Using a Bacterial Pathogen to Probe for Cellular and Organismic-level Host Responses
Summary
We describe both in vitro and in vivo infection assays that can be used to analyze the activities of host-encoding factors.
Abstract
There are a variety of strategies bacterial pathogens employ to survive and proliferate once inside the eukaryotic cell. The so-called ‘cytosolic’ pathogens (Listeria monocytogenes, Shigella flexneri, Burkholderia pseudomallei, Francisella tularensis, and Rickettsia spp.) gain access to the infected cell cytosol by physically and enzymatically degrading the primary vacuolar membrane. Once in the cytosol, these pathogens both proliferate as well as generate sufficient mechanical forces to penetrate the plasma membrane of the host cell in order to infect new cells. Here, we show how this terminal step of the cellular infection cycle of L. monocytogenes (Lm) can be quantified by both colony-forming unit assays and flow cytometry and give examples of how both pathogen- and host-encoded factors impact this process. We also show a close correspondence of Lm infection dynamics of cultured cells infected in vitro and those of hepatic cells derived from mice infected in vivo. These function-based assays are relatively simple and can be readily scaled up for discovery-based high-throughput screens for modulators of eukaryotic cell function.
Introduction
Infection-based experimental models are inherently challenging due to their dependence on the starting state conditions of the host and pathogen, the various pathogen infection strategies, and the difficulty of attributing pathogen- and host-driven processes based on outcomes. The bacterium Listeria monocytogenes (Lm) has become an ideal pathogen to probe host defense responses because of its genetic and microbiological tractability, its rapid and processive cellular infection strategy, and the relatively clear relationship between its cellular- and organismic-level infection phenotypes. The cellular infection of Lm proceeds through four distinct phases1: (i) cellular invasion that concludes with Lm being enclosed within a vacuole; (ii) Lm-directed dissolution of the vacuole membrane and release of Lm into the cytosol; (iii) intracytosolic replication; and (iv) physical penetration of the plasma membrane that results in either the infection of directly adjacent cells (such as in an epithelial sheet) or, in solitary cells, release of Lm into the extracellular milieu. Each of these phases are promoted by specific Lm-encoded factors (referred to as 'virulence factors') that, when deleted, cause infection defects in both cellular and animal models. This general infection strategy has been independently evolved by a number of the so-called 'cytosolic' pathogens2.
Colony-forming unit (CFU) assays are widely employed to evaluate both in vitro (i.e., cellular) as well as in vivo (i.e., organismic) infection outcomes. In addition to their high sensitivity, particularly for in vivo infections, CFU assays provide an unambiguous readout for pathogen invasion and intracellular survival/proliferation. CFU assays have been extensively used to analyze both Lm and host cell determinants that impact infection. As informative as these prior studies have been to analyze cellular invasion and intracytosolic replication, CFU assays have not, to the best of our knowledge, been used to track the fourth phase of the Lm infection process: cellular escape. Here, we describe relatively simple means of how cellular escape (hereafter referred to as 'emergence') can be monitored by CFU assay (as well as by flow cytometry) and show examples of how both pathogen- and host-encoded factors regulate this phase of the Lm infection cycle. The analysis of the terminal phase of the cellular Lm infection cycle may make it possible to identify additional pathogen and host cell infection-specific factors and activities.
Protocol
Mice were treated humanely in accordance with all appropriate government guidelines for the Care and Use of Laboratory Animals of the National Institutes of Health and their use was approved for this entire study by the University of Miami Institutional Animal Care and Use Committee (protocol 16-053).
1. Preparing Cells for Infection
- Propagate mouse macrophage-like cell line RAW 264.7 in DMEM tissue culture media supplemented with 10% fetal calf serum (henceforth referred to as DMEM/FCS) using a 125 mL flask and a tissue culture incubator maintained at 37 °C/5% CO2.
- The day before the infection, use a cell scraper to remove cells from the expansion flask and collect in a 15 mL screw cap conical tube. Centrifuge cells at 800 x g for 10 min, decant supernatant and suspend the cell pellet in 1 mL of DMEM/FCS (without antibiotics) and determine the titer using a hemocytometer or an automated cell counter.
- Adjust titer to 2 x 106 cells/mL and add 0.10 mL (2 x 105 cells) to wells of a 48-well tissue culture dish. Ensure that the cell suspension covers the entire surface of the well.
- Plate cells in additional wells for a later source of conditioned media. Also place 0.10 mL of DMEM/FCS in three additional wells to serve as a 'no cell control'.
- Incubate overnight in a tissue culture incubator at 37 °C/5% CO2. The next day, do not remove from incubator until the bacterium inoculum is prepared and ready to use.
2. Preparing Listeria monocytogenes (Lm) for infection
- Inoculate 2 mL of brain-heart infusion (BHI) with a single colony from a freshly-streaked agar plate (<2 days) of Lm and incubate overnight at 37 °C with shaking at 130 rotations/min.
