A Murine Model of Hemodialysis Access-Related Hand Dysfunction
Summary
This protocol details the surgical steps of murine common iliac arteriovenous fistula creation. We developed this model to study hemodialysis access-related limb pathophysiology.
Abstract
Chronic kidney disease is a major public health problem, and the prevalence of end-stage renal disease (ESRD) requiring chronic renal replacement therapies such as hemodialysis continues to increase. Autogenous arteriovenous fistula (AVF) placement remains a primary vascular access option for ESRD patients. Unfortunately, approximately half of the hemodialysis patients experience dialysis access-related hand dysfunction (ARHD), ranging from subtle paresthesia to digital gangrene. Notably, the underlying biologic drivers responsible for ARHD are poorly understood, and no adequate animal model exists to elucidate the mechanisms and/or develop novel therapeutics for the prevention/treatment of ARHD. Herein, we describe a new mouse model in which an AVF is created between the left common iliac artery and vein, thereby facilitating the assessment of limb pathophysiology. The microsurgery includes vessel isolation, longitudinal venotomy, creation of arteriovenous anastomosis, and venous reconstruction. Sham surgeries include all the critical steps except for AVF creation. Iliac AVF placement results in clinically relevant alterations in central hemodynamics, peripheral ischemia, and impairments in hindlimb neuromotor performance. This novel preclinical AVF model provides a useful platform that recapitulates common neuromotor perturbations reported by hemodialysis patients, allowing researchers to investigate the mechanisms of ARHD pathophysiology and test potential therapeutics.
Introduction
The establishment and preservation of functional vascular access remain an important primary goal for end-stage renal disease (ESRD) patients receiving renal replacement therapy via hemodialysis1. Repeated hemodialysis treatments are necessary to remove waste products, normalize electrolytes, and maintain fluid balance once kidney function becomes inadequate, and thus are necessary for long-term survival2. Therefore, vascular access represents a "lifeline" for patients with ESRD, and autogenous arteriovenous fistula (AVF) placement remains a preferred dialysis access option among this cohort3. However, approximately 30%-60% of hemodialysis patients experience a spectrum of hand disabilities, clinically defined as access-related hand dysfunction (ARHD). The symptoms of ARHD can range from weakness and discoordination to monoplegia and digital gangrene, which can occur early after AVF creation or develop gradually with fistula maturation. Further, ARHD complicates the ESRD treatment schedule, which is associated with poor quality of life, high risk of cardiovascular disease, and increased mortality2,3,4.
Several animal models have been developed to study vascular remodeling induced by hemodynamic alterations following AVF creation5,6,7,8,9,10,11,12,13,14,15. Large animal models with iliac or femoral AVF16,17,18,19,20 and rodent models using either carotid artery-jugular vein anastomosis or infrarenal aorta-inferior vena cava fistula formation are well established to examine the aforementioned aspects of AVF maturation and patency21. For example, venous hypertension, greater luminal diameter, and increased vein wall thickness are signatures of successful AVF maturation, whereas substantial fibrosis of the media and intimal hyperplasia or thrombus development with no changes in flow often characterize AVF failures6,15. However, large animal models lack the experimental flexibility or transgenic capabilities of murine models, while current rodent models do not readily facilitate the investigation of ARHD due to either the anatomic location and/or lack of associated limb pathology. Indeed, due to a lack of an established preclinical animal model that recapitulates the relevant clinical phenotype, research progress to elucidate the pathobiological mechanisms and develop novel therapeutic strategies has remained stagnant, despite a progressive increase in the number of symptomatic ARHD patients. Therefore, the primary aim of this study is to introduce a unique mouse model of ARHD, providing procedural steps of AVF microsurgery and characterization of AVF-related pathophysiology.
Protocol
All procedures were approved by the Institutional Animal Care and Use Committee (IACUC) of the University of Florida and Malcom Randall Veterans Affairs Medical Center.
NOTE: Young adult (8-10 weeks old) male C57BL/6J mice were purchased from The Jackson Laboratory and housed in a light (12 h light: 12 h dark cycle), temperature (22 °C ± 1 °C), and humidity (50% ± 10%) controlled animal facility. Five mice were allowed to dwell per cage (W:18 cm x L:29 cm x H:12.5 cm) with nesting materials, food, and water being made available ad libitum. Following 7 days of habitat acclimation with standard chow, the mice were changed to a casein-based chow diet for 7 days as a diet transition phase. Thereafter, mice were fed the casein-based chow with 0.2%-0.15% adenine supplementation for 2-3 weeks to induce renal dysfunction (CKD) prior to the AVF surgery as previously described22,23,24. Control mice received a casein-based chow diet without adenine supplementation (control). The control and CKD diets were maintained throughout the postoperative recovery period (POD).
1. Pre-operative measurements
- Assess baseline/pre-operative outcome measurements, aortoiliac vessel diameters and hemodynamic flow parameters using duplex ultrasound imaging and the hindlimb perfusion via laser Doppler as previously described25.
- Determine the unilateral hindlimb grip strength and treadmill gait appraisal to establish baseline hindlimb function as previously described25,26.
- Assess kidney function by measuring glomerular filtration rate (GFR) via FITC-inulin clearance and/or serum blood urea nitrogen (BUN) level as previously described22,24,27.
