Photoselective Vaporesection of the Prostate via an End-firing Lithium Triborate Crystal Laser
Summary
Here we present a protocol to perform Photoselective Vaporesection of the Prostate (PVRP) for benign prostatic hyperplasia (BPH) treatment.
Abstract
The occurrence of lower urinary tract symptoms (LUTS) caused by benign prostatic hyperplasia (BPH) is a common problem with a high incidence in the aging male population. Although it is not a life-threatening disease, BPH causes problems that seriously impact the quality of life. Here, we introduce a new technique called photoselective vaporesection of the prostate (PVRP) in treating BPH, which can be seen as a variation of photoselective vaporization of the prostate (PVP). This procedure presents several advantages compared to the PVP technique including less laser energy loss, less intraoperative complications as well as more tissue resection rate.
Introduction
Although transurethral resection of the prostate (TURP) is still accepted as the gold standard in benign prostatic hyperplasia (BPH) surgical treatment, laser surgeries have gradually become more popular due to the better patient tolerance, less intraoperative blood loss, satisfactory efficacy, and shorter postoperative recovery1,2,3. Currently, the most commonly used lasers for the BPH treatment worldwide are generated by lithium potassium titanyl phosphate or lithium triborate (LBO) crystals4,5. Traditionally, these are classified as sidefiring lasers compared to other types of laser, such as holmium laser and thulium laser.
Photoselective vaporization of the prostate (PVP) surgery could considerably decline TURP syndrome due to saline irrigation6,7, and compared to other types of lasers, the reliable efficacy of lower urinary tract syndrome (LUTS) by PVP was verified by a series of studies8,9,10. However, PVP associated with side-firing laser emission also has some disadvantages, including an energy loss of nearly 20% and a short lifespan of the laser fiber11,12,13. Moreover, PVP increases the possibility of missed diagnosis of prostate cancer due to complete tissue vaporization.
The introduction of Photoselective Vaporesection of the Prostate (PVRP) with an end-firing fiber successfully overcame most of the disadvantages of PVP mentioned above. First, the tip is capable of transmitting laser to the tissues with almost no energy loss intraoperatively. Second, when fiber debris collects on the tip, it is straightforward to maintain the ideal output power by simply removing the affected parts. Finally, laser resection enables the collection of specimens for postoperative pathologic examination. Hence, using this protocol in treating BPH could enhance the tissue removal rate, save the operative time and improve the intraoperative safety.
Protocol
All methods described here have been approved by ethics committee of Beijing Hospital. Indications for surgery are according to the European Association of Urology guidelines for nonneurogenic male LUTS. Contraindications include suspected prostate cancer or detrusor dysfunction.
1. Instruments for Operation
- Ensure the availability of a LBO crystal laser with a maximum power of 160 W.
- Employ an endfiring laser fiber and saline solution for intraoperative bladder irrigating.
- Use a 26F laser resectoscope to acquire good vision and to enhance the resection efficiency.
2. Preparation for Operation
- Provide an intravenous antibiotic preoperatively (intravenous administration of cefuroxime sodium 1.5 g with 100 mL 0.9%sodium chloride solution 30 min before the operation) to all the patients.
- Before the anesthesia, make the patient lay down on the operation table.
Note: General anesthesia is effective and appropriate for this operation, Anesthetist will finally determine the mode of anesthesia depending on patient's general condition. - Drape the patients in a sterile fashion in the dorsa lithotomy position.Do not perform any skin preparation.
3. Procedure Steps
- Vaporesection of the Median Lobe
- Examine the whole bladder cavity and prostatic urethra carefully through the resectoscope after the bladder is distended.
Note: This step helps urologist to locate some key anatomic sings including bilateral ureteral orifice and verumontanum. - Mark two lines initially. Ensure that these lines originate at 5 o'clock and 7 o'clock at the bladder neck and continue along the boundaries between the median and lateral lobes, finally terminating at the proximal margin of the verumontanum.
- Set laser power at 80 W. Vaporize the prostate tissue via a fiber by the laser vaporization along these lines until the white cyclic fibers are seen.
