Chronic Thromboembolic Pulmonary Hypertension and Assessment of Right Ventricular Function in the Piglet
Summary
Chronic Thromboembolic Pulmonary Hypertension (CTEPH) and Right Ventricular (RV) dysfunction were induced in piglets by progressive obstruction of the pulmonary arteries. Consequences were remarkably similar to those observed in CTEPH patients. This animal model would be a very useful tool for pathophysiology and therapeutic experiments on CTEPH and RV failure.
Abstract
An original piglet model of Chronic Thromboembolic Pulmonary Hypertension (CTEPH) associated with chronic Right Ventricular (RV) dysfunction is described. Pulmonary Hypertension (PH) was induced in 3-week-old piglets by a progressive obstruction of the pulmonary vascular bed. A ligation of the left Pulmonary Artery (PA) was performed first through a mini-thoracotomy. Second, weekly embolizations of the right lower pulmonary lobe were done under fluoroscopic guidance with n-butyl-2-cyanoacrylate during 5 weeks. Mean Pulmonary Arterial Pressure (mPAP) measured by ritght heart catheterism, increased progressively, as well as Right Atrial pressure and Pulmonary Vascular Resistances (PVR) after 5 weeks compared to sham animals. Right Ventricular (RV) structural and functional remodeling were assessed by transthoracic echocardiography (RV diameters, RV wall thickness, RV systolic function). RV elastance and RV-pulmonary coupling were assessed by Pressure-Volume Loops (PVL) analysis with conductance method. Histologic study of the lung and the right ventricle were also performed. Molecular analyses on RV fresh tissues could be performed through repeated transcutaneous endomyocardial biopsies. Pulmonary microvascular disease in obstructed and unobstructed territories was studied from lung biopsies using molecular analyses and pathology. Furthermore, the reliability and the reproducibility was associated with a range of PH severity in animals. Most aspects of the human CTEPH disease were reproduced in this model, which allows new perspectives for the understanding of the underlying mechanisms (mitochondria, inflammation) and new therapeutic approaches (targeted, cellular or gene therapies) of the overloaded right ventricle but also pulmonary microvascular disease.
Introduction
Chronic Thromboembolic Pulmonary Hypertension (CTEPH) is a subtype of Pulmonary Hypertension (PH) due to chronic pulmonary vascular bed obstruction by persistent and organized clots related to one or more acute pulmonary embolisms1-3. A combination of obstructive and non-obstructive microvascular disease leads to an additional increase in pulmonary vascular resistance4. The right ventricle must first adapt with compensated hypertrophy to maintain the cardiac output. Without treatment, the right ventricle dilates and fails over time. In the modern era, PH remains a progressive and often fatal disease despite the use of modern targeted therapies5. Many studies have shown that right ventricular (RV) adaptation to pressure overload is the main determinant of survival in PH patients. For that reason, understanding the mechanisms underlying the transition from adaptive to maladaptive RV remodeling is a keystone for treatment and development of new therapies. Because PH is rare and tissue sampling is almost infeasible in these frail patients, experimental studies are required. Furthermore, preclinical studies are mandatory to ascertain that a drug with benefit in the pulmonary vasculature does not cause RV impairment.
For many years, different experimental models of PH and RV failure have been developed with advantages and limitations6,7. In the pharmacological murine models (Monocrotaline, SU5416, Hypoxia), PH and RV failure occur secondary to a massive inflammation, ischemia or toxic stressor that might induce several “sides effects” and bias in molecular pathway analysis. Furthemore, RV endomyocardial biopsies in a murine model should be very challenging without sacrifying the animal. Surgical models in larger animals are more physiological but do not affect the pulmonary vasculature (pulmonary artery banding, systemic-to-pulmonary shunt) or induce acute PH and RVF (acute pulmonary embolism). The aim of this article is to describe an original model of CTEPH in piglet that is more representative of CTEPH pathophysiology. This large animal model enables repeated noninvasive and invasive measurements usually performed in clinical practice (right heart catheterization) to follow changes in pulmonary hemodynamics and RV function.
Protocol
This protocol was approved by the local ethics committee on animal experiments and by the Institutional Committee on Animal Welfare of our institution. All animals received humane care in compliance with the “Principles of Laboratory Animal Care” formulated by the National Society for Medical Research and the “Guide for the Care and Use of Laboratory Animals” prepared by the Institute of Laboratory Animal Resources and published by the National Institutes of Health (NIH Publication No. 86-23, revised 1996).
General considerations: All animals must be treated with respect, according to the 3Rs rules (National Centre for Replacement Refinement and Reduction of Animals in Research). Surgical procedures must be performed with a strict sterility and in the same way that for human beings. All medical devices must be sterile.
1. Anesthesia Protocol
NOTE: Large White piglets weighing 20 Kg (3-weeks-old) were used. Pulmonary Hypertension was induced progressively. The first step involved a left pulmonary artery (PA) ligation through a left thoracotomy. Following steps consisted of performing weekly PA embolizations during 5 weeks. All procedures were performed under general anesthesia.
- Do not feed the animals 12 hr before the procedure.
