A Large Animal Model for Acute Kidney Injury by Temporary Bilateral Renal Artery Occlusion
Summary
This study presents a highly reproducible large animal model of renal ischemia-reperfusion injury in swine using temporary percutaneous bilateral balloon-catheter occlusion of the renal arteries for 60 min and reperfusion for 24 h.
Abstract
Acute kidney injury (AKI) is associated with higher risk for morbidity and mortality post-operatively. Ischemia-reperfusion injury (IRI) is the most common cause of AKI. To mimic this clinical scenario, this study presents a highly reproducible large animal model of renal IRI in swine using temporary percutaneous bilateral balloon-catheter occlusion of the renal arteries. The renal arteries are occluded for 60 min by introducing the balloon-catheters through the femoral and carotid artery and advancing them into the proximal portion of the arteries. Iodinated contrast is injected in the aorta to assess any opacification of the kidney vessels and confirm the success of the artery occlusion. This is furtherly confirmed by the flattening of the pulse waveform at the tip of the balloon catheters. The balloons are deflated and removed after 60 min of bilateral renal artery occlusion, and the animals are allowed to recover for 24 h. At the end of the study, plasma creatinine and blood urea nitrogen significantly increase, while eGFR and urine output significantly decrease. The need for iodinated contrast is minimal and does not affect renal function. Bilateral renal artery occlusion better mimics the clinical scenario of perioperative renal hypoperfusion, and the percutaneous approach minimizes the impact of the inflammatory response and the risk of infection seen with an open approach, such as a laparotomy. The ability to create and reproduce this clinically relevant swine model eases the clinical translation to humans.
Introduction
Acute kidney injury (AKI) is a commonly diagnosed condition among surgical patients associated with significant morbidity and mortality1,2. Available data show that AKI can affect even half of all hospitalized patients worldwide and leads to 50% mortality rate in patients in the intensive care unit1,3. Despite its high prevalence, current AKI therapy remains limited to preventive strategies, such as fluid management and dialysis. Therefore, there is an ongoing interest in exploring alternative therapies for AKI4,5,6.
AKI is typically classified into pre-renal, intrinsic, and post-renal based on its etiology4,5,6. The majority of surgical patients with AKI are associated with pre-renal causes due to hypovolemia, resulting in ischemia-reperfusion injury (IRI) of the kidneys2. Clinically, urine output decreases, and creatinine levels increase due to decreased renal function. The kidney is a high-metabolic-rate organ and susceptible to ischemia. A highly reproducible large animal model of renal IRI is necessary to obtain a better insight into the pathophysiology of AKI and its potential therapeutic approaches5.
To mimic the clinical scenario of kidney hypoperfusion peri-operatively, a model of bilateral renal artery occlusion is deemed suitable. Previously described models entailing unilateral renal artery occlusion with or without resection of the contralateral kidney do not provide sufficient clinical applicability7,8. Although these models are sufficient for causing AKI, they do not resemble real-life clinical scenarios neither in terms of type nor duration of injury.
The aim of this paper is to present a porcine model of percutaneous bilateral temporary occlusion of the renal arteries by balloon-catheter occlusion under angiography. Bilateral renal artery occlusion mimics the clinical scenario of renal hypoperfusion, followed by the subsequent removal of the balloon for reperfusion9,10. The technical steps are described, including catheterization, catheter guidance, angiography, and hemodynamic monitoring. This method not only allows for a highly controlled and replicable occlusion of the renal arteries, but the percutaneous approach minimizes the impact of the inflammatory response by limiting the amount of insult to the body compared to an open approach.
Protocol
All in vivo studies were conducted in accordance with the National Institutes of Health's guidelines on animal care and use and were approved by the Boston Children's Hospital's Animal Care and Use Committee (Protocol 18-06-3715). All animals received humane care in compliance with the Guide for the Care and Use of Laboratory Animals. Figure 1 shows the timeline including anesthesia, surgical preparation, and timepoints for primary outcome measurements of this study.
1. Induction, anesthesia and intubation
- To prevent unnecessary stress and discomfort, sedate the swine by intramuscular injection of a mixture of tiletamine/zolazepam 4-6 mg/kg and xylazine 1.1-2.2 mg/kg as well as isoflurane 3% using a face mask.
- Cannulate the ear vein to obtain venous access with a 20 G IV cannula after disinfecting the area with 95% ethanol. Start a maintenance infusion (0.9% NaCl at 5 mL/kg/h).