Note: This is the sign of prostatic capsule. The two lines are merged into single line adjacent to the verumontanum. - Set laser power at 80 to 100 W. Mark several lines on surface of the middle lobe via laser fiber. Then divide the wedgeshaped middle lobe into several chunks according to these lines through vaporization technique. Then split each chunk from the middle lobe. Finally, remove the whole middle lobe.
- Examine the whole bladder cavity and prostatic urethra carefully through the resectoscope after the bladder is distended.
- Vaporesection of the Lateral Lobes
- Vaporize the tissue at 12 o'clock from the apex of the prostate to the bladder neck by rotating the cystoscope 180°. Do not let the laser fiber go too close to the apex at 12 o'clock which can cause postoperative urine incontinence.
Note: This technique enhances the resection rate of the tissue around the prostate roof. - Identify the lower margin of both the lateral lobes clearly once vaporesection is complete.
- Before removing the lateral lobes, set another 2 similar grooves that originate from the bladder neck at 3 o'clock and 9 o'clock to the proximal end of the verumontanum.
- Remove the tissue of the lateral gland. Set the laser power at 80 to 100 W and mark several lines on the surface of the left lobe via laser fiber that divides the left lobe into several chunks according to these lines through vaporization technique. Then split each chunk from the lobe and finally remove the whole left lobe. Repeat this procedure to remove right lobe.
- Remove the remnant gland tissue along the existing boundary of the capsule.
- Vaporize the tissue at 12 o'clock from the apex of the prostate to the bladder neck by rotating the cystoscope 180°. Do not let the laser fiber go too close to the apex at 12 o'clock which can cause postoperative urine incontinence.
- Channel Trimming
- Remember to trim some protruding tissues around the apex of the gland, to enhance the integrity of the cavity.
- To avoid intraoperative complications (i.e., capsule perforation or sphincter injury), use vaporization technique rather than resection to trim the tissue near the external urethral sphincter and lower the power to less than 80 Watt.
- Hemostasis and Catheterization
- Employ a glass syringe that matches the interface of the resectoscope to remove tissue chunk by water flow. Make sure there is no evidence of the residual tissue in the bladder and prostatic fossa through resectoscope, and identify the intact of the ureteral orifices.
- Employ a lower laser power (30 to 50 W) to stop bleeding around the surgical site. Keep an appropriate distance usually 3 to 5 mm between fiber and vessels to acquire a satisfying hemostasis effect.
- Remove the resectoscope from the urethra. Place a 22 French Foley catheter from urethral orifice to bladder cavity gently with 30 mL water in the balloon after sufficiently lubricating urethra by lidocaine gel.
- Postoperative Care
- Let the patient lay down on the bed for around 3 h postoperatively in the care unit until they completely wake up from anesthesia. Meanwhile, make sure patient monitors and medical oxygen are available during this time.
- Upon completely waking up, return the patient to the ward. Let the patient begin to drink some water and take some food. Record the urine output and pay attention to the color of the urine.
Representative Results
A total of 35 patients who underwent PVRP were included in one of our studies. The mean patient age was 72.1 ± 7.1 years (range 53-85 years).
Perioperative data are listed in Table 1. The mean laser emission time accounted for nearly 50% of the mean operative time. The blood loss in most patients was < 200 mL. However, the average deviated due to some moderate bleeding cases. Almost 90% of the patients had the catheter removed within 6 days postoperatively.
All patients returned to the hospital for follow-up examinations at the 1st and the 3rd month postoperatively (Table 2). Examinations including urinalysis combined with urine culture were performed to check for postoperative urinary tract infection (UTI).
