Assessment of Dependence in Activities of Daily Living Among Older Patients in an Acute Care Unit
Summary
During acute medical problems, older people may lose independence in activities of daily living (ADL). Assessment of baseline ADL and ADL on admission can guide personalized treatment plans aimed at preventing nosocomial dependence and ensuring better functional outcomes.
Abstract
During an acute medical problem, older people may lose functional independence. ADL scales are used to assess this loss of independence. The simplest and most convenient ADL scale is the Katz Index, which measures six ADL: bathing, dressing, toileting, transferring, continence, and feeding. A lower ADL score indicates greater loss of functional independence. The ADL score prior to the acute medical problem (baseline) is estimated by questioning the patient or the caregivers, and this score is then compared with that on hospital admission. The ADL score should be monitored from hospital admission until discharge to allow early detection of changes in functional independence. Identifying any loss of functional independence before and during hospitalization provides information to caregivers regarding the risk of short-term mortality risk and complications, and the prognosis after hospitalization.
Introduction
Medical problems can cause older people to lose functional independence, rendering them unable to carry out activities of daily living (ADL) without assistance from others. This loss of independence, which often results from cardiovascular comorbidities1, cognitive impairment2,3, and visual impairment4, impacts patient quality of life5 and life expectancy6, and increases healthcare costs7. Functional independence may progressively deteriorate, or be lost completely, with more severe comorbidities (cognitive impairment, heart failure, etc.). It may also worsen during an acute medical problem, such as stroke, myocardial infarction, lower limb fracture, or chest infection8. About 30% of patients aged between 70 and 80 years, and 60% of those aged over 80 years, experience such a loss of independence during hospitalization9,10. Patients may recover the functional independence they enjoyed prior to the acute medical problem, or it may persist thereafter despite appropriate treatment.
It is widely accepted that treatment aimed at maintaining or restoring functional independence during hospitalization for an acute medical problem is most effective if it is started as soon as possible11. Physical exercise during hospitalization improves function in the short and medium term12,13. In a hospitalized population, scores on measures of ADL were associated with muscle oxidative capacity and muscle function1. Hence, assessing a patient's functional independence at an early stage of hospitalization is a priority; this assessment should then be compared with the patient's level of ADL independence before hospitalization (baseline). Medical care, particularly nursing care, is aimed at restoring any loss of independence or maintaining the existing level thereof. This requires a reliable and reproducible assessment method; the most commonly used measure for this purpose is the Katz Index of Independence in Activities of Daily Living (Katz ADL).
The Katz ADL, developed in 1970, allows assessment of a patient’s ability to carry out basic ADL independently15,16. The scale measures patient independence in six activities: bathing, dressing, toileting, transferring, continence, and feeding. Each activity is scored as 0 or 1, where a score of 0 indicates dependence on another person, and 1 indicates independence. A total Katz ADL score of 6 denotes full independence, a score of 4 moderate dependence, and a score of 2 or less severe dependence.
For many years, the Katz ADL has proven useful in the assessment of functional status in older people. First, the Katz ADL assessment is very simple to perform and involves interviewing the patient or family members about the patient’s ability to perform the six ADL activities, or directly observing how well the patient performs these activities17. Furthermore, during an acute medical problem, the Katz ADL Index is sensitive to major, but not to minor, changes in health status. Thus, this tool is ideal for assessing the impact of an acute medical problem on patients’ functional status, whatever their chronic morbidities.
When initiating rehabilitation within the first days of an acute medical problem, it is necessary to determine the extent of the patient’s functional decline. For this purpose, we propose that the functional status of each patient should be assessed before hospitalization via interview, and that the ability to perform ADL be assessed within the first days of hospitalization via observation. These two assessments could guide early preventive and rehabilitative measures in parallel with a care plan for the acute event. The effectiveness of these measures for promoting recovery of functional independence can be monitored by repeated ADL assessment until discharge.
Protocol
The protocol has been approved by the human research ethics committee of the University Hospital of Bordeaux.
