Integrated Photoacoustic, Ultrasound, and Angiographic Tomography (PAUSAT) for NonInvasive Whole-Brain Imaging of Ischemic Stroke
Summary
This work demonstrates the use of a multimodal ultrasound-based imaging platform for noninvasive imaging of ischemic stroke. This system allows for the quantification of blood oxygenation through photoacoustic imaging and impaired perfusion in the brain through acoustic angiography.
Abstract
Presented here is an experimental ischemic stroke study using our newly developed noninvasive imaging system that integrates three acoustic-based imaging technologies: photoacoustic, ultrasound, and angiographic tomography (PAUSAT). Combining these three modalities helps acquire multi-spectral photoacoustic tomography (PAT) of the brain blood oxygenation, high-frequency ultrasound imaging of the brain tissue, and acoustic angiography of the cerebral blood perfusion. The multi-modal imaging platform allows the study of cerebral perfusion and oxygenation changes in the whole mouse brain after stroke. Two commonly used ischemic stroke models were evaluated: the permanent middle cerebral artery occlusion (pMCAO) model and the photothrombotic (PT) model. PAUSAT was used to image the same mouse brains before and after a stroke and quantitatively analyze both stroke models. This imaging system was able to clearly show the brain vascular changes after ischemic stroke, including significantly reduced blood perfusion and oxygenation in the stroke infarct region (ipsilateral) compared to the uninjured tissue (contralateral). The results were confirmed by both laser speckle contrast imaging and triphenyltetrazolium chloride (TTC) staining. Furthermore, stroke infarct volume in both stroke models was measured and validated by TTC staining as the ground truth. Through this study, we have demonstrated that PAUSAT can be a powerful tool in noninvasive and longitudinal preclinical studies of ischemic stroke.
Introduction
Blood transports oxygen (via the hemoglobin protein) and other important nutrients to tissues in our bodies. When the flow of blood through tissues is interrupted (ischemia), severe damage to the tissues can occur, the most immediate effects of which are due to a lack of oxygen (hypoxia). Ischemic stroke is the result of interrupted blood flow to a certain region of the brain. The brain damage resulting from an ischemic stroke can occur within minutes of a vessel blockage, and can often have debilitating and lasting effects1,2. A highly valuable strategy to evaluate the physiopathology after ischemic stroke and identify and test new treatments is the use of small-animal models in the lab. Treatments discovered in the lab aim to be translated to clinical use and improve patients' lives. However, the use of animals in biomedical research needs to be carefully evaluated according to Russell and Burch’s 3Rs principles: replacement, reduction, and refinement3. The objective of the reduction component is to reduce the number of animals without compromising data collection. With this in mind, being able to longitudinally evaluate the lesion evolution via noninvasive imaging allows a great advantage in reducing the number of animals required, as well as maximizing the information obtained from each animal4.
Photoacoustic tomography (PAT) is a hybrid imaging modality that combines optical absorption contrast with ultrasound imaging spatial resolution5. The imaging mechanism of PAT is as follows. An excitation laser pulse is illuminated on the target being imaged. Assuming the target absorbs light at the wavelength of the excitation laser, it will increase in temperature. This quick increase in temperature results in a thermoelastic expansion of the target. The expansion causes an ultrasound wave to propagate out from the target. By detecting the ultrasound wave at many positions, the time required for the wave to propagate from the target to the detectors can be used to create an image through a reconstruction algorithm. The ability of PAT to detect optical absorption in deep tissue regions differentiates PAT from ultrasound imaging, which detects boundaries of differing acoustic impedances of tissues5. In the visible and near-infrared spectra, the primary highly absorbing biomolecules that are abundant in organisms are hemoglobin, lipids, melanin, and water7. Of particular interest in the study of stroke is hemoglobin. Since oxyhemoglobin and deoxyhemoglobin have different optical absorption spectra, PAT can be used with multiple excitation laser wavelengths to determine the relative concentration of the two states of the protein. This allows the oxygen saturation of hemoglobin (sO2), or blood oxygenation, to be quantified in and outside of the infarct region8,9. This is an important measure in ischemic stroke, as it can indicate the level of oxygen in the damaged brain tissue following ischemia.
