A Training Program Using an Agility Ladder for Community-Dwelling Older Adults
Summary
The aim of this study is to present an agility training program for older people. The feasibility of this program is described, and the training protocol demonstrated by video imaging.
Abstract
Aging impairs physical and cognitive functions and limits daily activities. Agility training can improve or maintain physical functioning in older people. The purpose of this study is to report the physical fitness benefits of a training program for independent community-dwelling older adults using an agility ladder. Each training session lasted approximately 30 minutes, and the benefits were achieved with two sessions per week for 14 weeks. Training was timed and involved four different drills and varying levels of difficulty through time. The exercises were performed at the School of Physical Education of the University of Campinas, São Paulo state, Brazil. The study participants (n = 16; mean age of 66.9 ± 5.0 years) were instructed to perform the exercises as quickly as possible without making mistakes and were assisted by a physical trainer when they made mistakes. Assessments were performed both before and after training using five functional tests (i.e., Illinois agility, five times sit-to-stand, timed up-and-go, walking usual speed, and one-leg stand). Although the study sample was not compared with a control group, the results indicate that training protocols using an agility ladder are easy and practical and improve physical function performance in older adults.
Introduction
Being active while aging can optimize opportunities to improve physical, social, and mental health, enabling older people to participate actively in society1. Older adults should be payed attention to because of the consequences of aging2. People worldwide are living longer, and life expectancy is greater than 70 years for the first time in history. The number of individuals aged 60 years or older is increasing rapidly, and the health of these populations is usually poor. Aging impairs physical functions, mental capacity, and social interactions as a direct result of diseases or syndromes2.
Decrease in physical function may lead to falls, fractures, less access to health care, depression, and poor quality of life. Agility is crucial to prevent falls and maintain independence in older people. Sheppard and Young3 reported that agility involved "whole-body movements in different directions in response to a stimulus."
Most studies evaluate agility in high-performance athletes4, although a few studies assess this parameter in older adults. Agility training for older people comprises preplanned gait adaptability training and reaction training (i.e., response to a signal)5. Liu-Ambrose et al.6,7 found that agility training improved postural stability, balance, and balance confidence, and decreased the risk of falls in older people. Moreover, this type of training is integrative and improves cognitive functions (e.g., perception, mental flexibility, and working memory) as well as neuromuscular and cardiovascular functions8,9.
Agility training is characterized by a set of exercise drills and can be automated. However, a physical trainer/instructor is necessary to create and teach the drills and indicate the right moment to increase the level of difficulty. Some studies found that step training improved physical fitness (e.g., balance, agility, lower limb strength and power, and decreased risk of falls) and cognitive function (e.g., choice stepping reaction time, inhibitory action, and executive function)5,10,11. The present study uses an agility ladder as a cost-effective instrument to assess the effects of preplanned gait training on the physical fitness of independent community-dwelling older adults.
The agility ladder used in the present study was previously employed to train school children and athletes12,13. The ladder had a length of 4.8 meters and 12 transverse rungs and was drawn on the floor using a 2 cm wide adhesive tape (Figure 1). Building a ladder on the floor avoided interruptions during training12 and decreased the risk of injuries. The study population was healthy, with a mean age of 66.9 ± 5.0 years, and lived independently in a community setting. The participants received 30 minute training sessions twice a week for 14 weeks.
Protocol
The study was approved by the Research Ethics Committee of the University of Campinas (UNICAMP) under Protocol Number 2479761. Written informed consent was obtained in-person from all study participants. Sixteen participants of both sexes were recruited from the community of the metropolitan region of Campinas by searching the database of the Applied Kinesiology Laboratory (AKL). The inclusion criteria were 1) individuals aged 60 and older; 2) ability to answer the questionnaires used in this study; 3) ability to walk independently without difficulty; 4) availability to participate in the intervention during 3 months with at least 90% attendance. The exclusion criteria were 1) severe cardiovascular or pulmonary diseases; 2) orthopedic diseases that prevented performing daily activities; and 3) diseases that increased the risk of falls such as Parkinson's and Alzheimer's. All assessments were performed by researchers and professional physical trainers from the AKL.
1. Assessment
- Assess physical fitness using the following functional tests: Illinois agility, five times sit-to-stand, timed up-and-go, walking usual speed, and one-leg stand. Perform all tests before and after training.
NOTE: Here, the participants repeated each test 2x, and the best result was used.- Illinois agility test: Have the participants move through obstacles in multiple directions.
- The length of the course is 10 m and the width is 5 m. Place a marking cone in each corner of the course: a start and finish cone at one end, 5 m apart; two at the turning points on the other end of the course, 5 m apart; and four cones in the center of the course spaced 3.3 m apart from each other.
