Real-Time Dynamic Navigation System for the Precise Quad-Zygomatic Implant Placement in a Patient with a Severely Atrophic Maxilla
Summary
Here, we present a protocol to achieve precise quad-zygomatic implant placement in patients with severely atrophic maxilla using a real-time dynamic navigation system.
Abstract
Zygomatic implants (ZIs) are an ideal way to address cases of a severely atrophic edentulous maxilla and maxilla defects because they replace extensive bone augmentation and shorten the treatment cycle. However, there are risks associated with the placement of ZIs, such as penetration of the orbital cavity or infra-temporal fossa. Furthermore, the placement of multiple ZIs makes this surgery risky and more difficult to perform. Potential intraoperative complications are extremely dangerous and may cause irreparable losses. Here, we describe a practical, feasible, and reproducible protocol for a real-time surgical navigation system for precisely placing quad-zygomatic implants in the severely atrophic maxilla of patients with residual bone that does not meet the requirements of conventional implants. Hundreds of patients have received ZIs at our department based on this protocol. The clinical outcomes have been satisfactory, the intraoperative and postoperative complications have been low, and the accuracy indicated by infusion of the designed image and postoperative three-dimensional image has been high. This method should be utilized during the entire surgical procedure to ensure ZI placement safety.
Introduction
In the 1990s, Branemark introduced an alternative technique for bone grafting, the zygomatic implant (ZI), which has also been called the zygomaticus fixture1. It was initially used for the treatment of trauma victims and patients with tumor resection where there was a defect in the maxillary structure. After maxillectomy, many patients retained anchorage only in the body of the zygoma or in the frontal extension of the zygomatic bone1,2,3.
More recently, the ZI technique has been widely used in edentulous and dentate patients with a severely resorbed maxilla. The main indication for ZI implants is an atrophic maxilla. The use of four ZIs in an immediate loading system (fixed prosthodontics) is practical for surgeons with broad clinical experience, and it appears to represent an excellent alternative method to bone graft techniques2,4. However, there are risks when placing ZIs, either by freehand or using a surgical template for guidance. Risks include inaccurate placement within the alveolus, penetration of the orbital cavity or infra-temporal fossa, and inappropriate placement within the zygomatic prominence5. The placement of multiple ZIs makes this surgery risky and difficult to perform. Hence, improving the precision of ZI placement is critical to its clinical use and safety.
The real-time surgical navigation system provides a different approach. It provides real-time and completely visualized trajectories through the analysis of preoperative and intraoperative computed tomography images. With the real-time navigation system, both precision and safety have been improved with sophisticated surgery and treatment5,6. A practical, feasible, and reproducible protocol was developed using the real-time surgical navigation system to precisely place ZIs in the severely atrophic maxilla5,7,8,9,10. With this protocol, we have treated hundreds of patients with satisfactory clinical outcomes5,6,7,8,9,10. Here, we present the protocol with the detailed information on the treatment procedure.
Protocol
All of the clinical protocols were approved by the Medical Ethics Review Committee of the Shanghai Ninth People's Hospital, Shanghai Jiao Tong University, School of Medicine (SH9H-2020-T29-3).
1. Patient selection
- The patient inclusion criteria were as follows (Table 1).
- Ensure that the patient presents a completely edentulous maxilla or partially edentulous maxilla with few extremely loose teeth (Figure 1A-G).
- Ensure that the patient has severe atrophy of the maxilla and insufficient bone volume for conventional implant placement in the anterior and/or posterior maxilla.
- Ensure that the patient is aged within 18-80 years and does not have systemic disease.
- Ensure that the patient has undergone cone beam computed tomography (CBCT) with analyzed DICOM data9.
NOTE: The preoperative CBCT is obtained using a commercial instrument with the following scanning parameters: 7.1 mA, 96 kV, 0.4 mm voxel size, field of view of 23 cm (D) x 26 cm (H), and scan time of 18 s.- Using a planning software, confirm that the maxillary posterior bone height ranges from 1 to 3 mm in the premolar and molar regions (Cawood and Howell Class VI)11 (Table 2).
- Ensure that the measured anterior maxilla has an insufficient width to place regular implants of at least 3.75 mm diameter without additional bone grafting or insufficient height to allow the placement of implants shorter than 10 mm even with a titled approach7,12,13 (Figure 1G1-G6).
NOTE: The bone thickness for placing the apex of the ZI should at least be 5.75 mm14 (Fig. 2A – B) (Table 1).
- The patient exclusion criteria were as follows (Table 1).
- Sufficient bone for conventional implant treatment.
- Narrow residual bone for which buccal bone graft is considered more appropriate.
- Untreated maxillary sinusitis or a maxillary sinus cyst.
- Local or systemic contraindications for oral surgery and implant placement.