International Prostate Symptom Score (IPSS) and Quality of Life (QoL) are tools used to screen for, rapidly diagnose, track the symptoms of, and suggest management of the symptoms of BPH. It also can be used to evaluate the efficacy of BPH treatment. Compared to baseline values, the mean subgroup IPSS and QoL scores improved dramatically during follow-up. The IPSS storage score, IPSS voiding score, IPSS nocturia score, and the QoL score significantly decreased by 75.3%, 83.6%, 51.4%, and 71.7%, respectively (all P < 0.001). For the objective parameters, the mean prostate volume and the serum level of the total prostatespecific antigen decreased to 42.6% and 36.2%, respectively. The mean Qmax increased nearly 2-fold compared to the baseline and reached a maximum of 15.6 mL/s. The mean postvoid residual during followup was only 11.9 ± 6.5 mL. Table 3 presents the peri and postoperative complications. According to the modified ClavienDindo classification system15 a widely used and authoritative tool for grading surgical complications, only two cases were Grade 3B, one was a prostate capsule perforation and the other was a bladder neck contracture. Prostate capsule perforation was identified in a single case, which did not require specific therapy. No other perioperative complications were found. Three patients experienced high febrility due to acute UTI caused by extendedspectrum betalactamase Escherichia coli on postoperative days 5-6; all three patients received antibiotics and recovered rapidly. Five patients complained of urgency and frequency, but the urine culture revealed no abnormalities in three of them which could exclude UTI. The other two patients were diagnosed with UTI according to urine culture and recovered after effective antibiotic courses. Only a single patient experienced persistent urinary incontinence in the early postoperative period without evidence of UTI. This urinary incontinence was fully resolved after pelvic floor muscles training for several weeks. Another patient with difficulty in voiding was diagnosed with bladder neck contracture through cystoscopy. This was resolved after a bladder neck incision was performed under general anesthesia on the 40th day after PVRP.
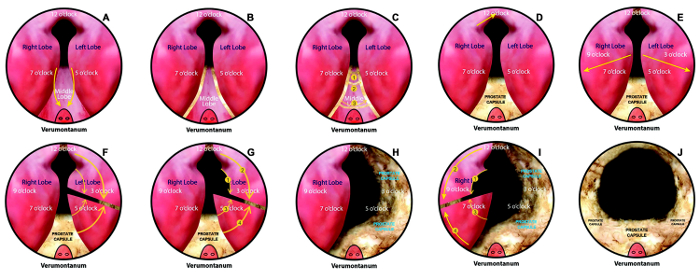
Figure 1: Key steps of photoselective vaporesection of the prostate. (A) Mark two lines originally at 5 o'clock and 7 o'clock at the bladder neck. These lines continue along the boundaries between the median and lateral lobes. (B, C) Vaporize the prostate tissue via laser vaporization along these lines, they are merged into single line adjacent to the verumontanum. Mark several lines on the surface of the middle lobe via laser fiber, divide the middle lobe into several chunks through vaporization technique and then split each chunk from the middle lobe, finally remove the whole middle lobe. (D) Vaporize the tissue at 12 o'clock from the apex of the prostate to the bladder neck. (E) Set another two similar grooves that originated from the bladder neck at 3 o'clock and 9 o'clock to the proximal end of the verumontanum. (F-I) Remove the tissue of the lateral glands, the technique is similar to middle lobe resection. (J) Channel trimming. Please click here to view a larger version of this figure.
| Perioperative data of 35 patients with benign prostatic hyperplasia who underwent photoselective vaporesection of the prostate |
||||
| Data are shown as mean ± SD, or otherwise noted. TURP: Transurethral resection of the prostate; BPH: Benign prostatic hyperplasia; SD: Standard deviation. | ||||
| Parameters | Data | |||
| Mean operative time (min) | 119.4 ± 41.1 | |||
| Mean laser time (min) | 58.9 ± 22.3 | |||
| Blood loss (ml) | 204.6 ± 129.4 | |||
| Bladder irrigation during the operation (L) | 40.4 ± 14.2 | |||
| Convert into TURP (n) | 4 | |||
| Postoperative pathology report, n | ||||
| BPH | 33 | |||
| Prostate cancer | 2 | |||
| Catheterization time (days) | 7.4 ± 2.0 | |||
| Postoperative hospital stay (days) | 7.3 ± 1.4 | |||
Table 1: Perioperative data of 35 patients with benign prostatic hyperplasia who underwent photoselective vaporesection of the prostate. Data are shown as mean ± SD or otherwise noted. TURP: Transurethral resection of the prostate; BPH: Benign prostatic hyperplasia; SD: Standard deviation.