- Do a premedication of the piglet, perform an intramuscular injection using 30 mg/kg of Ketamine Hydrochloride and aropine 0.05 mg/kg in the neck muscles, 30 min before the procedure.8
- When the pig is sedated, insert a catheter into the ear vein.
- Perform intravenous a bolus of fentanyl (0.005 mg/kg) and propofol (2mg/kg) before intubation. Inject intravenously in the ear vein Cisatracurium (0.3 mg/kg) and intubate the pig (non-selective intubation with a 7 French probe)9.
- Place continuous monitoring devices on the piglet: continuous EKG, expiratory CO2 and oxymetry8,9. Insert an arterial fluid field catheter through the carotid artery under echography guidance to monitor the systemic arterial pressure8-10.
- Maintain general anesthesia with isoflurane (2%) in 100% oxygen supplement, continuous intravenous infusion of fentanyl (0.004 mg/kg) and propofol (3 mg/kg).
- Add an antibioprophylaxy with an injection of Cefatoxine (1 g) and Gentamycine (80 mg).
- Prevent intra operative and post operative pain with injection of nalbuphine (0.01 mg/kg) t.i.d.
- Check every 15 min the completeness of the anesthesia: absence of movement, stable heart rate, blood pressure, oxygenation.
- Use of vet ointment on eyes to prevent dryness while under anesthesia.
2. Ligation of the Left Pulmonary Artery
- Install the piglet in left side-lying position, shave the operative area and disinfect the skin with an alcoholic solution. Use a local sterile field.
- Open the chest through a small left lateral thoracotomy (5 to 10 cm) in the 4th intercostals’ space. Do not go to behind the tip of the scapula. Carefully retract the lung towards the diaphragm.
- Once ideal surgical window located, retract the left azygos vein and dissect the main left pulmonary artery before tying it with a non-absorbable 2/0 silk.
NOTE: It is very important not to open the pericardium. - Close the chest layer after layer with absorbable sutures. Use a chest tube to remove the post operative pneumothorax. Remove the chest tube just after the piglet extubation.
3. Embolization of the Right Lower Lobe Pulmonary Artery
- After general anesthesia, put the piglet in a supine position. Carry out a continuous monitoring of the oxymetry, expiratory CO2, EKG, mean systemic blood pressure (mPA) and mean pulmonary artery pressure (mPAP) throughout the procedure.
- Insert all catheters percutaneously with echographic guidance. Insert an arterial 6 French catheter in the carotid artery for blood pressure monitoring and an 8 French sheath in the superior vena cava through the jugular vein (Perform the puncture 2 cm above the suprasternal notch with a 45° angle direction).
- Under fluoroscopic guidance, insert, through the 8 Fr sheath, a 5 French angiographic catheter in the right pulmonary artery. The tip of the catheter must be in a segmental lower lobe pulmonary artery.
- Prepare the material for pulmonary artery embolization: 1 ml of soft tissue glue containing N-butyl-2-cyanoacrylate is added to 2 ml of a lipidic contrast dye.
CAUTION: Avoid skin or eyes contact with the N-butyl-2-cyanoacrylate. - When the angiographic catheter is well positioned, inject 0.2 ml to 0.4 ml of the preparation in the pulmonary artery. Assess the tolerance of the embolization by measuring the mPAP / mPA ratio that should not exceed 0.5. Stop embolization if oxygen saturation was < 90% and/or the mPA dropped under 60 mm Hg and/or the cardiac output was under 2 L/min.
- Remove the angiographic catheter and sheaths and perform digital compressions of the puncture site.
4. Hemodynamic Assessment
- After general anesthesia, position the piglet in a supine position. Carry out a continuous monitoring of the oxymetry, expiratory CO2, EKG, systemic blood pressure (mPA) and pulmonary blood pressure (mPAP) throughout the procedure.
- Ventilate the piglets with the lowest FiO2 as possible according to the oxygen saturation (> 95%).
- Insert all catheter percutaneously under echographic guidance. An arterial 6 French catheter is inserted in the carotid artery and an 8 French sheath is inserted in the superior vena cava (Perform the puncture 2 cm above the suprasternal notch with a 45° angle direction).
- Insert a 7 French Swan-Ganz catheter in the pulmonary artery trunk. Assess the cardiac output by the thermo dilution technique, with injection of 10 ml of saline solution at 4 °C.
- Record the following parameters: systolic, diastolic and mean systemic and pulmonary arterial pressure, heart rate, oxygen saturation, right atrial pressure, cardiac output.
5. Echocardiographic Assessment of the Right Ventricle
- After general anesthesia, install the piglet in supine position and perform a trans thoracic echocardiography according human guidelines for RV screening. Record video loops during an end-expiratory pause.
6. Pressure-Volume Loops Assessment with the Conductance Method
- After general anesthesia, install the piglet in a supine position. Carry out a continuous monitoring of the oxymetry, expiratory CO2, EKG, systemic blood pressure (mPA) and pulmonary blood pressure (mPAP) throughout the procedure.