2. Surgical preparation
- Prepare the following surgical tools and supplies (Table of Materials): a hot bead sterilizer, eye lubricant, a pen trimmer, alcohol preps, chlorhexidine wipes, extra-fine Graefe forceps, sterilized 0.9% saline, 29 G and 31 G needle syringes, 2 x 2 non-woven sponges, medium single-ended round (SC-9) and small double-ended hard, sharp, pointed (SC-4) cotton swabs, low-temperature cautery, straight Dumont forceps, 45° angled Dumont forceps, straight Vannas spring scissors, curved Vannas spring scissors, round handled needle holders, multiple sizes of sutures (4-0 silk, 5-0 PGA, 6-0 silk, and 10-0 nylon sutures), heparin, absorbable gelatin sponge, a straight needle holder, and buprenorphine.
NOTE: Extremity fixing rubber bands and retractors for the abdomen and legs were handmade. - Sterilize surgical preps using autoclave with steam sterilization at 120-125 °C for 30 min followed by drying for 30 min prior to the surgery. Utilize 70% ethanol cleansing followed by hot bead sterilization (240-270 °C for 3 min) between each animal surgery.
- Prepare sterilized 0.9% normal saline, heparinized saline (100 IU/mL), and buprenorphine (0.01 mg/mL) using 29-31 G needle syringes.
3. Anesthesia and positioning
- Initiate mouse anesthesia in the induction chamber (0.8 mL/min, 2.5% isoflurane). Once the mouse is adequately anesthetized, place the mouse in a supine position on the surgery station covered by a sterile drape. Taper the isoflurane concentration down to ~1.2% during the shaving and positioning steps.
- Apply the ocular lubricant to protect the eyes from drying during the surgery.
- Using a pen trimmer, shave the abdominal hair for the operation and the leg hair for postoperative perfusion measurements. Clear the hair off the surgical field.
- Fixate the upper and lower extremities with rubber bands and tacks, check the depth of anesthesia by monitoring the toe pinch reflex, and titrate anesthesia as necessary. Perform the respiratory pattern evaluation every 3-5 min throughout the surgical procedure to calibrate the level of anesthesia.
4. Exploration of the surgical target area
- Clean the shaved skin area several times, alternating between alcohol prep and chlorhexidine wipes in a circular pattern to disinfect the surgical field.
- Make a midline laparotomy from the lower edge of the sternal margin to the pubis symphysis. Dissect out the pubis fat pad to obtain a wider operative field.
- Open the celiotomy to access the peritoneal contents with retractors and eviscerate the small and large intestines using medium, single-ended round cotton swabs. Cover the bowels with a saline-soaked non-woven sponge.
- Once adequate exposure of the retroperitoneal vasculature is obtained, cover the remaining bowel, kidneys, and ureters with small saline-soaked non-woven sponges. Evacuate a distended bladder by gently squeezing the bladder dome with medium, single-ended round cotton swabs as needed.
- Carefully dissect out the perivascular fascia and adipose tissue from approximately 1 cm proximal to the aortic bifurcation extending to the level of the left iliac bifurcation using straight Dumont forceps and small double-ended hard, sharp, pointed cotton swabs.
NOTE: The left iliac artery and vein are left adherent to one another while isolating the arteriovenous structures en masse. This step will provide sufficient vessel mobilization to facilitate AVF creation. - If any small venous branches are encountered originating from or converging with the left common iliac vein, ligate them using low-temperature cautery with or without 6-0 silk suture as needed.
- Pass the tip of the angled forceps under the left common iliac vascular bundle and gently spread multiple times to mobilize the vessels from the underlying retroperitoneal musculature (Figure 1A).
5. Creation of a common iliac arteriovenous fistula anastomosis
- Place two 4-0 silk sutures around the isolated left common iliac arteriovenous bundle and use them as ligatures (e.g., cross-clamps) to the vascular bundle. Create a single knot with each 4-0 silk tie and apply them sequentially from proximal to distal.
- Make sure that the silk-tie cross-clamps are placed sufficiently far apart to isolate ~2 mm of vessel length, and the sequential application of the suture ligatures will precipitate left iliac vein engorgement.
- Using the 4-0 silk suture strings as handles, rotate the left iliac arteriovenous vascular bundle clockwise and fine-tune the position to temporarily locate the vein anterior to the artery (Figure 1B).
- Make a longitudinal venotomy (~1 mm) with straight Vannas spring scissors and gently flush out residual blood from the venous lumen with 0.9% saline (Figure 1C). Use caution during this step, as a high-pressure saline flush can cause venous disruption.
NOTE: The region of red color that remains in the iliac artery after venous flushing provides a visual window for the following step. - Place an imbricating 10-0 nylon suture through the posterior wall of the vein.
NOTE: This portion of the iliac vein should be in immediate apposition to the anterior wall of the iliac artery, and the walls are naturally adherent. The suture should go through both walls and tie the suture down with a single knot (Figure 1D). Note that a small amount of bleeding, which originates from the stagnant blood in the iliac artery, will appear once the needle passes through both walls. If intra-luminal bleeding continues during this step, the silk suture cross-clamps may be too loose and need to be further tightened. - Grasp the imbricated suture ends and place them under gentle tension to displace the anterior wall from the posterior wall of the iliac artery. Make a ~1.0 mm x 0.3 mm elliptical incision using curved Vannas spring scissors, removing the adherent walls of both the iliac artery and vein.
NOTE: The arteriovenous fistula is thereby created once this common channel is established. It is possible to injure the lateral walls of the vein during this step as the posterior iliac vein/anterior iliac artery wall incision is performed through venotomy exposure. Caution should be taken to avoid this complication as this can considerably reduce the fistula diameter and lead to thrombus development. - Gently flush out residual blood of the exposed arterial lumen with 0.9% saline and heparinized saline (100 IU/mL)28 (Figure 1E).