| Pre- and post-operative functional parameters of 35 patients with benign prostatic hyperplasia who underwent photoselective vaporesection of the prostate | |||||
| Data are shown as mean ± SD. *Significant differences between pre- and post-operative 1 month groups; †Significant differences between pre- and post-operative 3 months groups; ‡Significant differences between postoperative 1 month and postoperative 3 months groups. IPSS: International Prostate Symptom Score; QoL: Quality of life; Qmax: Maximal urinary flow rate; tPSA: Total prostate-specific antigen; SD: Standard deviation. |
|||||
| Parameters | Preoperative (n = 35) | Postoperative 1 month (n = 35) | Postoperative 3 months (n = 35) | F | P |
| Storage scores in IPSS | 8.9 ± 3.3*,† | 4.4 ± 3.6‡ | 2.2 ± 1.9 | 33.025 | <0.001 |
| Voiding score in IPSS | 11.0 ± 3.2*,† | 4.1 ± 3.9‡ | 1.8 ± 1.7 | 86.58 | <0.001 |
| Nocturia score in PSS | 3.7 ± 1.1*,† | 2.4 ± 1.1‡ | 1.8 ± 0.9 | 29.15 | <0.001 |
| QoL score | 4.6 ± 0.9*,† | 2.3 ± 1.5‡ | 1.3 ± 1.0 | 107.08 | <0.001 |
| Prostate volume | 81.1 ± 36.6*,† | 35.4 ± 14.2‡ | 34.0 ± 14.1 | 45.83 | <0.001 |
| Qmax | 5.3 ± 3.9*,† | 12.5 ± 3.4‡ | 16.0 ± 4.3 | 58.84 | <0.001 |
| tPSA | 5.8 ± 4.6*,† | 3.1 ± 2.8‡ | 2.1 ± 1.7 | 12.21 | <0.001 |
Table 2: Pre– and post–operative functional parameters of 35 patients with benign prostatic hyperplasia who underwent photoselective vaporesection of the prostate. Data are shown as mean ± SD. *Significant differences between pre- and post-operative 1-month groups; †Significant differences between pre- and post-operative 3-months groups; ‡Significant differences between postoperative 1-month and postoperative 3-months groups. IPSS: International Prostate Symptom Score; QoL: Quality of life; Qmax: Maximal urinary flow rate; tPSA: Total prostate-specific antigen; SD: Standard deviation.
| Peri- and post-operative complications in 35 patients with benign prostatic hyperplasia who underwent photoselective vaporesection of the prostate |
||
| Complications were graded according to the modified Clavien-Dindo classification system. TURP: Transurethral resection of the prostate. | ||
| Complications | Patients, n (%) | Grade |
| Intraoperative | ||
| Acute urinary tract infection | 3 (8.6) | 2 |
| Prostate capsule perforation | 1 (2.9) | 3b |
| Blood transfusion | 0 | 2 |
| TURP syndrome | 0 | 4 |
| Bladder wall injury | 0 | 2 |
| Ureteric orifice injury | 0 | 2 |
| Urethra sphincter injury | 0 | 2 |
| Postoperative | ||
| Urinary tract infection | 2 (5.7) | 2 |
| Urinary incontinence | 1 (2.9) | 1 |
| Bladder neck contracture | 1 (2.9) | 3b |
| Postoperative bleeding | 0 | 2 |
Table 3: Peri– and post–operative complications in 35 patients with benign prostatic hyperplasia who underwent photoselective vaporesection of the prostate. Complications were graded according to the modified Clavien-Dindo classification system. TURP: Transurethral resection of the prostate.