- Insert an arterial 6 French catheter in the right or left carotid artery and an angiographic catheter in the left ventricle. Insert an 9 French sheath in the superior vena cava, an 8 French in the right or left femoral vein and an arterial PiCCO catheter in the right or left femoral artery. Insert all catheters percutaneously under echographic guidance.
- Perform the pressure and volume calibration of the conductance probe according to the manufacturer’s recommendations. Measure the blood resistivity (Rho) by sampling 5 ml of arterial blood. Harvest 5 ml of arterial blood, de-air the syringe and fill the probe for the measurement of the blood resistivity. 10-13.
- Insert the conductance catheter in the right ventricle through the 9Fr sheath in the superior veina cava. Place properly the end of the catheter with fluoroscopic guidance. Place the end of the catheter in the apex of the right ventricle and insert all long as possible in the ventricle.
- Control the quality of the loops. (Figure 6)
- Insert an ballon expendable in the inferior veina cava through the femoral vein. Place the extremity just below the right atrial. Use fluoroscopic guidance.
- Record pressure-volume loops of the right ventricle at basal state and during inferior vena cava occlusion as previously described10-12. (Figure 7)
7. Endomyocardial Biopsies of the Right Ventricle
- After general anesthesia, position the piglet in a supine position. Carry out a continuous monitoring of the oxymetry, expiratory CO2, EKG, systemic blood pressure (mPA) and pulmonary blood pressure (mPAP) throughout the procedure.
- Insert percutaneously a 10 French sheath in the superior vena cava. Insert a 7 French Swan-Ganz (SG) probe and a long 7.5 French catheter sheath in the right atrium. When the tip of the SG probe is well placed in the right ventricle (RV), inflate the balloon of the SG probe, push the long-sheath catheter in the RV against the balloon. Deflate the balloon and remove the SG probe leaving the long-sheath catheter in the RV. The good position of the long-sheath’s tip is controlled by fluoroscopy and echocardiography.
- Insert the biotome in the long-sheath and perform endomyocardial biopsies under echographic, fluoroscopic and EKG control.
8. General Post-surgery Care Considerations
- After surgery, extubate the piglet only after recovery of spontaneous respiratory functions.
- For post operative medication, perform an intramuscular injection of Cefatoxine (1 g) Die for 5 days and deliver appropieted analgesia (Buprenorphin, intramusculary injection 0.01 mg/kg Bid for 10 days.
- Do not leave an animal that has undergone surgery to the company of other animals until fully recovered.
9. Euthanasia Method
- Euthanize the animals in the followed situations; End of experimentation, lost of weight 15% or more in one week, unibability to adequately feed themselves, anorexia, not treatable infection, pain or other didease, desease too sévère : cyanosis, major dyspnea
- During general anesthesia with sevoluorane 8%, inject a high dose of propofol (0.5 mg/kg) associated with a lethal dose of potassium chloride (0.2 g/kg). When the heart is stopped in diastole, harveste the heart and lung bloc in order to do a histological and molecular study.
Representative Results
Feasability
This piglet model of chronic post-embolic pulmonary hypertension has been established in our laboratory in 2009-2010. Since 2011, we used 70 piglets and we performed 63 completed models. In our experience, the realization of this model required a learning curve.
Regarding the mortality, we observed 5 unplanned deaths (7.1%), mainly in the first part of our experience. The two critical steps were first, the pulmonary embolization and second, the endomyocardial biopsies. Four piglets died from severe acute right heart failure after pulmonary embolization. One piglet died from an unknown cause. Regarding the morbidity, 4 piglets (5.7%) had a major complication during procedures.
Two piglets needed urgent pericardial drainage during the endomyocardial biopsies procedure. They required urgent pericardo-synthesis because of a perforation of the right ventricular free wall. The recovery was uneventful in all cases. Since the use of echographic guidance to perform endomyocardial biopsies, we did not observe this complication anymore.
Two others piglets developed a pyothorax after the pulmonary artery ligation and they required euthanasia 7 days after de surgery.
We used Large White piglets with an average weight of 20 kg. All animals were males and came from a French farm (Gambais, France). The first hours after the surgery, the piglets were placed in a specific room with oxygen and underfloor heating. Then, they were housed alone or with another piglet in a 2 m2 cage.
The model of Chronic Pulmonary Hypertension in piglet was fulfilled 6 weeks after the left pulmonary ligation and 5 repeated embolizations (Figure 1). The left pulmonary artery was ligated through a small lateral thoracotomy. The first embolization of the right lower pulmonary artery was performed 5 days later. Embolizations are repeated weekly during 5 weeks with an average of 3.2±0.8 ml of N-butyl-2-cyanoacrylate per embolization. Effects on hemodynamics, pulmonary vasculature and right ventricle can be described as follows.
The sham animals underwent only a left thoracotomy without left pulmonary artery ligation. They do not have embolization of the pulmonary arteries but underwent repeated hemodynamics, echocardiographic and histologic assessments at the same time as the other animals.