- Following the creation of the AVF, repair the initial anterior wall venotomy using two or three 10-0 nylon sutures in an interrupted fashion (Figure 1F).
- Restore the vascular bundle to its original anatomic orientation and place a small piece of saline-soaked absorbable gelatin sponge adjacent to the repaired venotomy to facilitate hemostasis.
- Loosen the 4-0 single-knot cross-clamp ligatures sequentially from distal to proximal. Monitor the venotomy site closely for excessive bleeding while loosening each suture.
- If the repair is not adequately hemostatic, reapply the cross clamps and place another 10-0 nylon suture at the site of bleeding. If hemostasis is assured, remove the sutures and then the absorbable gelatin sponge.
- Gently rub the vascular bundle with small double-ended hard, sharp, pointed cotton swabs, which further facilitate the restoration of blood flow. Confirm technical success of the operation using visualization of pulsatile, bright red oxygenated blood entering the iliac vein and mixing with dark venous blood returning from the hindlimb.
- Inject heparinized saline (0.2 IU/g)15 into the IVC for systemic anticoagulation to improve AVF patency outcomes.
NOTE: Although this step occurs after the vascular reconstruction (as opposed to the human analog where heparinization occurs prior to vessel cross-clamping), a reduction in intraoperative bleeding and improved AVF patency were observed when performed at this stage of the procedure. Injection into a site covered by fascia and/or fat is preferable to prevent bleeding from the puncture site. - Re-inspect the surgical site for hemostasis after the injection of heparinized saline. If there are no bleeding concerns, close the midline fascia and then the skin incision with absorbable 5-0 PGA sutures in a running fashion.
- For sham operations, follow all the key steps of the procedure except for AVF formation. Apply a single knot of the 4-0 silk ligature at the proximal end of the left iliac arteriovenous bundle and match the clamp times to AVF surgeries (e.g., ~20 min, depending on microsurgeon proficiency).
6. Postoperative care and measurement
- After laparotomy closure, measure the blood perfusion of the bilateral tibialis anterior muscles and ventral paws using laser Doppler imaging.
NOTE: Unilateral perfusion deficits will confirm fistula diversion of arterial flow ("steal"). - Administer 0.1 mg/kg buprenorphine subcutaneously and return the mouse to a prewarmed mouse cage with highly absorbable soft bedding with nest.
- Allow the mouse to recover in the prewarmed mouse cage until the anesthesia wears off, which will be obvious when the mouse is ambulatory and interactive (~2 h). During recovery, give the mouse easy access to a moisturized, soft diet.
- Administer buprenorphine and/or subcutaneous saline hydration every 12 h up to 48 h and perform daily monitoring for 5 days post-operatively. Euthanize animals with a deteriorating condition or excessive tissue necrosis, classified as a modified ischemia score ≥229.
- Use serial duplex ultrasound assessments to evaluate fistula patency post-operatively; mice with fistula thrombosis are excluded from subsequent analyses unless the purpose of the experiments is to characterize AVF maturation failure.
- Determine other postoperative outcome measurements such as local hemodynamics, grip strength, and gait performance during the recovery time period. Collect fistula and muscle tissues to assess histomorphology at the end of the experiment during the sacrifice25,27.
Representative Results
Animals exposed to an adenine diet have reduced glomerular filtration rates (control: 441.3 ± 54.2 µL/min vs. CKD: 165.1 ± 118.3 µL/min, p < 0.05) and increased serum blood urea nitrogen levels (control: 20.39 ± 4.2 µL/min vs. CKD: 38.20 ± 10.65 µL/min, p < 0.05) compared to the animals that received casein-based chow, confirming the presence of kidney insufficiency prior to arteriovenous fistula surgery.
Validation of AVF patency
Although intra-operative visual confirmation of technical success is the initial identification of fistula patency, it does not fully guarantee patency or physiological maturation throughout the study period. Postoperative patency outcomes (i.e., success or failure) were determined using both duplex ultrasound imaging and histological examination, as we have previously demonstrated25. Figure 2 shows the representative B mode, pulse wave Doppler, and color Doppler ultrasound images and morphological sections of an arteriovenous fistula anastomosis, respectively. A patent fistula is directly visualized on color Doppler analysis with turbulent hemodynamics, as well as spectral broadening at the site of the fistula. Adaptive flow-mediated changes of the inflow and outflow vessels also indirectly confirm AVF patency. Specifically, the aorta has elevated peak systolic and end-diastolic velocity, the IVC develops pulsatility with elevated peak velocity, and vessel dilation in both the aorta and IVC is apparent (Figure 2A). In contrast, a failed or thrombosed fistula has almost no changes in inflow or outflow measurements and no turbulence or spectral broadening within the left iliac vasculature. Usually, fistula failure from thrombosis partially or fully occludes the left iliac artery, which is visualized as minimal to no flow on pulse-wave Doppler analysis. Figure 2B shows serial histology sections of an AVF 2 weeks after surgical creation. The sections are 5 µm thick and stained with Masson's trichrome. Surgical anastomosis of the artery and vein is obvious, and distinct venous arterialization is present (venous wall thickening and fibrosis with neointimal hyperplasia). Ultrasound imaging was performed on postoperative day 3 to rule out mice with early AVF failure, and then serial, non-invasive measurements were obtained throughout the study period. Morphological assessment provides period-specific vascular remodeling details at the time of sacrifice and was used to confirm ultrasound findings. An AVF patency rate of approximately 50% (20%-30% of postoperative death and 20%-30% of fistula failure)25 is to be expected initially, but the surgical success rate improves significantly (~5%-10% failure rate) with practice and increased proficiency.
