Subcutaneous Trigeminal Nerve Field Stimulation for Refractory Facial Pain
Summary
Treating chronic or neuropathic facial pain can be challenging when medical or standard treatment fails. Subcutaneous nerve field stimulation is the least invasive form of neuromodulation and is used for chronic back pain. We applied this technology to treat chronic and neuropathic trigeminal facial pain.
Abstract
Chronic or neuropathic trigeminal facial pain can be challenging to treat. Neurosurgical procedures should be applied when conservative treatment fails. Neuromodulation techniques for chronic facial pain include deep brain stimulation and motor cortex stimulation, which are complex to perform. Subcutaneous nerve field stimulation is certified for chronic back pain and is the least invasive form of neuromodulation. We applied this technique to treat chronic and neuropathic trigeminal pain as an individual therapy concept. First, trial stimulation is performed. Subcutaneous leads are placed in the painful trigeminal dermatome under local anesthesia. The leads are connected to an external neurostimulator that applies constant stimulation. Patients undergo a 12 day outpatient trial to assess the effect of the stimulation. Electrodes are removed after the trial. If the patient reports pain reduction of at least 50% in intensity and/or attack frequency, a reduction in medication or increase in quality of life, permanent implantation is scheduled. New electrodes are implanted under general anesthesia and are subcutaneously tunneled to an infraclavicular internal pulse generator. Patients are able to turn stimulation on and off and to increase or decrease the stimulation amplitude as needed.
This technique represents a minimal invasive alternative to other more invasive means of neuromodulation for trigeminal pain such as motor cortex stimulation or deep brain stimulation.
Introduction
The neurosurgical armamentarium to treat trigeminal pain is as large and diverse as the underlying etiologies. In cases of classical trigeminal neuralgia (TN) caused by arterial compression at the brainstem root entry zone of the trigeminal nerve microvascular decompression (MVD)1 is highly effective. Percutaneous destructive techniques at the Gasserian Ganglion (such as radiofrequency thermocoagulation, glycerol injection or balloon compression2) and stereotactic radiosurgery for trigeminal neuralgia3 can be applied in cases without neurovascular conflict or whenever there are contraindications for open microsurgery. However, all techniques are associated with certain recurrence rates of pain. Furthermore, the treatment itself bears risks for nerve damage resulting in neuropathic pain or even painful post-traumatic trigeminal neuropathy. AT last, trigeminal pain of central origins (e.g. post stroke pain) will not respond to MVD or destructive techniques at the Gasserian Ganglion but needs to be treated by neuromodulation such as deep brain stimulation (DBS) or motor cortex stimulation (MCS).
Neuromodulation is a term used for surgical techniques that appear to alter neural activity without causing irreversible tissue damage. Neuromodulative treatments are reversible, adaptable and usually work with intermittent or continuous application of electrical currents to parts of the peripheral or central nervous system. There are several certified (CE and/or FDA approved) treatments available to treat chronic and/or neuropathic pain of the trunk and the extremities such as epidural spinal cord stimulation (SCS), peripheral nerve field stimulation (PNFS) or dorsal root ganglion stimulation (DRG)4. However, currently there is no CE or FDA approved treatment available for chronic neuropathic facial and trigeminal pain.
Deep brain stimulation (DBS) and motor cortex stimulation (MCS) have been applied in multiple case series for patients with chronic facial pain of different origins5. However, both techniques present a high level of complexity and demand special physician expertise. There is a need for simple, cost efficient and effective neuromodulation for chronic trigeminal and facial pain when conservative treatment fails and destructive techniques want to be avoided.
Besides surgical approaches an array of non-invasive or temporary forms of neuromodulation is available to treat chronic pain (e.g. PENS: percutaneous electrical neurostimulation, TENS: transcutaneous electrical neurostimulation, TMS: transcranial magnetic stimulation).
Subcutaneous peripheral nerve field stimulation (sPNFS) is the least invasive form of neuromodulation6. One or more electrodes are placed in the subcutaneous tissue in the painful area. Continuous electrical stimulation is applied to create a pleasant paresthesia that covers the painful area. The exact mechanism of action is not known. However, despite all shortcomings the similar mechanisms like in the gate control theory – or variations of it – which postulates modulation of nociceptive input by inhibitory fibers is most often applied. Furthermore a local depolarization block of the peripheral nerve fibers with reduced excitability and changes in the micro environment regarding inflammatory proteins are discussed7.
As in most neuromodulation procedures a test trial with externalized electrodes connected to a pulse generator is performed to evaluate the effectiveness before a fully implantable pulse generator (IPG) is placed in the subcutaneous tissue and connected to the electrodes as the power source for the stimulation in case of therapeutic success. There is no general definition of a positive test trial however a reduction in pain of 50% or more on the visual analog scale (VAS) is most often regarded as a hallmark criterion. Furthermore, reduction in oral pain medication or increase in quality of life can be factors to favor implantation of a permanent system.
