Clinical Effects of Ultrasound-Guided Acupotomy in Knee Osteoarthritis Treatment
Summary
This paper introduces the operation method of ultrasound-guided acupotomy for knee osteoarthritis, which can reduce synovial thickness and improve knee joint function. It has the advantages of precise target, low treatment risk, few complications, and high safety.
Abstract
The protocol presented here demonstrates the operation method of ultrasound-guided acupotomy for knee osteoarthritis (KOA), including patient recruitment, preoperative preparation, manual operation, and postoperative care. The purpose of this protocol is to relieve pain and improve knee function in patients with KOA. A total of 60 patients with KOA admitted between June 2022 and June 2023 were treated with ultrasound-guided acupotomy. Pathological changes and knee function scores were compared before and after the treatment. After 1 week of treatment, the synovial thickness of the suprapatellar bursae was significantly lesser than before treatment (p < 0.05), the Hospital for Special Surgery Knee Score (HSS) was significantly higher than before treatment (p < 0.05), the Visual analogue scale (VAS) was significantly lower than those of the control group (p < 0.05) and Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) were significantly lower than those of the control group (p < 0.05). Therefore, ultrasound-guided acupotomy for the treatment of KOA can reduce synovial thickness, relieve pain, improve knee joint function, and have a remarkable curative effect.
Introduction
Knee osteoarthritis (KOA) is the most common degenerative disease of the knee joint, causing knee pain, bony enlargements, morning stiffness, knee activity limitations, and other symptoms. Knee pain and limited function are the primary factors affecting daily life and work in patients with KOA. Most people with KOA experience a partial or complete loss of the ability to work and self-care, which is the primary cause of chronic disability1. Epidemiological data2,3 show that the prevalence of KOA is positively correlated with age. With the aging Chinese population, the incidence of KOA is increasing every year. Globally, approximately 250 x 106 patients have osteoarthritis, and its incidence is increasing annually. By 2030, osteoarthritis will be one of the main causes of disability4, with approximately 85% of osteoarthritis cases of the knee5,6, which seriously affects the quality of life of patients and causes pain in their life and work, leading to a heavy economic burden to the country and individuals7,8. Therefore, finding safe and minimally invasive treatments for patients with KOA is an area of intense research in orthopedics.
The main treatments for KOA include conservative therapies like patient education, lifestyle adjustments, physical therapy, orthopedic aids and orthotics, and medication and surgery. The vast majority of intra-knee surgery is performed through arthroscopic surgery with little trauma and a low infection rate. However, arthroscopic surgery still has some traumatic effects. Patients with KOA often undergo surgery after conservative treatment has failed9.
Acupotomy is a less invasive surgery than arthroscopy. Acupotomy can be performed in conjunction with conservative treatment. The needle knife is generally about 10-15 cm long and 0.4-1.2 mm in diameter. The needle knife consists of three parts: handle, needle body, and blade. The blade is thin and sharp. Its width is equal to the diameter of the needle body. Traditional acupotomy refers to the treatment of tendon pain points by a surgeon under the condition that the internal tissue structure of the human body cannot be directly observed; the interventional treatment is carried out according to his/her own experience and knowledge of the local anatomical tissue, combined with the symptoms and tender points of the patient. Due to the high risk of the procedure, including damage to the surrounding soft tissues, nerves, and blood vessels, infection, uncertain effects, and the possibility of multiple procedures, the use of traditional acupotomy is quite limited. With the development of imaging technology, the use of visualization has become a developing trend in acupotomology10 and has broadened the clinical application of acupotomy. Ultrasound can be used to visualize muscle and fascial lesions in real-time, allowing complete identification of the relative anatomy and the lesions11,12, improving the accuracy and safety of acupotomy13. Currently, it is primarily used to treat joint pain in the neck, shoulder, waist, and leg14,15. Ultrasound-guided acupotomy has the advantages of being a precisely targeted therapy, low risk, few complications, and high safety. Therefore, this study evaluated ultrasound-guided acupotomy as a new therapeutic approach for KOA.
Protocol
All patients with KOA were evaluated in the outpatient Department of TCM Rehabilitation at Guangming Hospital of Shanghai Pudong New Area from June 2022 to June 2023 for a total of 60 cases. This study was approved by the ethics review committee at Guangming Hospital of Traditional Chinese Medicine of Shanghai Pudong New Area (Ethics number: GMEC-KY-2020034). Doctors informed patients and their families regarding the clinical significance, risks, and follow-up requirements of the study. Patients were included in the study after obtaining and signing informed consent either from the patients or their families. The surgeon was familiar with the anatomy of the knee joint and acupotomy treatment.