Pathophysiological characteristics following iliac arteriovenous fistula formation
Hemodynamic alteration: Characteristics of AVF hemodynamics and distal hindlimb perfusion must be quantified to contextualize access-related limb pathophysiology. B-mode and pulse-wave Doppler ultrasound measurements after surgery revealed inflow and outflow vessel dilation (IVC: 1.4-fold at POD3 and 1.6-fold at POD13 and IRA: 1.4-fold at POD3 and 1.7-fold at POD13, p < 0.05) and increases in peak systolic velocity (IVC peak systolic velocity: 5.5-fold at POD3 and 4.9-fold at POD13 and IRA peak systolic velocity: 2.8-fold at POD3 and 3.7-fold at POD13, P < 0.05) compared to the sham animals (Figure 3A–D). Further, unilateral hindlimb ischemia was apparent postoperatively, which confirms steal-mediated arterial hypoperfusion distal to the fistula. Left paw perfusion deficits are expected to be ~20% of the contralateral limb, and the perfusion deficit of the tibialis anterior muscle is ~60%. Mice partially recovered these deficits throughout the study period (Figure 3E,F).
Hindlimb dysfunction: Ipsilateral limb disability is expected after AVF creation, which involves mild (most cases) to severe (few cases) leg limping that can last for several days. Unresolved hindlimb paralysis and/or paw necrosis might be indicative of a severe ischemic insult caused by fistula size out of the normal range. Hindlimb neuromotor function was quantified via grip strength testing and treadmill gait pattern analysis, which were performed sequentially throughout the recovery period. Expected unilateral grip strength is ~50% of the contralateral limb on postoperative day 4, with gradual recovery. AVF mice also require reduced treadmill speeds during gait assessment (<20 cm/min) (Figure 3G,H).
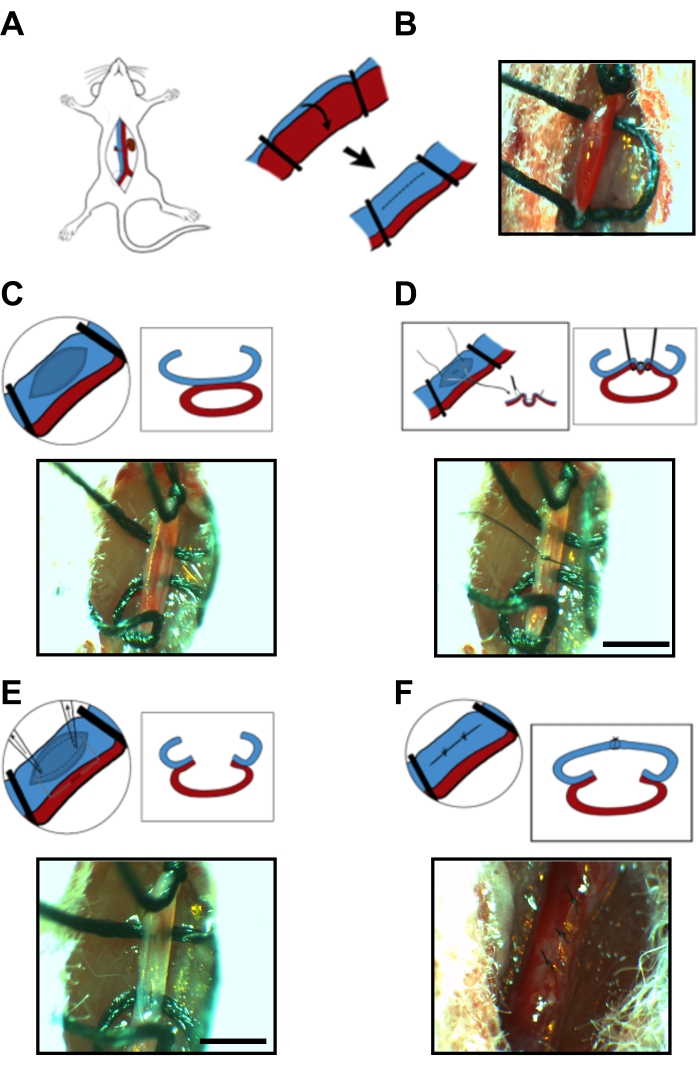
Figure 1: Microsurgery steps of arteriovenous fistula anastomosis. (A) Exposure of the surgical target area, including midline laparotomy and left iliac artery/vein isolation. (B) 4-0 suture ligatures (e.g., used as temporary vessel clamps) on the left common iliac arteriovenous bundle at proximal and distal sites. (C) A longitudinal venotomy on the anterior wall of the iliac vein. (D) 10-0 imbricating suture via the posterior wall of the iliac vein and the anterior wall of the iliac artery. (E) Elliptical incision with the imbricating distension. (F) Initial longitudinal venotomy from Image C is repaired using an interrupted 10-0 suture. Scale bar = 1 mm. Please click here to view a larger version of this figure.