- The next day, add 0.10 mL of overnight culture to 2 mL pre-warmed BHI and continue incubating at 37 °C with shaking until the optical density (OD600) is between 0.4 and 0.6.
- Determine approximate bacterial titer using an empirically-derived conversion formula. In our lab, an exponentially growing Lm culture in BHI is approximately 1.3 x 109 colony forming units (CFU)/OD600. Minimize the amount of time bacterial cultures are exposed to room temperature.
- Just prior to infection adjust the titer to 5 x 107 CFU/mL using pre-warmed DMEM/FCS as diluent.
3. Infection
- Working quickly and precisely, add 20 µL (1 x 106 CFU; multiplicity of infection, MOI = 5) of the freshly-prepared Lm inoculum (step 2.4 above) to wells by slightly tilting the dish and carefully placing the pipet tip in the overlying media;
NOTE: avoid touching the walls of the well with the pipet tip. - Gently pipet the contents of each well to ensure complete mixing; do not shake or significantly tilt the plate as this will spread Lm over the walls of the well. Return cell culture dish to 37 °C/5% CO2 incubator.
- Prepare a 10 µg/mL gentamicin solution using conditioned media from uninfected wells as diluent.
- At 30 minutes post infection (mpi), carefully add 30 µL of the gentamicin solution (final concentration 2.5 µg/mL) and gently pipet the contents of the well as before and return cell culture dish to 37 °C/5% CO2 incubator.
- At 60 mpi, harvest appropriate wells for either CFU assay (60 mpi time point) or FCM analysis (as described below in sections 4 and 5, respectively).
- For remaining wells, at various times thereafter either harvest cells as before or, for the Lm emergence assay, entirely remove media from well and replace with 150 µL of gentamicin-free conditioned media.
4. Sampling Processing and Analysis of Intracellular and Emergent Lm by CFU Assay
- To harvest, slightly tilt the dish and carefully remove the entire media from the well. Add 0.50 mL of distilled sterile water (dsH2O) to the well. After 30 s, transfer the resulting water lysate (100) to a 1.5 mL microcentrifuge tube and vortex vigorously for 10 s.
- Prepare 10-1 and 10-2 dilutions by adding either 4.5 µL or 50 µL of the water lysate to 450 µL of dsH2O and briefly vortex to ensure thorough mixing.
- Spread 50 µL of the 100, 10-1 and/or 10-2 samples onto lysogeny broth (LB) agar plates.
- To assay for emergent Lm (step 3.6 above), remove 10 µL of the overlaying media and divide it into two 5 µL aliquots: to one aliquot add 5 µL of DMEM/FCS and to the second aliquot add 5 µL of DMEM/FCS containing 5 µg/mL gentamicin. The latter control distinguishes between extracellular Lm (gentamicin sensitive) and intracellular Lm (gentamicin resistant) in the subsequent CFU assay.
- After 5 min at room temperature, add 90 µL of dsH2O, vortex vigorously for 10 s, and spread 50 µL on LB agar plates.
- Enumerate Lm colonies on LB agar plates following 2 days of incubation at 37 °C.
5. Sampling Processing and Analysis of Intracellular and Emergent Lm by Flow Cytometry (FCM)
- Prepare RAW 264.7 cells as described in steps 1.1-4. Adjust cells to 1 x 106 cells/mL and add 1 mL (1 x 106 cells) to wells of a 6-well tissue culture dish.
- Prepare bacterium inoculum as described in step 2.1-2.3 and infect cells with volume of inoculum corresponding to a MOI of 50 (5 x 107 CFU).
- At 1.5 hours post infection (hpi), collect media from first set of wells and place in a 1.5 mL microcentrifuge tube with 500 µL of 4% paraformaldehyde (PFA) and place on ice until all wells have been processed.
- To collect intracellular Lm, add 1 mL of dsH2O to the well and after 60 s, transfer the resulting water lysate to a 1.5 mL microcentrifuge tube with 500 µL of 4% PFA. Vortex vigorously for 10 s and place on ice until all wells have been processed. (Sample processing is described in step 5.8 below.)
- For remaining wells, remove media and replace with 1 mL of DMEM/FCS with 5 µg/mL gentamicin to kill extracellular Lm and promptly return cells to incubator.
- After 30 min (2 hpi) remove media and replace with DMEM/FCS without gentamicin.
- After 2 and 4 h (4 and 6 hpi) take second and third time points by collecting media and lysates as steps 5.3 and 5.4.
- Centrifuge tubes at 10,000 x g for 7 min. Remove supernatant without disturbing pellet.
- Suspend each pellet in staining cocktail of 50 µL of 4% PFA and 15 µL of phalloidin. Incubate tubes in the dark at 4 °C for 20 min.
- After incubation add 1 mL of FACS buffer to each tube and pipette up and down to mix.
- Spin tubes at 10,000 x g for 7 min. Remove supernatant without disturbing pellet.
- Suspend each pellet in 400 µL of FACS buffer for immediate use, or 200 µL of FACS buffer and 200 µL of 4% PFA if storing for later analysis.