1. Patient recruitment
- Diagnostic criteria
- Use the following diagnostic criteria to diagnose knee osteoarthritis, according to the Chinese Society of Osteology's guidelines for the diagnosis and treatment of osteoarthritis (GDTO)16. Check the affected knee for pain within the last month, and if any two of the following four criteria exist, diagnose as knee osteoarthritis: (1) radiographs (standing or weight-bearing) showing joint space narrowing, joint margin osteophyte formation, subchondral osteosclerosis, or cystic change; (2) age ≥ 60 years; (3) morning stiffness of ≤ 30 min; (4) bone grinding sound during activity.
- Inclusion criteria
- Use the following inclusion criteria to enroll patients in this study: (1) conform to the diagnostic criteria of KOA; (2) age between 40-75 years; (3) body mass index ≤ 25 kg/m2; (4) no cognitive dysfunction; (5) no previous knee surgery or acupotomy within 1 month; (6) understands the relevant contents of the study in detail, and have good medical compliance and a high degree of cooperation; (7) agree and sign the informed consent.
- Exclusion criteria
- Use the following exclusion criteria to not include patients in this study: (1) pregnant and lactating women; (2) patients with infection and muscle necrosis or deep abscess at the treatment site (knee); (3) patients with a history of fainting with the use of needles; (4) patients with a severe meniscus tear, anterior or posterior cruciate ligament tear, medial or lateral collateral ligament injury; (5) patients with knee joint pain caused by neurological diseases; (6) patients with severe cardiovascular, liver, kidney or hematopoietic system disease; (7) patients receiving other treatment options; (8) lidocaine hydrochloride allergy; (9) patients who do not want to be followed up.
- Dropout criteria
- Use the following exit criteria to allow patient dropout in this study: (1) voluntary withdrawal by the patient; (2) occurrence of other complications.
2. Acupotomy treatment
- Preoperative preparation
- Material preparation (Figure 1): sterilize disposable medical plastic cups, forceps, absorbent cotton balls, self-adhesive dressing, ultrasonic instruments (portable color ultrasound system), sterile ultrasound coupler, sterile protective cover for probe, 40 mm small disposable sterile needle knife, marker pen, disposable medical mask, hygiene hat, type II skin disinfectant, disposable sterile towel, 2% lidocaine hydrochloride, sterile water for injection, 10 mL disposable sterile syringe, sterile needle for injection, and surgical rubber gloves.
- Operation site: Prepare a treatment room with air disinfectant capabilities.
- Check patient information: check all basic patient information like name, age, and treatment site. Explain the needle-knife therapy procedure, including the possible risks and benefits of treatment. Ensure that the patient understands needle-knife treatment and remains relaxed during the procedure.
- Patient position: Ask the patient to lie down in a supine position, with the affected knee joint fully exposed and a thin pillow placed under the affected knee joint to place the joint in a relaxed state. Abduct the contralateral knee slightly, providing more room for the surgeon.
- Positioning (Figure 2)
- Tenderness points positioning: Mark the point where significant pain occurred in the affected knee joint due to the operator's finger pressure, such as the peroneal collateral ligament and iliotibial band point, patellar lateral retinaculum point, quadriceps tendon and suprapatellar bursa point, patellar medial retinaculum point, tibial collateral ligament point, pes anserinus bursa point.
- Ultrasound positioning17: Use the ultrasound probe (frequency 8-15 MHz, depth 1-4 cm) to scan along the short and long axis of the quadriceps tendon, the long axis of the knee tibial collateral ligament, the long axis of the fibular collateral ligament of the knee, the long axis of the patellar tendon and the tenderness point. Mark the points of local thickening, reduced echo, and loss of lamellar structure in ultrasound on the body surface.
- Operative steps (Figure 3)
- Following aseptic procedures, wear masks, hats, and sterile gloves.
- Ask the surgical assistant to open a 5 mL 2% lidocaine and 5 mL sterile water vial. Place a 10 mL syringe, a 25G needle, and a 40 mm disposable small sterile needle knife into a sterile plastic cup.
- Ask the surgical assistant to use cotton balls and type II skin disinfectant to disinfect the 15 cm area around the marked point on the knee. Place a sterile towel so that the mark point is in the middle of the sterile towel.
- Extract 5 mL of 2% lidocaine and 5 mL of sterile water with a 10 mL syringe to prepare 10 mL of working 1% lidocaine solution. Replace the 22G needle with a 25G needle (using a thinner needle for pain control).
- Fit the sterile protective cover over the probe. Hold the ultrasound probe in the left hand and the syringe in the right hand. Extrude the sterile ultrasonic gel and apply it to the probe.