- Intubate the pig with an endotracheal tube (size 7 for pigs weighing 40-50 kg) once anesthetic adequacy is confirmed. Perform balloon-ventilation with a frequency of 12 breaths/min and transport the pig to the operating theater.
- Place the animal on the operating table in the supine position. Immediately start mechanical positive pressure ventilation with FiO2 0.50, 10 mL/kg tidal volume, and a frequency of 12 breaths/min under continuous capnography.
- Place a pulse oximeter on the ear or the bottom lip for continuous monitoring.
- Maintain normothermia (37 °C) using an air-heated pad.
- To maintain general anesthesia, keep isoflurane administration at 0.5-4% through the endotracheal tube. Throughout the procedure, continuously monitor ECG, arterial blood pressure, temperature, and capnography to measure the depth of anesthesia.
- Insert a Foley catheter to check the fluid status of the animal and monitor the urine output by collecting urine in a drainage bag.
NOTE: Female swine are preferred over males due to the anatomical features of their urethra which allows easier catheterization.
2. Surgical preparation and vascular access
- Drape the animal in a sterile fashion.
- Disinfect the right lateral area of the neck by applying betadine and then 95% ethanol for 3 times.
- Perform a cut-down for the catheterization of the right carotid artery and the right jugular vein. Retract the sternocleidomastoid muscle laterally and dissect it down to the right carotid artery and the right jugular vein.
- Insert a 5F angiography sheath in both the artery and the vein. Secure it with a silk 2-0 suture.
- Insert a 5F angiography sheath using the Seldinger technique into the left femoral artery.
- To perform the Seldinger technique puncture the femoral artery using a hollow needle. Insert a soft tip guidewire through the lumen and advance it into the femoral artery.
- Hold the guidewire secure with the hand while removing the needle. Pass the angiography sheath over the guidewire into the femoral artery and withdraw the guidewire. Use ultrasound guidance, if necessary.
3. Induction of renal ischemia-reperfusion injury
- Administer 200 IU/kg sodium heparin intravenously to achieve systemic anticoagulation (target activated clotting time (ACT) > 300 s).
- Perform an angiography by injecting an iodinated contrast agent under fluoroscopy to identify the renal arteries.
NOTE: To reduce the risk for contrast-induced nephrotoxicity, dilute the iodinated contrast agent in a 1:1 solution with normal saline. Tabulate the dosage for all animals to ensure equivalent dosing. - Identify the renal arteries, manually advance the guidewire in the guiding catheter.
- Position the 5F JL4 guiding catheter in the left renal artery through the right carotid artery (Figure 1A).
- Position the second 5F JL4 guiding catheter in the right renal artery through the left femoral artery (Figure 1A).
- Use the guidewires to direct a 5F percutaneous transluminal angioplasty (PTA) dilatation catheter in each renal artery.
NOTE: It is preferable to position the balloon at the proximal renal artery so that no branches or collaterals of the renal artery are left patent after balloon inflation. - Position each balloon catheter in place and connect a pressure line to each catheter.
- Check the presence of arterial pulse waveforms in the pressure monitor to ensure the correct positioning of the catheter.
- Inflate each balloon and aim for a pressure of approximately 2.5 atm inside the balloon (Figure 1B).
- To confirm the cessation of blood flow to the kidneys observe the flattening of the pulse waveform at the tip of the balloon catheter.
- Inject iodinated contrast medium (1:1 dilution) and check for any opacification of the renal vessels.
NOTE: It is also possible to fill the balloon with an iodinated contrast agent for visualization of the inflated balloon. However, this method is not as sensitive as pulse waveform flattening to confirm occlusion of the renal arteries. - After 60 min of occlusion, carefully deflate and remove the balloon catheters from the renal arteries.
- Perform an angiography (using 1:1 diluted contrast medium) to confirm renal artery patency and the establishment of renal reperfusion (Figure 1C).
- Remove the 5F angiography sheath from the left femoral artery.
- Apply firm pressure at the site of catheterization for 30 min.
- Reverse the effect of heparin by the administration of protamine (3 mg/kg) until ACT normalizes.
- To sample urine during the post-operative period, secure a tube to the Foley catheter with a silk 2-0 suture using an interrupted stitch on the skin.