- Have the participants jog in a straight line from the start line to the first turning point and then in the opposite direction towards the first center cone. They should weave back and forth through the four center cones from one end of the course to the other. Then, they should run diagonally from the first center cone to the second turning point located on the far right and then in the opposite direction towards the finish line14.
- Five times sit-to-stand test: Have the participants rise from a chair 5x as quickly as possible with the arms crossed in front of the body, lifting the hips from the chair when the timer is started. The participants should stand up completely by extending the knees and sit down completely by maintaining the back against the chair15. Stop the timer after the participant sits down for the fifth time.
- Timed up-and-go (TUG) test: Have the participants get up from a chair without pushing up with their arms, walk as quickly as possible along a 3 m line demarcated on the floor upon hearing the command "Go," return to the same position, and sit down on the chair again. Timing starts as the participants get up from their chair and stopped when the participant sits down16.
- Walking usual speed test: Have the participants walk 10 m at their usual gait. Start the timer when a foot reaches the 1 m line and stop when a foot reaches the 11 m line. Do not include the first and last 1 m stretches in the analysis because they are used to measure acceleration and deceleration, respectively17. Present the results as velocity in m/s (Figure 2).
- One-leg stand test: Have the participants stand on the foot from the dominant leg while flexing the contralateral knee at 90°, folding the arms across the chest, and maintaining the head straight. Have the participants lift one foot from the floor when the timer is activated. Stop the timer when the foot touches the floor again. The maximum balance time is 30 seconds for each side. Test both legs18.
- Illinois agility test: Have the participants move through obstacles in multiple directions.
2. Training program design
- Have the participants perform agility training for 12 min, including four 3 min sets with a 1 min rest between each set (i.e., the first set starts with sequence 1). Each set is composed of four 30 s subsets, a 15 s rest between subsets (Figure 3), and 1 min rest between sets.
- In addition to the four exercise sequences, include a 10 min warm-up and 5 min cool-down, using whole-body low-intensity stretching.
NOTE: During this program, each participant trained 2x per week for 14 weeks.
- In addition to the four exercise sequences, include a 10 min warm-up and 5 min cool-down, using whole-body low-intensity stretching.
- Increase the level of difficulty by augmenting exercise complexity and volume, depending on individual adaptation to the program. The level of adaptation dictates the level of increase in the velocity of the drills.
- Increase training complexity after 6 weeks of training with four sequences of coordination. After a period of adaptation, substitute sequences 2 and 3 for more challenging drills.
- Increase the training time after 10 weeks of training. Start with 12 min of exercise (four 3 min sets) and end with 15 min (five 3 min sets).
NOTE: At the end of each 30 s subset, the time taken to perform the activity is recorded. This procedure allows comparison of the distance travelled by each participant during each session of the training program.
3. Agility ladder
- Perform the exercises using a ladder with a length of 4.8 m and 12 transverse rungs forming 12 squares (areas delimited by the rungs) measuring 40 cm 40 cm (Figure 1). Instruct the study subjects to step in the squares and not on the rungs.
4. Familiarization period
- Perform four sequences of the training program (1, 2A, 3A, and 4) during the 2 week familiarization period. Exercise sessions were spaced at least 48 h apart, and there was no time limit to complete the sequences in each session. Instruct the participants to practice these sequences to perform as well as possible during the training period.
5. Training program
NOTE: All drills start with both feet together on the start line.
- Sequence 1: Have participants place their left foot in the first square, the right foot in the second square, and so forth (Figure 4). Each sequence should be performed in both directions on the ladder for 30 s.
- Sequence 2A: Have participants position their right foot in the first square, then position the toes of the left foot in the first square, move the left foot to the second square, place the toes of the right foot on the second square, and so on (Figure 5).
- Sequence 2B: Increase the level of difficulty depending on individual adaptation to sequence 2A (Figure 6) by having participants move through the ladder in small jumps, with toe-tapping movements.
- Have participants jump to the first square with both feet together such that the sole of the right foot touches the ground while the toes of the left foot touch the ground.
- Then, have them jump to the second square with both feet together, ensuring that the sole of the left foot touches the ground while the toes of the right foot touch the ground.
- Have subjects repeat this sequence until the end of the ladder.
- Sequence 3A: Have participants perform the drill with diagonal and lateral movements.
- Have them place their left foot, followed by the right foot, outside the first square to the left.
- Then, have them put the right foot in the first square, followed by the left foot. They will then place the right foot outside the second square to the right, followed by the left foot.