NOTE: The surgical assistant assists the surgeon with this. - Place the probe in the marked position. Confirm the target in the ultrasound image. Insert the syringe needle into the skin from the probe side so that the syringe needle and the target are in the same field of view. Make sure no blood returns upon aspiration. Inject each target with 1-2 mL of 1% lidocaine working solution.
- Hold the needle knife in the right hand. Insert the needle knife into the lidocaine injection site. The needle knife insertion direction is parallel to the direction of muscle and ligament fibers to avoid cutting muscle fibers and ligament fibers. Make sure the needle knife and the target are in the same field of view. Avoid touching blood vessels and nerves.
- Perform a longitudinal incision, stripping, and release the adhesion18. The patient will feel local soreness and pain, and the surgeon will feel resistance under the knife needle. Remove the knife needle when the surgeon feels a sense of looseness under the knife.
- Postoperative care (Figure 3)
- Press the injection site with a dry sterile cotton ball for 1 min. Cover the surgical area with a sterile self-adhesive dressing. Help the patient get dressed and leave the operating room.
- Ask the patient to sit quietly at the door of the operating room for approximately 15 min to avoid postoperative discomfort. Ask the patient to remove the dressing after 24 h and avoid contact with water for 3 days to avoid infection19.
- Perform ultrasound-guided acupotomy once a week for a total of three acupotomy treatments.
3. Follow up evaluation
- Parameters for evaluation10,11,12,13,14,15,16,17,18,19,20,21,22
- Use the synovial thickness of the suprapatellar bursae, the Visual analog scale (VAS), the Hospital for Special Surgery Knee Score (HSS), and Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) to assess the outcome. Take measurements before treatment and 1 week after the 3 treatments were completed.
- Ultrasound-based evaluation
- Use the ultrasound to measure the synovial membrane thickness of suprapatellar bursae.
- Press the Power button to turn on the ultrasound machine. Press the Patient button, click on New Patient, and enter the patient's name.
- Ask the patient to lie in a supine position. Place a thin pillow under the popliteal fossa of the affected knee joint to fully expose it.
- Use the head end of the probe to find the superior edge of the patella. Place the tail end on the quadriceps tendon. Adjust the direction of the probe. Make sure that the acoustic beam is made perpendicular to the tendon and located on the synovial membrane of the suprapatellar bursae.
- Press the Freeze button to save the ultrasound image. Press the Caliper button to test the synovial thickness of the suprapatellar bursa. Record the measurement results.
4. Statistical analysis
- Use a statistical analysis software. Express the measurement data as mean ± standard deviation (SD). Use a T-test to compare the differences before and after treatment. Consider p <0.05 as statistically significant.
Representative Results
During the study, one patient received additional other treatments (intra-articular steroid injection) due to increased pain. In one patient, the synovial thickness of the suprapatellar bursae could not be detected on ultrasonography. One patient developed swelling and subcutaneous stasis around the wound after treatment, which improved after ice application without affecting normal treatment and follow-up. Two patients terminated the experiment, and the remaining 58 patients were included in the final statistical analysis.
Baseline features
The participants comprised 27 men and 31 women. Patients ranged in age from 40 to 75 years, with an average age of 57.79 ± 11.33 years. The duration of the disease ranged from 1 to 36 months, with an average duration of 20.78 ± 9.88 months (Table 1).
The synovial thickness of the suprapatellar bursae and VAS and WOMAC scores decreased, and HSS increased after ultrasound-guided acupotomy.
Post-treatment evaluation
After 1 week of treatment, the synovial thickness of the suprapatellar bursae in the treatment group (4.02 ± 0.83) was thinner than that in the control group (5.04 ± 0.67; t =7.978, p < 0.05). After 1 week of treatment, the VAS of the treatment group (4.17 ± 2.07) was significantly lower than that of the control group (6.14 ± 1.80; t = 8.157, p < 0.05). After 1 week of treatment, the WOMAC in the treatment group (38.97 ± 14.28) was significantly lower than that in the control group (59.26 ± 17.32; t = 9.087, p < 0.05). After 1 week of treatment, HSS in the treatment group (73.19 ± 14.75) was significantly higher than that in the control group (56.47 ± 14.47; t = -8.904, p < 0.05; Table 2).
The figures shown here are from the representative case of a 65-year-old female who had recurrent pain in the left knee joint over the past 1 month. Her joint stiffness increased in the morning and was relieved after 10 min of waking. Radiographs of the left knee joint revealed a narrowing of the joint space. The patient met the diagnostic criteria for KOA and voluntarily participated in the study. After contraindications were ruled out, the patient was advised of the possible benefits and risks of ultrasound-guided acupotomy. The patient had a pretreatment VAS score of 7, a WOMAC score of 53, an HSS score of 56, and the synovial thickness of the suprapatellar bursae was 6.5 mm (Table 3 and Figure 3). After 1 week of ultrasound-guided acupotomy, the patient's VAS score was 3, WOMAC score was 40, HSS score was 76, and synovial thickness of the suprapatellar bursa was 3 mm (Table 3 and Figure 4), indicating that the patient's pain, knee function, and synovial thickness of the suprapatellar bursa improved after ultrasound-guided acupotomy.