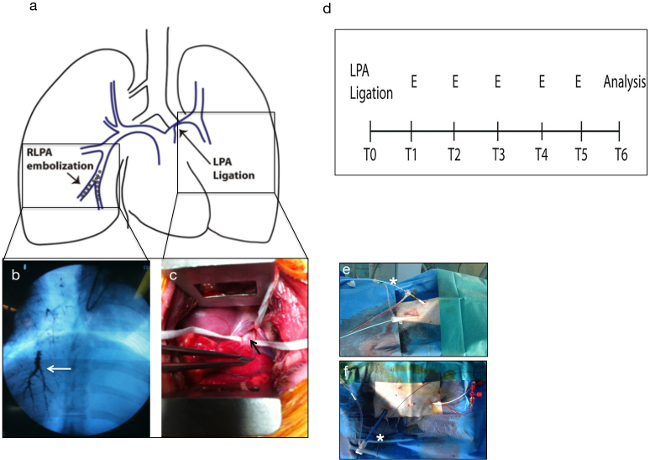
Figure 1. CTEPH animal model design. The left pulmonary artery ligation was followed by repeated embolization of the lower pulmonary lobe artery (A and D). LPA ligation (arrow) was performed through a small left thoracotomy (C). Embolizations were performed with fluoroscopic guidance weekly for 5 weeks (B). All experiments were performed under general anesthesia and percutaneous vascular accesses were used for embolizations and pressure measurements: (E) percutaneous superior veina cava (star) and right carotid artery catherization. (F) 8Fr sheath in the right femoral vein (star) and arterial thermodilution sheath sensor in the left femoral artery. Please click here to view a larger version of this figure.
Hemodynamic results
The mean pulmonary arterial pressure (mPAP) increased progressively after embolizations above 25 mm Hg. Hemodynamic data are summarized in Table 1. The right atrial pressure, the mPAP/mSAP ratio and the pulmonary vascular resistances also increased after repeated embolizations. The Cardiac Index trended to decrease after several embolizations, reflecting the RV dysfunction. The mPAP/mSAP ratio also increased progressively. This ratio must not exceed 0.5 just after acute embolization because of the increased risk of death. For this reason, embolizations must be performed with a maximum of 2 ml per injection. Reinjection of 1 ml can be performed if the previous one was well tolerated hemodynamically. In this model, the PH was only precapillary because the PCWP did not increase.
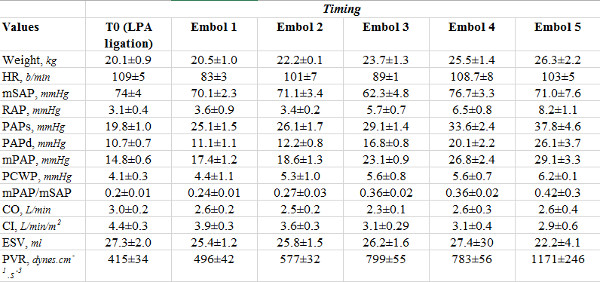
Table 1. Hemodynamic data from 8 piglets models of CTEPH. HR: heart rate; mSAP: mean systemic arterial pressure; RAP: right atrial pressure; PAPs: systolic pulmonary arterial pressure; PAPd: diastolic pulmonary arterial pressure; mPAP: mean pulmonary arterial pressure; PCWP: pulmonary capillary wedge pressure; CO: cardiac output; CI: cardiac index; ESV: ejection systolic volume; PVR: pulmonary vascular resistances.
Remodeling of pulmonary arteries
Bronchial circulation hypertrophy was noted in the left lung, the right lower lobe and along the mediastinal pleura. In pathology, large and numerous submucosal bronchial arteries were observed in the obstructive lungs (left lung and right lower lobe), reflecting the increase of angiogenesis in these territories. (Figure 2) Post obstructive pulmonary vasculopathy with media hypertrophy was also found in obstructed territories (left lung and right lower lobe), while overflow vasculopathy was observed in the non-obstructive territories (right upper lobe). (Figure 3) Pathology also showed the chronic obstruction of the right lower pulmonary artery lobe by an unresolved thrombus of N-butyl-2-cyanoacrylate and fibrin.
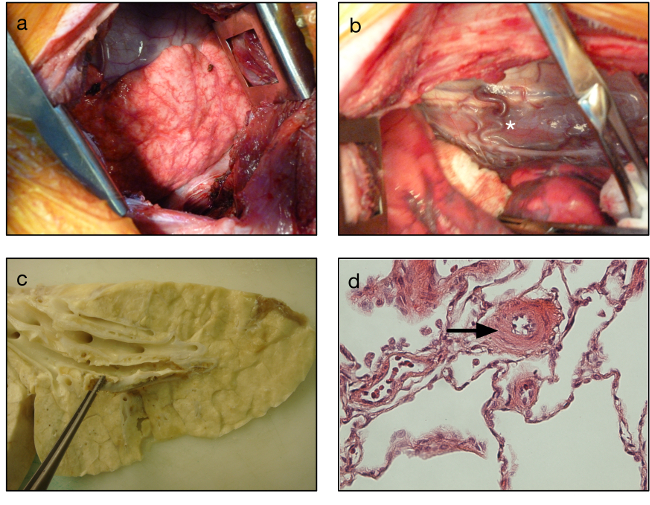
Figure 2. Vascular remodeling in the CTEPH model. Intraoperative views showing the development of bronchial arteries in the left lung and visceral pleura (A) and in the mediastinum (star, B). Gross anatomy of the harvested right lower lobe showing the unresolved intravascular clots (C). Media hypertrophy in the small pulmonary arteries seen in light microscopy (arrow) (D). Please click here to view a larger version of this figure.