- Run samples on a flow cytometry and analyze the collected data.
6. Sampling Processing and Analysis of Lm Colonization and Host Responses in the Liver
- Prepare Lm for infection as described in step 2.1-2.3.
- Calculate the necessary amount of subculture for desired titer of 3 x 106 CFU/mL.
- Just prior to infection dilute the amount of calculated bacteria with pre-warmed Hank's Balanced Salt Solution (HBSS) in a final volume of 1 mL. This is the input inoculum that is injected into the mouse.
- Using a 28 G½ 100U insulin syringe, draw 100 µL (3 x 105 CFU) of input inoculum and remove any visible air bubbles.
- Place the mouse (strain C57BL/6; males between 6 and 12 weeks old) into the holding restraint and use warm water (no more than 45 °C) to dilate the tail vein, then inject the input inoculum into the vein.
- Plate 10-2 and 10-3 dilutions of the input inoculum onto LB agar 10bcm plates and incubate overnight at 37 °C to determine the actual input dosage.
- At 18 hpi, humanely euthanize mouse (CO2 asphyxiation followed by cervical dislocation) and using sterile scissors cut open mouse peritoneum to collect frontal lobe of the liver using separate pairs of tweezers and scissors for the outside and inside of the mouse. Place the liver in a 6 cm Petri dish on ice.
- Cut the liver into small cubes and place into a glass vial with a magnetic stir bar. Add 2 mL of 2 mg/mL collagenase D reconstituted in DMEM without FCS. Incubate vials at 37 °C on a magnetic stirrer for 30−45 min. Once the tissue is homogenized, add 3 mL of DMEM/FCS to inactivate the collagenase.
- Filter the cells through a 70 µm cell strainer into a conical tube, adding more DMEM/FCS if necessary.
- Centrifuge cells at 800 x g to pellet at 4 °C for 10 min, remove supernatant and suspend cell pellet in 500 µL of ACK buffer to lyse red blood cells.
- Incubate cells at room temperature for 5 min in ACK buffer. Suspend cells in 1 mL of DMEM/FCS.
- Centrifuge cells at 800 x g to pellet at 4 °C for 10 min, remove supernatant and suspend in 1 mL of DMEM/FCS. Then, count the cells using a hemocytometer or an automated cell counter.
- Transfer 1 x 106 cells to 1.5 mL microcentrifuge tube and spin to pellet. Then suspend in 1 mL of dsH2O and vortex to lyse the cells. Plate 50 µL on LB plates at undiluted and 10-2 dilutions and incubate at 37 °C to enumerate Lm for CFU analysis.
- Transfer 1 x 106 cells into FACS tubes for each tissue sample according to the cell counts and wash with 1 mL of FACS buffer.
- Centrifuge cells at 800 x g to pellet at 4 °C for 10 min and remove supernatant.
- Prepare an antibody cocktail containing the antibodies of interest based on the recommended concentration for each antibody and FACS buffer. See Table of Materials for recommended amounts used in the analysis.
- Suspend pellet in 100 µL of antibody cocktail and incubate tubes in the dark at 4 °C for 30 min.
- After incubation, add 2 mL of FACS buffer to each tube and suspend cells.
- Centrifuge cells at 800 x g to pellet at 4 °C and discard the supernatant. Then suspend the pellet in 400 µL of FACS buffer for immediate use, or 200 µL of FACS buffer and 200 µL of 4% PFA if storing for later.
- Analyze cells by flow cytometry (see step 5.13).
Representative Results
Assessing the role of pathogen and host-encoded factors impacting cellular infection
Using the infection conditions described above, 0.15% of the input wild-type Lm is recovered after 1.5 h of co-incubation with cultured macrophages (Figure 1A). In the subsequent 1.5 h of co-incubation (3 h post infection, hpi), there was a 4-fold increase in recovery of viable Lm and from 3 to 6 hpi there was an additional 7.5-fold increase in the recovery of viable Lm. Since the cell-impermeable antibiotic gentamicin is added to the co-cultures at 1 hpi to eliminate extracellular Lm, the 30-fold increase in viable Lm levels between 1.5 and 6 hpi exclusively represents intracellular proliferation.
Lm rapidly gains access to the cytosol following its internalization within eukaryotic cells (see Introduction). Cytosolic Lm associates with the actin polymerization machinery by which means it propels itself capable of penetrating the plasma membrane. In the in vitro infection assay described above, if gentamicin is removed from the wells at 6 hpi, extracellular Lm can be readily detected 1 h later (7 hpi) in the overlying media (Figure 1B). No CFUs were recovered from control wells that were not seeded with macrophages but that were otherwise treated identically as seeded wells thereby showing that the appearance of extracellular Lm was entirely dependent on the presence of macrophages and not a result of incomplete antibiotic killing (not shown).
