A Two-Step Method for Percutaneous Transhepatic Choledochoscopic Lithotomy
Summary
This “two-step method” significantly improved the success rate of percutaneous transhepatic choledochoscopy and achieved a better prognosis of intrahepatic and extrahepatic choledocholithiasis.
Abstract
Intrahepatic and extrahepatic choledocholithiasis is a challenge in the field of biliary surgery. We present our experience using a two-step percutaneous transhepatic choledochoscopic lithotomy (PTCSL) procedure to treat challenging biliary stones. We retrospectively reviewed 81 patients with intrahepatic and extrahepatic choledocholithiasis treated using this two-step PTCSL from January 2013 to January 2020, including 40 males and 41 females, with an average age of 66 years. In contrast to traditional percutaneous transhepatic cholangioscopy (PTCS), a channel was established directly through a 16F Amplatz sheath, and the stone in the channel was removed with the aid of a nephroscope. The clinical efficacy and complications of all patients were analyzed. Eighty-one patients (81/81, 100%) had their biliary stones successfully removed; 62/81 patients (76.5%) had biliary stones completely removed after the first operation; 17/81 patients (21%) underwent a second operation; 2/81 patients (2.5%) needed a third operation to completely remove the stones. The incidence of severe bleeding during the operation was 0%, and there were no deaths. The use of the two-step PTCSL method is safe and efficacious, and contributes to a better prognosis of intrahepatic and extrahepatic choledocholithiasis.
Introduction
Intrahepatic and extrahepatic choledocholithiasis is a complex medical problem faced by surgeons and is very common in East Asian countries1. At present, surgical intervention is required for most choledocholithiasis, while the main treatments for bile duct stones include open surgery, percutaneous transhepatic choledochoscopic lithotomy (PTCSL), laparoscopic lithotomy2, percutaneous endoscopic biliary exploration3,4, and endoscopic retrograde cholangiopancreatography. However, patients with bilioenteric anastomosis or Billroth II reconstruction, with an abnormal anatomical structure such as a duodenal periampullary diverticulum, which makes the biliary duct difficult to access through an endoscopic approach5,6,7,8, or who have had previous complex abdominal surgeries, including partial gastrectomy, could not undergo endoscopic therapy or laparoscopic lithotomy. Endoscopic therapy may also not be suitable for hepatolithiasis with large and impacted stones. Therefore, PTCSL, in general, may be a better choice9.
The traditional PTCS approach follows such a procedure to expand the sinus gradually and perform percutaneous transhepatic biliary drainage10,11, which requires a relatively long hospitalization cycle, usually between 2 and 3 weeks, leading to the potential for biliary fistula, biliary tract infection, bleeding, and peritonitis, with multiple expanding sheath sizes. The procedure is composed of two parts. In the first step, the target bile duct is punctured, and the guide wire is inserted while observing the bile outflow. Then, a dilator is used to slowly expand the channel along the guide wire. After the channel is successfully established, the dilator is pulled out, a drain is placed into the target bile duct, and the guide wire is pulled out.
The percutaneous liver puncture and drainage (PTCD) is complete if the bile drainage is unobstructed and the drain is fixed without blood outflow. The sinus tract becomes stable 1 week after PTCD, when it can then be expanded. The guide wire is placed into the drain tube and expanded through the sinus tract along the guide wire with a 10F dilator, and finally placed into a 10F drain. The sinus tract is expanded once a week after surgery, with a 2F size increase each time, so that the sinus tract can be expanded to 16F at 4 weeks after PTCD. In the second step, after expansion of the sinus tract to 16F, the surgery to remove the stone is performed using a biliary fiber lens. Therefore, the traditional PTCSL described above requires a treatment cycle and contributes to high economic pressure for the patients. Moreover, low stone extraction efficiency and repeated and multiple surgical procedures for stone removal are also inevitable disadvantages of traditional PTCS, which limits the use of this technology.
From January 2013, we began to apply PTCS for the minimally invasive treatment of patients with complex intrahepatic and extrahepatic choledocholithiasis in our hospital but modified some key steps of traditional PTCS. In the first step, the surgery was performed at 1 week after PTCD, just when the sinus tract became stable, and the sinus was expanded to 16F directly, using a 16F expander which greatly reduced the preoperative preparation time. In the second step, different from the traditional technology, a Wolf nephroscope was used instead of a traditional choledochoscope to perform the operation, which we refer to as the "two-step PTCSL method." To determine whether the PTCSL procedure was safe, minimally invasive, and efficient, this study retrospectively reviewed 81 patients with intrahepatic and extrahepatic choledocholithiasis treated by the two-step PTCSL method from January 2013 to January 2020.
