Clinical Application of 24 G Cannula Needle and 3-0 Polypropylene Suture in Vas Deferens Exploration
Summary
This protocol presents the clinical application of a 24 G cannula and 3-0 polypropylene suture as a simple and effective method for the exploration of the vas deferens.
Abstract
The goal of this article is to present the application of a 24 G cannula and 3-0 polypropylene suture as a simple method for the exploration of the vas deferens. During the exploration of the vas deferens, a 24 G cannula needle was used to puncture it. The fluid in the smear confirmed the presence of sperm, to determine whether or not there was concomitant obstruction at the junction of the epididymis and the vas deferens. Then, a 3-0 polypropylene suture (this suture specification has the advantages of a smooth surface, robust quality, and can be passed through a 24 G cannula needle) was passed through the cannula needle to probe the location of the obstructed site. With this technique, exploration of the vas deferens could be more targeted and accurate.
Introduction
Microsurgical vasovasostomy (MVV) is a common treatment for vas deferens obstruction after herniorrhaphy in childhood1,2. The site of obstruction cannot be identified preoperatively, and it is not clear whether sperm are present in the vas deferens or not. This may lead to difficulty in selecting the incision and injury to the vas deferens during semi-open exploration, which decreases the success rate of anastomosis, prolongs the operation time, and increases the risk of abdominal exploration3,4.
Injury to the vas deferens in the inguinal canal is likely an after-effect of inguinal hernia surgery in childhood, which can usually be caused by ligation, incision, or overstretching1. The rate of azoospermia after herniorrhaphy in childhood is approximately 0.8%-2.0% in pediatric patients. However, in the infertile population, the rate of iatrogenic obstruction is significantly increased, with a history of vas deferens injury in 7.2% of andrological procedures2,3. Surgical exploration of the inguinal region is usually performed to look for vas deferens remnants for anastomosis4. In previous cases, the ruptured end of the vas deferens is usually not found during inguinal exploration, which leads to the termination of the operation and increases surgical trauma to the patient. Therefore, it is very important to use a simple method to determine the location of the obstruction to clarify the following surgical procedures.
In this study, a 24 G cannula was used to puncture the vas deferens to confirm the presence of sperm in it, and a 3-0 polypropylene suture was passed through the cannula to determine the location of the obstructed site. Based on this simple operation, we can determine the next surgical procedure. After practicing and summarizing the clinical operations, our specific surgical method is presented below.
Protocol
All methods described here were approved by the Ethics Committee of Union Hospital Tongji Medical College, Huazhong University of Science and Technology. We obtained the patient's consent to use his surgical footage as a video after the procedure.
1. Instruments for operation
- Ensure the availability of a surgical microscope system, microsurgical instrument, and microscopic bipolar electrocoagulation.
2. Preparation for operation
- Inclusion criteria
- Include all patients diagnosed with azoospermia who agree to undergo surgery. Have all female partners of the patients undergo gynecologic fertility testing
NOTE: In the presented study, patients underwent surgery at the hospital between June 2013 and July 2020. All female patients' partners' gynecologic fertility test results were normal. - Ensure normal serum levels of follicle-stimulating hormone and testosterone in all patients.
- Ensure that there are no genital malformations, hypertension, diabetes, hyperthyroidism, heart disease, pelvic trauma, abnormal psychological or mental disorders, or other serious preexisting diseases or conditions.
- Include all patients diagnosed with azoospermia who agree to undergo surgery. Have all female partners of the patients undergo gynecologic fertility testing
- Exclusion criteria
- Exclude patients with genital malformations, abnormal psychological or mental disorders, acute urinary tract infection or urinary tuberculosis, severe abdominal trauma or surgery, severe coagulation disorders, or other contraindications to anesthesia or laparoscopy.
- Perform an anesthesia risk assessment on patients prior to the surgery. Ask patients who have been taking aspirin to discontinue it.
- Mark the skin 15 cm around the perineum with a skin preparation knife to prepare for the surgery.
- Administer antibiotics to the patient via intravenous drip 30 min prior to surgery. Ideally, use cefoperazone sodium (2.0 g) together with 100 mL of 0.9% sodium chloride solution.
- Make sure that the patient is under general or intraspinal anesthesia.
3. Procedure
- Place the patient under general anesthesia with endotracheal intubation. Then, perform standard disinfection with 1% iodophor while the patient is in the supine position.
- Make a 3 cm incision along the mid-scrotal fold. Then, pinch one testicle and incise the flesh membrane to expose the testicular sheath and spermatic cord.