Figure 1: Prepare materials. All the materials and equipment needed for this operation, including sterilize disposable medical plastic cups, forceps, absorbent cotton balls, self-adhesive dressing, ultrasonic instruments (portable color ultrasound system), sterile ultrasound coupler, sterile protective cover for probe, 40 mm small disposable sterile needle knife, marker pen, disposable medical mask, hygiene hat, type II skin disinfectant, disposable sterile towel, 2% lidocaine hydrochloride, sterile water for injection, 10 mL disposable sterile syringe, sterile needle for injection, and surgical rubber gloves. Please click here to view a larger version of this figure.
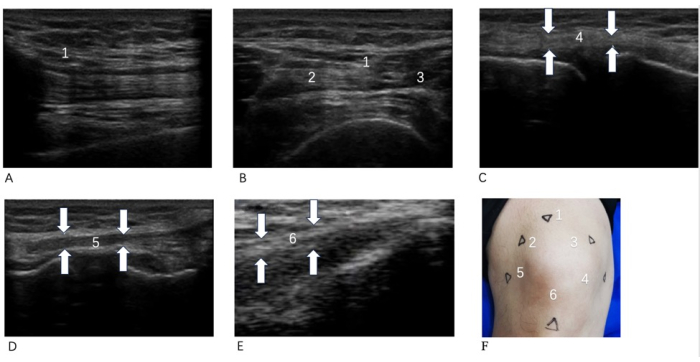
Figure 2: Therapeutic location map. (A) Quadriceps tendon long axis; (B) Quadriceps tendon short axis; (C) Knee tibial collateral ligament long axis; (D) Knee fibular collateral ligament long axis; (E) Patellar tendon long axis; (F) Body surface positioning. 1 Quadriceps tendon stop; 2 Quadriceps medial dilator; 3 Knee tibial collateral ligament; 4 Patellar tendons; 5 Fibular collateral ligaments of knee; 6 Quadriceps lateral dilator. The surface positioning points and ultrasound images of each positioning point for this operation. In (F), 1, 2, and 3 anchor points are in the quadriceps femoris; the long axis of the quadriceps femoris is shown in (A), and the short axis of the quadriceps femoris is shown in (B). Anchor point 4 was in the patellar tendon, corresponding to (C). Fixation point 5 was located in the collateral fibular ligament on the knee side, corresponding to (D). Point 6 is in the tibial collateral ligament on the knee side, corresponding to (E) Please click here to view a larger version of this figure.
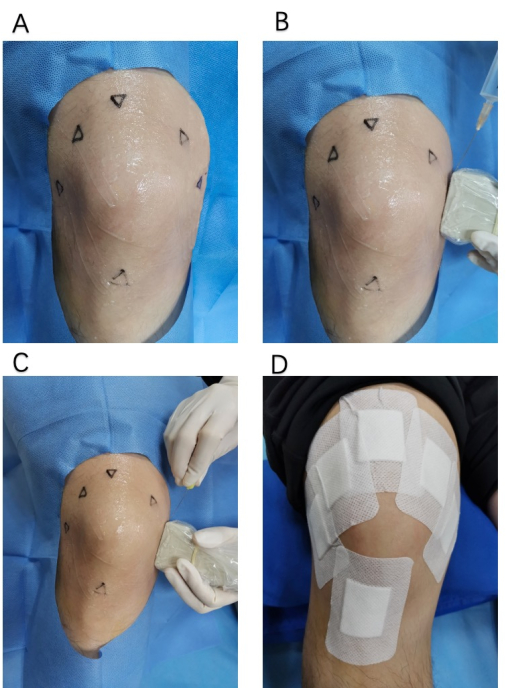
Figure 3: Acupotomy operation diagram. (A) The field of view and the scope of disinfection of the operation ; (B) Local anesthesia under ultrasound; (C) Acupotomy under ultrasound; (D) Postoperative care behavior of protecting the operated wound. Please click here to view a larger version of this figure.