The capability of Lm to survive and proliferate intracellularly is largely dependent on a suite of genes whose expression are controlled by the transcription factor Positive Regulatory Factor A (PrfA)1. Initially, there is a comparable recovery of the wild-type Lm strain and a Lm mutant strain deleted for this factor (ΔprfA) (Figure 1A). However, there is a subsequent reduction in the recovery of the ΔprfA strain after prolonged co-incubation such that the recovery at 6 hpi is 3-fold less than the recovery at 1.5 hpi. Relatedly and expectedly, ΔprfA bacteria were not detected in the overlying media at 7 hpi (Figure 1B).
The activity of PrfA is regulated at multiple levels. A number of constitutively active PrfA variants, encoded by hyper-virulent prfA* alleles, have been isolated3. A Lm strain possessing a prfA* has an initial infection profile that is comparable to the isogenic wild-type strain at 1.5 and 3 hpi (Figure 1A). However, between 3 and 6 hpi, the fold-increase of the prfA* strain significantly differed from that of the wild-type strain. Again, relatedly and expectedly, the prfA* strain was readily detected in the overlying media at 7 hpi at levels that significantly exceeded that observed for the wild-type Lm strain (Figure 1B).
Following its release into the cytosol, Lm associates with the cellular actin polymerization machinery that results in the bacterium being enveloped by polymerized actin. To confirm that extracellular Lm is derived from the actin-rich cytosol of the infected host cell, macrophages were either left uninfected or infected with a GFP-expressing prfA* strain and the overlying media was collected at 1.5, 4, and 6 hpi, stained with phalloidin that binds polymerized actin, and analyzed by flow cytometry. Media overlaying both uninfected and infected macrophages contained light-scattering bacterium-sized particulate matter (Figure 2A), however, only media from infected macrophages possessed GFP-positive signals within this size gating (Figure 2B; left panel). There was a time-dependent increase in the appearance of phalloidin-positive Lm in the media overlaying infected macrophages (Figure 2B; right three panels). Phalloidin-positive GFP-expressing Lm were also detected in lysates prepared from infected macrophages (Figure 2C; left panel). However, no phalloidin-positive Lm was detected in lysates prepared from macrophages infected with a GFP-expressing Lm mutant strain that lacked the virulence factor ActA that is required to recruit the actin-polymerization machinery to the outer surface of Lm following its release into the cytosol (Figure 2C; right panel). These data support a scenario that in an in vitro infection model 'emergent' extracellular Lm are derived from the infected cell cytosol.
In addition to Lm-encoding factors, a number of host factors have been identified that impact Lm cellular infection (see Discussion). Recently, the host factor Perforin-2 (P2) has been shown to be a critical component of cell-level defenses against a number of bacterial pathogens. Peritoneal exudate macrophages (PEMs) isolated from wild-type (P2+/+) and P2-/- mice are initially comparably infected by Lm as measured by CFU assay at 1 hpi (Figure 3A). In P2+/+ PEMs the number of CFUs recovered at 6 hpi is 10-fold greater compared to the levels recovered at 1 hpi. Similar to previously published findings, in P2-/- PEMs the number of CFUs recovered at 6 hpi is 80-fold greater compared to the levels recovered at 1 hpi4. Enhanced Lm intracellular proliferation in P2-/- PEMs was accompanied with greater levels of viable Lm detected in the overlying media compared to levels detected in P2+/+ PEMs (Figure 3B). These data show that in an in vitro assay that the appearance of emergent extracellular Lm can also report on host factors that impact infection.
In vivo infection and analysis of the liver
In addition to the in vitro infection assays described above, the relative infectivity of the wild-type, attenuated, and hyper-virulent Lm strains can also be assessed by in vivo infection assays. Mice were intravenously co-infected with an equal mixture of the wild-type and ΔprfALm strains and 18 h later were humanely euthanized, livers excised, and single cell preparations were made. Isolated liver cells were lysed and the resulting lysates subjected to a CFU assay that could distinguish between the wild-type and ΔprfALm strains. Compared to the 1:1 ratio of these two strains in the original inoculum (the 'input'), the ΔprfA/wild type ratio at 18 hpi (the 'output') was considerably less than unity (for 6 mice range was 0.001 to 0.330; mean 0.100) (Figure 4). In contrast, mice co-infected with an equal mixture of the wild-type and prfA*Lm strains the prfA*/wild type ratios ranged from 2.4 to 10.2 (mean 7.1). This experiment shows that the relative infectivity of these three Lm strains (wild type, ΔprfA, and prfA*) in an intact organism resembles that observed in in vitro infection assays.