- For edentulous patients, the maxillary residual bone volume does not meet the standard of classes V or VI of the Cawood Howell classification11.
2. Mini-screw implantation
- Administer local anesthesia to anesthetize the patient's maxilla, bilateral maxillary tuberosity, midline palatine suture, and both sides of the anterior nasal spine.
- Implant seven to eight mini-screws (diameter: 1.0 mm, length: 9.0 mm, square cavity: 1.0 mm) in the remaining maxilla under local anesthesia to act as registration points before trajectories planning in the bilateral tubera maxillae, midline palatine suture, and nasospinale.
- Select the bilateral maxillary tuberosity, midline palatine suture, and both sides of the anterior nasal spine as the bone anchorage areas for fiducials (Figure 3A-C).
NOTE: To increase the navigation accuracy, the mini-screws should be evenly and dispersedly placed in the indicated area.
3. Preoperative CBCT scanning for planning
- Perform CBCT using the following scanning parameters: 7.1 mA, 96 kV, 0.4 mm voxel size, field of view 23 cm (D) x 26 cm (H), and scan time of 18 s.
4. Setting registration points
- Import CBCT data into the presurgical planning software through the DVD drive.
- Mark all mini-screws as registration points for intraoperative imaging registration (Figure 3D).
- Mark the points on the central surface of the titanium mini-screws; this has to be set in a certain sequence.
NOTE: After the registration points are set, ensure that the intraoral coronal entrance points of the ZI are at or near the alveolar crest with the reference to the zygomatic anatomy-guided approach proposed by Carlos Aparicio15. The anterior ZI should be at the level of the lateral incisor/canine region and the posterior ZI in the second premolar/the first molar region. The apex of the mesial implant should be placed above that of the distal implant. According to the previous research, the posterosuperior region and the center of the zygoma were the ideal places for the apex of the mesial implant and the apex of the distal implant16. The length could only be chosen in the range of 30.0 to 52.5 mm. Cylindroid trajectories can be planned as the drilling path (Figure 3E-K).
- Mark the points on the central surface of the titanium mini-screws; this has to be set in a certain sequence.
5. Planning for quad-ZI surgery
NOTE: This protocol requires the navigation system.
6. Surgical procedure
- Lay the patient on the operating table in the supine position after general anesthesia.
NOTE: It is best to situate the patient in this position before he or she is placed under general anesthesia. Otherwise, it is difficult to switch the position. - Fixed skull reference: Rigidly secure the skull reference base to the calvaria with a single self-tapping titanium screw of 1.5 x 6 mm. Secure the reference array to the base and assemble with three marked reflective spheres (Figure 4A-C). Place the navigation system camera in the 1 o'clock position to monitor the skull reference.
- Registration: Specifically set the navigation system to the individual patient using a positioning probe with a tailor-made reflective ball to contact the outer surface of the mini-screws one after another. Then, display the available sagittal, coronal, axial, and 3D reconstruction images on the navigation screen (Figure 4D-E).
NOTE: After the registration procedure, check every fiducial marker for precision. The result is acceptable if the error is mostly <1.0 mm. Otherwise, the registration procedure should be repeated until the error becomes acceptable. - Standardization: Standardize the drilling before using it in the surgery. Use a calibration block with holes of different diameters to standardize the drill: diameter 2.5 mm (round bur), 2.9 mm (pilot drill), and 3.5 mm (expending drill). The drills should be straightly attached to the bottom of the block by the surgeon, and then the assistant needs to adjust the interface into the calibration module. The equipment will produce a sound once the process is complete.
- Gingiva flap opening: Determine the extent of the incision with the guidance of surgical navigation. Lift the full thickness flap to allow an adequate view for exposing the planned implant sites.
NOTE: The range of the periosteal elevation should contain the alveolar crest, lateral wall of the maxilla, and the inferior border of the zygomatic bone. - Entrance point marking: First, find the entry point with the help of the navigation probe. Then, use the zygoma handpiece to fix the entry points. Next, find the entry of the zygomatic bone with the probe. Use the zygoma handpiece to prepare the entry point of the zygomatic bone (Figure 4F-G).
NOTE: Ensure that both the operator and the assistants pay attention to the real surgical area to prevent errors made by the navigation system. - Initial preparation: Perform the drilling procedure ensuring that it follows the trajectories from the entry to the exit point as planned. Use the 2.9 mm drill first to prepare the path from the entry point, which was located using the navigation probe, to the entry of the zygomatic bone. Prepare the mesial one first, followed by the distal one.
NOTE: Check each step with the navigation probe to confirm that the path is correct according to the designed preoperative plan (Figure 4H-I). - Widen the implant bed: Use the handpiece to extend the path from the entrance of the zygomatic bone to the terminal point designed at the surface of the zygomatic bone.