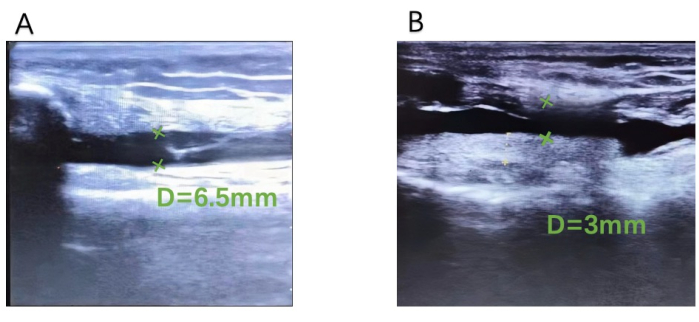
Figure 4: Suprapatellar bursae synovial thickness. (A) Before treatment and (B) after treatment. An ultrasound image of the suprapatellar bursa synovium thickness decreasing from 6.5 mm (A) to 3 mm (B) in the same patient before and after treatment. Please click here to view a larger version of this figure.
Table 1: Baseline information. The basic data of the 58 patients, including gender, mean age, and mean duration of disease. Please click here to download this Table.
Table 2: Scores collected between the treatment and control group. VAS, WOMAC, HSS, and Synovial thickness of suprapatellar bursae were compared between the two groups. For significance calculation, a t-test was used, and the data were expressed as the mean ± SEM. Compared with the control group, * p < 0.05. Please click here to download this Table.
Table 3: Representative patient data. The observation data of one representative patient, including basic information, changes in VAS, WOMAC, HSS, and suprapatellar bursa synovial thickness before and after treatment. Please click here to download this Table.
Discussion
There are three aspects of the treatment procedure that need special attention. The first is tenderness point localization. The surface of the total knee joint should be pressed to mark the location of the patient's pain response through the patient's complaint and the doctor's palpation. Peroneal collateral ligament and iliotibial band point, patellar lateral retinaculum point, quadriceps tendon and suprapatellar bursa point, patellar medial retinaculum point, tibial collateral ligament point, pes anserinus bursa point are frequent sites of pain and can be focused on.
The second is ultrasound localization. When observing the knee using musculoskeletal ultrasound, the fixation point is mainly observed by the following methods. Scanning was performed along the short axis and the long axis of the quadriceps tendon with an 8-15 MHz linear array probe, and the scanning depth was 1-4 cm. The common pathological manifestations of fixation sites were tendon thickening, hypoechoic, and loss of layered structure. Scanning was performed along the long axis of the medial and lateral collateral ligaments using an 8-12 MHz high-frequency linear array probe with a scanning depth of less than 3 cm. The common pathological manifestations of the fixation site were ligament thickening, local hypoechoic changes, irregular cortical bone of the lateral femoral condyle, and/or expansion of the bursal sac, low to anechoic effusion in the bursal sac, and septation in the bursal sac. A 10-12 MHz linear array probe was used to scan the sagittal section at a depth of 2-3 cm along the long axis section of the patellar tendon, and the sonographic findings were verified on the short axis section. The fixation point showed local thickening and hypoechoic, which was best located in the deep proximal part of the patellar tendon.
Finally, there is the method of interventional needle entry. When the ultrasound probe was positioned along the pathological images, the syringe needle and knife were inserted from the probe edge, and the needle direction was parallel to the direction of muscle and ligament fibers to avoid cutting muscle and ligament fibers. In the ultrasound field, it was determined that the needle entered the target position, avoiding contact with blood vessels and nerves.
During the course of treatment, the operator can improve the method or troubleshoot problems in the following ways. If the patient's tender point cannot be found, it can be replaced by the point where the patient complains of soreness and distention. Clinically, there may also be a large area of pain in the whole knee, but at this time, the pain is preferred to the more serious position, in principle, with no more than 15 treatment points. If the ultrasound image is blurred, it can be checked whether the ultrasound frequency selection is appropriate, or the depth of the observation position can be adjusted by changing the intensity of the probe pressing the skin.
The pathogenesis of KOA involves several factors and complex mechanisms that still need to be fully elucidated. The knee joint is composed of the inferior end of the femur, the superior end of the tibia, and the patella and is the most complex trochlear joint in the human body. Under the action of the muscles and ligaments, the knee joint maintains a normal alignment and balance of the lower limb force line. However, when pathological factors affect the knee joint, the knee muscles and ligaments are partially contracted, and local stress on the articular cartilage increases, which leads to poor joint alignment. In severe cases, the lower limb force line is unbalanced, and the string around the knee joint is stressed abnormally. It often leads to stress changes at the bowstring junction, that is, adhesion and contracture of the soft tissues around the knee, and further development will lead to bone hyperplasia, that is, the occurrence of KOA23,24,25,26.
