissecting scope for an optimal view of the nipple. Carefully use a set of fine forceps to further draw out the nipple away from the skin, but do not puncture or injure the nipple in any way. The forceps should never be tightly clamped together when manipulating the tissue, but used with a light hold which requires the minimal amount of stress on the nipple.
- Use the forceps in the left hand to gently hold the nipple in place. Slowly bring the preloaded syringe into the field of view using the right hand. The syringe should be held so that no repositioning has to occur in order to inject the contents.
- Once the syringe is in view, aim carefully at the small ductal opening within the center of the nipple, and insert the syringe.
- Without repositioning the hand, inject the contents of the syringe and remove the needle from the nipple.
- Load a second syringe with 50 μl of PBS for the control injection. Reposition the mouse on the stage and for the best view of the left #4 inguinal mammary gland nipple on the other side of the mouse’s lower abdomen. Repeat steps 3.4 to 3.7 using the PBS-loaded syringe.
- Once both injections are complete, discontinue anesthesia and move the mouse to a recovery cage. Monitor the female to insure that she becomes mobile within 5 min. Allow the mouse to remain in the recovery cage for 1 hr. After 1 hr of recovery, place the female back into the cage with her litter of pups. Mice should be periodically monitored for 6 hr post injection before proceeding to imaging. In our experience, no adverse consequences were noted in either the female or the pups during the period between injection and imaging. However, if signs of distress are observed in the female (e.g. hunched posture, biting or guarding of the injection site, general lethargy) or the pups (no movement, bluish color of skin) the experiment should be discontinued.
4. Bioluminescent Imaging to Visualize NF-κB Activity
- Once mice have been transported to the imaging facility, begin the imaging procedure by opening the software and initializing the machine. Turn on the isoflurane machine and air flow, ensuring that the anesthesia is flowing to both the box and the imaging chamber.
- Place the mouse under isoflurane anesthesia in the clear anesthesia box. Once breathing has slowed, use a toe pinch to confirm the mouse is fully anesthetized. Then, inject 100 μl of luciferin substrate into the mouse by retro-orbital injection5 using a sterile syringe.
- Immediately transfer the mouse to the imaging chamber and place her nose under the isoflurane nose-cone located there. The mouse should be supine. Secure each foot to the stage with tape.
- Input the appropriate settings to the IVIS software to take both a white light photographic image and an image of the bioluminescent activity. The exposure time should be 10 sec. Acquire the image.
- Once images have been acquired, allow the mouse to recover and then place her back in the cage with her pups and monitor periodically.
- The photographic and luminescent images are automatically overlaid and displayed on the screen, as in Figure 2. Analyze the acquired images by placing region of interest or “ROI” circles of equal size over each side of the mouse’s lower abdomen (one over the PBS-injected gland and one over the LPS-injected gland). Set the read-out to photons. A number should be displayed indicating the luminescence detected within each ROI (see Figure 2B). Use this number in statistical analysis.
- To display the optimum image, further adjust the threshold of signal displayed. This will not alter the total luminescence read-out but will allow you to remove background signal and visualize the differences between the control and LPS-treated gland. Decrease the amount of luminescence shown until the PBS-injected gland is free of background signal. This should leave the increased signal in the LPS-treated gland still apparent in the image, as seen in Figure 2.
- Additional analysis, including protein and RNA assays, can be completed with mammary tissue collected from the female post-mortem6.
5. Representative Results
To obtain interpretable results from these methods, LPS (or PBS) must be infused only into the mammary ducts, leaving the adjacent tissue undisturbed. Injection into the subcutaneous tissue surrounding the nipple will result in inflammation due to injury rather than the simulated infection. Injection of trypan blue dye diluted in PBS is helpful when learning the technique. Figure 3A shows a successfully injected gland infused with 100 μl of trypan blue in PBS. As shown, only the ductal tree should be filled with the injected solution, and there should be no bolus at the injection site. A “bolus” in this context is a build up of the injected liquid at the nipple or in the tissue surrounding the nipple without infusion into the ductal tree. This is shown in Figure 3B. Please note that the practice injections shown in Figure 3 were completed in a female at day 21 of lactation. During the height of lactation (day 8-10, the stage at which LPS is injected using the current protocol), milk is abundant and it is difficult to visualize the ducts and determine if the injection has been completed correctly. Therefore, later time points in lactation are better for practice injections.
Successful injection of LPS into the mammary ducts results in increased NF-κB activity within the gland. This should be evident in the reporter mouse upon IVIS imaging, and the LPS-injected gland should have substantially higher luciferase activity (measured by photon count) than the PBS-injected gland, as shown in Figure 2 (on average, the LPS gland reads 200% of the PBS control signal). A statistically significant increase in luminescence within the LPS-treated glands as compared to the contralateral control was achieved though the completion of a group of 4 mice 4. One additional study has also utilized intraductal mammary injection of either E. coli or LPS into NF-κB reporter transgenics. Similar to our own work, these authors saw a significant increase in reporter activity 6 hr after E. coli injection2.