NOTE: Ask the assistant to put a hand on the surface of the lateral orbital wall to ensure its safety. Ensure that the surgeon pays attention to the navigation screen rather than the surgical area. - Readings and measurements: Enlarge the trajectory with an expanding drill having a 3.5 mm diameter. Use the measuring bar and navigation probe to check the direction and position of the trajectory. Identify the length of the implant using the measuring tool (Figure 4B).
NOTE: If the depth does not meet the requirement of the planned length, it is better to prepare it to the set depth. - Implantation: Implant the ZIs using a specific manual tool.
- Suturing: After ZI implantation, use the navigation probe to verify correct positioning. Place multi-unit abutments and healing caps on the implants and suture the incision with polypropylene 4-0 suture. The hairline incision should also be sutured after the reference frame is removed.
7. Postoperative medication
- Administer the patient a 5-day prescription of antibiotics, analgesics, and mouthwash solution (chlorhexidine 0.12%).
8. Immediate restoration
- Perform immediate restoration in the patient within 72 h (Figure 5C-G).
9. Image integration
- Obtain postoperative CBCT scanning images and a panoramic radiograph to evaluate the ZI position within 72 h after surgery (Figure 5A-B). Export the postoperative data to the planning software to superimpose the image of the post-operative CBCT and the preoperative surgical plan comparing the location of the entrance point, end point, and angular deviation (Figure 5H-I, Table 4).
Representative Results
The enrolled patient was a 60-year-old woman without any systematic diseases (Figure 1A–D, F). After CBCT scanning, the alveolar ridge in the anterior maxilla was less than 2.9 mm, while the residual bone height in the posterior maxilla region was less than 2.4 mm (Figure 1E, G and Table 1). The width and thickness of the zygomatic bone were approximately 22.4-23.6 mm and 6.1-8.0 mm (Figure 2, Table 3), respectively. According to the Zygoma Anatomy-Guided Approach, the entrance of the anterior ZI was at the level of the canine region, and the posterior ZI was in the second premolar (Figure 3E). The distance between the margin of the anterior ZI and the orbit was 5.2 mm on the right and 3.6 mm on the left, while the distance between the margin of the posterior ZI and the pterygopalatine fossa was 2.9 mm on the right and 4.3 mm on the left (Figure 3F–K).
The surgery was performed using the navigation system (Figure 4A–G). After surgery, the patient received a temporary restoration within 3 days, which addressed both the aesthetic and pronunciation issues (Figure 5C–G). Postoperative CBCT scanning and image integration showed that the errors of the entrance from the left posterior ZI to the left anterior ZI, then to the right anterior ZI, and last to the right posterior ZI were 1.25 mm, 1.35 mm, 1.35 mm, and 1.85 mm, respectively. The errors of the target from the left posterior ZI to the right posterior ZI were 2.25 mm, 1.55 mm, 2.40 mm, and 1.20 mm, respectively. The errors of the ZI angle were 3.50°, 3.59°, 3.20°, and 2.15°, respectively (Figure 5H–I, Table 4).
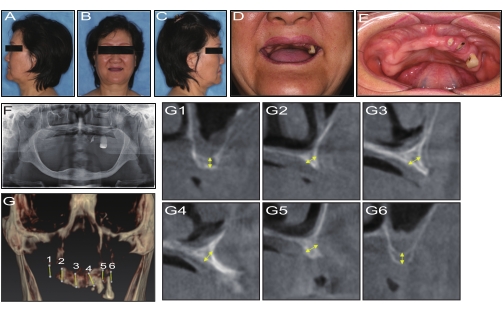
Figure 1: Preoperative examination. (A,C) Preoperative profile view. (B) Preoperative frontal image. (D) Frontal image of the smile line. (E) Intraoral view of the maxilla. (F) Preoperative panoramic radiograph. (G1–6) CBCT curve section. Please click here to view a larger version of this figure.
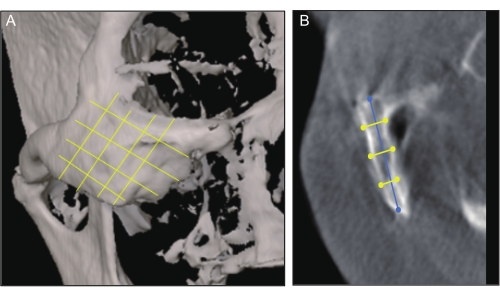
Figure 2: CT measurement. (A) Skull frontal view showing the zygoma divided into superior, middle, and inferior parts by the cross line. (B) Longitudinal tomography showing the measurements of the zygomatic thickness (yellow line) and length (blue line). Please click here to view a larger version of this figure.