The therapeutic mechanism of acupotomy27 involves the regulation of the dynamic balance of the soft tissues by releasing adhesions. This can increase the local pain threshold in patients with myofascitis. Entrapment of the cutaneous nerve can be relieved by reducing the tension and decompressing the soft tissue at the point of tenderness. Clinical studies have concluded that the treatment of KOA with acupotomy, alone or in combination with other treatments, can significantly reduce intra-articular inflammation, improve bone metabolism, promote joint repair, improve knee joint function, and enhance patients' quality of life28. Animal experimental studies have shown that acupotomy can not only effectively improve the degree of fatigue of the anterior tibial muscle of rabbits with KOA and adjust the physiological and mechanical behavior of the tendons of the anterior tibial muscle29 but also greatly improve the strength of the collateral ligament of the knee of animals with KOA and improve the mechanical properties of the soft tissues around the knee. Thus, the mechanical balance of the knee joint can be restored to achieve a therapeutic effect in KOA.
Currently, most clinical uses of autonomy still adopt the blind acupuncture method, that is, without the aid of imaging, only by the experience of the surgeon and the patient's feedback during the operation. Needle-knife treatment without ultrasound increases the requirement for surgeons to have technical experience and also increases the surgical risk and pain to patients, which is not conducive to the promotion of needle-knife treatment of KOA. Therefore, visualization during acupotomy with modern imaging techniques has become a trend in promoting acupotomy use.
Musculoskeletal ultrasound, which refers to the ultrasonic diagnosis and evaluation technique applied to the musculoskeletal system, was used in this study. It plays an important role in the monitoring and diagnosis of soft tissue injury and soft tissue lesions30. Musculoskeletal ultrasound can accurately display the anatomical position, adjacency, shape, and size of muscles, tendons, and ligaments and can also dynamically help observe the movement of muscles and tendons in real time, accurately guiding the location of needle-knife operations and accurately evaluate the site after a procedure31.
In this study, VAS, HSS, WOMAC, synovial thickness of suprapatellar bursae, and adverse reactions were used to evaluate the efficacy and safety of ultrasound-guided autonomy for KOA. VAS evaluated the severity of pain by visual simulation. HSS evaluated knee joint function in five aspects: pain, function, range of motion, muscle strength, flexion deformity, and stability. WOMAC evaluated the structure and function of the knee joint in terms of pain, stiffness, and physical function. Musculoskeletal ultrasound can measure the synovial thickness of suprapatellar bursae. Adverse effects include fainting, nausea, vomiting, infection, swelling and pain around the pinhole, and an increase in pain during treatment.
The results indicate that the synovial thickness of the suprapatellar bursae in the treatment group was significantly lower (p < 0.05), HSS was significantly higher (p < 0.05), and WOMAC osteoarthritis index score was significantly lower than that in the control group (p < 0.05). Although there was 1 case of adverse reaction, the symptoms were mild and did not affect treatment and follow-up.
It is necessary to acknowledge the limitations of this study. Although many studies31,32,33 have proposed using the synovial thickness of suprapatellar bursae as diagnostic and evaluation criteria for KOA, there is still no consensus or guidelines. As a self-controlled study, this study lacks efficacy in comparison with other treatment methods, and the follow-up time and sample size need to be increased, which may have affected the generalizability and accuracy. In the future, more randomized, controlled, double-blind trials are needed to demonstrate the advantage of ultrasound-guided acupotomy for KOA.
In summary, ultrasound-guided acupotomy can display the location of the acupotomy and the anatomical structure of the lesion in real-time to achieve accurate release of adhesions and reduce operational injuries. This study showed that ultrasound-guided acupotomy had a curative effect on KOA, which significantly reduced synovial thickness, relieved pain, and improved knee joint function. At the same time, ultrasound-guided acupotomy has the advantages of low side effects and high safety, which is worthy of popularization and application.
Disclosures
The authors have nothing to disclose.
Acknowledgements
We are grateful to Shanghai Three-year Action Plan to Further Accelerate the Inheritance and Innovation of Traditional Chinese Medicine (ZY(2021-2023)-0201-01); Pudong New Area Health System Pudong Famous TCM Training Program (PWRzm2020-15); Chinese Medicine Rehabilitation Service Enhancement Project (Medical 032); Innovation project of Longhua Hospital: Clinical study of acupotomy combined with knee balance exercise in the treatment of knee osteoarthritis (CX202045); Clinical study of acupotomy combined with Mulligan dynamic joint loosening in the treatment of periarthritis of shoulder (PKJ2020-Y76); Pudong New Area Health Commission Pudong Famous Chinese Medicine Successor Training Plan (PWRzj2020-21); TCM special disease Brand Construction Doubling Plan – Small acupotomy Special Disease (PDZY-2021-0304).