- Leave the angiography sheaths in the right carotid artery and the right jugular vein in place and secure them with a silk 2-0 suture using an interrupted stitch to allow for blood sampling throughout the study.
- Close the neck incision with a silk 2-0 suture using a continuous stitch in 2 layers.
- Administer bupivacaine (3 mg/kg) at the incision site to minimize pain.
- Continue to hydrate the animal with 0.9% NaCl at 5 mL/kg/h for a total of 2 h following the end of ischemia.
- Place a fentanyl patch (25-50 µg/h) on the back of the animal to minimize post-operative pain.
- Administer an intramuscular injection of buprenorphine (0.005-0.1 mg/kg) to minimize post-operative pain.
- Monitor the animal and maintain it on mechanical ventilation until awaking.
4. Animal recovery
- Following awaking, accommodate the animal in a temperature-controlled room.
- Continue to turn the animal from one lateral side to the other until it regains full consciousness and ability to ambulate.
- Provide water and food ad libitum.
5. Functional assessment
- Collect the blood and the urine samples according to the desired protocol.
NOTE: In this study, the following time points were designated: baseline (1 h following initiation of the hydration protocol and before occlusion of the renal arteries), end of ischemia, and reperfusion (2 h, 6 h, 24 h). - Collect the arterial and the venous blood samples. Store them in lithium heparin or EDTA coated vacutainers for subsequent analysis.
NOTE: Draw blood directly from the catheters in the carotid artery and jugular vein. - Collect the urine samples from the Foley catheter and store them in 15 mL tubes for analysis.
NOTE: Collect the urine from the drainage bag connected to the Foley catheter. - To determine urine output, empty the drainage bag and collect urine for 1 h.
NOTE: For the 6 h timepoint at which a drainage bag is not connected to the Foley catheter, close the tube connected to the Foley catheter for 30 min and then collect the urine with a 60 mL syringe to determine urine output.
6. Euthanasia
- Following the end of the reperfusion period, perform anesthesia and monitor as described above.
- Continue hydration with 0.9% NaCl at 5 mL/kg/h.
- Use the arterial and the venous catheters for blood sampling and the Foley catheter to determine urine output. Collect the final blood and urine samples and calculate the urine output.
- Perform a 15-cm midline laparotomy incision using a size 10 blade from the xiphoid down to the mid pelvis.
- Use a straight lateral retractor to retract the abdominal skin.
- Dissect the lateral peritoneal attachments of the abdominal wall to expose the right and left retroperitoneum.
- Identify and bluntly dissect both renal arteries and veins.
- Ligate both renal arteries and veins with a 2-0 silk suture and perform bilateral nephrectomies to collect whole tissue specimens for histological and metabolic analysis.
- Euthanize the animal with the preferred method of euthanasia (e.g., exsanguination, pentobarbital)
Representative Results
Functional analysis
The representative results of this study arise from 6 animals and the data shown are mean ± standard error of the mean.Renal function is assessed by determining the urine output, estimated glomerular filtration rate (eGFR), plasma creatine, and blood urea nitrogen (BUN). The biomarkers of renal function are assessed using a portable chemistry analyzer. eGFR is calculated according to the following formula: eGFR =1.879 × BW1.092/PCr0.6 (BW: body weight in kg; PCr: plasma creatinine in mg/dL)10,11.
Following 60 min of bilateral renal artery occlusion, urine output was significantly decreased from 3.6 mL/kg/h ± 0.5 mL/kg/h to 0.2 mL/kg/h ± 0.1 mL/kg/h (p < 0.01). This decrease remained significant at 6 h (1.2 mL/kg/h ± 0.1 mL/kg/h; p = 0.02 vs. baseline) and 24 h (1.3 mL/kg/h ± 0.4 mL/kg/h; p = 0.02 vs. baseline) following reperfusion. Similarly, a significant decrease was observed in eGFR, which dropped from 2.5 mL/kg/h ± 0.1 mL/kg/h at baseline to 1.7 mL/kg/h ± 0.1 mL/kg/h (p < 0.001) at the end of ischemia and to 1.5 mL/kg/h ± 0.1 mL/kg/h (p < 0.001), 1.2 mL/kg/h ± 0.1 mL/kg/h (p < 0.001) and 0.9 mL/kg/h ± 0.1 mL/kg/h (p < 0.001) at 2 h, 6 h and 24 h reperfusion, respectively (Figure 2A-B).