- Have subjects continue this sequence until the end of the ladder (Figure 7).
- Sequence 3B: Use this sequence to increase the difficulty level depending on individual adaptation to sequence 3A.
- Have participants position their left foot outside the ladder next to the first square to the left, and then the right foot in the first square, followed by the left foot, maintaining both feet together. Then, they will put the right foot outside the second square to the right and then the left foot in the second square, followed by the right foot, keeping both feet together (Figure 8).
- Sequence 4: Have participants place their right foot in the first square, the left foot outside the ladder to the left next to the rung separating the first and second squares, and the right foot outside the ladder across from the left foot.
- Have participants put the left foot in the second square, the right foot outside the ladder to the right next to the rung separating the second and third squares, and the left foot outside the ladder opposite the right foot. Have the subjects follow this pattern until the end of the ladder (Figure 9).
Representative Results
Sixteen male and female independent community-living older people with a mean age of 66.9 ± 5.0 years were enrolled in the study. The interventions and assessments were performed at the School of Physical Education of UNICAMP.
Statistical analysis was performed using Minitab 18 software. The Mann-Whitney test was used to compare the functional test results before and after training. P values smaller than 0.05 were considered significant. Delta was calculated as follows: (baseline values – post-training values) / baseline values x 100.
Significant differences between before and after training were determined using physical function tests to assess agility (Illinois test), lower limb strength and power (five times sit-to-stand), dynamic balance (TUG), gait (walking usual speed test), and static balance (one-leg stand).
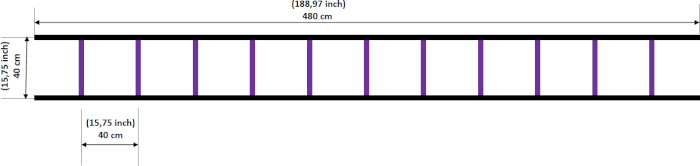
Figure 1: Agility ladder. The ladder had a length of 4.8 m and 12 rungs, forming 12 squares (40 cm x 40 cm). Please click here to view a larger version of this figure.
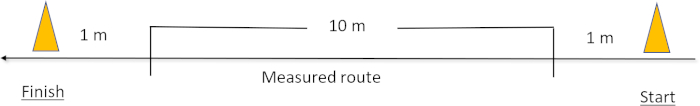
Figure 2: Walking usual speed test. Please click here to view a larger version of this figure.
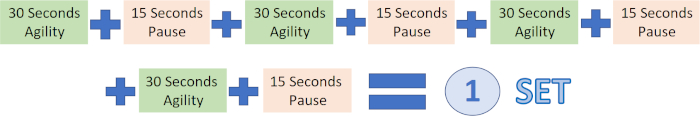
Figure 3: Exercise set. Each 3-min set was composed of four 30 s subsets and a 15 s rest between subsets. Please click here to view a larger version of this figure.
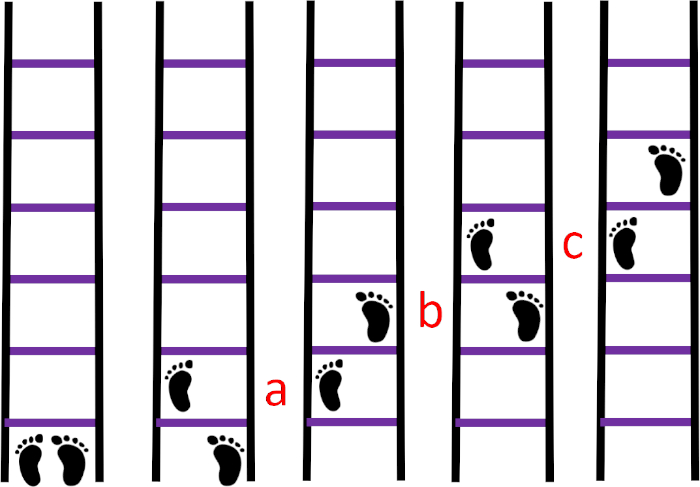
Figure 4: Sequence 1. (A) the left foot in the first square, (B) the right foot in the second square, (C) the left foot in the third square. Please click here to view a larger version of this figure.