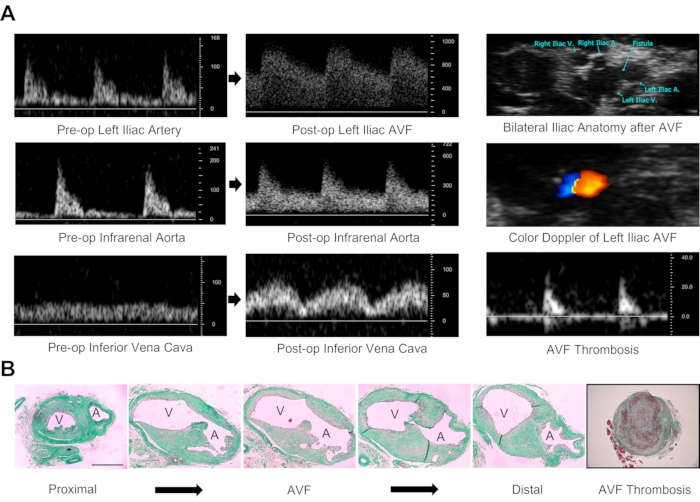
Figure 2: Validation of arteriovenous fistula patency. (A) Doppler ultrasound determination of AVF patency. Characteristics of a patent fistula include arterial and venous dilation on B-mode imaging, turbulent flow on color Doppler analysis of the left iliac vasculature, pulsatile spectral broadening on pulse-wave Doppler assessment of the left iliac vessels, increases in peak systolic and end-diastolic velocity of the infrarenal aorta, and pulsatility within the IVC with increases in peak systolic velocity. Diminished or absent flow within the iliac vessels is suggestive of AVF failure/thrombosis. The duplex ultrasound technique provides both morphological and physiological data. Velocity measurements are in millimeters per second. (B) Morphological assessment of AVF anastomosis 14 days after fistula creation. Images were stained with Masson's trichrome. There are anatomical changes in serial section microscopy from proximal (left end) to distal (right end) common iliac arteriovenous anatomy. Occlusion of the vasculature due to clot and/or excessive neointimal hyperplasia confirms AVF failure. Images are 10x magnification. A: Common iliac artery, V: Common iliac vein. Scale bar = 500 µm. Please click here to view a larger version of this figure.
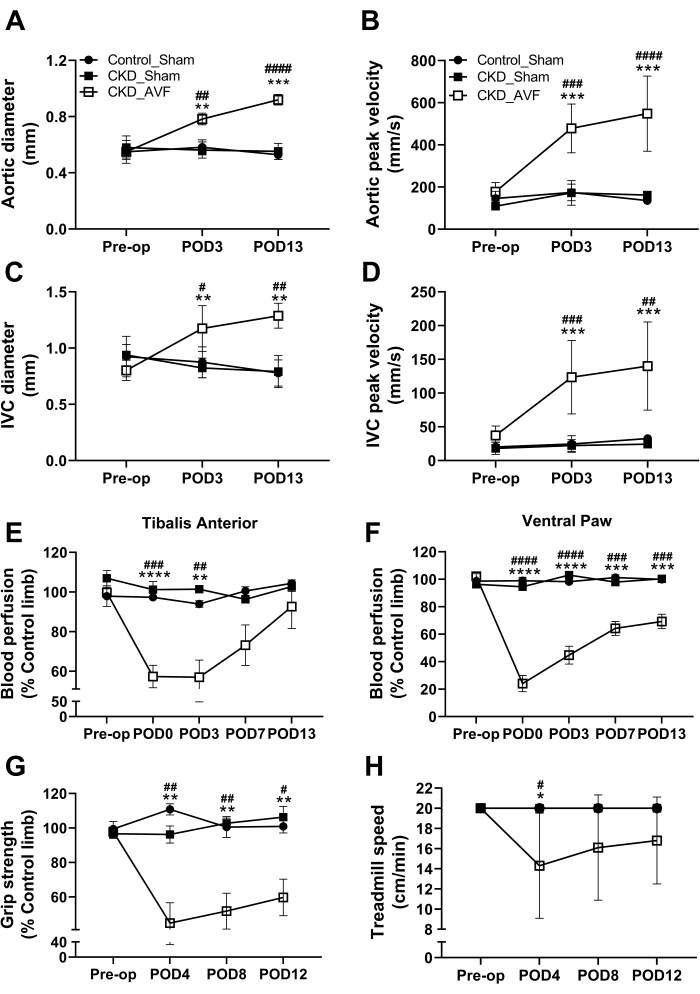
Figure 3: Pathophysiological characteristics prior to and following AVF formation. Quantification of ultrasound imaging in (A) infrarenal aortic diameter, (B) infrarenal aortic peak systolic velocity, (C) inferior vena cava diameter, and (D) inferior vena cava peak systolic velocity pre-operatively and at postoperative days 3 and 13. Local blood perfusion (Laser doppler) measurement on (E) tibialis anterior and (F) ventral paw before surgery and throughout the 2 week recovery period. Neuromotor functional testing included (G) grip strength and (H) treadmill test pre- and post-operatively. Data were analyzed using a two-way ANOVA, and Tukey's post-hoc test was performed when appropriate. Values are means ± SD. *p < 0.05, **p < 0.01, ***p < 0.001, ****p < 0.0001 vs. Control_Sham. #p < 0.05, ##p < 0.01, ###p < 0.001, ####p < 0.0001 vs. CKD_Sham. N = 6-10/group. Please click here to view a larger version of this figure.