Plasma creatinine was significantly increased at 2 h (2.7 mg/dL ± 0.2 mg/dL; p < 0.01), 6 h (3.7 mg/dL ± 0.3 mg/dL; p < 0.001) and 24 h (5.6 mg/dL ± 0.7 mg/dL; p < 0.001) of reperfusion compared to baseline (1.1 mg/dL ± 0.1 mg/dL). BUN was 6.5 mg/dL ± 0.8 mg/dL at baseline and increased to 17.8 mg/dL ± 3.3 mg/dL (p < 0.001) and 36.2 mg/dL ± 2.9 mg/dL (p < 0.001) at 6 h and 24 h of reperfusion, respectively (Figure 2C-D).
Gross anatomy and histology
There were evident necrotic and hemorrhagic areas which were unevenly distributed in both kidneys at the end of the 60 min of bilateral renal ischemia and the 24 h of reperfusion (Figure 3A). Masson's Trichrome staining revealed confluent coagulative necrosis which was located at the proximal tubules of the renal cortex. (Figure 3B). Plastic embedded sections (1 µm) were also assessed since they provide significant details of the histology (Figure 3C). All Masson's Trichrome slides were evaluated for cell necrosis, loss of brush border, cast formation, and tubule dilatation. Then, a semi-quantitative scoring system for acute tubular necrosis (ATN) was implemented as follows: 0 if none; 1 if less than 10%; 2 if between 11%-25%; 3 if between 26%- 45%; 4 if between 46%-75%; and 5 if greater than 76%. ATN scoring showed significant injury in the renal cortex (score of 4.5 ± 0.3) and considerable injury in the medulla (score of 2.7 ± 0.4).
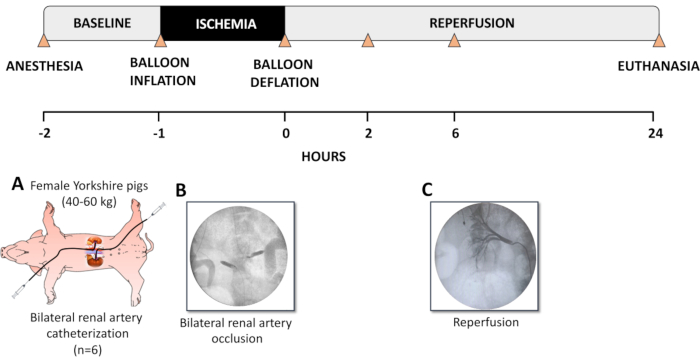
Figure 1. Description of the experimental model. (A) Female Yorkshire pigs (40-60 kg) were sedated and intubated. The left femoral artery and the right carotid artery were catheterized with a 5F angiography sheath. Right jugular venous lines and a Foley urinary catheter were also placed. Selective catheterization of the renal arteries was performed using a 5F multipurpose guide-catheter. (B) Occlusion of the renal arteries was performed using a 5F percutaneous transluminal angioplasty (PTA) dilatation catheter inflated in the proximal portion of the renal artery, totally occluding the blood flow to the kidneys for 60 min. Confirmation of the occlusion was acquired by injection of iodinated contrast medium in the aorta and by checking for any opacification of the vessels of the kidneys. (C) Following 60 min of occlusion, the balloons were deflated and carefully removed. Angiography was performed to confirm renal artery patency and the establishment of renal reperfusion. The animals were then allowed to reperfuse the kidneys under physiological conditions for the next 24 h and were subsequently euthanized. Blood and urine samples were collected right before and after bilateral renal ischemia, at 2, 6, and 24 h after occlusion (timepoints indicated with triangles). This figure has been modified from Doulamis et al11. Please click here to view a larger version of this figure.