Protocol
The study was approved by the Ethics Committee of the Second Affiliated Hospital of Shantou University Medical College (Shantou, China).
1. Preparations
- Apply strict exclusion criteria to select patients and obtain signed informed consent forms12 (Table 1).
- Apply the following admission criteria:
- Select patients who voluntarily received the two-step PTCSL treatment.
- Select those patients who were confirmed to have hepatic and extrahepatic bile duct stones by adjuvant examination.
- Select patients who had undergone previous complicated abdominal surgery, such as partial gastrectomy combined with biliary-intestinal anastomosis or Billroth II reconstruction, or who had anatomical abnormalities and were unable to undergo an endoscopic retrograde cholangiao pancreatography (ERCP) examination.
- Select patients with liver function preoperatively assessed as Child-Pugh A or B grades.
- Select patients with normal function of the heart, lung, and other organs.
- Ensure the availability of the laparoscopic imaging system, images of the pneumoperitoneum, Wolf nephroscope, adjustable pressure pump, and hydroelectric lithotripter.
2. Procedure
- Percutaneous transhepatic cholangial drainage (PTCD)
- Insert an indwelling 8F biliary drainage tube 1 week before the operation to drain and reduce the swelling of bile duct.
- Wait for the sinus tract to become stable at 1 week after PTCD.
NOTE: The puncture methodology must be chosen according to the particular area of bile conduit calculi when operating. For example, the left hepatic duct approach is performed under the xiphoid process and abdominal wall of the lower edge of the right costal arch.
3. Percutaneous transhepatic choledochoscopic lithotomy (PTCSL)
- Before administering general anesthesia, instruct the patient to lie flat on the operating table. Following general anesthesia, disinfect the surgical site 3x with iodophor.
- Inject 20 mL of saline into the bile duct along the drainage tube; pull the PTCD tube out after a guide wire is inserted into it.
- For placement of the fascia dilator and sheath, expand the sinus using a 16F expander and join a 16F belt dilator so that the 16F sheath can reach the bile duct where the stone might have been placed.
- After locating the stones, use clamping forceps to both break and remove the stones. For hard stones, use a hydraulic lithotripter to break the stone. Wash out small stones and powdered stones using an adjustable pressure pump. At the end of the procedure, leave a drainage tube inside the patient for 1 week (Figure 1).
Representative Results
All patients had their biliary tract stones cleared successfully, with 58 patients (58/81, 72%) having bile duct stones completely removed after the first operation, 18 patients (18/81, 22%) requiring a second operation, and five patients (5/81, 6%) undergoing a third operation to completely remove the stones. Three patients had recurrent intrahepatic cholelithiasis in the 5th and 6th postoperative years. There were 56 patients (56/81, 68.7%) who underwent percutaneous liver surgery, as well as 25 patients (25/81, 31.3%) who underwent surgery by indwelling a sinus formed by a "T" tube.
The number of stones was equal to one in 70 patients (70/81, 86.6%), equal to two in eight patients (8/81, 10.4%), and greater than or equal to three in three patients (3/81, 3.0%). The stones were all cleared by using lithotomy forceps or a holmium-laser which is more effective in handling hard stones13. The patients required hospitalization at various times during their treatment course. Minor intraoperative biliary bleeding was observed in two patients, and one patient had a biliary infection after surgery, which extended the hospitalization cycle. The average hospital stay was 11 days (range 7-20 days). There was one complication of a small amount of reactive pleural effusion requiring admission (1/81, 1.2%), no deaths, and no massive hemorrhaging of the biliary tract (Table 2).