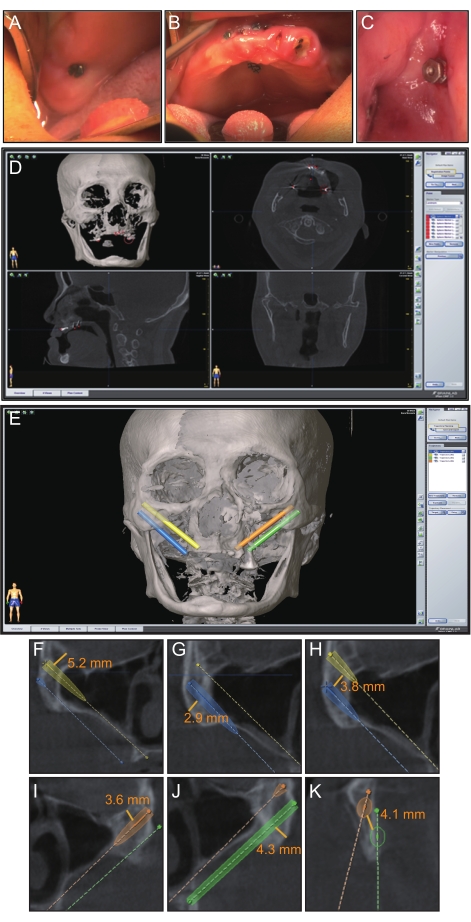
Figure 3: Preoperative planning. (A–C) Eight miniscrews were dispersedly implanted in the remaining maxilla to be registered. (D) Preoperative registration point settings on the navigation software. (E) Preoperative implant planning on the navigation software. (F–K) Distances for ZI planning. Please click here to view a larger version of this figure.
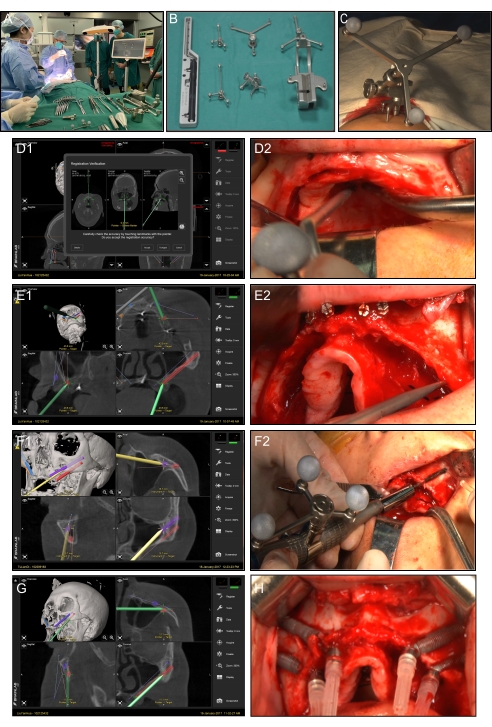
Figure 4: Navigation surgery. (A) Navigation surgery scene. (B) Navigation surgical tools. (C) Cephal bracket mounted to the patient's head for the purpose of tracking. (D1) Screen view of the navigation probe registration application in the sagittal coronal axial. (D2) Intraoral view of the navigation probe application. (E1) Screen view of the entry point location procedure using the navigation probe. (E2) Intraoral view of the procedure using the navigation probe. (F1,F2) Constant visualization of the drilling trajectory displayed on the screen in real-time. The entire procedure from the entry point to the exit point. (G) Screen view of the ZI position verification using the navigation probe. (H) Accomplishment of ZI placement. Please click here to view a larger version of this figure.
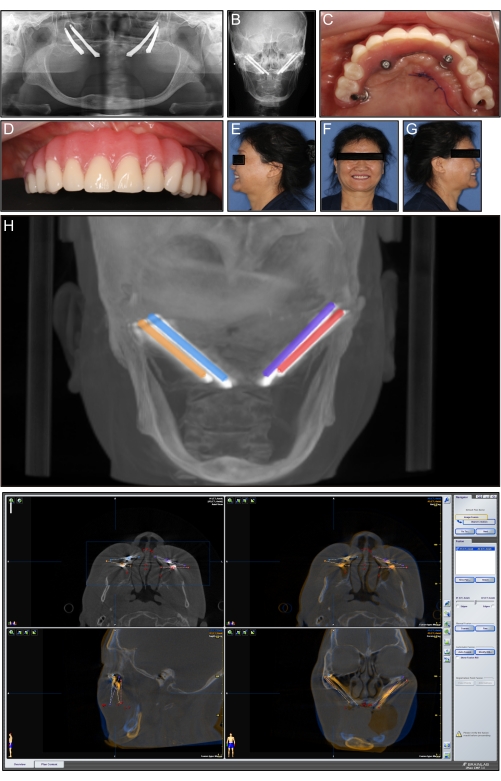
Figure 5: Postoperative view and image infusion. (A) Postoperative panoramic radiograph. (B) Postoperative frontal cephalometrics. (C) Intraoral view of the immediate temporary restoration. (D) Anterior view of the immediate temporary restoration. (E) Postoperative profile view after the immediate temporary restoration. (F) Frontal image after the immediate temporary restoration. (G) Postoperative profile view after the immediate temporary restoration. (H) Preoperative image integrated with the postoperative image, and measurement of the planned-placed deviations of implants. (I) Postoperative CBCT image integration observed in sagittal, coronal, and axial view. Please click here to view a larger version of this figure.