Peripheral nerve field stimulation is certified for the use in chronic low back pain8 and has been used for localized chronic pain syndromes (e.g. post-herniorrhaphy pain). It is also used as occipital nerve stimulation (ONS) to treat chronic migraine and cluster headaches9. Several non-randomized studies have shown the use of sPNFS in the trigeminal dermatomes for chronic and neuropathic intractable pain of different origins (classical TN, atypical TN, post-herpetic trigeminal neuropathy, MS associated trigeminal neuropathy, persistent idiopathic facial pain)10,11,12.
Subcutaneous trigeminal nerve field stimulation (sTNFS) is easy and fast to perform. Contrary to DBS or MCS, sTNFS can be performed as an outpatient procedure (if reimbursed). There is no risk of intracranial or epidural bleeding. Seizures do not occur. Trial stimulation is performed in an ambulatory setting so that the patient can assess the stimulation effect while performing his everyday routine rather than being bound to a hospital bed. No extensive intra- or preoperative imaging is necessary to determine the correct position of the electrodes. sTNFS can be considered as a therapeutic option to modulate pain perception and processing before applying a percutaneous destructive procedure or as a less invasive type of neuromodulation before thinking about MCS or DBS in patients with neuropathic or central pain.
Protocol
NOTE: All procedures are performed as individual healing attempts ("Individueller Heilversuch"). And comply with the local ethics board (Ethikkommission Heidelberg) as well as national laws regarding individual healing attempts. Patients are extensively informed by the treating physician about the nature of the therapy, the procedures, the risks and benefits. All patients give written informed consent before beginning with the procedure. Individual healing attempts need the approval for reimbursement by the patient's health care service. This has to be obtained by the treating physician before scheduling the procedures.
1. Indication
- Make a diagnosis of chronic, treatment resistant, trigeminal nociceptive and/or neuropathic pain in one or more unilateral trigeminal branches.
- Include individuals who fit the following criteria: duration of pain of at least 6 months, and two or more failed attempts of standard medical and/or surgical therapy.
- Document information on the number and duration of daily attacks as well as the type and dose of pain medication (for both permanent and paroxysmal pain). Assess the quality of life with the SF-36 questionnaire by asking the patient to rate his or her current state.
NOTE: SF-36 is a questionnaire that consists of eight domains regarding quality of life (e.g. vitality, physical pain) to be rated on a scale between 0 and 100. - Exclude individuals with any major psychiatric disease (e.g. depression, schizophrenia), medical contraindication, severe medical conditions for surgery and general anesthesia, allergies to titanium or local anesthesia reagents (e.g. Mepivacain).
2. Trial Electrode Placement
- Place the patient in supine position and turn his head to the contralateral side of the pain.
- Thoroughly disinfect the facial area with a non-colored skin disinfection agent.
- Apply sterile drapes around the surgical field to minimize the risk of contamination and infection.
- Mark the painful area according to the patient's information with a sterile pen to plan the electrode position and position of the skin puncture.
- Plan the skin puncture no further away than 9 cm (length of the Tuhoy cannula) from the medial border of the painful area.
- For the first trigeminal branch, choose a position to puncture the skin on the lateral side of the forehead roughly 10 cm lateral and 1 cm above the medial border of the eyebrow.
- For the second trigeminal branch, choose a position roughly 1 cm anterior of the tragus.
- For the third trigeminal branch, choose a position that is located roughly 1 cm anterior and 4 cm below the tragus to perform the skin puncture.
- Do not perform a skin puncture 2 or more cm anterior of the tragus to spare facial nerve fibers from injury.
- Mark the desired direction of the implanted electrode with a sterile surgical pen for guidance.
- Inject 1 mL of a local anesthetic (e.g. 1% Mepivacain) with a 20 G cannula into the subcutaneous tissue at each site of the planned skin puncture and wait several minutes for the local anesthetic effect. Perception of pain is absent, however pressure and movement are still perceived.
- Perform the skin puncture with a 14 G Tuhoy needle at the previously marked position. Place the tip of the Tuhoy cannula roughly 0.5 cm below the skin surface to stay within the subcutaneous tissue.
- Withdraw the needle and repeat step 2.5 in case the patient feels any pain at the site of the skin puncture.
- Push the Tuhoy cannula gently through the subcutaneous tissue in the previously marked direction and aim for the medial border of the painful area.
- For the first trigeminal branch, aim towards midline parallel to the eyebrow. For the second trigeminal branch, aim towards the wing of the nose. For the third trigeminal branch, aim towards the chin.