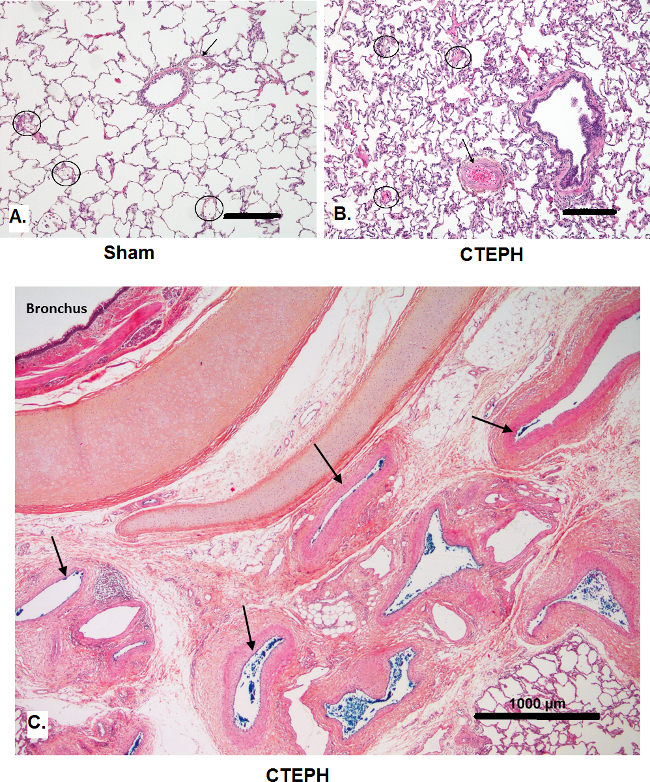
Figure 3. Comparative pulmonary vascular remodeling in Sham and CTEPH animals (Hematoxylin and eosin staining). Histology from a sham piglet (A): the pulmonary artery (arrow) and three microvessels (circles) display slender walls and no hypertrophic changes can be observed. In a CTEPH piglet after 5 weeks (B), pulmonary arteries (arrow) in the periphery of the upper right lobe show medial thickening. However, microvessels (circles) in this territory present with only very mild changes (scale bars, 200 µm). At higher magnification (C), bronchial arteries (arrows) from the upper right lobe (unobstructed territory) appear unremodelled and of normal size in a CTEPH piglet at 5 weeks (scale bar, 1,000 µm). Please click here to view a larger version of this figure.
Remodeling of right ventricle
Significant enlargement associated with right ventricular hypertrophy and fibrosis was observed after 6 weeks (Table 2 and Figure 4 and video 1 and video 2). The RV area, Right Atrial (RA) area, RV diameters were increased after repeated embolizations. The RV wall thickness also increased. RV hypertrophy was confirmed in light microscopy after heart’s harvesting. In echocardiography, Tricsupid Annula Plane Systolic Excursion (TAPSE) and Right Ventricular Fractionnal Area Change (RVFAC) were decreased after 6 weeks reflecting RV dysfunction in this model. RV function impairment was also found with PVL analysis with a decrease of the ventricular-arterial coupling (Table 3).
| Timing | ||
| Values | T0 (LPA ligation) | 6 weeks |
| RV diastole area, cm2 | 4.5±0.2 | 7.1±0.9 |
| RV basal diameter, cm | 1.5±0.8 | 3.7±1.3 |
| RV free wall thickness, cm | 0.3±0.02 | 0.59±0.04 |
| RA area, cm2 | 3.9±0.4 | 5.9±0.3 |
| RVFAC, % | 0.50±0.03 | 25.0±1.0 |
| RV TAPSE, cm | 1.6±0.2 | 1.11±0.07 |
| LV EF, % | 55.7±4.9 | 52.2±6.0 |
Table 2. RV remodeling in echocardiography. RVFAC: right ventricular fractional area change; TAPSE: tricuspid annular plane excursion; LV EF: left ventricular ejection fraction.
| Timing | ||
| Values | T0 (LPA ligation) | 6 weeks |
| RV Stroke Work, mm Hg.ml-1 | 579±55 | 2248±148 |
| RV Elastance, Ees | 0.33±0.06 | 0.40±0.06 |
| Pulmonary arterial Elastance, Ea | 0.32±0.05 | 0.51±0.03 |
| RV coupling, Ees/Ea | 1.33±0.19 | 0.78±1.0 |
Table 3. Functional remodeling of right ventricle in Pressure-Volume Loops analysis.