| Inclusion criteria | Exclusion criteria |
| 1. Completely edentulous maxilla or be going to be edentulous maxilla | 1. Sufficient bone for conventional implant treatment |
| 2. Severe atrophy of the maxilla | 2. Bone graft was considered more appropriate |
| 3. Age range from 18-80 | 3. Untreated maxillary sinusitis |
| 4. Insufficient width for anterior maxilla to place regular implants of at least 3.75 mm | 4. Local or systemic contraindications for oral surgery |
| 5. Maxillary posterior bone height ranging from 1 to 3 mm in the premolar and molar regions | 5. A medication history of bisphosphonates |
| 6. The bone thickness for placing the apex of the ZI was at least 5.75 mm |
Table 1: Patient inclusion and exclusion criteria.
| Anterior region width (mm) | Pre-molar region width (mm) | Molar region height (mm) | |
| Left | 2.8 | 2.5 | 2.4 |
| Right | 2.9 | 2.9 | 2.2 |
Table 2: Differences in alveolar bone thickness at points on the anterior region, and residual alveolar bone height at points on the premolar region and molar regions.
| Zygomatic bone thickness (mm) | Zygomatic bone width (mm) | |||||
| Superior | Middle | Inferior | Superior | Middle | Inferior | |
| Left | 7.4 | 5.3 | 7.8 | 23 | 23.6 | 24.1 |
| Right | 8 | 6.1 | 5.7 | 22.4 | 23.1 | 25.9 |
Table 3: Differences in zygomatic thicknesses at points on the superior, middle, and inferior areas.
| Starting position error (mm) | Teminal position error (mm) | Angular deviation (°) | |
| Distal of the left ZI | 1.25 | 2.25 | 3.5 |
| Mesial of the left ZI | 1.35 | 1.55 | 3.95 |
| Mesial of the right ZI | 1.35 | 2.4 | 3.2 |
| Distal of the right ZI | 1.85 | 1.2 | 2.15 |
Table 4: Resulting deviation of four zygomatic implants.
Discussion
Reconstructive rehabilitation of the atrophic maxilla using grafts is difficult because it requires good surgical technique, coverage of high-quality soft tissue over the graft, a significant amount of patient cooperation, and patients with health favorable for the finial restoration17,18. The placement of dental implants for reconstruction in patients with maxillary atrophy represents a significant clinical challenge. The pattern of facial bone resorption is associated with age and is especially evident in the edentulous maxilla, and particularly more noticeable in those using complete removable prostheses19,20. Thus, the development of the ZI represents an effective alternative for cases involving tumors, trauma, and ectodermal dysplasia. The main advantage of this technique is that it only requires one surgical approach, thus reducing the number of treatment stages and achieving the goal of immediate restoration. The immediate loading procedure also results in greater esthetic and functional patient satisfaction because in this technique, there is no edentulous mouth phase. After implant placement, restoration is performed immediately21. It also avoids the need for further bone-harvesting surgeries in donor sites22,23. It achieves stable bone anchorage in the zygomatic bone within the posterior maxilla region, which has bone quality type IV that does not allow the insertion of standard implants, through the addition of two to four standard implants in the anterior region or via the quadruple ZI approach24,25. Presently, the indication of this surgical technique has been applied to cases of trauma, severe periodontitis, and ectodermal dysplasia.
The ZI margin should be at a safe distance from important anatomic landmarks, such as the orbit and pterygopalatine fossa, and also for the interval between the two ZIs to ensure adjacent tissue impregnability andstabile implant osseointegration22. In some cases, computer-based guides, which are tailored planned for each patient, may have flaws that reduce their accuracy2,26. A real-time surgical navigation system could be applied to guide the drilling and placement of ZIs. With the assistance of the surgical navigation system, the incision extent can be limited, to some extent, to around the operated area. Moreover, drilling along the trajectory can avoid neighboring critical structures, such as the orbital cavity and infratemporal fossa, decreasing the risk of intraoperative complications and simplifies the operation.