- Dissect the fascia between the vas deferens and the spermatic cord vessels. Separate along the space between the vas deferens vasculature and the vasculature of the spermatic cord with a vascular clamp. Secure the vas deferens with tissue forceps and prepare it for vesicocentesis.
- Insert a 24 G cannula needle obliquely 15° downward along the long axis of the vas deferens. Pull out the needle core after the obvious tactile breakthrough, and slide the soft trocar to the lumen.
- Inject 2 mL of 0.9% sodium chloride solution into the vas deferens using a 5 mL syringe connected to the 24 G cannula. If resistance is high, this confirms that there is an obstruction in the vas deferens.
- Take a sample of fluid from the syringe and give it to an examiner to examine it under the microscope for sperm.
- Advance the 3-0 polypropylene suture through the trocar. If there is resistance, it indicates obstruction. Measure the length of the suture to determine the site of obstruction.
4. Postoperative care
- Make the patient stay in the ICU for ~1-2 h postoperatively, until he fully regains consciousness.
- Send the patient back to the ward when he fully wakes up.
- Implant a catheter for 6-24 h.
- Lift the scrotum with underwear for 1 week.
Representative Results
There were 67 patients enrolled in the study. As shown in Table 1, the mean age of the patients was 28.8 ± 3.7 years (range: 23-45 years). The time since herniorrhaphy was 24.5 ± 3.2 years (range: 21-43 years). The female partners were 25.2 ± 3.2 years (range: 23-42 years) years old. A total of 11 (16.4%) patients had pain in the scrotum. Four patients (6.0%) were underweight (BMI < 18.5 kg/m2), 53 (79.1%) had normal weight (BMI 18.5-24.9 kg/m2), eight (11.9%) were overweight (BMI 25-29.9 kg/m2), and two (3.0%) were obese (BMI > 30 kg/m2) .
In our study, the sites of obstruction were classified into three groups. (1) The obstruction of the vas deferens is at the incision of the original hernia repair (>2 cm); (2) the obstruction of the vas deferens is 2 cm higher than the original incision; (3) the obstruction of the vas deferens is more than 5 cm from the upper edge of the original incision. Table 2 shows the location of vas deferens obstruction and the results according to the surgical method in the different subgroups. The smear showed that 25 cases (37.3%) had no sperm in the cannula fluid. Of these, three (12.0%) underwent bilateral VV surgery with the obstruction site in the original incision, and the patency rate was 33.3% (one of three). In total, 22 (88.0%) underwent assisted reproductive technology (ART), in which the obstruction of the vas deferens was 2 cm higher than the upper edge of the original incision. The smear detected sperm in the fluid of the cannula needle in 42 (62.7%) cases. Of these, 29 (69.0%) underwent bilateral VV surgery with the obstruction site in the original incision, and the patency rate was 79.3% (23 of 29). A total of 10 (23.0%) underwent laparoscopy-assisted (lapa)-VV, with the obstruction site 2 cm higher than the original incision, and the patency rate was 40% (four of 10). A further three (7.10%) underwent seminal vesiculoscopy (SV), in which the obstruction site was 5 cm higher than the original incision, and the patency rates was 33.3% (one of three).
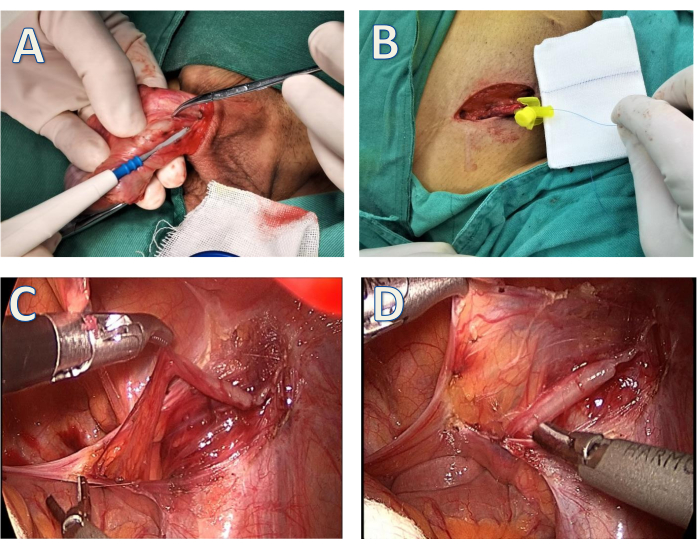
Figure 1: Schematic of the procedure. (A) The thickened vas deferens was separated. (B) A 3-0 polypropylene suture was passed through the cannula needle to probe the position of the obstructed site. (C) The vas deferens was identified beneath the peritoneum. (D) The vas deferens was mobilized with its blood supply off scar tissue. Please click here to view a larger version of this figure.