- Make sure to maintain a depth of 0.5 cm and turn the sharp tip of the Tuhoy needle away from the skin to prevent any unintended skin perforation.
- Slightly bend the Tuhoy cannula manually to take the curvature of the skull into account if needed.
- Remove the Tuhoy cannula's stylet and insert the test electrode into the Tuhoy needle. A soft resistance is detected once the electrode reaches the end of the Tuhoy needle.
NOTE: The electrode is 60 cm long and has a diameter of 1.3 mm. Eight contacts for stimulation (each 3 mm long) are arranged in a row with a 6 mm distance in between contacts. The electrode is stabilized by an internal removable stylet. - Remove the Tuhoy cannula while keeping the electrode in position by gentle pressure towards the medial border of the painful area.
- Pull out the electrode's stylet for about 5 cm and insert the contacts into the port of the screening cable connected to the external neurostimulator.
- Repeat steps 2.6-2.10 for each additional electrode.
- Start test stimulation. Inform the patient that once activated a tingling sensation (paresthesia) in the painful area will be perceived.
- Use the physician programmer to activate stimulation.
- Apply bipolar stimulation with alternating anodes and cathodes on the contacts (e.g. 1+, 2-, 3+, 4-, 5+, 6-, 7+, 8-) with a frequency of 30-40Hz and a pulse width of 120-180 µs.
- Increase the stimulation amplitude until the patient can easily perceive the stimulation without being painful.
NOTE: Patients usually report perception of stimulation at amplitude of 0.5 to 2 V.- Watch for signs of direct muscle stimulation like ptosis or facial muscle contractions indicating that the electrode is too deeply implanted.
- Ask the patient what percentage of the painful area is covered by paresthesia. Try to achieve an at least 80% paresthesia coverage.
- Increase the stimulation amplitude and/or pulse width with the physician programmer to enlarge the field of stimulation.
- In case of direct muscle stimulation and/or insufficient paresthesia coverage, stop stimulation, disconnect the electrode from the screening cable, remove the electrode and repeat steps 2.6-2.13.
- Stop stimulation, disconnect the electrode from the screening cable and fully remove the electrode's stylet while keeping the electrode in place with forceps.
- Use the fixation device with the applicator to keep the electrode in place at the site of the skin puncture. Suture it to the skin using a non-absorbable 3-0 silk suture.
- Move the fixation device with the applicator over the distal end of the electrode all the way until it touches the skin surface. Push the lever to apply the fixation piece to the electrode. Remove the applicator.
- Suture the electrode with the fixation device to the patient's skin with two single stitches.
- Apply sterile draping at the site of the skin puncture.
- Reconnect the electrode to the screening cable.
3. Stimulation Trial and Assessment of Therapy
- Program the stimulation regimen.
NOTE: Active contacts, stimulation frequency, pulse width and amplitude are adjusted for optimal pain relief. Stimulation regimens will differ among patients. However, a bipolar stimulation (alternating cathodes and anodes in the electrodes), and a low frequency stimulation (30-40 Hz) are common in most patients. - Instruct the patient to use the handheld patient controller to turn stimulation on and off and to increase or decrease stimulation.
- To switch stimulation on or off and to change stimulation amplitude, activate the handheld patient controller by pushing the on/off button. Place the handheld patient controller on the external pulse generator and press the black "communicate" button on the side of the patient controller.
- Press the grey "stimulation off" button on the side of the patient controller to turn stimulation off and the white "stimulation on" button to turn stimulation on.
- Press the "+" and "-"button on the front of the patient controller to increase or decrease the stimulation amplitude.
NOTE: Information on stimulation amplitude, stimulation status and battery capacity are provided on the patient controller display. - Ask the patient to continuously stimulate. Instruct to switch the stimulation off for 1 h per day to compare the pain with and without stimulation.
- Discharge the patient for a 12 day ambulatory stimulation trial.
- Assess the effect of the stimulation at the outpatient clinic.
- Ask the patient to rate the pain with and without stimulation with a number between 0 and 10 on the VAS
NOTE: A pain reduction of at least 50% on the visual analogue scale (VAS) is regarded as successful trial stimulation. The VAS is a numerical rating scale that ranges from 0 "no pain" to 10 "most pain imaginable" and is subjective to the patient's assessment. Further measures for success are: reduction of attack frequency of 50% or more, reduction of medication and increase in quality of life. Compare the data with the preoperative status.
- Ask the patient to rate the pain with and without stimulation with a number between 0 and 10 on the VAS
- Take A/P (antero-posterior) and lateral x-rays of the skull to document the position of the electrodes for the second procedure14.
- Remove the draping, cut the sutures and remove the test electrodes. Apply new draping after disinfection and inspection of the site of the skin puncture.