The host can also be monitored to determine whether the varying level of infectivity of the wild-type, ΔprfA, and prfA* strains are associated with a corresponding gradation of the innate immune response. Previously it has been shown that resident macrophages (Küpffer cells) and infiltrating inflammatory monocytes and neutrophils play critical and interrelated roles in protecting the liver during Lm infection5,6,7,8. Cells prepared from uninfected mice and mice infected with the GFP-expressing wild-type Lm strain for 18 h were stained with cell type-specific markers and analyzed by flow cytometry. In terms of non-immune cells of the liver (e.g., hepatocytes and endothelial cells), there were no detectable differences between uninfected and infected mice. In contrast, there were notable infection-related changes in the liver in terms of the proportion of immune cells that positively stained for the leukocyte common antigen CD45 (Figure 5A). Specifically, mice infected with the wild-type and prfA*Lm strains had significantly higher levels of CD45+ cells in the liver compared to uninfected mice whereas the levels of CD45+ liver cells in mice infected with the attenuated ΔprfALm strain were not notably different than levels observed in uninfected mice. To further characterize both resident and infiltrating immune cell populations, CD45+ cells can be furthered subtyped. As observed by others9, a notable shift with infection is the almost complete disappearance of resident Küpffer Cells (CD11bmid F4/80+) in the liver and the concomitant appearance of a distinct population of CD11bhi cells that represent infiltrating neutrophils (Figure 5B; lower middle panel). Also appearing in the liver at 18 hpi, are CD11bmid F4/80– cells appear that, since they also are Ly6Chi, represent infiltrating inflammatory monocytes (Figure 5B; lower middle and right panels). In infected mice these latter cells are the only cells in which appreciable GFP signal was detected following 18 hs of infection (Figure 5C). This latter finding is similar to that recently reported by Jones and D'Orazio who showed that in mice, Lm primarily is associated with Ly6Chi monocytes that infiltrate the gut following food-borne infection10. The profile of liver CD45hi cells of mice infected with the Lm ΔprfA strain resembled that of uninfected mice whereas mice infected with the hyper-virulent LmprfA* strain had modestly enhanced levels of infiltrating neutrophils and inflammatory monocytes compared to mice infected with the wild-type Lm strain (data not shown).
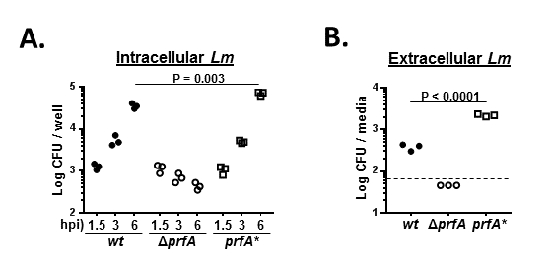
Figure 1: Infection of cultured macrophages by Listeria monocytogenes (Lm). The mouse macrophage cell line RAW 264.7 were infected in vitro with either wild-type Lm (wt; filled circles), attenuated Lm (ΔprfA; open circles), or hyper-virulent (prfA*; open squares) Lm strains (see text for details). (A) At 1.5, 3, and 6 hours post infection (hpi), macrophages were lysed and the cellular contents were analyzed by colony-forming unit (CFU) assay. (B) Infected macrophages were briefly treated with the antibiotic gentamicin to eliminate non-internalized Lm and at 6 hpi the overlaying media was collected and analyzed by CFU assay. Dotted line represents the detection limit of the assay. Each data point represents an independent well/infection and P values were determined by Student's t test. Shown are the results of a single representative experiment performed three times with similar outcomes. Please click here to view a larger version of this figure.
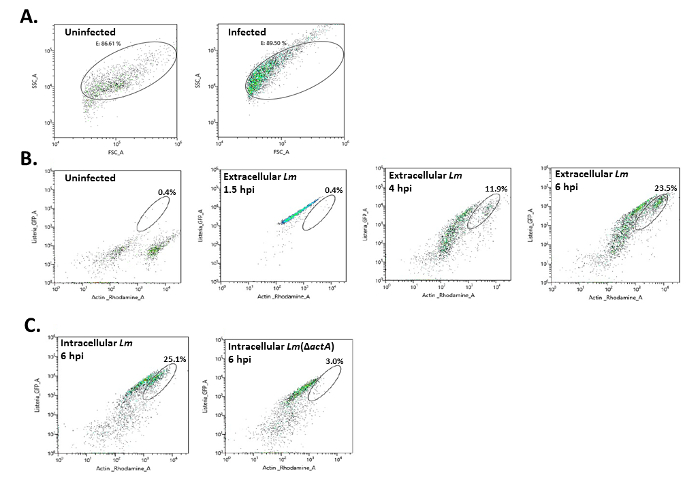
Figure 2: Actin-bound Lm analyzed by flow cytometry. The mouse macrophage cell line RAW 264.7 were either left uninfected or infected in vitro with GFP-expressing Lm. The overlying media was removed, centrifuged, and the collected material stained with actin-binding phalloidin. The stained material was analyzed by flow cytometry and shown is the light-scattering plots (A) indicating the gating used for the GFP- and phalloidin-associated levels of extracellular (i.e., media-derived) Lm shown in (B). (B) The indicated area represents the GFP/actin double positive Lm and their abundance as a percentage of the total events within the light-scattering gates. (C) Mouse macrophages were infected with either GFP-expressing Lm or a GFP-expressing Lm strain lacking the gene encoding ActA (ΔactA) that recruits the actin-polymerization machinery of the host cell to the Lm cell surface. At 6 hpi, infected cells were lysed and the released cellular contents, including the intracellular Lm, were stained for actin and analyzed by flow cytometry. Shown are the results of a single representative experiment performed three times with similar outcomes. Please click here to view a larger version of this figure.