| Characteristics | N |
| Patient age, years | |
| Mean±SD | 28.8±3.7 |
| Range | 23-45 |
| Time since herniorrhaphy, years | |
| Mean±SD | 24.5±3.2 |
| Range | 21-43 |
| Female partner age, years | |
| Mean±SD | 25.2±3.2 |
| Range | 23-42 |
| With scrotal pain, n (%) | |
| Yes | 11(16.4%) |
| No | 56(83.6%) |
| BMI | |
| Underweight (<18.5 kg/m2) | 4(6.0%) |
| Normal (18.5-24.9 kg/m2) | 53(79.1%) |
| Overweight (25-29.9 kg/m2) | 8(11.9%) |
| Obese (≥30 kg/m2) | 2(3.0%) |
| BMI, body mass index. |
Table 1: Basic information of the patients. Abbreviation: BMI = body mass index. Data for this table is reprinted with permission from Wang et al.5
| Sperm exist in the vas deferens | Patients, n (%) | The site of obstruction | Patients, n (%) | Treatment (%) | Patency n (%) |
| No | 25(37.3) | < 2cm | 3(12.0) | MVE+MVV | 1(33.3) |
| >2cm | 22(88.0) | ART | – | ||
| Yes | 42(62.7) | <2cm | 29(69.0) | Bi-VV | 23(79.3) |
| >2cm | 10(23.8) | Lapa-VV | 4(40.0) | ||
| >5cm | 3(7.1) | SV | 1(33.3) |
Table 2: The site of vas deferens obstruction and the results based on operative manners in different subgroups. Abbreviations: MVE = microsurgical vasoepididymostomy; MVV = microsurgical vasovasostomy; Bi-VV = bilateral vasovasostomy; lapa-VV = laparoscopy-assisted vasovasostomy; SV = seminal vesiculoscopy; ART = assisted reproductive technology.
Discussion
As mentioned before, the location of the vas deferens stump cannot be determined at the inguinal incision, which requires exploration of the original inguinal incision. In this study, we can use this simple operation to determine the site of obstruction and make surgical decisions. If the site of obstruction is in the original incision, MVV can be considered. If the vas deferens injury is not found in the inguinal canal, we can use lapa-VV or SV.
When pasty fluid without sperm was found and the obstruction of the vas deferens was 2 cm higher than the original incision, the procedure was stopped and the incision was sutured. However, because of the long operation time, costly procedure, large surgical incision, and uncertain results of the combined lapa-VV-MVE operation, many patients might refuse to undergo this operation and opt for ART6.
Patients in whom natural pregnancy could not be achieved, mainly because of poor semen quality, considered intracytoplasmic sperm injection (ICSI) or artificial insemination as another option. Artificial insemination by the male or ICSI can be attempted more than once. Complications were recorded after 12 months7,8. Patients with long-term epididymal stasis may develop epididymal obstruction causing pasty vasal fluid without sperm9. The combination of MVV and MVE may be a potential therapeutic option in some patients10.
Consistent with open surgery, VV is a difficult inguinal operation after herniorrhaphy, and the site of obstruction cannot be identified preoperatively. Overexploration may result in injury to the testicular and vas deferens vessels, or the recurrence of hernia repair11. Surgery is difficult to perform, especially when the remnants of the vas deferens cannot be found. Therefore, intraoperative evaluation of the site of obstruction is very important.
In our study, there are several possibilities for exploration: if a smear reveals that there is no sperm in the cannula fluid, there may be a concomitant obstruction at the junction of the vas deferens and epididymis. If the obstruction of the vas deferens is 2 cm higher than the top of the original incision palpated by the polypropylene suture, consideration may be given to undergoing ART directly. If the obstruction site is in the original incision, MVE + MVV may be considered. If a smear demonstrates that sperm is present in the fluid of the cannula while the obstruction site with the 3-0 polypropylene suture is in the incision of the original hernia repair, the original inguinal incision can be examined directly. If a smear demonstrates that sperm is present in the cannula fluid while the 3-0 polypropylene suture is within 2 cm of the top of the original incision for evidence of obstruction, laparoscopy-assisted vas deferens exploration can be considered, and the proximal vas deferens can be pulled out of the external inguinal ring for anastomosis. If a smear demonstrates that sperm is present in the fluid of the cannula while the 3-0 polypropylene suture is more than 5 cm from the upper edge of the original incision, seminal vesicle dysplasia or ejaculatory duct obstruction may be present. In combination with preoperative semen volume and seminal vesicle magnetic resonance imaging (MRI), endoscopic examination of the seminal vesicle could be considered.