Discussion
The prevalence of hemodialysis patients with ARHD following AVF creation has continued to increase30,31. Indeed, unresolved symptomatic complications4,32,33 such as pain, weakness, paresthesia, and/or reduced range of motion can negatively impact patient wellbeing4,32,33,34,35,36 and threaten their capacity to receive high-quality repetitive hemodialysis treatment. Although the achievement of durable hemodialysis access is a top priority for ESRD patients, for subjects afflicted by ARHD, these potentially debilitating symptoms must be addressed to improve patient-centered outcomes. In the present study, as an important preclinical milestone in the field of ARHD research, we introduce a detailed surgical procedure to generate a mouse model of iliac AVF, which facilitates the examination of AVF-associated limb pathophysiology. In addition to the expected alterations in aorto-iliac and IVC hemodynamics, iliac AVF creation produced clinically relevant features of limb dysfunction, including peripheral tissue ischemia with gross motor impairment.
Each microsurgery step should be performed with exquisite care to avoid potential vessel trauma, which can cause substantial changes in both hemodynamics and limb pathology. During the ligation, the 4-0 silk tie knot should only be tightened enough to prevent blood flow through the surgical site of interest. Excessive suture ligature knot tension can injure the vessel wall, which can cause undesirable bleeding and could contribute to intimal hyperplasia, leading to decreased AVF patency. In particular, venotomy repair is one of the most important steps of the surgical procedure. Too large a bite in the vein wall can lead to vessel stenosis and, ultimately, thrombosis, while too shallow a repair can cause dehiscence with hemorrhage. Similarly, bleeding can also occur if the venotomy repair sutures are spaced too far apart. In our experience, a ~0.025-0.03 mm interval between sutures is enough to create a hemostatic repair.
In addition to the reproducibility of the surgical technique, utilizing a disease- or symptom-specific animal model is one of the most important contributions of the current work. In the present study, animals were exposed to a 0.2%-0.15% adenine diet for 2-3 weeks prior to and following AVF surgery to establish renal dysfunction and a uremic milieu analogous to ESRD patients. Compared to surgical CKD models (e.g., 5/6 nephrectomy), an adenine diet model has several advantages, including very low mortality rates and less inter-observer variation27,37. Notably, the severity and pathophysiological consequences can be modified based on the concentration and/or duration of the adenine diet38,39. Coupled with the diet-induced nephropathy, the current animal model described herein can set the stage for researchers to study the pathophysiologic mechanisms by which uremia affects ARHD. Further, additional animal models of disease can be added to the surgical model to test the influence of highly prevalent comorbid conditions, such as diabetes, hypertension, or coronary artery disease.
Although the presented iliac AVF procedure reproducibly models key aspects of limb pathophysiology relevant to hemodialysis patients with ARHD, there are some limitations and complications worthy of discussion. First, mice subjected to this procedure do not have true "vascular access"; thus, experiments involving experimental hemodialysis treatments are not possible. Second, the severity of limb dysfunction is impacted by the size of the arteriovenous communication, so consistent AVF creation is critical for reproducible outcomes. For example, the creation of a large AVF can produce severe hindlimb ischemia, which can culminate in limb necrosis. New microsurgeons beginning the procedure are encouraged to use histological analyses of the created AVFs to analyze the size for consistency. In mice subjected to other AVF models, cardiac remodeling, including hypertrophy and possibly heart failure, has been reported 40,41,42. Cardiac alterations in the current model have not been rigorously assessed, although we have qualitatively observed cardiac hypertrophy compared to sham animals. Furthermore, future long-term analyses are needed to evaluate how the murine cardiovascular system adapts to the iliac AVF formation and maturation. One additional concern is that younger C57BL6 mice have an ability to generate arteriogenesis and angiogenesis responses to ischemic stimuli, leading to collateral vessel formation, as shown by the modest recovery in laser Doppler limb perfusion in this study. Thus, it is possible that mice will completely recover from AVF limb pathology once more robust collateral networks have formed; however, future studies are needed to map the collateral growth and distal vasculature changes.
To date, the underlying mechanisms by which hand function is impaired and/or exacerbated by AVF placement are incompletely understood. Given that the mouse genome is well characterized and there is ready access to a wide array of transgenic models for gene manipulation in mice, this iliac AVF surgical model provides a useful tool for biomedical discovery surrounding ARHD. Compared to other rodent AVF models, which employ central vasculature surgery (e.g., aorto-caval fistula model), or large animal models with femoral or iliac AVF, the present iliac AVF model with or without adenine diet-induced uremia provides investigators with a robust experimental platform that can be used to interrogate the underlying biological mechanisms associated with hemodialysis ARHD and generate novel targeted therapies. Furthermore, preclinical models are generally considered to be crucial for the early development and validation of pharmaceutical therapies, of which none are currently available to treat/prevent ARHD. Notably, this model is also amenable to alterations in both the size of AVF and the severity of renal dysfunction, which allows investigators to carefully modulate the severity of the pathology. In conclusion, this unique preclinical mouse AVF model can serve as a practical platform to facilitate preclinical therapeutic development aimed at reducing hand disability following AVF placement.
Disclosures
The authors have nothing to disclose.
Acknowledgements
We sincerely thank Dr. Guanyi Lu from the Division of Vascular Surgery and Endovascular Therapy at the University of Florida for the technical support on the development of the iliac AVF model, as well as surgical training, and Ravi Kumar from the Department of Applied Physiology and Kinesiology at the University of Florida for the technical support getting the live microsurgical images.
This work was supported by grants from the National Institutes of Health and National Heart, Lung, and Blood, Institute numbers R01-HL148697 (to S.T.S.), as well as the American Heart Association grant number POST903198 (to K.K.).