Materials
| Disposable sterile injection needle | Shanghai Mishava Medical Industry Co., Ltd | 601900973 | Type specification:0.5 x 38 RWLB |
| Disposable medical mask | Shanghai Honglong Medical Supplies Equipment Co., LTD | 20162140493 | Type specification: 17.5 x 9.5cm |
| Disposable sterile small needle-knife | Wujiang Yunlong Medical equipment Co., Ltd | PR-4040 | Type specification:40 mm x 40 mm |
| Disposable sterile syringe | Shandong Weigo Group Medical polymer Products Co., Ltd | 601909174 | Type specification:10 mL |
| Disposable sterile towel | Xinxiang Huakang Medical Material Co., LT | 20182140517 | Type specification: 80x100cm |
| Hygiene hat | Shanghai Honglong Medical Supplies Equipment Co., LTD | 20150071 | Type specification: 21x14cm |
| Lidocaine hydrochloride | Shanghai Hefeng Pharmaceutical Co., Ltd | 6904996104121 | Type specification:5 mL |
| Marker pen | Zebra Trading (Shenzhen) Co., Ltd | 4901681518111 | Type specification:1.0 mm/0.5 mm |
| Sterile absorbent cotton ball | Shanghai Honglong Medical Supplies Equipment Co., Ltd | 601905637 | Type specification:0.3 25 g |
| Sterile disposable medical plastic cup | Shanghai Honglong Medical Supplies Equipment Co., Ltd | 709008633 | Type specification:Waist-shaped disc |
| Sterile dressing block | Ningbo Haishu Shenyuan Medical Materials Co., Ltd | 601909470 | Type specification:7.5 cm x 7.5 cm x 8 floors |
| Sterile medical tweezers | Shanghai Honglong Medical Supplies Equipment Co.,Ltd | 603917444 | Type specification:Small size |
| Sterile protective cover for probe | Yangzhou Puen Medical Technology Co., LTD | 20200046 | Type specifications: 20x150cm |
| Sterile rubber surgical gloves | Guilin Hengbao health protection Co., Ltd | 6971787071320 | Type specification:6.5 |
| Sterile self-adhesive dressing | Shanghai ISO Medical Products Co., Ltd | 601909414 | Type specification:10 cm x 15 cm |
| Sterile ultrasonic coupler | Jiangsu Huadong Medical Equipment Industrial Co., LTD | 6972830280430 | Type Specifications: 20g |
| Sterile water for injection | Shanghai Xinyi Jinzhu Pharmaceutical Co., Ltd | 6938493300953 | Type specification:5 mL |
| Type II skin disinfectant | Shanghai Likang Disinfection high-tech Co., Ltd | 6909157000359 | Type specification:500 mL/ bottle |
| Ultrasound | Suzhou Daer Medical Equipment Co., Ltd | 100018857 | uSmart3300 portable color ultrasound system |
References
- Joo, P. Y., Borjali, A., Chen, A. F., Muratoglu, O. K., Varadarajan, K. M. Defining and predicting radiographic knee osteoarthritis progression: A systematic review of findings from the osteoarthritis initiative. Knee Surg Sports Traumatol Arthrosc. 30 (12), 4015-4028 (2022).
- Tan, X. F., Guo, Y. X. Research progress of predisposing factors of knee osteoarthritis. Rheumatism Arthritis. 11 (1), 60-64 (2022).
- Alrowali, L. M. G. Magnetic resonance evaluation of knee osteoarthritis among the Saudi population. Pak J Med Sci. 35 (6), 1575-1581 (2019).
- Thomas, E., Peat, G., Croft, P. Defining and mapping the person with osteoarthritis for population studies and public health. Rheumatology. 53 (2), 338-345 (2014).
- Primorac, D., et al. Knee osteoarthritis: A review of pathogenesis and state-of-the-art non-operative therapeutic considerations. Genes. 11 (8), 854 (2020).
- Tang, X., et al. The prevalence of symptomatic knee osteoarthritis in China: Results from the China health and retirement longitudinal study. Arthritis Rheumatol. 68 (3), 648-653 (2016).
- Hunter, D. J., Schofield, D., Callander, E. The individual and socioeconomic impact of osteoarthritis. Nat Rev Rheumatol. 10 (7), 437-441 (2014).
- Wang, B., et al. Systematic review of the epidemiology and disease burden of knee osteoarthritis in China. Chin J Evid-Based Med. 18 (2), 134-142 (2018).
- Michael, J. W., Schlüter-Brust, K. U., Eysel, P. The epidemiology, etiology, diagnosis, and treatment of osteoarthritis of the knee. Dtsch Arztebl Int. 107 (9), 152-162 (2010).