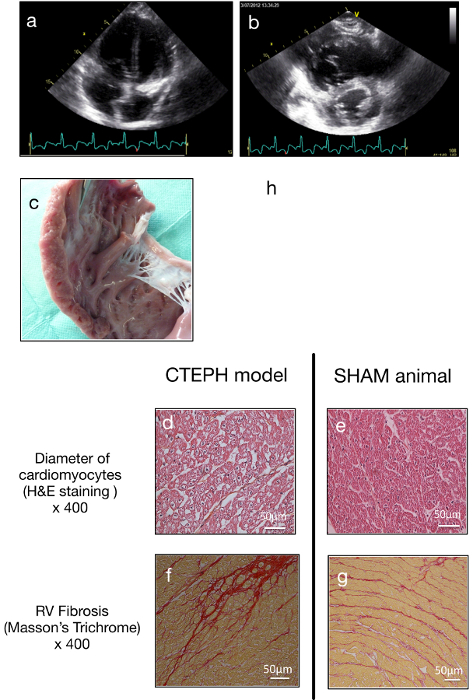
Figure 4. Right ventricular remodeling. Echocardiography showed enlargement of the right ventricle in the four cavities view (A) and short parasternal axis (B). Note the shift of the interventricular septum and the compression on the left ventricle. RV hypertrophy was confirmed macroscopically (C) and by light microscopy with enlargement of transversal axis of cardiomyocytes compared with sham (D and E). As showed in (H), the Fulton ratio correlated with the mean pulmonary arterial pressure. RV fibrosis rate was increased in the CTEPH animals compared to SHAM (F and G). Please click here to view a larger version of this figure.
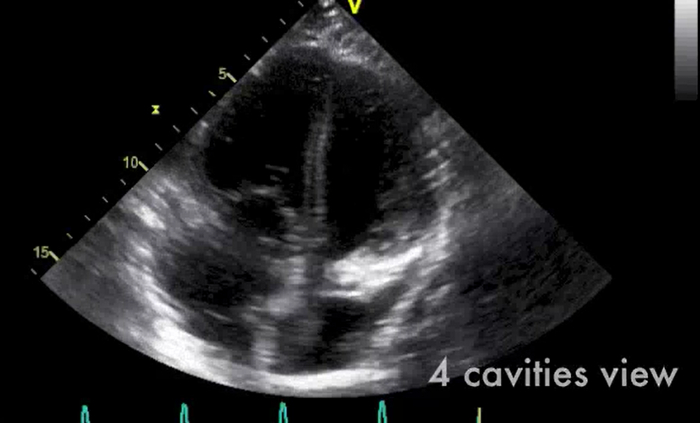
Video 1: Transthoracic 4 cavities and short axis views showing enlargement of the right ventricle. Please click here to view this video.
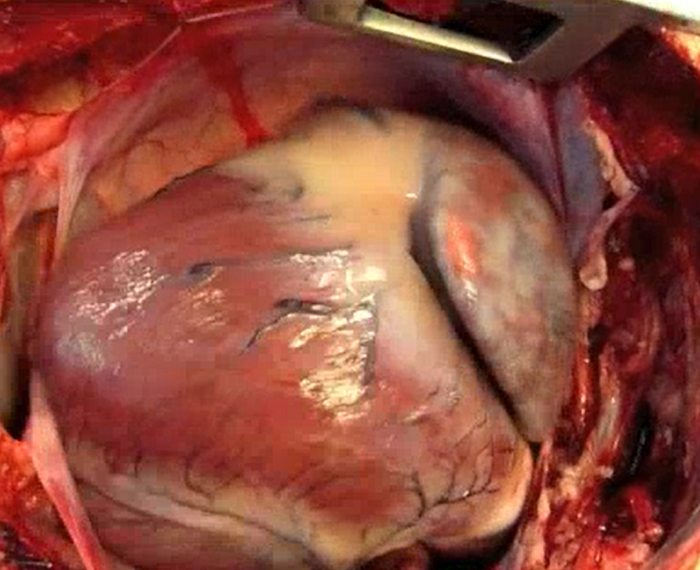
Video 2: Operative view after median sternotomy. The dilated right ventricle fill the pericardium. Please click here to view this video.
In order to perform a genetic and metabolic study, a technique of endomyocardial biopsies of the right ventricle was developed in the present model of chronic pressure overload. This technique is safe and allows repeated fresh myocardial sampling in anesthetized piglets. Echocardiographic and fluoroscopic control reduced the risk of RV wall perforation with the biotome. The long catheter technique is a good strategy to avoid tricuspid valve injury (Figure 5).
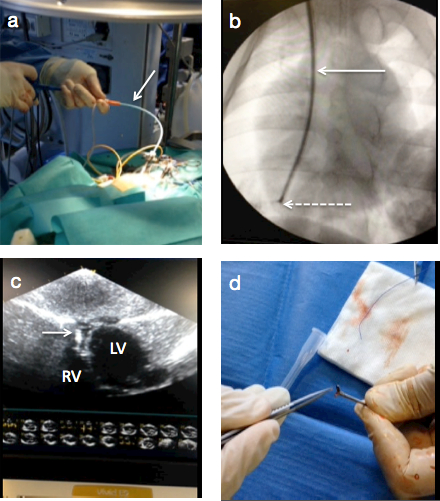
Figure 5. Endomyocardial biopsies in the CTEPH model. (A) a 55 cm jugular biotome is insert in the right ventricle through a transcutaneous 7 Fr long catheter sheath. Forceps progression was controlled with echocardiography (C) and fluoroscopy (B) and a 6mm3 myocardial piece is extracted (D). Please click here to view a larger version of this figure.