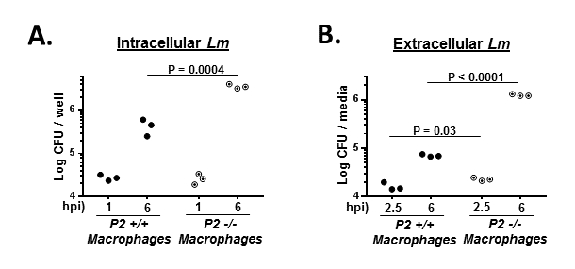
Figure 3: Infection of wild-type and Perforin-2 knockout macrophages by Lm. Peritoneal macrophages isolated from either a wild-type (P2+/+; filled circles) or knockout (P2-/-; dotted circles) were infected in vitro with Lm. (A) At 1 and 6 hpi, macrophages were lysed and the cellular contents analyzed by CFU assay. (B) Infected peritoneal macrophages were briefly treated with the antibiotic gentamicin and at 2.5 and 6 hpi the overlaying media was collected and analyzed by CFU assay. Each data point represents an independent well/infection and P values were determined by Student's t test. Shown are the results of a single representative experiment performed three times with similar outcomes. Please click here to view a larger version of this figure.
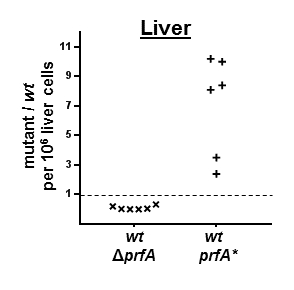
Figure 4: Lm infection of the mouse. Groups of 6 mice were infected with an equal mixture of either the wild-type Lm (wt) and attenuated Lm (ΔprfA) strains or an equal mixture of the wild-type Lm and hyper-virulent (prfA*) strains. At 18 hpi mice the Lm burden in the liver was determined by CFU assay. In this experiment the wild-type Lm strain possesses an antibiotic-resistance gene that allows it to be distinguished from the antibiotic-sensitive Lm mutant strains. Liver homogenates were plated on both antibiotic-containing and antibiotic-free media and the ratio of mutant and wild-type Lm were plotted. The dotted line represents the mutant/wild-type ratio of the infecting dose. The absolute levels of the wild-type Lm in the two cohorts of mice were 12 and 15 CFU/106 liver cells, respectively. Shown are the results of a single representative experiment performed two times with similar outcomes. Please click here to view a larger version of this figure.
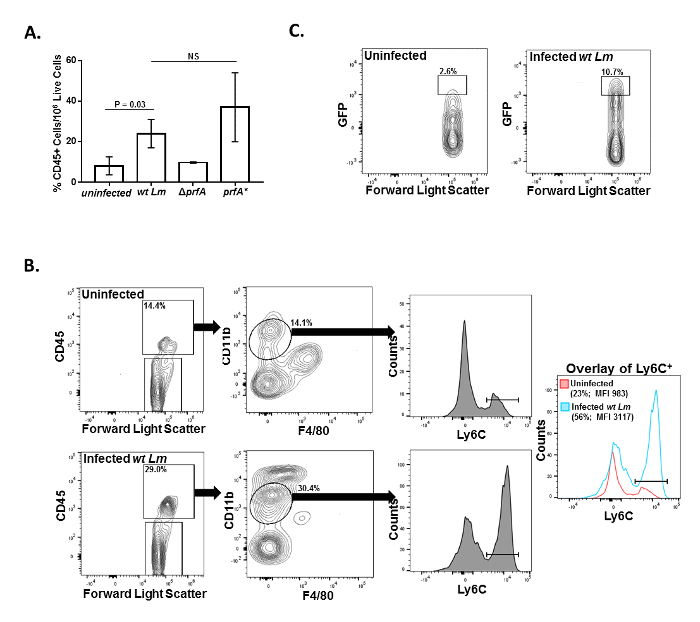
Figure 5: Immunological response to Lm infection in the mouse liver. Mice were either uninfected or systemically infected with 2 x 105 CFU of GFP-expressing Lm strains for 18 h. Single-cell preparations of livers were analyzed by flow cytometry for expression of immune- and myeloid-specific markers. (A) The percentage of cells staining positive for the immune-specific cell surface marker CD45+ per 106 isolated total live liver cells shown for uninfected mice and mice infected with either the wild-type (wt Lm), attenuated (ΔprfA), or hyper-virulent (prfA*) Lm strains. Plotted is the mean of three mice per group and P values were determined by Student's t test. (B) Shown in the left panels are the staining profile of CD45-staining liver cells from an individual uninfected mouse (top) and an individual wt Lm– infected (bottom); in the middle panels is shown the expression levels of myeloid-specific markers CD11b and F4/80 of the CD45+ cells; and on the right panels is shown the Ly6C expression levels of the indicated gated cells. In the far right panel is shown an overlay of the Ly6C+ cells from the uninfected and infected mice including the percentage and mean fluorescence intensities (MFI) of the CD11b+ F4/80– cells positive for the indicated Ly6C gate. Shown is a representative mouse from 3 mice per group. (C) Ly6C+ cells derived from livers of uninfected and infected mice (described (B); middle and right panels) were analyzed for GFP expression by flow cytometry. Please click here to view a larger version of this figure.