- Zhou, Q. Y., et al. Opportunities and challenges in the development of visual acupotomies. Chinese J Tradl Chinese Med. 35 (10), 4801-4804 (2019).
- Gao, G. X., Zhang, S. Clinical study of musculoskeletal ultrasound-guided knife-needle relaxation in treatment of Cervical radiculopathy. Hebei Chinese Med. 43 (4), 662-665 (2021).
- Wang, J., et al. Clinical study of musculoskeletal ultrasound-guided acupotomy in the treatment of greater occipital nerve entrapment syndrome. South China J Def Med. 34 (8), 527-530 (2019).
- Ren, S., et al. Ultrasound-guided acupotomy combined with ozone in the treatment of 40 cases of subacromial bursitis. Chinese J Orthoped Traumatol Tradl Chinese Med. 29 (6), 71-73 (2021).
- Dai, M., Li, K. P., Wu, X. L. Research status and application advantages of ultrasonic visualization acupotomology. J Liaoning Uni Tradl Chinese Med. 22 (6), 170-173 (2020).
- Zeng, X., et al. Research progress of ultrasound acupotoma visualization. J Acupunct Res. 46 (6), 546-548 (2019).
- Joint Surgery Group of the Orthopedic Branch of the Chinese Medical Association. Guidelines for the diagnosis and treatment of osteoarthritis (2021 edition). Chin J Orthop. 41 (18), 1291-1314 (2021).
- Malanga, G., Mautner, K. . Atlas of ultrasound-guided musculoskeletal injection. , (2014).
- Hu, Z. J. . Clinical practice of practical small needle knife. , (2018).
- Chinese society of acupuncture and moxibustion minimally invasive acupotomology professional committee. . Acupotomology clinical diagnosis, treatment and operation norms. , (2012).
- He, S., Renne, A., Argandykov, D., Convissar, D., Lee, J. Comparison of an emoji-based visual analog scale with a numeric rating scale for pain assessment. JAMA. 328 (2), 208-209 (2022).
- Whittaker, J. L., et al. OPTIKNEE 2022: consensus recommendations to optimise knee health after traumatic knee injury to prevent osteoarthritis. Br J Sports Med. 56 (24), 1393-1405 (2022).
- Alrawashdeh, W., et al. Effectiveness of total knee arthroplasty rehabilitation programmes: A systematic review and meta-analysis. J Rehabil Med. 53 (6), (2021).
- Xu, Y., et al. Discussion on the treatment strategy of knee osteoarthritis based on the theory of transfascia and myofascia. Chinese J Tradl Chinese Med. 35 (7), 3293-3296 (2019).
- Liang, C., et al. Effects of acupotomy intervention on the biodynamics of medial collateral ligament and the expression of Integrin β1, Col-II genes in KOA rabbits. Chinese J Tradl Chinese Med. 30 (5), 1689-1693 (2015).
- Zhang, L., Liu, H., Xiu, Z. Meta-analysis of the therapeutic effect of acupotomy on knee osteoarthritis based on the theory of transtendon. Chinese Ethnic Folk Med. 29 (8), 54-57 (2020).
- Zhang, T. M., Du, Y. J. A brief introduction to the mechanical anatomical system of human bowstring. China Med Rev. 14 (3), 164-168 (2017).
- Zhao, Y., Fang, W., Qin, W. Mechanism of small acupotomy in closed treatment of myofascitis. Chinese J Acupuncture Moxibustion. 34 (9), 907-909 (2014).
- Shi, X., Liu, Y. Short-term effect of acupotomy on improving symptoms of knee osteoarthritis. J Guangzhou Uni Chinese Med. 36 (1), 74-78 (2019).
- Zhou, S., et al. Effect of acupotomy on surface electromyography and biomechanical behavior of tendons of tibial anterior muscle in rabbits with knee osteoarthritis. J Beijing Uni Chinese Med. 41 (8), 675-680 (2018).
- Geng, W., et al. Meta-analysis of musculoskeletal ultrasound in the diagnosis of soft tissue injury. J Naval Med. 43 (1), 78-83 (2022).
- Liu, Q., et al. Visualization development of acupotomy with ultrasonic-assisted means. J Hubei Uni Tradl Chinese Med. 18 (4), 117-120 (2016).
- Xu, D. H., et al. Tiaohe Yinyang acupotomy for knee osteoarthritis: a randomized controlled trial. Zhongguo Zhen Jiu. 42 (12), 1351-1356 (2022).
- Zhao, L., et al. Zhuifeng Tougu capsules in the treatment of knee osteoarthritis (cold dampness obstruction syndrome): a randomized, double blind, multicenter clinical study. Chin Med. 19 (1), 18 (2024).