NOTE: The protocol described in this section involves evaluation of ADL dependence using the Katz ADL. The six activities assessed are described above18. The Katz ADL is administered at the Bordeaux University Hospital, on admission and discharge, to all patients over 75 years of age, i.e., all those in acute geriatric medicine wards. Inpatients in geriatric units present with numerous comorbidities and it is recommended that staff assess all such patients. In theory, the Katz ADL could be administered to all patients at risk of losing their independence due to an acute medical problem, which would include some younger patients. However, ADL dependence is infrequent in younger adults, as the prevalence of disabling diseases is low in that population. Nevertheless, the protocol could also be implemented in other departments, particularly internal medicine, cardiology, and neurology.
1. Protocol for administering the Katz ADL before hospitalization
- Evaluate bathing activity.
- To evaluate bathing, ask patients how they bathe and whether they need someone to help them with bathing. If so, ask them which part of the body they require help with. Then, note whether they are independent (1 point) or dependent (0 point) in bathing activities.
NOTE: Independent patients bathe their entire body alone, with the exception of the back, genital area, or a disabled extremity. Dependent patients need help to bathe several parts of their body, or to get in and out of the shower or bathtub.
- To evaluate bathing, ask patients how they bathe and whether they need someone to help them with bathing. If so, ask them which part of the body they require help with. Then, note whether they are independent (1 point) or dependent (0 point) in bathing activities.
- Evaluate dressing.
- Ask patients whether they can dress and undress alone, and whether they can take their clothes out of the closet without help. Ask whether they need help with putting on socks or other items of clothing. Then, note whether they are independent (1 point) or dependent (0 point) in dressing activities.
NOTE: An independent person gets their clothes out of the closet and puts them on, including fastening them where applicable. Shoe tying is not included among dressing activities. A dependent person needs some help with dressing or needs to be completely dressed by someone else.
- Ask patients whether they can dress and undress alone, and whether they can take their clothes out of the closet without help. Ask whether they need help with putting on socks or other items of clothing. Then, note whether they are independent (1 point) or dependent (0 point) in dressing activities.
- Evaluate toileting.
- Ask patients whether they go to the toilet unassisted at home. Ask whether they can sit down and stand up from the toilet, arrange their clothing as needed, and clean the genital area without help. Then, note whether they are independent (1 point) or dependent (0 point) in toileting.
NOTE: An independent person goes to the toilet, sits and stands up from the toilet, arranges clothes, and cleans the genital area without help. A dependent person needs help transferring to the toilet and cleaning up, or uses a bedpan or commode.
- Ask patients whether they go to the toilet unassisted at home. Ask whether they can sit down and stand up from the toilet, arrange their clothing as needed, and clean the genital area without help. Then, note whether they are independent (1 point) or dependent (0 point) in toileting.
- Evaluate transferring.
- Ask patients whether they can move from the bed to a chair, and from a chair to the bed, without human assistance. Then, note whether they are independent (1 point) or dependent (0 point) in transferring.
NOTE: An Independent person moves into or out of a bed or chair unassisted or using a mechanical transferring aid. A dependent individual needs help from another person to move from a bed to a chair or requires a complete transfer.
- Ask patients whether they can move from the bed to a chair, and from a chair to the bed, without human assistance. Then, note whether they are independent (1 point) or dependent (0 point) in transferring.
- Evaluate continence.
- Ask patients whether they have complete self-control over urination and defecation. If not, ask whether they can use a urinary catheter or diaper without help. Then, note whether they are independent (1 point) or dependent (0 point) with respect to continence.
NOTE: Independent patients exercise complete self-control over urination and defecation, or use a urinary catheter or diapers without help. The dependent person is partially or totally incontinent (bowel or bladder) and needs help to manage these functions.
- Ask patients whether they have complete self-control over urination and defecation. If not, ask whether they can use a urinary catheter or diaper without help. Then, note whether they are independent (1 point) or dependent (0 point) with respect to continence.
- Evaluate feeding.
- Ask patients whether they eat without help; if so, ask whether they are able to cut meat or open the lid of a yogurt container. Then, note whether they are independent (1 point) or dependent (0 point) in feeding activities. An independent person can eat a prepared and delivered meal without assistance.
NOTE: An independent person transfers food from the plate into the mouth without help. A dependent person needs partial or total help with feeding.