Discussion
Due to its rapid and processive cellular infection program, Lm is an ideal pathogen to probe cellular activities that impact infection. A number of host factors have been identified that either positively or negatively affect Lm cellular infection11,12,13,14. Two such host factors characterized in our laboratory, Perforin-2 and the Heme Regulated Inhibitor (P2 and hI), regulate distinct features of the Lm infection process. As shown in Figure 3, P2 deficient cells are highly susceptible to Lm and this enhanced susceptibility also is true of the P2 knockout mice4. Detailed comparative studies of P2-expressing and P2-deficient macrophages showed that the latter cells formed highly acidified Lm-containing phagosomes that resulted in enhanced virulence gene expression. The hypothesis that differential virulence gene expression contributes to the enhanced susceptibility of P2-deficient macrophages was supported by the finding that the hyper-virulent prfA* strain, that, as mentioned earlier, expresses virulence genes at a constitutively high level, infected P2-expressing and P2-deficient macrophages equally well4. Thus, the availability of a hyper-virulent Lm strain made it possible to test the hypothesis that the P2 host factor negatively regulates pathogen virulence factor deployment. For hI, we showed that this host factor regulates the intracellular trafficking of Lm such that its emergence from the infected cell is restricted; this cellular activity is likely the bases for the enhanced susceptibility of hI-deficient mice for Lm infection15,16.
In studies that documented cellular activities occurring within minutes of infection, it is crucial that prior to their co-incubation, that both the bacteria and the host cells are not excessively exposed to fluctuating temperatures or other environmental conditions that may activate stress responses that would overlap (and confound) infection-induced activities. For the studies described above, this includes such seemingly simple points as minimizing the handling time of Lm just prior to initiating infection. For example, if a bacterial culture is removed from a shaking 37 °C incubator and allowed to sit on a bench top, shifts in both temperature and oxygen availability (among other things) will activate adaptations that may affect the initial phase of the subsequent interaction with the host cell. Similarly, host cells are also sensitive to temperature and media shifts that may affect initial infection responses. Although in practice it is impossible to completely eliminate all fluctuations in bacterial and host cell culturing conditions, by reducing them as much as possible and establishing a standard operating plan, variation between experiments will be minimized.
An additional variable, that in our opinion the importance of which is also underappreciated, is that of the use of antibiotics in cell culture infection models. Gentamicin is often the antibiotic of choice because it is relatively impermeable to the eukaryotic plasma membrane. In both older and current literature, it is generally used at 50 µg/mL to kill extracellular (i.e., non-internalized) bacteria. Recently it has been directly demonstrated that when present at 25 µg/mL, there is sufficient diffusion of gentamicin across the eukaryotic membrane to kill intracellular Lm17. In our experience, this level of gentamicin kills Lm immediately upon contact, whereas much lower levels, in the 2 to 5 µg/mL range kill >99.9% Lm in less than 5 min4. Lawrenz and colleagues have shown that the widely-used gentamicin concentrations of 25–50 µg/mL are also sufficient to kill intracellular Yersinia pestis18. Interestingly, this group also showed considerable differences between cell types in terms of gentamicin permeabilization highlighting that optimal conditions should be determined for each pathogen-host cell pairing.
Divulgaciones
The authors have nothing to disclose.