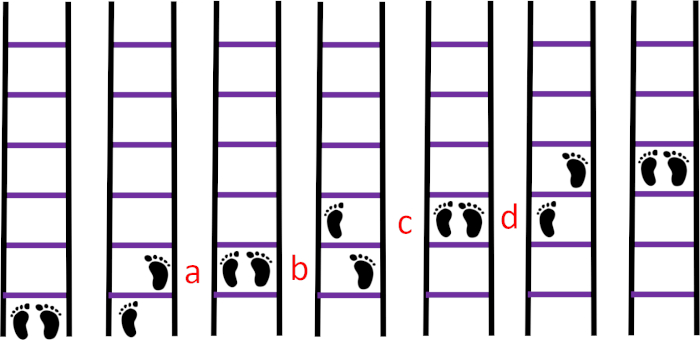
Figure 5: Sequence 2A. (A) The right foot in the first square, (B) the left foot in the first square, (C) the left foot in the second square, (D) the right foot in the second square. Please click here to view a larger version of this figure.
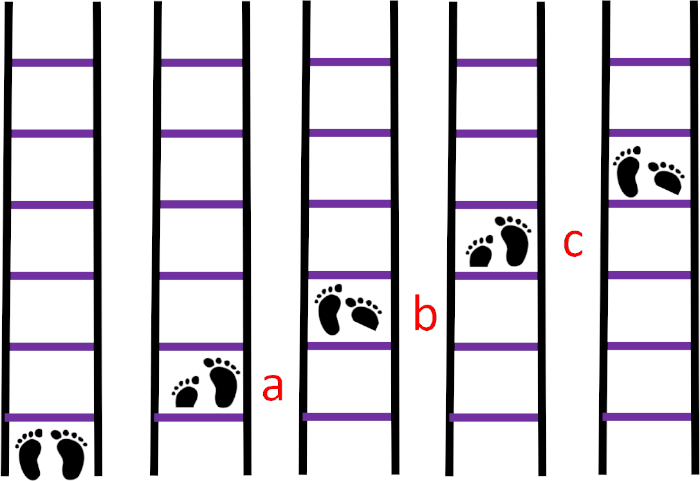
Figure 6: Sequence 2B. (A) The right foot in the first square and the toes of the left foot in the first square, (B) the left foot in the second square and the toes of the right foot in the second square, (C) the right foot in the third square and the toes of the left foot in the third square. Please click here to view a larger version of this figure.
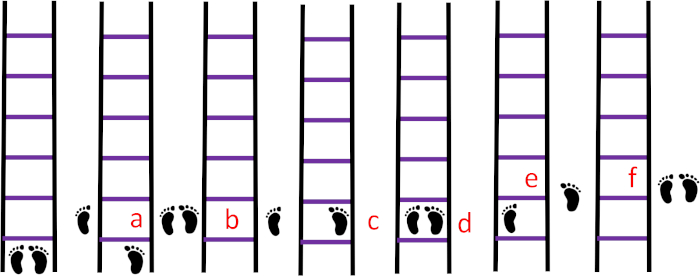
Figure 7: Sequence 3A. (A) The left foot outside the ladder to the left next to the first square, (B) the right foot outside the ladder next to the left foot, (C) the right foot in the first square, (D) the left foot in the first square, (E) the right foot outside the ladder to the right next to the first square, (F) the left foot next to the right foot. Please click here to view a larger version of this figure.
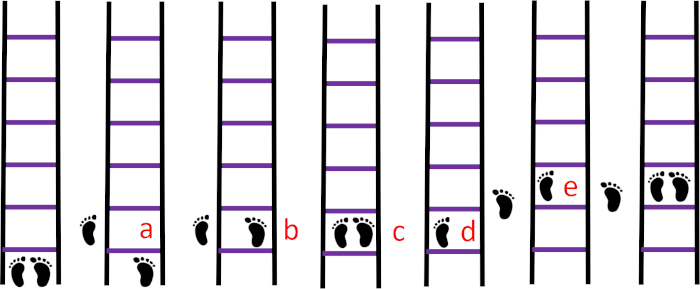
Figure 8: Sequence 3B. (A) The left foot outside the ladder to the left next to the first square, (B) the right foot in the first square, (C) the left foot next to the right foot, (D) the right foot outside of the ladder to the right next to the first square, (E) the left foot next to the right foot. Please click here to view a larger version of this figure.
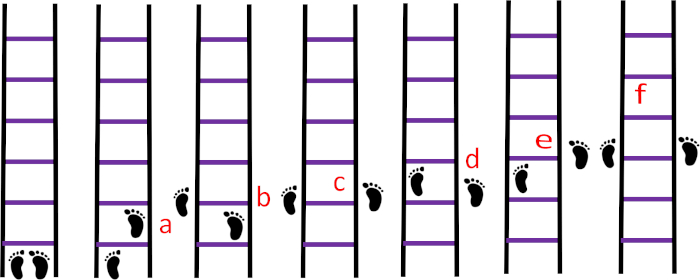
Figure 9: Sequence 4. (A) The right foot in the first square, (B) the left foot outside the ladder to the left next to the rung that separates the first and second squares, (C) the right foot outside the ladder to the right across from the left foot, (D) the left foot in the second square, (E) the right foot outside the ladder to the right next to the rung that separates the second and third squares, (F) the left foot outside the ladder across from the right foot. Please click here to view a larger version of this figure.