- Ask patients whether they eat without help; if so, ask whether they are able to cut meat or open the lid of a yogurt container. Then, note whether they are independent (1 point) or dependent (0 point) in feeding activities. An independent person can eat a prepared and delivered meal without assistance.
- Calculate the ADL score by summing the scores for all activities.
2. Administration of ADL scale on hospital admission
- Bathing
- During the first day of hospitalization, offer patients a shower. If they feel able to take one, accompany them to the bathroom and check whether they are able to wash by themselves. If patients do not feel able to do this, offer to wash them in bed or at the basin.
- Observe whether patients are able to do this on their own or whether they need guidance or help with certain parts of the body. Then, note whether they are independent or dependent in bathing (following the same definition of independent and dependent as in step 1.1).
- Dressing
- During the first day of hospitalization, propose that patients get dressed. Ask them to choose clothes from the closet and put them on; if patients have difficulty, help them to get dressed.
- In the evening, follow the same procedure, but as applied to undressing.
- Note whether the patient is independent or dependent in dressing (following the same definition of independent and dependent as in step 1.2).
- Toileting
- During the first few days of hospitalization, check whether patients are able to go to the toilet alone, sit and stand up from the toilet, arrange their clothing, and clean the genital area.
- Evaluate whether a commode or bedpan is needed. Note whether patients are independent or dependent in toileting (following the same definition of independent and dependent as in step 1.3).
- Transferring
- On the first day of hospitalization, ask patients to transfer from the bed to a chair and from the chair to the bed. If patients have any difficulty, first offer mechanical transferring aids, and if necessary, help them to make the transfer. Then, note whether patients are independent or dependent for transferring (following the same definition of independent and dependent as in step 1.4).
- Feeding
- During the first meal at the hospital, observe whether patients are able to eat alone, including cutting meat and opening the lid of a yogurt container. Help them if necessary. Then, note whether the patient is independent or dependent for eating (following the same definition of independent and dependent as in step 1.6).
- Calculate the ADL score by summing the scores for all activities.
3. Compare functional independence scores before the acute medical problem and at the time of hospital admission
- Identify the activities in which patients have lost independence during the acute medical problem. Identify activities in which patients were dependent prior to the problem.
- Encourage patients to regain their lost independence through rehabilitative care.
- Help to maintain any independence that was not lost during the acute medical problem.
4. Recalculate ADL score throughout hospitalization (twice per week)
- Perform the same assessment steps described in Step 2.
- Discuss the assessment results during a staff meeting where nurses, nurse assistants, physicians, and physiotherapists are present.
- Compare ADL scores to identify improvement or deterioration of functional independence.
- Maintain or modify rehabilitative care according to the evolution of functional independence; the goal is for patients to recover their former level of independence.
5. Evaluate the ADL score at discharge and compare it to the score prior to hospitalization
- Determine whether patients have lost functional independence as a result of the acute medical problem.
- Adapt the home help protocol as needed.
Representative Results
Here, we consider two example cases after completion of the protocol: one with full recovery of the baseline level of ADL function at discharge, and one with no or partial recovery.
Discharged with baseline level of ADL function
In this group of patients, two ADL function trajectories were possible, as shown in Figure 1: patients who maintained their ADL score throughout hospitalization (Trajectory A) and those whose score at hospitalization was lower than at baseline, but who regained their baseline level of function by discharge (Trajectory B). Patients of either trajectory discharged with their baseline ADL function (had an 83.8% and 67% chance of maintaining it 1 month and 1 year after discharge, respectively. In this study, the 1-year mortality rate was 17.8% in this group of patients and there was no difference therein between patients who followed trajectory A and those who followed trajectory B11.
Discharged with new or additional disability in ADL
In our cohort, three types of cases were identified, as shown in Figure 2: patients who retained their baseline independence on admission to the hospital but showed deterioration during hospitalization and did not regain full independence thereafter (trajectory C); patients who lost their baseline independence prior to hospitalization for the acute problem and did not regain it during hospitalization (trajectory D); and patients who showed deterioration of independence both prior to and during hospitalization, and did not regain full independence (trajectory E)19. Of the patients discharged with new or additional disabilities in ADL, 33.5% recovered their baseline level of ADL function within the first month after discharge, and 30.1% did so within the first year. The 1-year mortality rate was 41.3% for these patients. There was no significant difference between patients who followed trajectory C and those who followed trajectory D11.