Discussion
Here, we share our experiences with PVRP. First, PVRP enabled better exposure of the prostate capsule with proper demarcation and reduced the risk of capsule perforation. Second, the tissue removal should be carried out along the surgical capsule, especially with the groove at 12 o'clock, which facilitates tissue resection around the roof of the prostatic urethra and provides a satisfactory tissue removal rate. Third, it is essential to remove the middle lobe initially to acquire a wider channel in the prostatic urethra and enhance the operative visualization. In cases with large middle lobes with bladder neck involvement, we strongly recommend that markers should be drawn on the middle lobe before it is removed separately. Fourth, unlike the thulium laser, LBO laser cannot be absorbed by water, thus, the potential risk of tissue perforation is increased when the laser beam is concentrated at a certain place for a long time. This issue can be easily avoided by distending the bladder, frequently moving the fiber tip, and decreasing the output power when the fiber tip is close to the bladder neck and prostate apex. Finally, for the great majority of the glands, the LBO laser produced a satisfactory hemostatic effect.
We usually decrease the output power to about 50 Watt and maintain an appropriate distance between the fiber tip and hemorrhage site, otherwise excessive tissue vaporization may incur capsule perforation.
The exception to this is bleeding in the bladder neck where the vascularity shows huge variability among patients; in highly vascular areas, LBO laser may be inappropriate for the management of hemorrhage. The likelihood of severe bleeding seems to correlate with the prostate volume, and bipolar TURP loop should be employed in these cases. In one of our studies, four of 35 procedures were converted to TURP to achieve hemostasis. Other researchers reached a similar conclusion that bleeding is the most common intraoperative complication and is also the main reason for longer operative time6. A hemostat can reportedly help manage intractable bleeding during the procedure16. There is a learning curve for beginners to fully grasp the hemostasis technique. So, for the sake of safety during the procedure, we strongly recommend that beginners should not choose the case whose prostate volume is more than 80 mL.
LBO laser showed a significant advantage in for the treatment of BPH and markedly improved both the subjective and objective parameters of patients compared to their baseline data. In addition, the PVRP technique enabled the collection of specimens for pathological examination.
Compare to existing procedure in BPH treatment, PVRP demonstrates satisfactory short-term clinical outcomes and safety in the treatment of LUTS. In addition, this promising technique has apparent advantages in enhancing tissue resection rate and obtaining pathological specimens. With some equipment improvement and procedure adjustment, this technique could provide a blueprint for the prostate enucleation protocol with Lithium Triborate Crystal Laser in the future.
Disclosures
The authors have nothing to disclose.
Acknowledgements
The authors have no acknowledgements.
Materials
| FLARE surgical Laser Fiber | REALTON | The FLARE Surgical laser Fiber is a 600 micron fiber with an straight tip that transmits the laser energy directly. this product is packaged sterile for disposable use and should not be re-sterilized or reused. Dispose of properly after use. | |
| AURORA Surgical Green Laser System | REALTON | pvp-160-021 | The AURORA Surgical green laser system is a diode-pumped, frequency-doubled Nd:YAG solid state laser. The AURORA Surgical green laser system features a “Plug and Play” capability that self-adjusts to the facility’s individual voltage requirements, eliminating the need for electrical modifications. The laser system also includes an air-cooled internal mechanism, ensuring safe operating temperatures with no external water connections. Laser energy emission and system status selection is activated through a surgeon-controlled, color-coded footswitch or system touch screen feature located in the laser console. |
References
- Capitán, C., Blázquez, C., Martin, M. D., Hernández, V., de la Peña, E., Llorente, C. GreenLight HPS 120W laser vaporization versus transurethral resection of the prostate for the treatment of lower urinary tract symptoms due to benign prostatic hyperplasia: A randomized clinical trial with 2-year follow-up. Eur Urol. 60 (4), 734-739 (2011).
- Cornu, J. N., Ahyai, S., Bachmann, A., de la Rosette, J., Gilling, P., Gratzke, C., et al. A systematic review and meta-analysis of functional outcomes and complications following transurethral procedures for lower urinary tract symptoms resulting from benign prostatic obstruction: An update. Eur Urol. 67 (6), (2014).