- In case of successful trial stimulation, schedule an appointment for a procedure to implant electrodes and an internal pulse generator (IPG).
NOTE: Schedule the second surgery 4-6 weeks after the trial electrodes are removed to enable good wound healing, to minimize the risk of infection and to give the patient time to reflect on the amount of pain reduction during the trial stimulation. - Document the effective stimulation regimen during the trial stimulation for programming the IPG after the second surgery.
- Connect the physician programmer's antenna with the external pulse generator
- Choose the "connect" option on the programmer's display
- Go to the "Stimulation Settings" section and document the patient's stimulation regimen in the file.
4. Implantation of Permanent Electrodes and IPG
- Place the patient in a supine position under general anesthesia. Turn the head to the contralateral side of the pain. Place a pillow under the ipsilateral shoulder to expose the clavicle.
- Administer intravenous single shot antibiotics (e.g. 2 g cephazoline) 20 min before the start of the procedure.
- Shave the area around the ear of the painful side of the face. Remove any loose hair. If necessary, tape away the surrounding hair to prevent them from moving into the surgical field.
- Thoroughly disinfect the surgical field from the facial area, around the ear down to the clavicular area.
- Mark the desired position of the permanent electrodes using the x-rays obtained during the outpatient appointment and the marks of the previous skin punctures for guidance.
- Apply sterile draping around the entire surgical field.
- Perform the skin puncture with a 14 G Tuhoy cannula and implant the permanent electrodes as previously described for the first trial procedure.
NOTE: Size and length of the electrodes are identical to the trial electrodes (length 60 cm, diameter 1.3 mm, 8 contacts). - Make a 1 cm long vertical incision in the supraauricular area and form a small subcutaneous pocket there.
- Insert the Tuhoy cannula to subcutaneously tunnel from the supraauricular incision to the sites of the skin puncture. Remove the Tuhoy cannula's and the electrode's stylets and insert the distal end of the electrode into the cannula.
NOTE: The third trigeminal branch requires the length of two Tuhoy cannulas and an additional small skin incision in the preauricular area to fully cover the distance.- Remove the Tuhoy cannula while keeping the electrode in place with forceps.
- Use a 3-0 non-absorbable silk suture to suture the electrode to the muscle fascia to prevent electrode dislocation.
- In case the patient wears glasses, fix the electrodes at a position that is located above the frame of the glasses to prevent local pain and skin erosion.
- Perform a 6 cm long infraclavicular incision and manually form a subcutaneous pocket to house the IPG. Use a bipolar electrical forceps to coagulate any bleeding vessels.
- Insert a tunneling spear in the infraclavicular incision and subcutaneously tunnel behind the ear towards the supraauricular incision.
- Make a small retroauricular incision for the spear to exit the skin. Then use a second spear to tunnel from the supraauricular to the retroauricular incision.
- Remove the spears' stylets and insert the electrodes until they are buried in the subcutaneous tissue without any loops or kinks.
- Remove the spear by pulling it out from the infraclavicular incision while keeping the electrodes in place with a forceps.
- Pay attention to not penetrate the skin with the tunneling spear (especially in patients that have previously undergone surgery for microvascular decompression as they have a retroauricular scar).
- Connect the electrodes to the IPG and secure them with torque screws.
- Suture the IPG to the pectoralis muscle fascia with a non-absorbable silk suture (3-0) to prevent IPG dislocation.
- Check the system impedance to detect any faulty connection or damaged electrode contacts.
- Place the antenna of the Physician Programmer in a sterile drape and position it over the IPG. Connect the programmer with the IPG and go to the "check electrode impedance" section.
NOTE: Low impedances under 250 Ohm indicate open circuits. High impedances over 500 OHM indicate insufficient connection of the electrode to the IPG or electrode breakage.
- Perform skin closure with subcutaneous absorbable 3-0 sutures and non-absorbable 3-0 cutaneous sutures in the facial area and absorbable intracutaneous sutures at the site of the IPG.
- Disinfect all wounds, clean the surgical field with saline and apply sterile draping.
5. Postoperative Care
NOTE: The patient is transferred to the ward to be observed overnight and is given oral analgesic medication.
- Program the IPG using the stimulation regimen of the trial stimulation (see 3.8).
- Place the Physician Programmer's antenna on the skin over the IPG and choose the "connect" option to communicate with the neurostimulator.
- Insert the stimulation regimen documented at the end of the trial stimulation in the "stimulation settings" section.
- Adjust the stimulation settings according to the patient's statements regarding the paresthesia coverage. Increase amplitude and/or pulse width to achieve a wider field of stimulation. Decrease amplitude and/or pulse width in case of painful stimulation of direct muscle stimulation.
- Provide the patient with a personal patient controller as during the trial stimulation to enable him or her to switch stimulation on or off or to change the stimulation amplitude.