Possible errors during execution of the protocol
Our protocol is simple to implement. Errors are most likely to occur when determining the baseline ADL score, especially when it is obtained through interviews with patients. Some patients may underestimate or overestimate their prior level of functional independence at home. Furthermore, patient recall may be distorted by cognitive impairment. Considering the high prevalence of cognitive impairment among those in geriatric acute care wards, we recommend questioning the family, nurses working in the home or nursing home, or the attending physician to obtain the most accurate baseline ADL score. This questioning is mostly done by telephone after hospital admission.
Examples of results obtained at Bordeaux University Hospital
The present protocol was implemented in 2017 and applied to all patients over 75 years of age. During the year since the implementation of the protocol, loss of functional independence was observed less often. In 2016, of the 699 hospitalized older patients to whom the protocol was applied, 25.97% showed a loss of functional independence, compared to 19.48% of 852 patients in 2019.
Although systematic application of the protocol to all hospitalized geriatric patients was required, data were not consistently entered in the medical records. In 2017, only 36.78% of medical records mentioned ADL data; in 2019, these data were present in 51.26% of medical records. Thus, health professionals in the hospital should be encouraged both to carry out the protocol and record the patient outcomes.
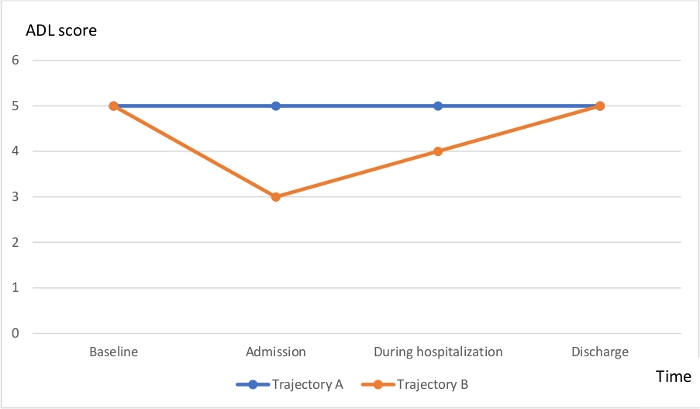
Figure 1: Favorable trajectories of ADL dependence during an acute medical problem, from baseline to post-event status. Trajectory A: Mild baseline ADL dependence with no decline at any point during the event; Trajectory B: Mild baseline ADL dependence, decline during the acute event, and recovery before discharge. Please click here to view a larger version of this figure.
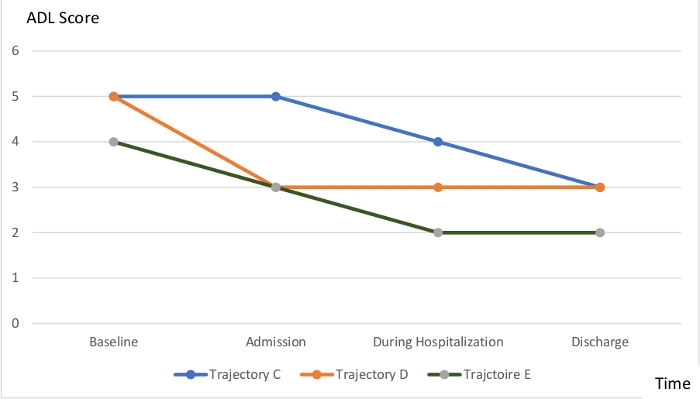
Figure 2: Unfavorable trajectories of ADL dependence during an acute medical problem, from baseline to post-event status. Trajectory C: Mild baseline dependence, no decline noted on admission but decline during hospital stay. Trajectory D: Mild baseline dependence, decline noted on admission, no recovery during hospital stay or at discharge. Trajectory E: Moderate baseline dependence, decline noted on admission, further decline during hospital stay, no recovery before discharge. Please click here to view a larger version of this figure.