- Kang, H. W., Jebens, D., Malek, R. S., Mitchell, G., Koullick, E. Laser vaporization of bovine prostate: A quantitative comparison of potassium-titanyl-phosphate and lithium triborate lasers. J Urol. 180 (6), 2675-2680 (2008).
- Herrmann, T. R., Liatsikos, E. N., Nagele, U., Traxer, O., Merseburger, A. S. EAU Guidelines Panel on Lasers, Technologies. EAU guidelines on laser technologies. Eur Urol. 61 (4), 783-795 (2012).
- Braeckman, J., Denis, L. Management of BPH then 2000 and now 2016 – From BPH to BPO. Asian J Urol. 4 (3), 138-147 (2017).
- Bachmann, A., Tubaro, A., Barber, N., d’Ancona, F., Muir, G., Witzsch, U., et al. A European multicenter randomized noninferiority trial comparing 180 W GreenLight XPS laser vaporization and transurethral resection of the prostate for the treatment of benign prostatic obstruction: 12-month results of the GOLIATH study. J Urol. 193 (2), 570-578 (2015).
- Peyronnet, B., Pradere, B., Brichart, N., Bodin, T., Bertrand, P., Members of French Group of GreenLight Users, ., Bruyère, F. Complications associated with photoselective vaporization of the prostate: Categorization by a panel of GreenLight users according to Clavien score and report of a single-center experience. Urology. 84 (3), 657-664 (2014).
- Cho, S. Y., Park, S., Jeong, M. Y., Ro, Y. K., Son, H. 120W GreenLight high performance system laser for benign prostate hyperplasia: 68 patients with 3-year follow-up and analysis of predictors of response. Urology. 80 (2), 396-401 (2012).
- Elmansy, H. M., Elzayat, E., Elhilali, M. M. Holmium laser ablation versus photoselective vaporization of prostate less than 60 cc: Long-term results of a randomized trial. J Urol. 184 (5), 2023-2028 (2010).
- Hong, K., Liu, Y. Q., Lu, J., Xiao, C. L., Huang, Y., Ma, L. L. Efficacy and safety of 120W thulium: Yttrium-aluminum-garnet vapoenucleation of prostates compared with holmium laser enucleation of prostates for benign prostatic hyperplasia. Chin Med J (Engl). 128 (7), 884-889 (2015).
- Hermanns, T., Sulser, T., Fatzer, M., Baumgartner, M. K., Rey, J. M., Sigrist, M. W., et al. Laser fiber deterioration and loss of power output during photo-selective 80-W potassiumtitanyl-phosphate laser vaporization of the prostate. Eur Urol. 55 (3), 679-686 (2009).
- Hermanns, T., Strebel, D. D., Hefermehl, L. J., Gross, O., Mortezavi, A., Müller, A., et al. Lithium triborate laser vaporization of the prostate using the 120 W, high performance system laser: High performance all the way?. J Urol. 185 (6), 2241-2247 (2011).
- Schwartz, J., Renard, J., Wolf, J. P., Moret, M., Iselin, C. E. High-power potassium-titanyl-phosphate laser fibres for endovaporization of benign prostatic hyperplasia: How much do they deteriorate during the procedure?. BJU Int. 107 (12), 1938-1942 (2011).
- Son, H., Ro, Y. K., Min, S. H., Choo, M. S., Kim, J. K., Lee, C. J. Modified vaporization-resection for photoselective vaporization of the prostate using a GreenLight high -performance system 120-W Laser: the Seoul technique. Urology. 77 (2), 427-432 (2011).
- Mandal, S., Sankhwar, S. N., Kathpalia, R., Singh, M. K., Kumar, M., Goel, A., et al. Grading complications after transurethral resection of prostate using modified Clavien classification system and predicting complications using the Charlson comorbidity index. Int Urol Nephrol. 45 (2), 347-354 (2013).
- Gong, Y. G., Liu, R. M., Gao, R. Photoselective vaporesection of the prostate with a front-firing lithium triborate laser: Surgical technique and experience after 215 procedures. Eur Urol. 67 (6), 1142-1159 (2015).