Acoustic angiography (AA) is a contrast-enhanced ultrasound imaging method that is particularly useful for imaging the morphology of vasculature in vivo10. The method relies on the use of a dual-element wobbler transducer (a low frequency element and a high frequency element) in conjunction with microbubbles injected into the circulatory system of the imaging subject. The low-frequency element of the transducer is used for transmitting at the resonant frequency of the microbubbles (e.g., 2 MHz), while the high-frequency element is used to receive the super harmonic signals of the microbubbles (e.g., 26 MHz). When excited at a resonant frequency, the microbubbles have a strong nonlinear response, resulting in the production of super harmonic signals that surrounding body tissues do not produce11. By receiving with a high-frequency element, this ensures that only the microbubble signals are detected. Since the microbubbles are confined to the blood vessels, the result is an angiographic image of blood vessel morphology. AA is a powerful method for imaging ischemic stroke, as the microbubbles that flow through the circulatory system are not be able to flow through blocked vessels. This allows AA to detect regions of the brain that are not perfused due to ischemic stroke, which indicates the infarct region.
Preclinical ischemic stroke research generally relies on the use of histology and behavioral testing to assess the location and severity of the stroke. Triphenyltetrazolium chloride (TTC) staining is a common histological analysis used to determine the stroke infarct volume. However, it can only be used at an endpoint, since it requires the animal to be euthanized12. Behavioral tests can be used to determine motor function impairment at multiple time points, but they cannot provide quantitative anatomical or physiological values13. Biomedical imaging provides a more quantitative approach to studying the effects of ischemic stroke noninvasively and longitudinally9,14,15. However, existing imaging technologies (such as small-animal magnetic resonance imaging [MRI]) can come at a high cost, be unable to provide concurrent structural and functional information, or have limited penetration depth (as most optical imaging techniques).
Here, we combine photoacoustic, ultrasound, and angiographic tomography (PAUSAT; see system diagram in Figure 1), which allows for complementary structural and functional information of blood perfusion and oxygenation following ischemic stroke16. These are two important aspects in assessing the severity of injury and monitoring the recovery or response to treatments. Using these integrated imaging methods can increase the amount of information obtained by each animal, reducing the number of animals required and providing more information in the study of potential treatments for ischemic stroke.
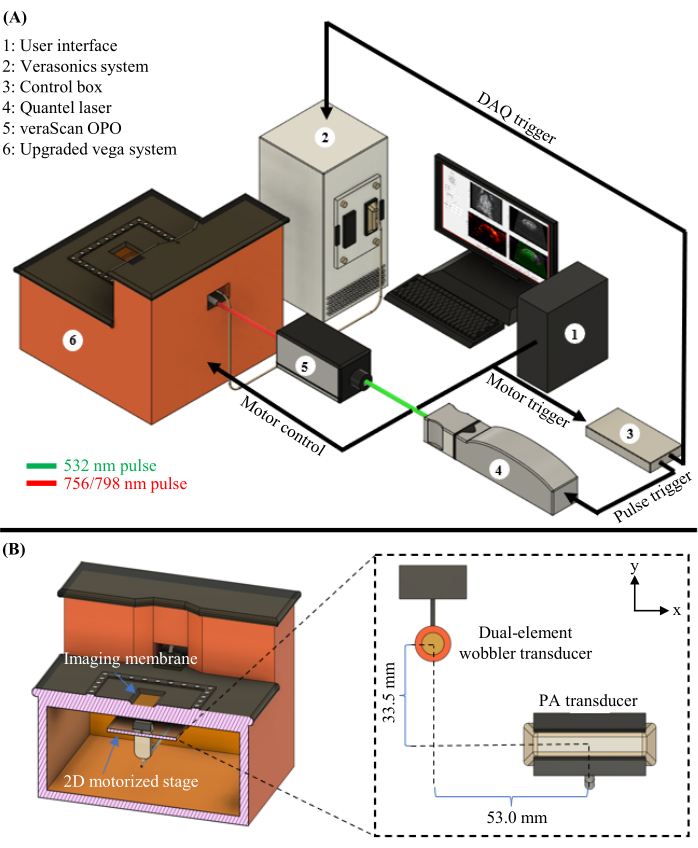
Figure 1: PAUSAT diagram. (A) Complete schematic of the PAUSAT system, including the laser and OPO used for PAT. (B) Inside view of the PAUSAT system, including two ultrasound transducers. The dual-element wobbler transducer is used for both B-mode ultrasound and AA, and the linear-array transducer is used for PAT. Both transducers are mounted on the same 2D motorized stage, allowing for scanning to generate volumetric data. This figure has been modified from16. Please click here to view a larger version of this figure.
Protocol
Representative Results
Discussion
There are a few vital aspects of this method that, if done incorrectly, can lead to significantly decreased image quality and quantitative analysis. The most commonly occurring result of user-error in PAUSAT images is either a lack of signal or very low signal strength, both of which can occur for a variety of reasons. One such reason is a problem with the acoustic coupling. Large air bubbles in the water surrounding the mouse's head during imaging can often block the ultrasound from travelling to or from the transdu…
Divulgazioni
The authors have nothing to disclose.