Discussion
The protocol is not appropriate in all situations
Our protocol was designed for patients who have been hospitalized for an acute medical problem. However, other tools, such as the Barthel Index, should be used in rehabilitation centers. The original Katz ADL scale scores functional ability only on a 7-point scale (scores of 0–6); subtle fluctuations in functional dependence may therefore be overlooked. The Barthel Index, which is generally comparable to the Katz ADL, yields weighted and summed scores. The six activities included in the Katz ADL scale are also evaluated by the Barthel Index, but with several differences: bowel and bladder control are considered separately, and mobility is addressed in greater detail (i.e., both on level surfaces and when climbing stairs). Also, the total score is based on 10 activities, each of which is scored as 0, 5, 10 or 15 points. Transferring and mobility are the only activities scored on 15 points. The maximal overall score is 100 points, with higher scores indicating greater independence. The Barthel Index should ideally be scored during a multidisciplinary meeting involving the physician, nurse, physiotherapist, and occupational therapist, because the score guides the rehabilitation plan20.
Furthermore, the Katz ADL score is not pertinent during follow-up assessment of cognitive impairment. ADL dependence, as assessed by the Katz ADL score, occurs at a late stage in the treatment of major cognitive problems. The hierarchical model of functional dependence was developed for epidemiological population-based studies. Older subjects may become dependent, in terms of the performance of basic ADL activities, at the stage considered as severe dependence based on the Katz index. Prior to that stage, moderate dependence is indicated by the need for help from another person to perform instrumental activities of daily living (IADL), which include household activities, making telephone calls, shopping, transferring, and managing medications or finances without help21. IADL dependence is included among the criteria for diagnosis of major cognitive disabilities.
The questionable "continence" item
In our protocol, we modified the evaluation of "continence." Incontinence is an impairment rather than a disability; therefore, unlike the original ADL scoring system, we award the patient 1 point if they can manage their incontinence on their own. A patient can be incontinent and still be functionally independent.
The 12-item ADL scale: an alternative
An ADL scale with 12 items (and thus a maximum possible score of 12 points) is currently preferred for comprehensive gerontological assessments performed in a day hospital, to ensure precise evaluation of functional independence outside of the context of an acute problem22. The 12-item ADL scale is more sensitive to changes in ADL dependence than the 6-point version but is still less sensitive than the Barthel Index. It may be instructive to apply the 12-item scale after the 6-item version for patients who exhibit no change between their baseline and admission ADL scores. The 12-item ADL scale evaluates the same six activities as Katz's ADL scale; the difference lies in the scoring system. In the case of the former instrument, a score of 0 indicates independence, 1 corresponds to moderate dependence, and 2 indicates dependence. Thus, the feeding item is scored as 1 if the subject is able to eat alone but needs help to cut meat or to open the lid of a yogurt container. Several elements are considered by the 12-item ADL scale that do not decrease the ADL score, such as the need for assistance when using the toilet for only one part of the body, or the need for assistance when tying one's shoes. We have not yet tried to incorporate the 12-item ADL scale into our protocol; combining multiple tools may prove disruptive for health care teams, where efficient prevention of ADL dependence relies on simple tools that are easy to memorize and apply as frequently as necessary.
Divulgazioni
The authors have nothing to disclose.
Acknowledgements
The University of Bordeaux and University Hospital of Bordeaux supported this publication.
Materials
| Clothing and underwear | Any | ||
| Hospital Bathroom with toilet | |||
| Meal Tray | |||
| Medical Bed | Any | ||
| Medical Chair | Any | ||
| Papers | |||
| Pens | |||
| Table Bed | Any |
Riferimenti
- Jin, Y., et al. Cardiovascular Health Is Associated With Disability Among Older Community Dwelling Men and Women. Journal of Aging and Health. 31 (8), 1339-1352 (2019).
- Mograbi, D. C., et al. The impact of dementia, depression and awareness on activities of daily living in a sample from a middle-income country. Int J Geriatr Psychiatry. 33 (6), 807-813 (2018).
- Sauvaget, C., Yamada, M., Fujiwara, S., Sasaki, H., Mimori, Y. Dementia as a predictor of functional disability: a four-year follow-up study. Gerontology. 48 (4), 226-233 (2002).