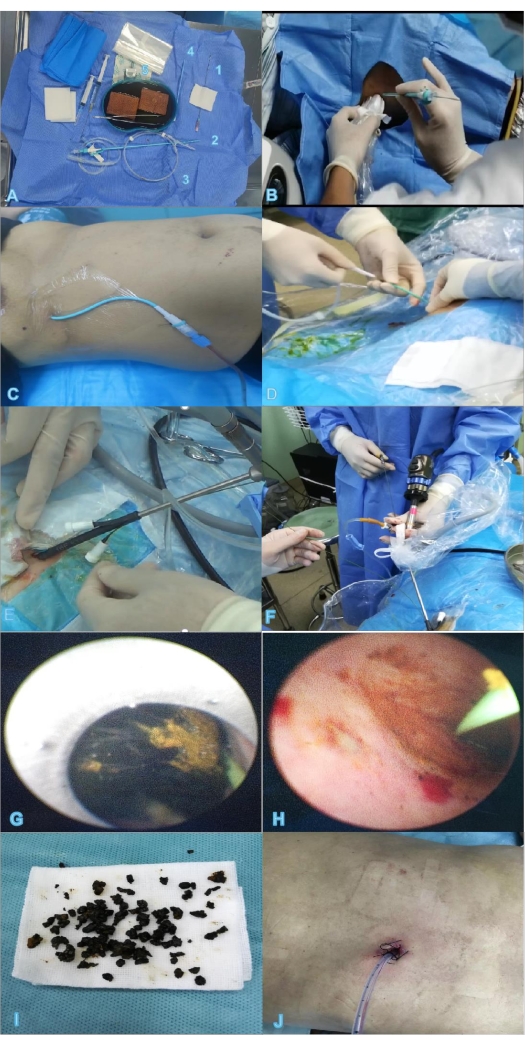
Figure 1: Two-step percutaneous transhepatic choledochoscopic lithotomy. (A) Instruments and materials required for PTCD, for example, puncture needle (1), trocar (2), guide wire (3), expander (4), blade (5). (B) Ultrasound-guided puncture. (C) Indwelling PTCD tube after successful puncture. (D) Insertion of the guide wire. (E,F) Insertion of the percutaneous nephroscope into the sheath to remove stones. (G) Removal of the stone under direct sight. (H) The stone is mostly removed. (I) The removed stone. (J) Two days after extubation, the wound has basically healed. Abbreviation: PTCD = percutaneous transhepatic catheter drainage. Please click here to view a larger version of this figure.
| Variables | n (%) N=81 |
| Age (years) | 66 (19-82) |
| Sex | |
| Male | 40 (49.4%) |
| Female | 41 (50.6%) |
| Surgical history | 60 (74.1%) |
| Principal complaint | |
| Stomachache | 9 (11.1%) |
| Stomachache + Jaundice | 14 (17.3%) |
| Stomachache + Fever | 22 (27.2) |
| Charcot triad | 36 (44.4%) |
| Child-Pugh score | |
| Grade A | 30 (37.0%) |
| Grade B | 51 (63.0%) |
| Grade C | 0 |
| Location of stone | |
| Left lobe | 3 (3.7%) |
| Right lobe | 4 (4.9%) |
| Bilateral | 6 (7.4%) |
| Common bile duct, CBD | 14 (17.3%) |
| CBD + Left lobe | 18 (22.2%) |
| CBD + Right lobe | 9 (11.1%) |
| CBD + Bilateral | 27 (33.4%) |
Table 1: Preoperative data. Abbreviation: CBD = common bile duct.
| Representative Results | Two-step PTCSL method | |
| N=81 | n% | |
| Stone extraction efficiency | 81 | 100% |
| Numbers of operations | ||
| 1 | 58 | 72% |
| 2 | 18 | 22% |
| 3 | 5 | 6% |
| Operation path | ||
| percutaneous transhepatic | 56 | 68.70% |
| "T" tube | 25 | 31.30% |
| Number of stones | ||
| 1 | 70 | 86.60% |
| 2 | 8 | 10.40% |
| ≥3 | 3 | 3.00% |
| Average hospital stay | 11 days | – |
| Complications | ||
| reactive pleural effusion | 1 | 1.20% |
| massive hemorrhage of the biliary tract | 0 | 0% |
| minor intraoperative biliary bleeding | 2 | 2.50% |
| biliary infection | 1 | 1.20% |
| fistula injury | 0 | 0% |
| drainage tube shedding | 0 | 0% |
| recurrence rate | 3 | 3.70% |
Table 2: Representative results. Abbreviation: PTCSL = percutaneous transhepatic choledochoscopic lithotomy.