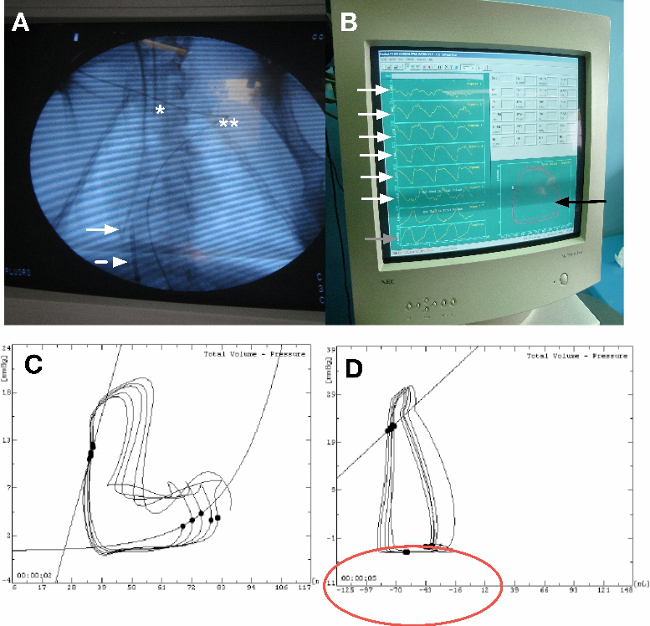
Figure 6. Appropriate placement of the conductance probe for PV loops assessment. (A) Place the end of the probe at the apex of the right ventricle under fluoroscopic guidance (solid arrow). Insert minimum 3 segments in the right ventricle and the probe has to be straight line. Insert an occlusion balloon in the inferior veina cava through the femoral vein. The end of the balloon must be just at the right atrium entry (dashed arrow) (*: intubation probe; ** EKG wire. (B) Verify that the volume segments of the probe must be in phase in diastole and systole and the “good shap of the loop on the screen. (C) Example of bad shape of the PV loop due to a wrong placement of the volume segments in the right ventricle. (D) Example of a bad volume calibration. The ventricular volumes are negatives. Please click here to view a larger version of this figure.
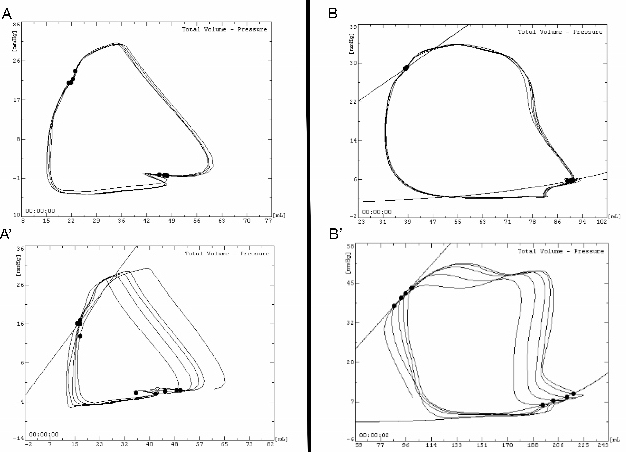
Figure 7. Example of PV loop shape at basal state and during inferior veina cava occlusion in SHAM (A and A’) and CTEPH piglet (B and B’). PV loop in normal right ventricle has a triangle shape, with lower pressure and volume values compared with right ventricle under pulmonary hypertension. Please click here to view a larger version of this figure.
Discussion
As in human clinical practice, respect of asepsis rules is mandatory during all surgical procedures. In the original CTEPH piglet model described by O. Mercier et al., the left pulmonary artery ligation was performed after opening the pericardium, through a median sternotomy14. Because the pericardium was left opened, the interaction between the right ventricle and the pericardium was impaired and right heart failure was delayed. Adverse effect of RV enlargement on cardiac output has been demonstrated to be significantly lower when the pericardium is open15. For this reason, it seems better not to open the pericardium at the time of the left PA ligation. Although it is a more technically demanding technique (care must be paid to preserve the phrenic nerve and the left lung) and despite the problem of pain control, left lateral thoracotomy offered the best approach for the left PA ligation outside the pericardium. As left PA ligation does not result in increased mPAP, progressive embolization of the right lower lobe PA was necessary. The second critical point of this model is the risk of massive pulmonary embolism after right lower lobe PA embolization. Maximum injection of 2 ml by 2 ml of N-butyl-2-cyanoacrylate was done and hemodynamic tolerance was appreciated between each injection. The mPAP / mPA ratio should not exceed 0.5. In addition, embolization wa sstopped if oxygen saturation was < 90% and/or the mPA dropped under 60 mmHg and/or the cardiac output was under 2 L/min.