- Jacobs, J. M., Hammerman-Rozenberg, R., Maaravi, Y., Cohen, A., Stessman, J. The impact of visual impairment on health, function and mortality. Aging Clinical and Experimental Research. 17 (4), 281-286 (2005).
- Lyu, W., Wolinsky, F. D. The Onset of ADL Difficulties and Changes in Health-Related Quality of Life. Health and Quality of Life Outcomes. 15 (1), 217 (2017).
- Keeler, E., Guralnik, J. M., Tian, H., Wallace, R. B., Reuben, D. B. The impact of functional status on life expectancy in older persons. The Journals of Gerontology Series A Biological Sciences and Medical Sciences. 65 (7), 727-733 (2010).
- van Lier, L. I., et al. Predictors of Societal Costs of Older Care-Dependent Adults Living in the Community in 11 European Countries. Health Services Insights. 12, 1178632918820947 (2019).
- Gill, T. M., Allore, H. G., Gahbauer, E. A., Murphy, T. E. Change in disability after hospitalization or restricted activity in older persons. JAMA. 304 (17), 1919-1928 (2010).
- Chodos, A. H., et al. Hospitalization-Associated Disability in Adults Admitted to a Safety-Net Hospital. Journal of General Internal Medicine. 30 (12), 1765-1772 (2015).
- Gill, T. M., Gahbauer, E. A., Han, L., Allore, H. G. The role of intervening hospital admissions on trajectories of disability in the last year of life: prospective cohort study of older people. BMJ. 350, 2361 (2015).
- Boyd, C. M., et al. Recovery of activities of daily living in older adults after hospitalization for acute medical illness. Journal of the American Geriatrics Society. 56 (12), 2171-2179 (2008).
- Blanc-Bisson, C., Dechamps, A., Gouspillou, G., Dehail, P., Bourdel-Marchasson, I. A randomized controlled trial on early physiotherapy intervention versus usual care in acute care unit for elderly: potential benefits in light of dietary intakes. The journal of nutrition, health & aging. 12 (6), 395-399 (2008).
- Martinez-Velilla, N., et al. Effect of Exercise Intervention on Functional Decline in Very Elderly Patients During Acute Hospitalization: A Randomized Clinical Trial. JAMA Internal Medicine. 179 (1), 28-36 (2019).
- Bourdel-Marchasson, I., et al. Muscle phosphocreatine post-exercise recovery rate is related to functional evaluation in hospitalized and community-living older people. The journal of nutrition, health & aging. 11 (3), 215-221 (2007).
- Katz, S. Assessing self-maintenance: activities of daily living, mobility, and instrumental activities of daily living. Journal of the American Geriatrics Society. 31 (12), 721-727 (1983).
- Katz, S., Downs, T. D., Cash, H. R., Grotz, R. C. Progress in development of the index of ADL. Gerontologist. 10 (1), 20-30 (1970).
- Ciesla, J. R., Shi, L., Stoskopf, C. H., Samuels, M. E. Reliability of Katz’s Activities of Daily Living Scale when used in telephone interviews. Evaluation & the Health Professions. 16 (2), 190-203 (1993).
- Carvalho, T., Polachinido Valle, A., Ferrari Jacinto, A., Ferreira de Sá Mayoral, V., Fortes Villas Boas, P. Impact of hospitalization on the functional capacity of the elderly: A cohort study. Revista Brasileira de Geriatria e Gerontologia. 21, 134-142 (2018).
- Mahoney, F. I., Barthel, D. W. Functional Evaluation: The Barthel Index. Maryland Medicine Journal. 14, 61-65 (1965).
- Peres, K., Verret, C., Alioum, A., Barberger-Gateau, P. The disablement process: factors associated with progression of disability and recovery in French elderly people. Disability and Rehabilitation. 27 (5), 263-276 (2005).
- Lawton, M. P., Brody, E. M. Assessment of older people: self-maintaining and instrumental activities of daily living. Gerontologist. 9 (3), 179-186 (1969).
- Barberger-Gateau, P., et al. Health measures correlates in a French elderly community population: the PAQUID study. Journal of Gerontology. 47 (2), 88-95 (1992).