Please note, due to constitutive NF-κB activity in the brain and other abdominal organs, the heads and abdomens of our reporter mice consistently show a signal when imaged, even at baseline prior to any manipulation. Thus, this signal should be ignored with regard to this experiment. An obvious signal should remain within the LPS-injected mammary gland after the image read-out is adjusted to minimize background luminescence in the PBS gland. Figure 2 shows images with the background reduced.
Unsuccessful injection of the gland will most likely result in damage to the nipple. This will cause pointed, skin-level inflammation that will be evident upon imaging. This type of wounding signal will be very strong and confined to the nipple area where the damage occurred, not emanating throughout the gland, as seen after a successful LPS injection into the ducts.
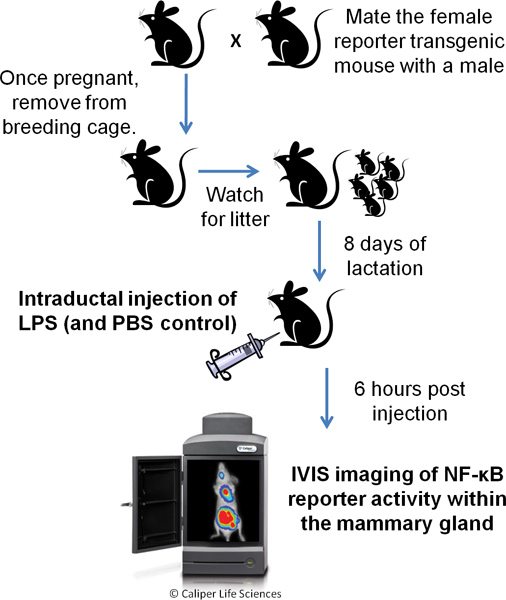
Figure 1. Schematic of Procedure.
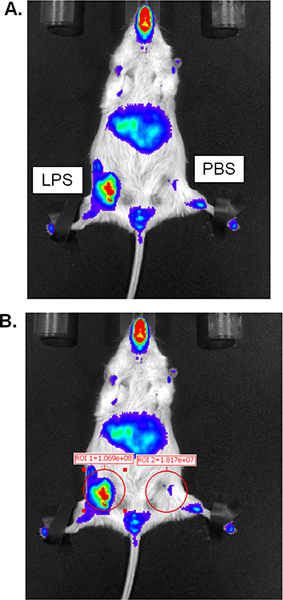
Figure 2. Representative results from IVIS bioluminescent imaging. (A) Acquired image with background reduced, revealing increased luciferase activity in the LPS-injected gland. (B) Image from A with region of interest quantifications added. Click here to view larger figure.
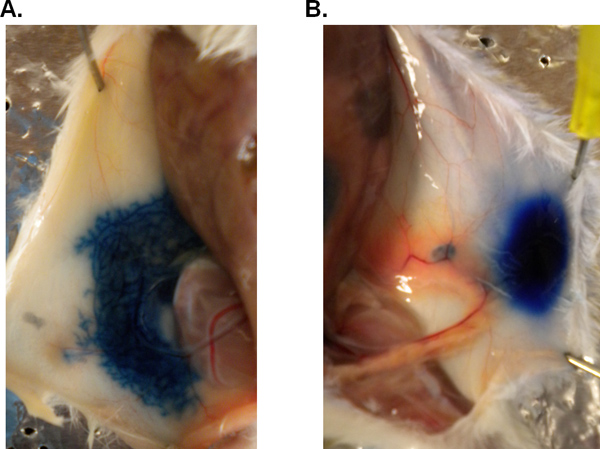
Figure 3. Practice injection: mammary gland injected with dye via intraductal injection. To test the accuracy of delivery via the nipple, a mouse at day 21 of lactation was injected with 100 μl of trypan blue dye diluted in PBS. Following sacrifice, the gland was exposed for visualization. (A) successful injection and (B) bolus of dye at the nipple.
Discussion
Here we utilize a transgenic NF-κB reporter mouse and an optimized injection technique to model mastitis, inflammation of the breast tissue most commonly caused by bacterial infection. The most critical step in this procedure is the intraductal injection itself.
In practice, it is usually apparent whether the intraductal injection has been successful. The injection of the agents (LPS or PBS) should feel fluid and there should be little to no resistance as the syringe is emptied. The most common pitfall is damage to the nipple leading to obstructed passage into the gland. This can be visualized by looking at the nipple through the dissecting scope. Damage can be avoided by sufficient practice, delicacy when manipulating the nipple, and by ensuring that only the smallest of needles (31G or higher) is used to perform the procedure. Additionally, if the needle is not positioned correctly, or if it slips mid-injection, a build-up of LPS or PBS can form at the injection site and the liquid will not pervade the ducts. If this happens, you may either visually see the accumulation of liquid in the skin around the nipple, or the injection will not feel fluid. Although this pitfall cannot totally be eliminated, occurrences can be avoided for the most part by practice and through the use of the proper tools.