Discussion
Intrahepatic and extrahepatic choledocholithiasis contribute to biliary obstruction, and the associated cholangitis could lead to gram-negative endotoxemia with clinical manifestations of septic shock or multiorgan dysfunction. Thus, biliary stones represent a complex disease that can be challenging for surgeons, especially in cases of patients who have had previous complex abdominal surgeries or patients with abnormal anatomical structure. PTCSL is being widely used around the world, but there remains a need for innovative, less invasive procedures that can eradicate the stones and restore unobstructed biliary drainage14.
Traditional PTCS requires repeated surgery, a long treatment course, and complications such as biliary infection, bleeding, fistula injury, and drainage tube shedding. However, there are several types of complications, mainly biliary sepsis, haemobilia, and bile duct injuries15,16, occurring in approximately 7% of patients treated with PTCSL. After 10 years post-surgery17,18,19, the recurrence rate for intrahepatic calculi post PTCSL varies from 21% to 40%, and among the patients, bile duct strictures is the main risk factor18. Moreover, the recurrence rate is 45% after 7 years post-surgery20 for common bile duct calculi post-PTCSL. Only three deaths have been reported after PTCSL, which were caused by biliary sepsis16,17.
In this study, the recurrence rate for intrahepatic and extrahepatic choledocholithiasis post PTCSL is 3.70%, and PTCSL shortens the whole lithotripsy period, operation time, and the distance between skin entrance sites and targeted biliary ducts. In addition, biliary duct dilation times and intraoperative blood losses were also slightly reduced. In our opinion, the two-step PTCSL method is advantageous compared with traditional PTCS. In the first step, the surgery is performed at the time when the sinus tract becomes stable at 1 week after PTCD, and the sinus is directly expanded using a 16F expander; this not only greatly reduces the preoperative preparation time but also reduces the friction against the bile duct caused by the expander to greatly decrease hemorrhaging of the biliary tract. In the second step, a Wolf nephroscope, instead of a traditional choledochoscope, is used to perform the operation, which reduces the financial burden on the patients and makes it easier to remove the stones, so that the treatment is minimally invasive for cholangioscopic lithotripsy.
However, there are some limitations to this method. First, this is a retrospective study of patients undergoing the two-step PTCSL procedure in this hospital. Hence, there was inevitable selection bias when the patients were enrolled. Therefore, comparison with other techniques in prospective randomized trials is essential to future applications of this technique. Second, some patients in this report lacked long-term follow-up data that may impact the results. Third, the sample size of this study was limited because the number of patients undergoing two-step PTCSL was quite small. These results need to be confirmed in larger populations in multiple centers. In conclusion, PTCSL may generally be a better choice for the treatment of complex intrahepatic and extrahepatic choledocholithiasis. This two-step PTCSL procedure is easy to learn and may be a safe and effective way to achieve better prognosis of intrahepatic and extrahepatic choledocholithiasis.
Disclosures
The authors have nothing to disclose.
Acknowledgements
None.
Materials
| 0.9% Normal saline solution | – | ||
| 16-F series fascia dilator | type PLVW, Cook Medical | ||
| adjustable pressure pump | type APL; Guangzhou Jielun Medical Equipment Co. , Ltd, Guangdong Province, China | ||
| biliary balloon dilator | ATB advance; Cook Medical | ||
| blade | – | ||
| camera system | 1088i HD Camera Control Unit, PAL 220 V; Stryker Corporation | ||
| Cavity mirror protective sleeve | – | ||
| clamp | 5Fr, Richard Wolf GmbH, Germany | ||
| color ultrasound machine | DC-N2S, Mindray | ||
| Cook net basket | NGE-017115-MB, COOK Medical Inc. , Bloomington, USA | ||
| drainage pack | – | ||
| expander | – | ||
| guide wire | – | ||
| hydroelectric lithotripter | Aymed Medical,  stanbul, Turkey stanbul, Turkey |
||
| Iodophor | – | ||
| Kidney basin | – | ||
| light source | Voice-control compatible X8000 Xenon Light Source of 300 W;Stryker Corporation, MI | ||
| Medical syringe | – | ||
| puncture needle | – | ||
| suction apparatus | – | ||
| surgical gauze | – | ||
| trocar | – | ||
| Wolf nephroscope | 12-degree Ultra-Wide-Angle Ureteroreno-scope; Richard Wolf GmbH, Germany | ||
| zebra guide wire | type HAW; Cook Medical, Bloomington, IN |
References
- Shu, J., et al. Robotic-assisted laparoscopic surgery for complex hepatolithiasis: a propensity score matching analysis. Surgical Endoscopy. 33 (8), 2539-2547 (2019).