Five embolizations were usually perform for each CTEPH model. The number and the frequency of the embolizations can be adjusted according to the warranted severity of induced pulmonary hypertension. Four days between 2 successive embolizations had to be respected for a better hemodynamic tolerance. Additional embolizations or a longer observation time may replicate the advanced stages of CTEPH with severe RV failure.
This model does not replicate the origin of the disease but just the consequences of chronic pulmonary vascular obstruction. There are no clues on the pathophysiology of fresh clots becoming organized and fibrous intravascular material rather than disappear.
This is the first large-animal model of chronic PH that is reproducible in a short time frame allowing further therapeutic testing. All animals increased the mPAP above 25 mm Hg within 6 weeks after the beginning of the experiment. It reproduced all the morphological, functional and biological changes seen in human CTEPH right ventricles. In addition, the pulmonary microvascular lesions were reproduced in two separate vascular territories (obstructed vs. non obstructed). At least, this model reproduced the interaction between the injured pulmonary vasculature (occluded and remodeling territories) and the right ventricle.
Several physiological studies have been based on this original and unique CTEPH model11,12,16. It allows new perspectives for the understanding of the underlying mechanisms of RV failure (mitochondria, inflammation) and new therapeutic approaches (targeted, cellular or gene therapies). This model may also help to investigate mechanisms of RV recovery after surgical treatment of PH. Indeed, left lung reperfusion can be performed, reproducing surgical PA desobtruction and RV unloading. Interactions between pulmonary microvascular disease and the right ventricle would be the aim of further studies as both are interdependent and new therapy should target both of them.
Divulgations
The authors have nothing to disclose.
Acknowledgements
The authors thank the team at the Laboratory of Surgical Research, Marie Lannelongue Hospital, for technical assistance and animal care. The VividE9 cardiac ultrasound system (General Electric Medical System) was financed by a grant from the Cardio-vasculaire-Obésité Domaine D'Intérêt Majeur (CODDIM cod 100158, RégionIle-de-France, France).
References
- Simonneau, G., et al. Updated clinical classification of pulmonary hypertension. J Am Coll Cardiol. 54, S43-S54 (2009).
- Dartevelle, P., et al. Chronic thromboembolic pulmonary hypertension. Eur Respir J. 23 (4), 637-648 (2004).
- Hoeper, M. M., Mayer, E., Simonneau, G., Rubin, L. J. Chronic thromboembolic pulmonary hypertension. Circulation. 113 (16), 2011-2020 (2006).
- Galie, N., Kim, N. H. Pulmonary microvascular disease in chronic thromboembolic pulmonary hypertension. Proc Am Thorac Soc. 3 (7), 571-576 (2006).
- Humbert, M., et al. Survival in patients with idiopathic, familial, and anorexigen-associated pulmonary arterial hypertension in the modern management era. Circulation. 122 (2), 156-163 (2010).
- Guihaire, J., et al. Experimental models of right heart failure: a window for translational research in pulmonary hypertension. Semin Respir Crit Care Med. 34 (5), 689-699 (2013).
- Mercier, O., Fadel, E. Chronic thromboembolic pulmonary hypertension: animal models. Eur Respir J. 41 (5), 1200-1206 (2013).
- Kaiser, G. M., Heuer, M. M., Fruhauf, N. R., Kuhne, C. A., Broelsch, C. E. General handling and anesthesia for experimental surgery in pigs. J Surg Res. 130 (1), 73-79 (2006).
- Flegal, M. C., Kuhlman, S. M. Anesthesia monitoring equipment for laboratory animals. Lab Anim (NY). 33 (7), 31-36 (2004).
- Guihaire, J., et al. Right ventricular reserve in a piglet model of chronic pulmonary hypertension. Eur Respir J. , (2014).
- Guihaire, J., et al. Right ventricular plasticity in a porcine model of chronic pressure overload. J Heart Lung Transplant. 33 (2), 194-202 (2014).
- Guihaire, J., et al. Non-invasive indices of right ventricular function are markers of ventricular-arterial coupling rather than ventricular contractility: insights from a porcine model of chronic pressure overload. Eur Heart J Cardiovasc Imaging. 14 (12), 1140-1149 (2013).
- Kass, D. A., Yamazaki, T., Burkhoff, D., Maughan, W. L., Sagawa, K. Determination of left ventricular end-systolic pressure-volume relationships by the conductance (volume) catheter technique. Circulation. 73 (3), 586-595 (1986).
- Mercier, O., et al. Piglet model of chronic pulmonary hypertension. Pulm Circ. 3 (4), 908-915 (2013).
- Brooks, H., Kirk, E. S., Vokonas, P. S., Urschel, C. W., Sonnenblick, E. H. Performance of the right ventricle under stress: relation to right coronary flow. J Clin Invest. 50 (10), 2176-2183 (1971).
- Boulate, D., et al. Pulmonary microvascular lesions regress in reperfused chronic thromboembolic pulmonary hypertension. J Heart Lung Transplant. , (2014).