Materials
| ACK Lysing Buffer | Gibco | A1049201 | |
| ArC Amine Reactive Compensation Beads | Life Technologies | A10346 | |
| BHI (Brain Heart Infusion) broth | EMD Milipore | 110493 | |
| Cell Strainer, 70 µm | VWR | 10199-656 | |
| Collagenase D | Roche | 11088858001 | |
| DMEM media | Gibco | 11965-092 | |
| FACS tubes | BD Falcon | 352054 | |
| FBS – Heat Inactivated | Sigma-Aldrich | F4135-500ML | |
| Hanks’ Balanced Salt solution | Sigma-Aldrich | H6648-6X500ML | |
| LB agar | Grow Cells MS | MBPE-4040 | |
| LIVE/DEAD Fixable Yellow Dead Cell Stain kit | Life Technologies | L349S9 | |
| Rhodamine Phalloidin | Thermo Fischer | R415 | |
| SP6800 Spectral Analyzer | Sony | ||
| Syringe 28G 1/2" 1cc | BD | 329461 | |
| TPP Tissue Culture 48 Well Plates | MIDSCI | TP92048 | |
| TPP Tissue Culture 6 Well Plates | MIDSCI | TP92406 | |
| UltraComp eBeads | eBioscience | 01-2222-42 | |
| Antigen | |||
| CD11b | Biolegend | Flurochrome = PE Cy5, Dilution = 1/100, Clone = M1/70 | |
| CD11c | Biolegend | Flurochrome = AF 647, Dilution = 1/100, Clone = N418 | |
| CD45 | Biolegend | Flurochrome = APC Cy7, Dilution = 1/100, Clone = 30-F11 | |
| F4/80 | Biolegend | Flurochrome = PE, Dilution = 1/100, Clone = BM8 | |
| Live/Dead | Invitrogen | Flurochrome = AmCyN, Dilution = 1/100 | |
| Ly6C | Biolegend | Flurochrome = PacBlue, Dilution = 1/200, Clone = HK1.4 | |
| MHC II | Biolegend | Flurochrome = AF 700, Dilution = 1/200, Clone = M5/114.15.2 | |
| NK 1.1 | Biolegend | Flurochrome = BV 605, Dilution = 1/100, Clone = PK136 |
Referencias
- Freitag, N. E., Port, G. C., Miner, M. D. Listeria monocytogenes – from saprophyte to intracellular pathogen. Nature Review Microbiology. 7 (9), 623-628 (2009).
- Ray, K., Marteyn, B., Sansonetti, P. J., Tang, C. M. Life on the inside: the intracellular lifestyle of cytosolic bacteria. Nature Review Microbiology. 7 (5), 333-340 (2009).
- Miner, M. D., Port, G. C., Freitag, N. E. Functional impact of mutational activation on the Listeria monocytogenes central virulence regulator PrfA. Microbiology. 154, 3579-3589 (2008).
- McCormack, R., et al. Perforin-2 Protects Host Cells and Mice by Restricting the Vacuole to Cytosol Transitioning of a Bacterial Pathogen. Infection and Immunity. 84, 1083-1091 (2016).
- Gregory, S. H., et al. Complementary adhesion molecules promote neutrophil-Kupffer cell interaction and the elimination of bacteria taken up by the liver. Journal of Immunology. 168, 308-315 (2002).
- Shi, C., et al. Monocyte trafficking to hepatic sites of bacterial infection is chemokine independent and directed by focal intercellular adhesion molecule-1 expression. Journal of Immunology. 184, 6266-6274 (2010).
- Pitts, M. G., Combs, T. A., D’Orazio, S. E. F. Neutrophils from Both Susceptible and Resistant Mice Efficiently Kill Opsonized Listeria monocytogenes. Infection and Immunity. 86, 00085 (2018).
- Carr, K. D., et al. Specific depletion reveals a novel role for neutrophil-mediated protection in the liver during Listeria monocytogenes infection. European Journal of Immunology. 41 (9), 2666-2676 (2011).
- Blériot, C., et al. Liver-resident macrophage necroptosis orchestrates type 1 microbicidal inflammation and type-2-mediated tissue repair during bacterial infection. Immunity. 42 (1), 145-158 (2015).
- Jones, G. S., D’Orazio, S. E. F. Monocytes are the predominant cell type associated with Listeria monocytogenes in the gut, but they do not serve as an intracellular growth niche. Journal of Immunology. 198, 2796-2804 (2017).
- Agaisse, H., et al. Genome-wide RNAi screen for host factors required for intracellular bacterial infection. Science. 309, 1248-1251 (2005).
- Cheng, L. W., et al. Use of RNA interference in Drosophila S2 cells to identify host pathways controlling compartmentalization of an intracellular pathogen. Proceedings of the National Academy of Science U S A. 102, 13646-13651 (2005).
- Singh, R., Jamieson, A., Cresswell, P. GILT is a critical host factor for Listeria monocytogenes infection. Nature. 455, 1244-1247 (2008).
- Burrack, L. S., Harper, J. W., Higgins, D. E. Perturbation of vacuolar maturation promotes listeriolysin O-independent vacuolar escape during Listeria monocytogenes infection of human cells. Cellular Microbiology. 11, 1382-1398 (2009).
- Shrestha, N., et al. The host-encoded Heme Regulated Inhibitor (HRI) facilitates virulence-associated activities of bacterial pathogens. PLoS One. 8, 68754 (2013).
- Bahnan, W. The eIF2α Kinase Heme-Regulated Inhibitor Protects the Host from Infection by Regulating Intracellular Pathogen Trafficking. Infection and Immunity. 20, 00707 (2018).
- Kortebi, M., et al. Listeria monocytogenes switches from dissemination to persistence by adopting a vacuolar lifestyle in epithelial cells. PLoS Pathogen. 13, 1006734 (2017).
- VanCleave, T. T., Pulsifer, A. R., Connor, M. G., Warawa, J. M., Lawrenz, M. B. Impact of Gentamicin Concentration and Exposure Time on Intracellular Yersinia pestis. Frontiers in Cellular and Infection Microbiology. 7, 505 (2017).