Acknowledgements
The authors would like to acknowledge the engineering team at SonoVol Inc. for their technical support. This work was partially sponsored by the American Heart Association Collaborative Sciences Award (18CSA34080277), to J. Yao and W. Yang; The United States National Institutes of Health (NIH) grants R21EB027981, R21 EB027304, RF1 NS115581 (BRAIN Initiative), R01 NS111039, R01 EB028143; The United States National Science Foundation (NSF) CAREER award 2144788; the Chan Zuckerberg Initiative Grant (2020-226178), to J. Yao; and NIH grants R21NS127163 and R01NS099590 to W. Yang.
Materials
| 20 GA catheter | BD Insyte Autoguard Winged | 381534 | For mouse intubation |
| 2,3,5-Triphenyltetrazolium chloride | Sigma | T8877 | Necessary for TTC-staining brain for validation |
| 532nm Laser | Quantel | Q-smart 850 | Laser used to pump the OPO for PAT |
| Automatic Ventilator Rovent Jr. | Kent Scientific | RV-JR | To keep mice under anesthesia during surgical procedure |
| Black braided silk 4-0 USP | Surgical Specialties | SP116 | Used for sutures on the neck for pMCAO surgery |
| Bupivacaine | Hospira | 0409-1159-18 | Used prior to closing wounds during surgical procedure |
| C57BL/6 Mice | Jackson Lab | #000664 | Mice used for studying ischemic stroke (2-6 month old male/female) |
| Clear suture | Ethicon | 8606 | Used for closing wound (PT stroke and pMCAO). A clear suture won't interfere with PAT |
| Cold Light LED | Schott | KL 1600 | Needed to create PT stroke |
| Disposable Razor Blade | Accutec Blades | 74-0002 | For sectioning mouse brain |
| Electric drill | JSDA | JD-700 | Used to expose MCA during pMCAO procedure |
| Electrocauterization tool | Wet-Field | Wet-Field Bipolar-RG | Stops blood flow after drilling during pMCAO procedure |
| Hair removal gel | Veet | 8282651 | Used to remove hair from mouse prior to imaging |
| High Temperature Cautery Loop Tip | BOVIE Medical Corporation | REF AA03 | Used to avoid bleeding when separating the temporal muscle from the skull |
| IR Detector Card | Thorlabs | VRC5 | Used to ensure light path is aligned |
| Laser Power Meter | Ophir | StarBright, P/N 7Z01580 | Can be used to calibrate the laser energy prior to imaging |
| Laser Speckle Imaging System | RWD Life Science Co. | RFLSI-III | Can be used to validate stroke surgery success |
| Lubricant Eye Ointment | Soothe | AB31336 | Can be used to avoid drying of the eyes |
| Manually adjustable stage | Thorlabs | L490 | Used with custom ramp for multiple focal depth AA imaging |
| Modified Vega Imaging System | Perkin Elmer | LLA00061 | System containing both B-mode/AA and PAT transducers |
| Optical Parametric Oscillator | Quantel | versaScan-L532 | Allows for tuning of excitation wavelength in a large range |
| Programmable Ultrasound System | Verasonics | Vantage 256 | Used for PAT part of system |
| Rose Bengal | Sigma | 330000 | Necessary to induce PT stroke |
| Suture | LOOK | SP116 | Used for permanent ligation of CCA |
| Temperature Contoller | Physitemp | TCAT-2 | Used to maintain stable body temperature of mice during procedures |
| VesselVue Microbubbles | Perkin Elmer | P-4007001 | Used for acoustic angiography (2.43 × 10^9 microbubbles/mL) |
Riferimenti
- Durukan, A., Tatlisumak, T. Acute ischemic stroke: overview of major experimental rodent models, pathophysiology, and therapy of focal cerebral ischemia. Pharmacology Biochemistry and Behavior. 87 (1), 179-197 (2007).
- Vander Worp, H. B., van Gijn, J. Clinical Practice. Acute ischemic stroke. The New England Journal of Medicine. 357 (6), 572-579 (2007).
- Tannenbaum, J., Bennett, B. T. Russell and Burch’s 3Rs then and now: the need for clarity in definition and purpose. Journal of the American Association for Laboratory Animal Science. 54 (2), 120-132 (2015).
- Hochrainer, K., Yang, W. Stroke proteomics: from discovery to diagnostic and therapeutic applications. Circulation Research. 130 (8), 1145-1166 (2022).
- Wang, L. V., Yao, J. A practical guide to photoacoustic tomography in the life sciences. Nature Methods. 13 (8), 627-638 (2016).
- Aldrich, J. E. Basic physics of ultrasound imaging. Critical Care Medicine. 35 (5), S131-S137 (2007).