In this case report, a passive optical dynamic navigation system was utilized requiring the use of fiducial markers firmly attached to the patient's dental arch during CBCT scanning27. A large number of implant placement-related studies, including the quad-approach for ZI placement and three ZIs studies, have shown the effective minimization of planned-placed deviations indirectly by reporting the reduction of intraoperative and post-operative complications with the assistance of the real-time surgical navigation system8,10,28,29,30,31. However, in these previous studies, more than six fiducial markers with a polygonal distribution were implemented by the operators before surgery. This meant that the bilateral maxillary tuberosity, the midline palatine suture, and both sides of the anterior nasal spine were selected as the area for titanium mini-screw anchorage32. Furthermore, all of the fiducial markers were recommended to be bone anchored to more than one titanium screw in each of the regions to ensure precise registration accuracy. It also avoided screws splitting off or moving during the open-flap surgery.
Another important procedure is the verification of error. The importance of the precision verification throughout the entire surgery cannot be overemphasized. Verification can be divided into four levels. The first level is the verification after the navigation registration procedure. The second level is the verification when locating the entry point on both the alveolar crest and the zygomatic bone. The third level is the verification during the drilling procedure with the zygomatic handpiece. The fourth level is the verification after ZI implementation to ensure accurate ZI position and direction. Furthermore, throughout the procedure, navigation calibration is also very important. Finally, both the operator and the surgical assistant should pay attention to the reference frame to ensure its stability, because any slight touch will likely affect the surgical navigation.
In the present case report, deviations generally appeared to be greater when the implants were placed in distal locations or with the placement of long implants33,34. Throughout the process, it was easy to locate the ZIs and it was safer to implant them by means of the real-time navigation system. Although the entry deviation, exit deviation, and angle deviations were limited under the guidance of the real-time surgical navigation system for ZI placement, it should be utilized during the entire surgical procedure to ensure safety.
Disclosures
The authors have nothing to disclose.
Acknowledgements
The authors thank Dr. Shengchi Fan for kindly providing valuable navigation technical support. This case report was funded by the Key project of China's Ministry of Science and Technology (2017YFB1302904), the Natural Science Foundation of Shanghai (No. 21ZR1437700), the Clinical research plan of SHDC (SHDC2020CR3049B), and the Combined Engineering and Medical Project of Shanghai Jiao Tong University (YG2021QN72).
Materials
| Bistoury scalpel | Hufriedy Group | 10-130-05 | |
| Branemark system zygoma TiUnite RP 35mm | Nobel Biocare AB | 34724 | TiUnite implant with overlength to place from the maxilla to the zygoma |
| Branemark system zygoma TiUnite RP 40mm | Nobel Biocare AB | 34735 | TiUnite implant with overlength to place from the maxilla to the zygoma |
| Branemark system zygoma TiUnite RP 42.5mm | Nobel Biocare AB | 34736 | TiUnite implant with overlength to place from the maxilla to the zygoma |
| Branemark system zygoma TiUnite RP 45mm | Nobel Biocare AB | 34737 | TiUnite implant with overlength to place from the maxilla to the zygoma |
| Branemark system zygoma TiUnite RP 47.5mm | Nobel Biocare AB | 34738 | TiUnite implant with overlength to place from the maxilla to the zygoma |
| Branemark system zygoma TiUnite RP 50mm | Nobel Biocare AB | 34739 | TiUnite implant with overlength to place from the maxilla to the zygoma |
| Branemark system zygoma TiUnite RP 52.5mm | Nobel Biocare AB | 34740 | TiUnite implant with overlength to place from the maxilla to the zygoma |
| CBCT | Planmeca Oy,Helsinki, Finland | Pro Max 3D Max | |
| connection to handpiece | Nobel Biocare AB | 29081 | the accessories to connect the intrument |
| Drill guard | Nobel Biocare AB | 29162 | the accessories to protect the lips and soft tissue during the surgery |
| Drill guard short | Nobel Biocare AB | 29162 | the accessories to protect the lips and soft tissue during the surgery |
| Handpiece zygoma 20:1 | Nobel Biocare AB | 32615 | the basic instrument for implant drill |
| Instrument adapter array size L | BRAINLAB AG | 41801 | |
| Instrument adapter array size M | BRAINLAB AG | 41798 | |
| Instrument calibration matrix | BRAINLAB AG | 41874 | a special tool for drill to calibration |