Materials
| 0.15% Adenine diet | ENVIGO | TD.130899 | 20% casein, 0.15% adenine, 0.9% P |
| 0.2% Adenine diet | ENVIGO | TD.130900 | 20% casein, 0.2% adenine, 0.9% P |
| 10-0 Nylon suture | AD surgical | XXS-N1005T4 | |
| 29 G needle syringes | Exel International | 14-841-32 | |
| 31 G needle syringes | Advocate | U-100 insulin syringe | |
| 4-0 silk suture | AD surgical | S-S41813 | |
| 45-degree angled dumont forceps | Fine Science Tools | 11253-25 | |
| 5-0 PGA suture | AD surgical | PSGU-518R13 | |
| 6-0 silk suture | AD surgical | S-S618R13 | |
| Absorbable gelatin sponge | ETHICON | 1975 | |
| Alcohol preps | Covidien | 5110-cs4000 | 70% isopropyl alcohol |
| Buprenorphine | NA | NA | 0.01 g/mL |
| C57BL6/J mice | Jaxon Laboratory | ||
| Casein diet | ENVIGO | TD.130898 | 20% casein, 0.9% P |
| Cotton swabs | CONSTIX | SC-9 | Medium single-ended round cotton swab |
| Cotton swabs | CONSTIX | SC-4 | Small double-ended hard, sharp, pointed cotton swab |
| Curity non-woven sponges (2×2) | Covidien | 9022 | |
| Curved Vannas spring scissors | Fine Science Tools | 15001-08 | |
| Doppler ultrasound | VisualSonics | Vevo 2100 | |
| Extra fine graefe forceps | Fine Science Tools | 11150-10 | 2 pairs |
| Eye lubricant | CLCMEDICA | Optixcare eye lube | |
| Heparin (5000 U/mL) | National Drug Codes List | 63739-953-25 | 100 IU/mL |
| Hot bead sterilizer | Fine Science Tools | 18000-50 | |
| Low-temperature cautery | Bovie | AA04 | |
| Pen trimmer | Wahl | 5640-600 | |
| Powder-free surgical gloves | Ansell | 7824PF | |
| Round handled needle holders | Fine Science Tools | 12076-12 | |
| Sterile towel drape | Dynarex | DY440-MI | |
| Sterilized 0.9% saline | National Drug Codes List | 46066-807-25 | |
| Straight dumont forceps | Fine Science Tools | 11253-20 | |
| Straight needle holder | Fine Science Tools | FST 12001-13 | |
| Straight vannas spring scissors | Fine Science Tools | 25001-08 | |
| TrizChLOR4 | National Drug Codes List | 17033-279-50 |
References
- Gameiro, J., Ibeas, J. Factors affecting arteriovenous fistula dysfunction: a narrative review. The Journal of Vascular Access. 21 (2), 134-147 (2020).
- Culleton, B. F., Asola, M. R. The impact of short daily and nocturnal hemodialysis on quality of life, cardiovascular risk and survival. Journal of Nephrology. 24 (4), 405 (2011).
- Huber, T. S., et al. Access-related hand ischemia and the hemodialysis fistula maturation study. Journal of Vascular Surgery. 64 (4), 1050-1058 (2016).
- Rehfuss, J. P., et al. The spectrum of hand dysfunction after hemodialysis fistula placement. Kidney International Reports. 2 (3), 332-341 (2017).
- Caplice, N. M., et al. Neoangiogenesis and the presence of progenitor cells in the venous limb of an arteriovenous fistula in the rat. American Journal of Physiology-Renal Physiology. 293 (2), 470-475 (2007).
- Castier, Y., et al. Characterization of neointima lesions associated with arteriovenous fistulas in a mouse model. Kidney International. 70 (2), 315-320 (2006).
- Croatt, A. J., et al. Characterization of a model of an arteriovenous fistula in the rat: the effect of L-NAME. The American Journal of Pathology. 176 (5), 2530-2541 (2010).
- Guzman, R. J., Krystkowiak, A., Zarins, C. K. Early and sustained medial cell activation after aortocaval fistula creation in mice. Journal of Surgical Research. 108 (1), 112-121 (2002).
- Kojima, T., et al. The relationship between venous hypertension and expression of vascular endothelial growth factor: hemodynamic and immunohistochemical examinations in a rat venous hypertension model. Surgical Neurology. 68 (3), 277-284 (2007).
- Misra, S., et al. The rat femoral arteriovenous fistula model: increased expression of matrix metalloproteinase-2 and -9 at the venous stenosis. Journal of Vascular and Interventional Radiology. 19 (4), 587-594 (2008).
- Nath, K. A., Kanakiriya, S. K., Grande, J. P., Croatt, A. J., Katusic, Z. S. Increased venous proinflammatory gene expression and intimal hyperplasia in an aorto-caval fistula model in the rat. The American Journal of Pathology. 162 (6), 2079-2090 (2003).
- Nath, K. A., et al. The murine dialysis fistula model exhibits a senescence phenotype: pathobiological mechanisms and therapeutic potential. American Journal of Physiology-Renal Physiology. 315 (5), 1493-1499 (2018).
- Yamamoto, K., et al. The mouse aortocaval fistula recapitulates human arteriovenous fistula maturation. American Journal of Physiology-Heart and Circulatory Physiology. 305 (12), 1718-1725 (2013).
- Yang, S. T., et al. Adult mouse venous hypertension model: common carotid artery to external jugular vein anastomosis. Journal of Visualized Experiments: JoVE. (95), e50472 (2015).
- Wong, C. Y., et al. A novel murine model of arteriovenous fistula failure: the surgical procedure in detail. Journal of Visualized Experiments: JoVE. (108), e53294 (2016).