- If a rechargeable IPG is implanted, instruct the patients on how to check the battery capacity with their handheld device and how to perform the recharging procedure.
NOTE: Patients receive oral prophylactic postoperative antibiotics (e.g. 960 mg trimethoprime sulfamethoxazole twice daily) for 5 days.
- Discharge the patient on the day after surgery.
- Remove sutures seven days after the surgery in the outpatient clinic.
- Make follow-up appointments 4 and 12 weeks after surgery to assess the stimulation effect and to change stimulation settings if needed.
Representative Results
As subcutaneous trigeminal nerve field stimulation (sTNFS) is not a standard treatment and the number of patients that can potentially benefit from it is rather small compared to other diseases, there are only smaller case series that present results of sTNFS. In one series, 10 patients underwent test stimulation for sTNFS. Eight of the patients responded to the therapy and received permanent implantation of electrodes and an IPG11. The patients suffered from trigeminal neuralgia, trigeminal neuropathy associated with multiple sclerosis, post-herpetic trigeminal neuropathy, radiogenic trigeminal neuropathy and persistent idiopathic facial pain (Table 1). Pain was reduced from 9.3 point to 0.75 points on the VAS after 11.3 months of follow-up.
In another recently published series, 8 patients were tested with sTNFS (Figure 1). Six of the 8 patients proceeded to permanent implantation10. The patients suffered from trigeminal neuralgia with and without concomitant persistent facial pain and post-herpetic trigeminal neuropathy. Pain according to VAS was reduced from 8.5 to 1.4 points after a mean follow-up of 15.2 months. This series is also the first to describe a 73% reduction in the mean number of painful daily attacks. All but one of the patients was able to reduce or even stop all pain medication.
We provide an updated chart of all patients with permanent implantations treated at our department in Table 2. We were able to achieve a mean reduction of 6.8 VAS points (-79%; mean VAS preOP: 8.6, mean VAS postOP: 1.8) and a mean reduction in the number of daily attacks of 12.2 (-75, 3%; mean number of attacks preOP: 16.2, mean number of attacks postop: 4.0). reduction of pain medication was possible in 72.7% of patients.
The largest series published so far is comprised of 35 patients that were tested with 15 patients that received permanent implantation. Average pain reduction was 73% over a follow-up of 15 months12. However, in this series patients were treated also for conditions that do not affect the trigeminal nerve as such like temporomandibular joint (TMJ) disorders and general "headaches" that are not further specified.
In a series of 60 implanted patients a combination of subcutaneous supra- and infraorbital electrodes with occipital ones is also described as a treatment for chronic headache disorders13.
The surgical procedure is described similarly in all series however not all authors report on the duration between trials stimulation and permanent implantation.
We believe that a 4-6-week interval is crucial to reduce the number of false-positive results at the end of the test trial when patients overestimate the therapeutic effect. There is not a single parameter for outcome in pain treatment. VAS is a basic tool to subjectively quantify pain intensity. Documentation of the number of daily attacks, the amount of pain medication can help to assess outcome.
Although constant and paroxysmal pain can be both reduced by sTNFS, we observe a trend that patients with a strong neuropathic and constant pain component such as in post-herpetic trigeminal neuropathy are the most satisfied with the therapy. We lack a proper explanation for this observation as the exact mechanism of action of sTNFS is still unclear.
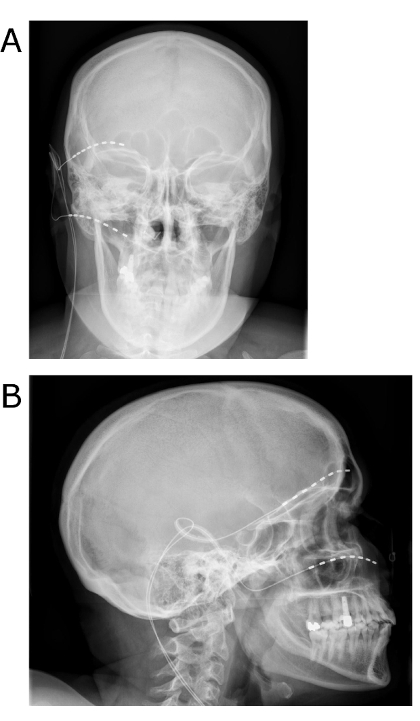
Figure 1: Postoperative x-rays after sTNFS. The patient underwent first and second trigeminal branch sTNFS for refractory trigeminal neuralgia A/P view (a) and lateral view (b). Please click here to view a larger version of this figure.
| Possible indications for sTNFS |
| trigeminal neuralgia |
| post-herpetic trigeminal neuropathy |
| multiple sclerosis associated trigeminal neuropathy |
| radiogenic triogeminal neuropathy |
| persistent idiopathic facial pain |
Table 1: Possible indications for sTNFS as reported in the literature. In all cases the pain should be chronic and be refractory to standard treatment before applying sTNFS.