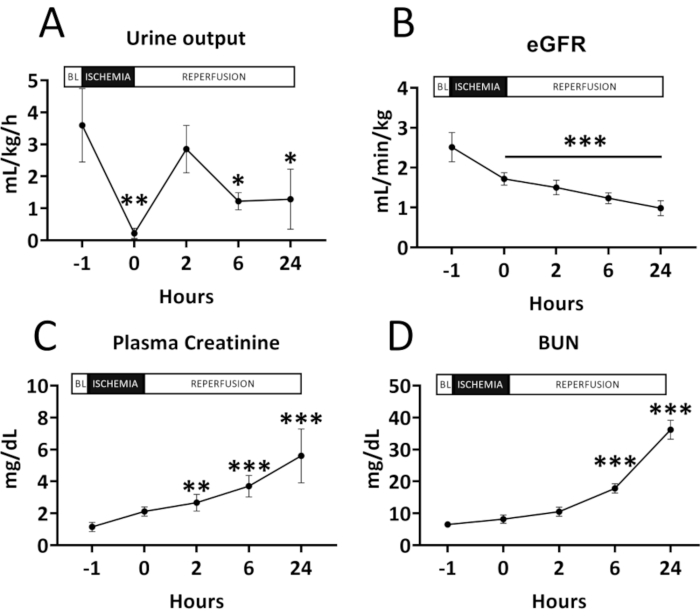
Figure 2. Renal function before and after renal ischemia-reperfusion injury. (A) Urine output; (B) Estimated glomerular filtration rate (eGFR); (C) Plasma creatinine and (D) Blood urea nitrogen (BUN). All results are shown as mean and standard deviation for each timepoint. A significant decrease can be seen in the urine output and the eGFR following ischemia-reperfusion injury. Accordingly, a significant increase is noted in plasma creatinine and BUN. Data were analyzed by two-way repeated measures ANOVA with the Benjamini and Hochberg's false discovery rate (n=6). *p < 0.05 vs Baseline; **p < 0.01 vs Baseline; ***p < 0.001 vs Baseline. Please click here to view a larger version of this figure.
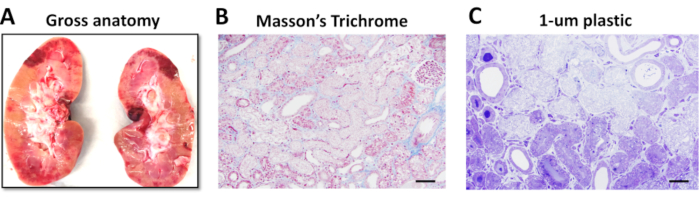
Figure 3. Gross kidney anatomy and renal tissue injury at 24 hours of reperfusion following renal ischemia-reperfusion injury. (A) Gross anatomy of the left kidney showing pale areas indicative of infarction and red hemorrhagic areas following 60 min of bilateral renal artery occlusion and 24 h of reperfusion. (B) Renal Cortex of vehicle shows extensive coagulative necrosis of primarily proximal tubules, following 60 min of ischemia and 24 h of reperfusion (Masson's Trichrome, original magnification 20x). (C) These 1 µm plastic (araldite-epon) embedded sections demonstrate in greater detail the confluent tubular necrosis consisting primarily of matrix with swelling and degenerative changes of organelles (Toluidine blue, original magnification 40x). Scale bar = 200 µm. This figure has been modified from Doulamis et al11. Please click here to view a larger version of this figure.
Discussion
AKI is a common clinical disorder affecting up to 50% of hospitalized adult patients worldwide6,12. A clinically relevant animal model is needed to further investigate the pathophysiology of the disease and potential therapeutic targets. Although there are several murine models replicating AKI, these do not completely mimic their respective clinical scenarios and the anatomy of the human kidney. This study proposes a clinically relevant swine model to allow for translation to humans13.
Here, the protocol describes a percutaneous approach which is not only clinically relevant but also minimizes the inflammatory response and the risk for infection that accompanies an open approach. It should also be highlighted that a consistent hydration protocol should be used for all animals in order to achieve optimal hemodynamic control and avoid renal hypoperfusion11. This can be easily done when the animal is anesthetized but cannot always be accurately performed during the recovery period when water is provided ad libitum.
Iodinated contrast medium should be used cautiously in order to avoid contrast-induced nephrotoxicity. This can be achieved by 1:1 or 1:2 dilution with normal saline. In this study, we used a dose which is 10 times lower than the estimated safety threshold for humans (3.33 mL/kg)9,14.
Among others, the study uses eGFR for the assessment of renal function based on a formula accounting for the body weight and plasma creatinine levels10,11. It should be noted that although the use of inulin for the determination of GFR has been previously documented, its use was deferred in the current protocol due to severe hypotensive vasospastic reaction after inulin infusion. This can be avoided by using steroids or epinephrine prior to inulin administration. However, the use of these drugs may not be appropriate according to each study design. For this reason, a validated formula to estimate the eGFR based on plasma creatinine and body weight was used11.An alternative way for determining GFR would be using the formula: (urine creatinine x urine flow rate) / (plasma creatinine x kidney weight).