| I-plan automatic image fusion software STL data import/export for I-plan VectorVision2®, (I-plan CMF software) | BRAINLAB AG | inapplicability | the software for navigation surgery planning |
| Multi-unit abutment 3mm | Nobel Biocare AB | 32330 | the connection accessory between the implant and the titanium base |
| Multi-unit abutment 5mm | Nobel Biocare AB | 32331 | the connection accessory between the implant and the titanium base |
| Periosteal elevator | Hufriedy Group | PPR3/9A | the instrument for open flap surgery |
| Pilot drill | Nobel Biocare AB | 32630 | the drill for the surgery |
| Pilot drill short | Nobel Biocare AB | 32632 | the drill for the surgery measuring the depth of the implant holes |
| Pointer with blunt tip for cranial/ENT | BRAINLAB AG | 53106 | |
| Reference headband star | BRAINLAB AG | 41877 | |
| Round bur | Nobel Biocare AB | DIA 578-0 | the drill for the surgery |
| Screwdriver manual | Nobel Biocare AB | 29149 | |
| Skull reference array | BRAINLAB AG | 52122 | a special made metal reference for navigation camera to receive the signal |
| Skull reference base | BRAINLAB AG | 52129 | |
| Suture vicryl 4-0 | Johnson &Johnson, Ethicon | VCP310H | |
| Temporary copping multi-unit titanium (with prosthetic screw) | Nobel Biocare AB | 29046 | the temporary titanium base to fix the teeth |
| Titanium mini-screw | CIBEI | MB105-2.0*9 | the mini-screw for navigation registration |
| Twist drill | Nobel Biocare AB | 32628 | the drill for the surgery |
| Twist drill short | Nobel Biocare AB | 32629 | the drill for the surgery |
| Zygoma depth indicator angled | Nobel Biocare AB | 29162 | |
| Zygoma depth indicator straight | Nobel Biocare AB | 29162 | the measurement scale for |
| Zygoma handle | Nobel Biocare AB | 29162 | the instrument for zygomatic implant placement |
References
- Francischone, C. L., Vasconcelos, L. W., Filho, H. N., Francischone, C. E., Sartori, I. M. Chapter 15. The zygoma fixture. The osseointegration book. From calvarium to calcaneus. , 317-320 (2005).
- Weischer, T., Schettler, D., Mohr, C. Titanium implants in the zygoma as retaining elements after hemimaxillectomy. The International Journal of Oral & Maxillofacial Implants. 12 (2), 211-214 (1997).
- Jensen, O. T., Brownd, C., Blacker, J. Nasofacial prostheses supported by osseointegrated implants. The International Journal of Oral & Maxillofacial Implants. 7 (2), 203-211 (1992).
- Duarte, L. R., Filho, H. N., Francischone, C. E., Peredo, L. G., Branemark, P. I. The establishment of a protocol for the total rehabilitation of atrophic maxillae employing four zygomatic fixtures in an immediate loading system–a 30-month clinical and radiographic follow-up. Clinical Implant Dentistry and Related Research. 9 (4), 186-196 (2007).
- Hung, K. F., et al. Accuracy of a real-time surgical navigation system for the placement of quad zygomatic implants in the severe atrophic maxilla: A pilot clinical study. Clinical Implant Dentistry and Related Research. 19 (3), 458-465 (2017).
- Wu, Y., Wang, F., Huang, W., Fan, S. Real-time navigation in zygomatic implant placement: Workflow. Oral and Maxillofacial Surgery Clinics of North America. 31 (3), 357-367 (2019).
- Wang, F., et al. Reliability of four zygomatic implant-supported prostheses for the rehabilitation of the atrophic maxilla: a systematic review. The International Journal of Oral & Maxillofacial Implants. 30 (2), 293-298 (2015).
- Xiaojun, C., et al. An integrated surgical planning and virtual training system. IEEE 2010 International Conference on Audio, Language and Image Processing (ICALIP). , 1257-1261 (2010).
- Fan, S., et al. The effect of the configurations of fiducial markers on accuracy of surgical navigation in zygomatic implant placement: An in vitro study. The International Journal of Oral & Maxillofacial Implants. 34 (1), 85-90 (2019).
- Xiaojun, C., Ming, Y., Yanping, L., Yiqun, W., Chengtao, W. Image guided oral implantology and its application in the placement of zygoma implants. Computer Methods and Programs in Biomedicine. 93 (2), 162-173 (2009).
- Cawood, J. I., Howell, R. A. A classification of the edentulous jaws. The International Journal of Oral & Maxillofacial Surgery. 17 (4), 232-236 (1988).
- Davo, R., Pons, O., Rojas, J., Carpio, E. Immediate function of four zygomatic implants: a 1-year report of a prospective study. European Journal of Oral Implantology. 3 (4), 323-334 (2010).
- Jensen, O. T. Complete arch site classification for all-on-4 immediate function. The Journal of Prosthetic Dentistry. 112 (4), 741-751 (2014).
- Triplett, R. G., Schow, S. R., Laskin, D. M. Oral and maxillofacial surgery advances in implant dentistry. The International Journal of Oral & Maxillofacial Implants. 15 (1), 47-55 (2000).