Simple surgery with a 24 G cannula and a 3-0 polypropylene suture results in little injury to the vas deferens, optimizes the surgical process, increases the intensity of surgical decision making, and provides a simple and effective method to maximize the patient's interests.
Divulgazioni
The authors have nothing to disclose.
Acknowledgements
We thank ZHZ for the conception and design of the study. JW and YPZ performed and supervised the operation. YH, YBX, SL contributed to data analysis. JW and WJL prepared the draft of the video. All authors participated in the revision of the manuscript. All authors read and approved the final manuscript.
Materials
| 0.9% sodium chloride solution | Guangdong Otsuka Pharmaceutical Co. LTD | 21M1204 | Inject into the vas deferens |
| 1% iodophor | Guangzhou Qingfeng Disinfection Products Co., LTD | Q/QFXD2 | Skin disinfection |
| 24G cannula needle | Suzhou Linhua Medical Instrument Co., LTD | 20193141896 | Size:24G, Type:Pen type, with wings, with injection port, Y type |
| 3-0 monofilament polypropylene | Covidien Medical Equipment international trading (Shanghai) Co., LTD | DOL2861y | Taper Point, Size 3-0, Blue, 36", Needle V-20, 1/2 Circle |
| 5 mL syringe | Kindly Medical, Shanghai | K20210826 | Inject 0.9% sodium chloride solution into the vas deferens |
| F16 Catheter | Guangzhou Weili Co., Ltd | 20190612 | Drainage of urine |
| micro haemostatic forceps | Shanghai Medical Instrument (Group) Co., LTD. | W40350 | Used in surgical procedures |
| micro scissors | Shanghai Medical Instrument (Group) Co., LTD. | WA1010 | Used in surgical procedures |
| micro tweezers | Shanghai Medical Instrument (Group) Co., LTD. | WA1020 | Used in surgical procedures |
| Olympus microscope | Olympus Corporation | Scipu001158 | 4×N.A.0.10 W.D.22.0mm 10×N.A.0.25 W.D.10.5mm 40×N.A.0.65 W.D.0.56mm 100×N.A.1.25 W.D.0.13mm |
| Operating microscope system | Carl Zeiss Co., Ltd | OPMI VARIO 700 |
Riferimenti
- Chen, X. F., et al. Clinical features and therapeutic strategies of obstructive azoospermia in patients treated by bilateral inguinal hernia repair in childhood. Asian Journal of Andrology. 16 (5), 745-748 (2014).
- Sparkman, R. S. Bilateral exploration in inguinal hernia in juvenile patients. Review and appraisal. Surgery. 51, 393-406 (1962).
- Pollak, R., Nyhus, L. M. Complications of groin hernia repair. The Surgical Clinics of North America. 63 (6), 1363-1371 (1983).
- Sheynkin, Y. R., Hendin, B. N., Schlegel, P. N., Goldstein, M. Microsurgical repair of iatrogenic injury to the vas deferens. The Journal of Urology. 159 (1), 139-141 (1998).
- Wang, J., et al. Treatment for Vas Deferens Obstruction Following Childhood Herniorrhaphy. Urology. 112 (1), 80-84 (2018).
- Smith, R. P., et al. The significance of sperm heads and tails within the vasal fluid during vasectomy reversal. Indian Journal of Urology. 30 (2), 164-168 (2014).
- Jungwirth, A., Diemer, T., Kopa, Z., Krausz, C., Tournaye, H. European Association of Urology guidelines on male infertility. 2017 edition. , 23-24 (2017).
- Bromage, S. J., Falconer, D. A., Lieberman, B. A., Sangar, V., Payne, S. R. Sperm retrieval rates in subgroups of primary azoospermic males. European Urology. 51 (2), 539-540 (2007).
- Du, J., et al. Differential diagnosis of azoospermia and etiologic classification of obstructive azoospermia: role of scrotal and transrectal US. Radiology. 256 (2), 493-503 (2010).
- Pasqualotto, F. F., Pasqualotto, E. B., Agarwal, A., Thomas Jr, A. J. Results of microsurgical anastomosis in men with seminal tract obstruction due to inguinal herniorrhaphy. Revista do Hospital das Clinicas. 58 (6), 305-309 (2003).
- Shaeer, O. K. Z., Shaeer, K. Z. Laparoscopy-assisted pelvi-scrotal vasovasostomy. Andrologia. 36 (5), 311-314 (2004).