For the assessment of the ATN score, the use of Masson’s Trichrome staining is preferable to conventional hematoxylin and eosin staining as it can better trace tissue injury. Another alternative may be the use of plastic embedded sections, which provide greater details as they allow for thinner slicing of the sample11. This preclinical model of AKI can be used to mimic several clinical scenarios such as kidney transplantation, renal hypoperfusion following cardiogenic shock (e.g., myocardial infarction, aneurysm rupture, aortic dissection), transcatheter procedures at high risk of renal ischemia and cardiovascular procedures with prolonged cardiocirculatory arrest times.
This study has some limitations. The study used only female animals. This was done to reduce any possible effects related to urinary catheterization, which is less traumatic in females than males. In addition to this limitation, the study used young, otherwise healthy animals, thus eliminating confounding variables that may be related to coexisting diseases. In conclusion, the current study describes a highly reproducible large animal model of renal IRI, which can be used to decrease the burden of AKI.
Offenlegungen
The authors have nothing to disclose.
Acknowledgements
We would like to thank Dr. Arthur Nedder for his help and guidance. This work was supported by the Richard A. and Susan F. Smith President's Innovation Award, Michael B. Klein and Family, The Sidman Family Foundation, The Michael B. Rukin Charitable Foundation, The Kenneth C. Griffin Charitable Research Fund, and The Boston Investment Council.
Materials
| 0.9% sodium chloride injection, usp, 100 ml viaflex plastic container | Baxter | 2B1302 | For animal hydration |
| Agent contrast 100.0ml injection media btl ioversal 74% | CARDINAL HEALTH | 133311 | For visualizing the vasculature |
| Bard Bardia Closed System Urinary Drainage Bag | BARD Inc | 802001 | For urine collection |
| BD Vacutainer K2 EDTA | BD | 367841 | For blood sample storage |
| BD Vacutainer Lithium Heparin | BD | 366667 | For blood sample storage |
| Betadine | Henry Schein | 6906950 | For skin disinfection |
| Bookwalker retractor | Codman | For skin retraction | |
| Bupivacaine 0.25% | Hospira | Administer at incision site for analgesia | |
| Buprenorphine SR | Zoo Pharm | 10mg/ml bottle, Dose: 0.2mg/kg SC | |
| Cath angio 5.0 Fr x100.0 cm 0.038 in JR4 | MERIT MEDICAL SYSTEM INC | 7523-21 | For identification of the renal arteries |
| Cuffed endotracheal tube | Emdamed | To establish a secure airway for the duration of the operation | |
| EKG Medtronics- Physiocontrol LifePak 20 Oxygen saturation monitor | GE Healthcare Madison WI | For oxygen saturation monitoring | |
| Encore 26 inflator | BOSTON SCIENTIFIC | 710113 | For inflating the balloon catheters |
| Ethanol 95% (Ethyl alcohol) | Henry Schein | For skin disinfection | |
| Fentanyl patch | Mylan | Dose: 25-50mcg/hr, TD | |
| Gold silicone coated Foley | TELEFLEX MEDICAL INC | 180730160 | For urine collection |
| Heparin sodium | LEO Pharma A/S | Dose: 200 IU/kg IV | |
| i33 ultrasound machine | Phillips | Use ultrasonographic guidance for femoral catherization if necessary | |
| Inqwire diagnostic guide wire – 0.035" (0.89 mm) – 260 cm (102") – 1.5 mm j-tip | MERIT MEDICAL SYSTEM INC | 6609-33 | For guiding the balloon catheters to the renal arteries |
| Intravenous catheter, size 20 gauge | Santa Cruz Biotechnology | Inc SC-360097 | For fluid administration |
| Isoflurane | Patterson Veterinary Supply, Inc. | 21283620 | Dose: 3%, INH |
| Metzenbaum blunt curved 14.5 cm – 5(3/4)" | Rudolf Medical | RU-1311-14M | For tissue dissection and cutting |
| Neonatal disposable transducer kit with 30ml/hr flush device and double 4-way stopcocks for continuous monitoring | Argon Medical | 041588505A | For pressure measurement |