| Effects of sTNFS | ||||||||
| # | age/sex | Disorder | Affected Branches | VAS preOP | VAS last Follow-Up | Daily attacks preOP | Daily attacks last Follow-Up | Redution of pain medication |
| 1 | 27/f | Postherpertic Neuropathy | V1 & V2 , right | 8 out of 10 | 2 out of 10 | 10 | 2 | yes |
| 2 | 34/f | Classical Trigeminal Neuralgia | V1 & V2, left | 10 out of 10 | 2 out of 10 | 3 | 1 | yes |
| 3 | 25/f | Classical Trigeminal Neuralgia | V1 & V2 , right | 8 out of 10 | 1 out of 10 | 30 | 2 | yes |
| 4 | 77/m | Classical trigeminal Neuralgia | V1 & V2, right | 10 out of 10 | 1 out of 10 | 50 | 2 | no |
| 5 | 81/f | Postherpertic Neuropathy | V1, right | 8 out of 10 | 1 out of 10 | 20 | 10 | yes |
| 6 | 80/f | Classical Trigeminal Neuralgia | V1 & V2 , right | 8 out of 10 | 1 out of 10 | 10 | 1 | yes |
| 7 | 52/m | Classical Trigeminal Neuralgia | V2 & V3, right | 10 out of 10 | 5 out of 10 | 10 | 2 | no |
| 8 | 66/f | MS associated Neuropathy | V2 & V3, left | 8 out of 10 | 1 out of 10 | 15 | 1 | yes |
| 9 | 78/f | Postherpetic Neuropathy | V1, right | 5 out of 10 | 2 out of 10 | 5 | 1 | no |
| 10 | 60/f | MS associated Neuropathy | V2 & V3, right | 10 out of 10 | 1 out of 10 | 10 | 2 | yes |
| 11 | 38/m | Classical Trigeminal Neuralgia | V2 & V3, right | 10 out of 10 | 3 out of 10 | 15 | 2 | yes |
Table 2: Results of sTNFS on reduction of pain intensity and attack frequency for different etiologies of trigeminal pain.
Discussion
With subcutaneous trigeminal nerve field stimulation (sTNFS), we present a surgical technique to perform minimally invasive neuromodulation for chronic refractory pain of the trigeminal nerve of different etiologies.
To reduce complications thorough disinfection of the entire surgical field is vital. Any unnecessary skin perforation can increase the risk of device infection with the consecutive loss of the system. Physicians should always pay attention to the implantation depth of the electrodes as they can erode the skin when implanted closer than 0.5 cm to the skin surface. Securing the electrodes with a fixation device should be thoroughly performed as small electrode dislocations can result in a significant loss of paresthesia coverage.
Compared to competing techniques such as MCS or DBS, it does not require specialized radiological planning such as MRIs in case of DBS or intraoperative electrophysiological monitoring in case of MCS. Electrodes can be correctly placed by communicating with the patient awake during the test stimulation procedure. Simple and inexpensive skull x-rays can be used to document the final electrode position.
The published results suggest that during the documented follow-up there is no wearing-off effect of stimulation so far. Interestingly in a DBS series only 70% of patients had their systems implants after 6 months15. At the end of the follow-up this number went down as far as 46% of patients with a benefit from DBS for neuropathic pain.
Although we have not observed this effect so far, it would not be a surprise if a certain percentage of patients will experience lower efficacy of therapy after some time. We have observed the fact that a patient who was very pleased with the effect after test stimulation, was almost impossible to satisfy with the permanently implanted electrodes although the positioning was identical. Whether additional psychological aspects come into play here has to be further evaluated.
The rate of pain reduction by sTNFS in the small published series10,11,12 varies from 73-92% which is an excellent result. However, documented follow-up is shorter compared to larger series of MCS16. Here 43% of patients with trigeminal neuropathic pain were responders with an at least 50% reduction of pain after a mean of 36 months of follow-up.
In our own published series10 we were the first ones to document a reduction in the frequency of daily attacks with sTNFS. As most of the patients report certain triggers such as talking or eating, a reduced in the number of attacks can result in better quality of life, as basic daily activities are less likely to be affected by painful attacks. Prospective documentation of quality of life (e.g. with the SF-36 questionnaire) can help to quantify this effect. sTNFS is not the only type of neuromodulation of the trigeminal nerve. Direct stimulation of the trigeminal ganglion was developed in the 1980s and performed in selected cases. Here an electrode was placed at the foramen ovale similarly to cannula placement in percutaneous destructive techniques. A response rate of 52% was published; however, the rate of dislocated electrodes with the need of surgical revision was as high as 30%17.