- Korkes, F., et al. Percutaneous treatment of complex biliary stone disease using endourological technique and literature review. Einstein. 13 (4), 611-615 (2015).
- Gamal, E. M., et al. Percutaneous video choledochoscopic treatment of retained biliary stones via dilated t-tube tract. Surgical Endoscopy. 15 (5), 473-476 (2001).
- Khalid, M., et al. Percutaneous endoscopic biliary exploration in complex biliary stone disease: Case series study. International Journal of Surgery. 24, 73-78 (2020).
- Kim, J. H., et al. Percutaneous transhepatic cholangioscopic treatment of patients with benign bilio-enteric anastomotic strictures. Gastrointestinal Endoscopy. 58 (5), 733-738 (2003).
- Hwang, J. H., et al. Risk factors for recurrent cholangitis after initial hepatolithiasis treatment. Journal of Clinical Gastroenterology. 38 (4), 364-367 (2004).
- Bonnel, D. H., et al. Common bile duct and intrahepatic stones: results of transhepatic electrohydraulic lithotripsy in 50 patients. Radiology. 180 (2), 345-348 (1991).
- Kondo, S., et al. A clinicopathologic study of primary cholesterol hepatolithiasis. Hepato-gastroenterology. 42 (5), 478-486 (1995).
- Williams, E., et al. Updated guideline on the management of common bile duct stones (CBDS). Gut. 66 (5), 765-782 (2017).
- Makuuchi, M., et al. Ultrasonically guided cholangiography and bile drainage. Ultrasound in Medicine & Biology. 10 (5), 617-623 (1984).
- Jeng, K. S., et al. Percutaneous transhepatic cholangioscopy in the treatment of complicated intrahepatic biliary strictures and hepatolithiasis with internal metallic stent. Surgical Laparoscopy. 10 (5), 278-283 (2000).
- Zhuo, H., et al. Percutaneous transhepatic choledochoscopic lithotomy (PTCSL) is effective for the treatment of intrahepatic and extrahepatic choledocholithiasis. Surgical Laparoscopy, Endoscopy & Percutaneous Techniques. 31 (3), 326-330 (2020).
- Hazey, J. W., McCreary, M., Guy, G., Melvin, W. S. Efficacy of percutaneous treatment of biliary tract calculi using the holmium: YAG laser. Surgical Endoscopy. 21 (7), 1180-1183 (2007).
- Ozturk, A., et al. New surgical technique applied with urological instruments in bilobar multiple hepatolithiasis: Ultra-mini percutaneous hepatolithotomy. Turkish Journal of Urology. 43 (3), 371-377 (2017).
- Ozcan, N., et al. Percutaneous transhepatic removal of bile duct stones: results of 261 patients. Cardiovascular and Interventional Radiology. 35 (3), 621-627 (2012).
- Kint, J. F., et al. Percutaneous treatment of common bile duct stones: results and complications in 110 consecutive patients. Digestive Surgery. 32 (1), 9-15 (2015).
- Yeh, Y. H., et al. Percutaneous trans-hepatic cholangioscopy and lithotripsy in the treatment of intrahepatic stones: a study with 5 year follow-up. Gastrointestinal Endoscopy. 42 (1), 13-18 (1995).
- Jan, Y. Y., et al. Percutaneous trans-hepatic cholangioscopic lithotomy for hepatolithiasis: long-term results. Chang Gung Medical Journal. 17 (1), 149 (1994).
- Cheon, Y. K., et al. Evaluation of long-term results and recurrent factors after operative and nonoperative treatment for hepatolithiasis. Surgery. 146 (5), 843-853 (2009).
- Tsutsumi, K., et al. A comparative evaluation of treatment methods for bile duct stones after hepaticojejunostomy between percutaneous transhepatic cholangioscopy and peroral, short double-balloon enteroscopy. Therapeutic Advances in Gastroenterology. 10 (1), 54-67 (2017).