- Jacques, S. L. Optical properties of biological tissues: a review. Physics in Medicine and Biology. 58 (11), R37-R61 (2013).
- Li, M., Tang, Y., Yao, J. Photoacoustic tomography of blood oxygenation: a mini review. Photoacoustics. 10, 65-73 (2018).
- Menozzi, L., Yang, W., Feng, W., Yao, J. Sound out the impaired perfusion: Photoacoustic imaging in preclinical ischemic stroke. Frontiers in Neuroscience. 16, 1055552 (2022).
- Gessner, R. C., Frederick, C. B., Foster, F. S., Dayton, P. A. Acoustic angiography: a new imaging modality for assessing microvasculature architecture. International Journal of Biomedical Imaging. 2013, 936593 (2013).
- Dayton, P. A., Rychak, J. J. Molecular ultrasound imaging using microbubble contrast agents. Frontiers in Bioscience. 12, 5124-5142 (2007).
- Isayama, K., Pitts, L. H., Nishimura, M. C. Evaluation of 2, 3, 5-triphenyitetrazolium chloride staining to delineate rat brain infarcts. Stroke. 22 (11), 1394-1398 (1991).
- Ruan, J., Yao, Y. Behavioral tests in rodent models of stroke. Brain Hemorrhages. 1 (4), 171-184 (2020).
- Parthasarathy, A. B., Kazmi, S. M. S., Dunn, A. K. Quantitative imaging of ischemic stroke through thinned skull in mice with Multi Exposure Speckle Imaging. Biomedical Optics Express. 1 (1), 246-259 (2010).
- Hingot, V., et al. Early ultrafast ultrasound imaging of cerebral perfusion correlates with ischemic stroke outcomes and responses to treatment in mice. Theranostics. 10 (17), 7480-7491 (2020).
- Menozzi, L., et al. Three-dimensional non-invasive brain imaging of ischemic stroke by integrated photoacoustic, ultrasound and angiographic tomography (PAUSAT). Photoacoustics. 29, 100444 (2022).
- Llovera, G., Roth, S., Plesnila, N., Veltkamp, R., Liesz, A. Modeling stroke in mice: permanent coagulation of the distal middle cerebral artery. Journal of Visualized Experiments. (89), e51729 (2014).
- Trotman-Lucas, M., Kelly, M. E., Janus, J., Fern, R., Gibson, C. L. An alternative surgical approach reduces variability following filament induction of experimental stroke in mice. Disease Models & Mechanisms. 10 (7), 931-938 (2017).
- Labat-Gest, V., Tomasi, S. Photothrombotic ischemia: a minimally invasive and reproducible photochemical cortical lesion model for mouse stroke studies. Journal of Visualized Experiments. (76), e50370 (2013).
- Matsumoto, Y., et al. Visualising peripheral arterioles and venules through high-resolution and large-area photoacoustic imaging. Scientific Reports. 8 (1), 14930 (2018).
- Xu, Y., Wang, L. V., Ambartsoumian, G., Kuchment, P. Reconstructions in limited-view thermoacoustic tomography. Medical Physics. 31 (4), 724-733 (2004).
- Yal Tang, ., et al. High-fidelity deep functional photoacoustic tomography enhanced by virtual point sources. Photoacoustics. 29, 100450 (2023).
- Zheng, W., Huang, C., Zhang, H., Xia, J. Slit-based photoacoustic tomography with co-planar light illumination and acoustic detection for high-resolution vascular imaging in human using a linear transducer array. Biomedical Engineering Letters. 12 (2), 125-133 (2022).
- Wang, Y., et al. Slit-enabled linear-array photoacoustic tomography with near isotropic spatial resolution in three dimensions. Optics Letters. 41 (1), 127-130 (2016).
- Vu, T., Li, M., Humayun, H., Zhou, Y., Yao, J. A generative adversarial network for artifact removal in photoacoustic computed tomography with a linear-array transducer. Experimental Biology and Medicine. 245 (7), 597-605 (2020).
- Zhang, H., et al. Deep-E: A fully-dense neural network for improving the elevation resolution in linear-array-based photoacoustic tomography. IEEE Transactions on Medical Imaging. 41 (5), 1279-1288 (2022).
- Hauptmann, A., et al. Model-based learning for accelerated, limited-view 3-D photoacoustic tomography. IEEE Transactions on Medical Imaging. 37 (6), 1382-1393 (2018).
- Li, M., et al. Three-dimensional deep-tissue functional and molecular imaging by integrated photoacoustic, ultrasound, and angiographic tomography (PAUSAT). IEEE Transactions on Medical Imaging. 41 (10), 2704-2714 (2022).