Reported complications and side effects of sTNFS are mostly minor and include all types of hardware malfunction (electrode breakage, electrode or IPG dislocation)18. In our series one wound infection with the consecutive need to remove the entire system temporarily occurred. Compared to potential complications of MCS or DBS (seizures, intracranial bleeding) the ones of sTNFS can be regarded as minor.
sTNFS and other means of neuromodulation should not be applied when the patients report alternating sites of the pain and bilateral facial pain as these rarely have a somatic origin that can be targeted with electrical stimulation. Furthermore, bilateral electrode implantation requires extensive subcutaneous tunneling across the scalp and is associated with a high number of electrode dislocations. Like all neuromodulation therapies the hardware is rather expensive and creates costs that are several times higher than those of a percutaneous destructive procedure (with comparable results19) that is also covered by the health care system in most countries. Although the implanted components are granted MRI conditionality when used as a system for epidural spinal cord stimulation, this is not applicable in the case of subcutaneous stimulation.
All reported series on sTNFS are retrospective and therefore biased to a certain degree. A prospective randomized controlled trial is necessary to properly assess the effect of this technique. The use of sTNFS in trigeminoautonomic cephalgias such as Cluster Headache is also tempting as this family of headaches affects the first trigeminal branch only.
Pain always has a subjective component that can vary among individuals. One should note that the outcome measures for sTNFS or in fact any pain treatments rely on the patient's subjective statements or behavior without proper ways to objectify them. Therefore, patients who can precisely describe the location perception and quality of pain tend to be able to also properly assess the effect during the trial stimulation. Quantitative sensory testing (QST) might be a future step to quantify changes in pain perception and thresholds with and without neuromodulation. Patient selection is critical for sTNFS and any type of neuromodulation for chronic and neuropathic facial pain. However, sTNFS is the neuromodulation technique that is the easiest and safest to perform as well as the cheapest to test and can be considered before more invasive neuromodulation procedures.
Divulgations
The authors have nothing to disclose.
Acknowledgements
This work was in part supported by the Collaborative Research Center 1158 (SFB1158 From nociception to chronic pain: Structure-Function properties of neural pathways and their reorganization), funded by the DFG (Deutsche Forschungsgemeinschaft).
Materials
| myStim Patient Programmer | Medtronic | 97740 | enables the patient to turn off and on stimulation |
| Prime Advanced | Medtronic | 97702 | non-rechargeable IPG as powersource for stimulation |
| Restore Ultra | Medtronic | 97712 | rechargeable IPG as powersource for stimulation |
| Charging System | Medtronic | 97754 | used by the patient to recharge the Restore Ultra IPG |
| N'Vision Programmer | Medtronic | 8840 | used by the physician to program the IPG and define stimulation parameters |
| External Neurostimulator | Medtronic | 37022 | external IPG as powersource for trial stimulation with externalized electrodes |
| Advanced Screening Cable | Medtronic | 355531 | connects externalized electrodes to the external neurostimulator during trial stimulation |
| Tunnelling Spear 60cm | Medtronic | 3655-60 | used to subcutaneously tunnel the permanent electrodes to an infraclavicular pocket that houses the IPG |
| Tunnelling Spear 38cm | Medtronic | 3655-38 | used to subcutaneously tunnel the permanent electrodes to an infraclavicular pocket that houses the IPG |
| Tuhoy Cannula | Medtronic | 3550-32 | 14 gauge Epidural Tuhoy cannula (length 9cm) to subcutaneously implant the electrodes |
| InjexFixation Device | Medtronic | 97791 / 97792 | used to fixate the electrodes on the skin or on the muscle fascia |
| Octad Compact | Medtronic | 3878-60 | permanent electrode (length 60cm) implanted in the subcutaneous tissue with 8 contacts |
| Vectris Trial Lead | Medtronic | 977D260 | externalized electrode (length 60cm) used during the stimulation trial |
| Ethilon*II 3-0 | Ethicon | EH7933H | non-absorbable suture for skin closure |
| Seide 2-0 | Resorba | 40221 | non-absorbable silk suture to fixate electrodes and IPG |
| Resolon DS21 | Resorba | 881413 | absorbable suture for subcutaneous wound closure |
| Feather disposable scalpel | Feather | 5205052 | single use scalpel for skin incision and suture cutting |
| Scandicain 1% | Astra Zeneca | 23186 | 1% Mepivacain solution for local anesthesia |
| Cosmopor E steril 10×6 | Hartmann | 900871 | Sterile draping for IPG wound |
| Cosmopor E steril 7,2×5 | Hartmann | 900870 | Sterile draping for skin punctures and small incisions |
| Foliodrape Comfort 50×50 | Hartmann | 252302 | Sterile draping for the surgical field |
| Cephazolin | Fresenius | 6062403.00.00 | Single shot perioperative antibiotic |
| Kepinol forte 800mg/160mg | Dr. R. Pfleger Chemische Fabrik | 2485177 | Postoperative prophylactic oral antibiotic |
| Poly-Alcohol | Antiseptica | UN1219 | Coloured skin disinfectant used during the permanent implantation |
| Cutasept F | Bode | 976800 | Un-Coloured skin disinfectant used during the trial implantation |
References
- Sandel, T., Eide, P. K. Long-term results of microvascular decompression for trigeminal neuralgia and hemifacial spasm according to preoperative symptomatology. Acta Neurochir. (Wien). 155 (9), 1681-1692 (2013).