The technique used here for injection was critical for this particular experiment. Some published methods for intraductal injection into the mammary gland require cutting/removal of the nipple and/or incision through the skin 7,8. In this case, as the primary end-point of the study was to determine NF-κB related inflammation within the gland, any incisions or perturbation of the skin or nipple were undesirable and would induce an inflammatory signal due to the tissue injury that would confound the LPS-induced signal.
Additionally, our injection was completed with a commercially available insulin syringe and without the use of a drawn micropipette or micromanipulators, as in several other methodologies for injection that do not utilize nipple removal 9, 10. We believe this was only feasible because the lactating nipple is slightly enlarged and somewhat easier to inject than a young, virgin mouse nipple. To inject virgin mice, more rigorous tools may be required.
It is clear from Figure 2 that if correctly performed, injection of LPS into the ducts of the mouse mammary gland causes localized inflammation as visualized by an increase in NF-κB luciferase reporter activity. Others have analyzed more extensively this model of acute mastitis, through either E. coli or LPS injection into the mammary gland and subsequent analysis of the tissue2-3, 8, 10-14. Among many findings, these studies illustrate that the inflammatory response is modulated by interactions with CD14, and that it results in a neutrophil influx regulated by mammary alveolar macrophages. As suggested in both our previously published work 4, as well as that of others 2 this model of mastitis may be further used to study mechanisms and therapeutics relevant in humans, where as many as 3-33% of breastfeeding women suffer from this painful infection (percentage varies based on study methodology) 15. It may also prove a useful research tool for those in the dairy industry, where mastitis is a costly disease leading to significant losses in milk production each year 16.
Finally, the NGL transgenic reporter mice used here and the similarly functioning HLL reporter mice 17 have been used in numerous studies to verify, quantify, and track the up or down regulation of NF-κB activity within a variety of disease and developmental models including acute lung injury, lung cancer, airway branching morphogenesis, insulin resistance, obesity, and myocardial infarction 1, 17-21. This model provides an additional example of the utility of these reporter transgenics.
Disclosures
The authors have nothing to disclose.
Acknowledgements
This work was funded by NIH grant CA113734 awarded to F Yull and the Department of Veterans Affairs (TS Blackwell).
Materials
| Name of the reagent | Company | Catalogue number | Comments |
| Lipopolysaccharide from Escherichia coli (LPS) |
Sigma | L 2880 | serotype 055:B5 |
| PBS | Mediatech, Inc. | 46-013-CM | |
| 31 Gauge insulin syringe | Becton Dickinson | 328438 | Short needle |
| Forceps | World Precision Instruments | 15908 | |
| Dissecting scope | Leica | M3Z | |
| Terrell Isoflurane, USP | MINRAD INC. for Rx Elite | NDC 66794-011-25 | |
| IVIS 200 imaging system | Caliper (formerly Xenogen) | N/A | |
| Syringe for luciferin injection | Becton Dickinson | 309597 | 1cc; 26G5/8 |
| D-Luciferin Firefly, sodium salt monohydrate (Luciferin substrate) |
Biosynth Chemistry and Biology | L-8240 | Dilute to 10 mg/ml |
References
- Everhart, M. B., Han, W., Sherrill, T. P., Arutiunov, M., Polosukhin, V. V., Burke, J. R., Sadikot, R. T., Christman, J. W., Yull, F. E., Blackwell, T. S. Duration and intensity of NF-κB activity determine the severity of endotoxin-induced acute lung injury. The Journal of Immunology. 176, 4995-5005 (2006).
- Notebaert, S., Carlsen, H., Janssen, D., Vandenabeele, P., Blomhoff, R., Meyer, E. In vivo imaging of NF-κB activity during Escherichia coli-induced mammary gland infection. Cellular Microbiology. 10, 1249-1258 (2008).
- Elazar, S., Gonen, E., Livneh-Kol, A., Rosenshine, I., Shpigel, N. Y. Neutrophil recruitment in endotoxin-induced murine mastitis is strictly dependent on mammary alveolar macrophages. Veterinary Research. 41, 10 (2010).
- Connelly, L., Barham, W., Pigg, R., Sait-Jean, L., Sherrill, T., Cheng, D. S., Chodosh, L. A., Blackwell, T. S., Yull, F. E. Activation of nuclear factor kappaB in mammary epithelium promotes milk loss during mammary development and infection. J. Cell. Physiol. 222, 73-81 (2010).