- Krishnamoorthy, M. K., et al. Anatomic configuration affects the flow rate and diameter of porcine arteriovenous fistulae. Kidney International. 81 (8), 745-750 (2012).
- Wang, Y., et al. Venous stenosis in a pig arteriovenous fistula model-anatomy, mechanisms and cellular phenotypes. Nephrology Dialysis Transplantation. 23 (2), 525-533 (2008).
- Loveland-Jones, C. E., et al. A new model of arteriovenous fistula to study hemodialysis access complications. The Journal of Vascular Access. 15 (5), 351-357 (2014).
- Nugent, H. M., et al. Perivascular endothelial implants inhibit intimal hyperplasia in a model of arteriovenous fistulae: a safety and efficacy study in the pig. Journal of Vascular Research. 39 (6), 524-533 (2002).
- Butterfield, A. B., et al. Inverse effect of chronically elevated blood flow on atherogenesis in miniature swine. Atherosclerosis. 26 (2), 215-224 (1977).
- Kwei, S., et al. Early adaptive responses of the vascular wall during venous arterialization in mice. The American Journal of Pathology. 164 (1), 81-89 (2004).
- Berru, F. N., et al. Chronic kidney disease exacerbates ischemic limb myopathy in mice via altered mitochondrial energetics. Scientific Reports. 9 (1), 15547 (2019).
- Khattri, R. B., Thome, T., Ryan, T. E. Tissue-specific 1H-NMR metabolomic profiling in mice with adenine-induced chronic kidney disease. Metabolites. 11 (1), 45 (2021).
- Thome, T., et al. Impaired muscle mitochondrial energetics is associated with uremic metabolite accumulation in chronic kidney disease. Journal of Clinical Investigation Insight. 6 (1), 139826 (2021).
- Kim, K., et al. Development of a murine iliac arteriovenous fistula model for examination of hemodialysis access-related limb pathophysiology. Journal of Vascular Surgery-Vascular Science. 2, 247-259 (2021).
- Castro, B., Kuang, S. Evaluation of muscle performance in mice by treadmill exhaustion test and whole-limb grip strength assay. Bio-protocol. 7 (8), 2237 (2017).
- Kim, K., et al. Skeletal myopathy in CKD: a comparison of adenine-induced nephropathy and 5/6 nephrectomy models in mice. American Journal of Physiology-Renal Physiology. 321 (1), 106-119 (2021).
- Yang, B., Shergill, U., Fu, A. A., Knudsen, B., Misra, S. The mouse arteriovenous fistula model. Journal of Vascular and Interventional Radiology. 20 (7), 946-950 (2009).
- Brenes, R. A., et al. Toward a mouse model of hind limb ischemia to test therapeutic angiogenesis. Journal of Vascular Surgery. 56 (6), 1669-1679 (2012).
- Bello, A. K., et al. Assessment of global kidney health care status. Journal of the American Medical Association. 317 (18), 1864-1881 (2017).
- Levin, A., et al. Global kidney health 2017 and beyond: a roadmap for closing gaps in care, research, and policy. The Lancet. 390 (10105), 1888-1917 (2017).
- Hassabi, M., et al. Comparing strength and range of motion of the upper limb with AV fistula access with the contralateral upper limb among patients treated with hemodialysis. Researcher Bulletin of Medical Sciences. 22 (1), 1 (2017).
- Capitanini, A., Galligani, C., Lange, S., Cupisti, A. Upper limb disability in hemodialysis patients: evaluation of contributing factors aside from amyloidosis. Therapeutic Apheresis and Dialysis. 16 (3), 242-247 (2012).
- Altintepe, L., et al. Physical disability, psychological status, and health-related quality of life in older hemodialysis patients and age-matched controls. Hemodialysis International. 10 (3), 260-266 (2006).
- Castaneda, C., et al. Resistance training to reduce the malnutrition-inflammation complex syndrome of chronic kidney disease. American Journal of Kidney Diseases. 43 (4), 607-616 (2004).
- Hurton, S., et al. Upper extremity complications in patients with chronic renal failure receiving haemodialysis. Journal of Renal Care. 36 (4), 203-211 (2010).
- Mazumder, M. K., Giri, A., Kumar, S., Borah, A. A highly reproducible mice model of chronic kidney disease: Evidences of behavioural abnormalities and blood-brain barrier disruption. Life Sciences. 161, 27-36 (2016).
- Jia, T., et al. A novel model of adenine-induced tubulointerstitial nephropathy in mice. BioMed Central Nephrology. 14, 116 (2013).
- Kieswich, J. E., et al. A novel model of reno-cardiac syndrome in the C57BL/ 6 mouse strain. BioMed Central Nephrology. 19 (1), 346 (2018).
- Abassi, Z., Goltsman, I., Karram, T., Winaver, J., Hoffman, A. Aortocaval fistula in rat: a unique model of volume-overload congestive heart failure and cardiac hypertrophy. Journal of Biomedicine and Biotechnology. 2011, 729497 (2011).
- Brower, G. L., Levick, S. P., Janicki, J. S. Inhibition of matrix metalloproteinase activity by ACE inhibitors prevents left ventricular remodeling in a rat model of heart failure. American Journal of Physiology-Heart and Circulatory Physiology. 292 (6), 3057-3064 (2007).
- Francis, B. N., Abassi, Z., Heyman, S., Winaver, J., Hoffman, A. Differential regulation of ET (A) and ET (B) in the renal tissue of rats with compensated and decompensated heart failure. Journal of Cardiovascular Pharmacology. 44, 362-365 (2004).