- Montanto, N., Papacci, F., Cioni, B., Di Bonaventura, R., Meglio, M. What is the best treatment of drug-resistant trigeminal neuralgia in patients affected by multiple sclerosis? A literature analysis of surgical procedures. Clin Neurol Neurosurg. 115 (5), 567-572 (2013).
- Régis, J., et al. Radiosurgery for trigeminal neuralgia and epilepsy. Neurosurg Clin N Am. 10 (2), 359-377 (1999).
- Liem, L., Mekhail, N. Management of Post-Herniorraphy Chronic Neuropathic Groin Pain: A Role For Dorsal Root Ganglion Stimulation. Pain Pract. 16 (7), 915-923 (2016).
- Stadler, J. A., Ellens, D. J., Rosenow, J. M. Deep brain stimulation and motor cortical stimulation for neuropathic pain. Curr Pain Headache Rep. 15 (1), 57-62 (2011).
- Petersen, E. A., Slavin, K. V. Peripheral nerve/field stimulation for chronic pain. Neurosurg Clin N Am. 25 (4), 789-797 (2014).
- Slavin, K. Peripheral Nerve stimulation for Neuropathic Pain. Neurotherapeutics. 5 (1), 100-106 (2008).
- Kloimstein, H., et al. Peripheral Nerve Field stimulation (PNFS) in chronic low back pain: a prospective multicenter study. Neuromodulation. 17 (2), 180-187 (2014).
- Young, W. B., Silberstein, S. D. Occipital Nerve stimulation for primary headaches. J Neurosurg Sci. 56 (4), 307-312 (2012).
- Jakobs, M., Unterberg, A., Treede, R. D., Schuh-Hofer, S., Ahmadi, R. Subcutaneous trigeminal nerve field stimulation for refractory trigeminal pain: a cohort analysis. Acta Neurochir. (Wien). 158 (9), 1767-1774 (2016).
- Klein, J., Sandi-Kahun, S., Schackert, G., Juratli, T. A. Peripheral nerve field stimulation for trigeminal neuralgia, trigeminal neuropathic pain, and persistent idiopathic facial pain. Cephalalgia. 36 (58), 445-453 (2016).
- Ellis, J. A., Meija Munne, J. C., Winfree, C. J. Trigeminal branch stimulation for the treatment of intractable craniofacial pain. J Neurosurg. 123 (1), 283-288 (2015).
- Verrills, P., Rose, R., Mitchell, B., Vivian, D., Barnard, A. Peripheral nerve field stimulation for chronic headache: 60 cases and long-term follow-up. Neuromodulation. 17 (1), 54-59 (2014).
- Slotty, P. J., Bara, G., Vesper, J. The surgical technique of occipital nerve stimulation. Acta Neurochir. (Wien). 157 (1), 105-108 (2015).
- Boccard, S. G., Pereira, E. A., Moir, L., Aziz, T. Z., Green, A. L. Long-term outcomes of deep brain stimulation for neuropathic pain. Neurosurgery. 72 (2), 221-230 (2013).
- Rasche, D., Ruppolt, M., Stippich, C., Unterberg, A., Tronnier, V. M. Motor cortex stimulation for long-term relief of chronic neuropathic pain: a 10 year experience. Pain. (1-2), 43-52 (2006).
- Merhkens, J. H., Steude, U. Chronic electrostimulation of the trigeminal ganglion in trigeminal neuropathy: current state and future prospects. Acta Neurochir Suppl. 97 (Pt 2), 91-97 (2007).
- Slavin, K. V., Colpan, M. E., Munawar, N., Wess, C., Nersesyan, H. Trigeminal an occipital peripheral nerve stimulation for craniofacial pain: a single-institution experience and review of the literature. Neurosurg Focus. 21 (6), E5 (2006).
- Cheng, J. S., Lim, D. A., Chang, E. F., Barbaro, N. M. A Review of percutaneous treatments for trigeminal neuralgia. Neurosurgery. 10, 25-33 (2014).