- Yardeni, T., Eckhaus, M., Morris, H. D., Huizing, M., Hoogstraten-Miller, S. Retro-orbital injections in mice. Lab Animal. 40, 155-160 (2011).
- Plante, I., Stewart, M. K., Laird, D. W. Evaluation of mammary gland development and function in mouse models. J. Vis. Exp. (21), e2828 (2011).
- Behbod, F., Kittrell, F. S., LaMarca, H., Edwards, D., Kerbawy, S., Heestand, J. C., Young, E., Mukhopadhyay, P., Yeh, H., Allred, D. C., Hu, M., Polyak, K., Rosen, J. M., Medina, D. An intraductal human-in-mouse transplantation model mimics the subtypes of ductal carcinoma in situ. Breast Cancer Research. 11, R66 (2009).
- Zheng, J., Watson, A. D., Kerr, D. E. Genome-wide expression analysis of lipopolysaccharide-induced mastitis in a mouse model. Infection and Immunity. 74, 1907-1915 (2006).
- Nguyen, D., Beeman, N., Lewis, M., Schaack, J., Neville, M. C., Ip, M. M., Asch, B. B. . Intraductal Injection into the Mouse Mammary Gland. Methods in Mammary Gland Biology and Breast Cancer Research. , 259-270 (2000).
- Lee, J. W., Paape, M. J., Zhao, X. Recombinant bovine soluble CD14 reduces severity of experimental Escherichia coli mastitis in mice. Veterinary Research. 34, 307-316 (2003).
- Elazar, S., Gonen, E., Livneh-Kol, A., Rosenshine, I., Shpigel, N. Y. Essential role of neutrophils but not mammary alveolar macrophages in a murine model of acute Escherichia coli mastitis. Veterinary Research. 41, 53 (2010).
- Bannerman, D. D., Paape, M. J., Hare, W. R., Sohn, E. J. Increased levels of LPS-binding protein in bovine blood and milk following bacterial lipopolysaccharide challenge. Journal of Dairy Science. 86, 3128-3137 (2003).
- Gonen, E., Vallon-Eberhard, A., Elazar, S., Harmelin, A., Brenner, O., Rosenshine, I., Jung, S., Shpigel, N. Y. Toll-like receptor 4 is needed to restrict the invasion of Escherichia coli P4 into mammary gland epithelial cells in a murine model of acute mastitis. Cellular Microbiology. 9, 2826-2838 (2007).
- Notebaert, S., Demon, D., Vanden Berghe, ., Vandenabeele, T., P, ., Meyer, E. Inflammatory mediators in Escherichia coli-induced mastitis in mice. Comparative Immunology, Microbiology, and Infectious Diseases. 31, 551-565 (2008).
- Osterman, K. L., Rahm, V. A. Lactation mastitis: bacterial cultivation of breast milk symptoms, treatment, and outcome. Journal of Human Lactation. 16, 297-302 (2000).
- Sordillo, L. M., Streicher, K. L. Mammary Gland Immunity and Mastitis Susceptibility. Journal of Mammary Gland Biology and Neoplasia. 7, 135-146 (2002).
- Blackwell, T. S., Yull, F. E., Chen, C. L., Venkatakrishnan, A., Blackwell, T. R., Hicks, D. J., Lancaster, L. H., Christman, J. W., Kerr, L. D. Use of genetically altered mice to investigate the role of nuclear factor-kappa B activation and cytokine gene expression in sepsis-induced ARDS. Chest. 116, 73S-74S (1999).
- Stathopoulos, G. T., Sherrill, T. P., Cheng, D. S., Scoggins, R. M., Han, W., Polosukhin, V. V., Connelly, L., Yull, F. E., Fingleton, B., Blackwell, T. S. Epithelial NF-kappaB activation promotes urethane-induced lung carcinogenesis. Proceedings of the National Academy of Sciences. 104, 18514-18519 (2007).
- Blackwell, T. S., Hipps, A. N., Yamamoto, Y., Han, W., Barham, W. J., Ostrowski, M. C., Yull, F. E., Prince, L. P. NF-κB signaling in fetal lung macrophages disrupts airway morphogenesis. The Journal of Immunology. 187, 2740-2747 (2011).
- Chiang, S. H., Bazuine, M., Lumeng, C. N., Geletka, L. M., Mowers, J., White, N. M., Ma, J. T., Zhou, J., Qi, N., Westscott, D. The protein kinase IKKepsilon regulates energy balance in obese mice. Cell. 138, 961-975 (2009).
- Singh, M. V., Kapoun, A., Higgins, L., Kutschke, W., Thurman, J. M., Zhang, R., Singh, M., Yang, J., Guan, X., Lowe, J. S. Ca2+/calmodulin-dependent kinase II triggers cell membrane injury by inducing complement factor B gene expression in the mouse heart. The Journal of Clinical Investigation. 119, 986-996 (2009).