| Powerflex pro PTA dilatation catheter 6 x 20 mm – shaft length (135cm) | CARDINAL HEALTH | 4400602X | For occlusion of the renal arteries |
| Pressure monitoring lines mll/mll – 12" clear, mll/mll | Smiths Medical | B1571/MX571 | For pressure measurement |
| Procedure pack | Molnlycke Health Care | 97027809 | Surgical drape, gauze pads, syringes, beaker etc |
| Protamine | Henry Schein | 1044148 | For heparin reversal |
| Scalpel blade – size #10 | Cardinal Health (Allegiance) | 32295-010 | For the skin incisions |
| Stopcock iv 4 way lrg bore rotg male ll adptr strl | Peoplesoft | 1550 | For connecting tubings |
| Straight lateral retractor | Codman | For skin retraction | |
| Suture perma hnd 18in 2-0 braid silk blk | CARDINAL HEALTH 1 | A185H | For suturing incision site and securing catheters |
| Syringe contrast injection 10ml fixed male luer red | MERIT MEDICAL SYSTEM INC | MSS111-R | To administer the contrast agent |
| Syringe medical 60ml ll plst strl ltx free disp | CARDINAL HEALTH 1 | BF309653 | For urine collection and flushing of the angiocath |
| Tilzolan (tiletamine/zolazepam) | Patterson Veterinary Supply, Inc. | 07-893-1467 | Dose: 4-6 mg/kg, IM |
| Xylazine | Putney, INC | Dose: 1.1-2.2 mg/kg, IM |
Referenzen
- Ali Pour, P., Kenney, M. C., Kheradvar, A. Bioenergetics consequences of mitochondrial transplantation in cardiomyocytes. Journal of the American Heart Association. 9 (7), 014501 (2020).
- Giraud, S., Favreau, F., Chatauret, N., Thuillier, R., Maiga, S., Hauet, T. Contribution of large pig for renal ischemia-reperfusion and transplantation studies: The Preclinical Model. Journal of Biomedicine and Biotechnology. 2011, 14 (2011).
- Amdisen, C., et al. Testing Danegaptide effects on kidney function after ischemia/reperfusion injury in a new porcine two week model. PLoS ONE. 11 (10), 1-13 (2016).
- Bhargava, P., Schnellmann, R. G. Mitochondrial energetics in the kidney. Nature Reviews Nephrology. 13 (10), 629-646 (2017).
- Bonventre, J. V., Weinberg, J. M. Recent advances in the pathophysiology of ischemic acute renal failure. Journal of the American Society of Nephrology. 14 (8), 2199-2210 (2003).
- Case, J., Khan, S., Khalid, R., Khan, A. Epidemiology of Acute Kidney Injury in the Intensive Care Unit. Critical Care Research and Practice. 2013, 9 (2013).
- Jabbari, H., et al. Mitochondrial transplantation ameliorates ischemia/reperfusion-induced kidney injury in rat. Biochimica et Biophysica Acta (BBA) – Molecular Basis of Disease. 1866 (8), 165809 (2020).
- Malagrino, P. A., et al. Catheter-based induction of renal ischemia/reperfusion in swine: Description of an experimental model. Physiological Reports. 2 (9), 1-13 (2014).
- Freeman, R. V., et al. Nephropathy requiring dialysis after percutaneous coronary intervention and the critical role of an adjusted contrast dose. American Journal of Cardiology. 90 (10), 1068-1073 (2002).
- Gasthuys, E., et al. Postnatal maturation of the glomerular filtration rate in conventional growing piglets as potential juvenile animal model for preclinical pharmaceutical research. Frontiers in Pharmacology. 8 (431), 1-7 (2017).
- Doulamis, I. P., et al. Mitochondrial transplantation by intra-arterial injection for acute kidney injury. American Journal of Physiology – Renal Physiology. 319 (3), 403-413 (2020).
- Rewa, O., Bagshaw, S. M. Acute kidney injury-epidemiology, outcomes and economics. Nature Reviews Nephrology. 10 (4), 193-207 (2014).
- Grossini, E., et al. Levosimendan Protection against Kidney Ischemia/Reperfusion Injuries in Anesthetized Pigs. Journal of Pharmacology and Experimental Therapeutics. 342 (2), 376-388 (2012).
- Laskey, W. K., et al. Volume-to-creatinine clearance ratio. A pharmacokinetically based risk factor for prediction of early creatinine increase after percutaneous coronary intervention. Journal of the American College of Cardiology. 50 (7), 584-590 (2007).