- Aparicio, C. A proposed classification for zygomatic implant patient based on the zygoma anatomy guided approach (ZAGA): a cross-sectional survey. European Journal of Oral Implantology. 4 (3), 269-275 (2011).
- Hung, K. F., et al. Measurement of the zygomatic region for the optimal placement of quad zygomatic implants. Clinical Implant Dentistry and Related Research. 19 (5), 841-848 (2017).
- Kahnberg, K. E., Nystrom, E., Bartholdsson, L. Combined use of bone grafts and Br fixtures in the treatment of severely resorbed maxillae. The International Journal of Oral & Maxillofacial Implants. 4 (4), 297-304 (1989).
- Nystrom, E., Kahnberg, K. E., Gunne, J. Bone grafts and Br implants in the treatment of the severely resorbed maxilla: A 2-year longitudinal study. The International Journal of Oral & Maxillofacial Implants. 8 (1), 45-53 (1993).
- Jensen, S. S., Terheyden, H. Bone augmentation procedures in localized defects in the alveolar ridge: Clinical results with different bone grafts and bone-substitute materials. The International Journal of Oral & Maxillofacial Implants. 24, 218-236 (2009).
- Bedrossian, E. Rehabilitation of the edentulous maxilla with the zygoma concept: A 7-year prospective study. The International Journal of Oral & Maxillofacial Implants. 25 (6), 1213-1221 (2010).
- Dhamankar, D., Gupta, A. R., Mahadevan, J. Immediate implant loading: A case report. Journal of Indian Prosthodontic Society. 10 (1), 64-66 (2010).
- Aparicio, C., et al. Zygomatic implants: indications, techniques and outcomes, and the zygomatic success code. Periodontol 2000. 66 (1), 41-58 (2014).
- Chrcanovic, B. R., Abreu, M. H. Survival and complications of zygomatic implants: A systematic review. Journal of Oral and Maxillofacial Surgery. 17 (2), 81-93 (2013).
- Brånemark, P. I., et al. Zygoma fixture in the management of advanced atrophy of the maxilla: Technique and long-term results. Scandinavian Journal of Plastic and Reconstructive Surgery and Hand Surgery. 38 (2), 70-85 (2004).
- Balshi, T. J., Wolfinger, G. J., Petropoulos, V. C. Quadruple zygomatic implant support for retreatment of resorbed iliac crest bone graft transplant. Implant Dentistry. 12 (1), 47-53 (2003).
- Chrcanovic, B. R., Oliveira, D. R., Custódio, A. L. Accuracy evaluation of computed tomography-derived stereolithographic surgical guides in zygomatic implant placement in human cadavers. The Journal of Oral Implantology. 36 (5), 345-355 (2010).
- Gellrich, N. C., et al. Computer-assisted secondary reconstruction of unilateral posttraumatic orbital deformity. Plast and Reconstructive Surgery. 110 (6), 1417-1429 (2002).
- Watzinger, F., et al. Placement of endosteal implants in the zygoma after maxillectomy: A Cadaver study using surgical navigation. Plast and Reconstructive Surgery. 107 (3), 659-667 (2001).
- Wagner, A., et al. Computer-aided placement of endosseous oral implants in patients after ablative tumour surgery: Assessment of accuracy. Clinical Oral Implants Research. 14 (3), 340-348 (2003).
- Casap, N., Wexler, A., Tarazi, E. Application of a surgical navigation system for implant surgery in a deficient alveolar ridge postexcision of an odontogenic myxoma. The Journal of Oral & Maxillofacial Surgery. 63 (7), 982-988 (2005).
- Pellegrino, G., Tarsitano, A., Basile, F., Pizzigallo, A., Marchetti, C. Computer-aided rehabilitation of maxillary oncological defects using zygomatic implants: A defect-based classification. The Journal of Oral & Maxillofacial Surgery. 73 (12), 1-11 (2015).
- Fan, S., et al. The effect of the configurations of fiducial markers on accuracy of surgical navigation in zygomatic implant placement: An in vitro study. The International Journal of Oral & Maxillofacial Implants. 34 (1), 85-90 (2019).
- D’Haese, J., Van De Velde, T., Elaut, L., De Bruyn, H. A prospective study on the accuracy of mucosally supported stereolithographic surgical guides in fully edentulous maxillae. Clinical Implant Dentistry and Related Research. 14 (2), 293-303 (2012).
- Stübinger, S., Buitrago-Tellez, C., Cantelmi, G. Deviations between placed and planned implant positions: an accuracy pilot study of skeletally supported stereolithographic surgical templates. Clinical Implant Dentistry and Related Research. 16 (4), 540-551 (2014).