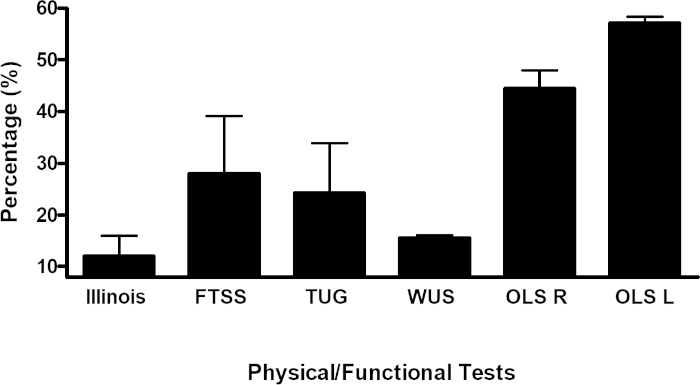
Figure 10: Delta values of the function test results. The percentage of training (delta) of each measurement was assessed over time. FTSS, five times sit-to-stand; WS, walking speed; TUG, timed up-and-go; OLS, one-leg stand using the right left (R) and left leg (L). Please click here to view a larger version of this figure.
| Tests | Pre | Post | P-Value |
| Illinois (s) | 35.9 ± 5.4 | 31.5 ± 4.5 | 0.02* |
| FTSS (s) | 10.7 ± 2.0 | 7.7 ± 1,1 | <0.01* |
| TUG (s) | 7.7 ± 1.2 | 5.8 ± 0.7 | <0.01* |
| WS (m/s) | 1.3 ± 0.1 | 1.5 ± 0,1 | <0.01* |
| OLS R (s) | 16.4 ± 10.4 | 23.7 ± 9.0 | 0.03* |
| OLS L (s) | 15.7 ± 8.5 | 24.6 ± 8.1 | 0.01* |
Table 1: Functional test results at baseline and post-training. Data are presented as means ± standard deviations and were considered significantly different at p < 0.05. *The Mann-Whitney test was used to compare differences between before and after training. FTSS, five times sit-to-stand; WS, walking speed; TUG, timed up-and-go; OLS, one-leg stand (OLS); R, right leg; L, left leg.
Discussion
Several agility training programs are used for different populations, including sports teams4, children12, and older people6,10. These programs include square stepping exercises10,11 like the sequences described in the present study and can significantly improve the overall physical fitness of older adults by decreasing the risk of falls, fractures, immobilizations, and dependence.
The training protocol presented in this study, with explanations about exercise drills and training volume and intensity, constitutes another approach to improve agility in older people. This protocol is cost-effective, practical, readily accessible, and easily adapted to specific populations by changing velocity and complexity19. Furthermore, this method improved physical fitness even in robust and healthy populations.
The literature stresses the importance of using power exercises for older people. Muscle power is decreased with advancing age20. Therefore, neuromuscular performance is reduced even in robust and healthy older adults. This study reports an alternative training method using an agility ladder to help improve or maintain muscle power. Furthermore, the outcomes can be compared with those of other training programs, such as square stepping, which present physical and cognitive benefits10. Older people can benefit from several stimuli from a single exercise8,10.
This type of training can be included in multicomponent exercise programs for older people and has been shown to improve muscle strength and power, physical endurance, flexibility, and balance21. Nonetheless, few studies have evaluated the benefits of agility training in multicomponent programs, and most of these programs do not contemplate agility training21. Nevertheless, agility training can be included in multicomponent training because it improves physical functioning in older adults5,10,11, as demonstrated in the present study.
Agility ladders are effective for health training in specific population groups (e.g., populations with mild cognitive impairment who had a stroke). Furthermore, the complexity of coordination in preplanned gait and reaction training improves executive function5,6,9,11.
The study population was robust, healthy, and physically active. Therefore, further studies are necessary to assess the potential benefits of this protocol in frail and inactive older people. The two main limitations of this study were the small sample size and the lack of a control group. For this reason, the present results were not compared with those of a group that did not receive the intervention or those in traditional strength or endurance training programs. Notwithstanding, the present exercise protocol significantly improved overall physical fitness in this population.
Declarações
The authors have nothing to disclose.
Acknowledgements
This study was funded by the Coordination for the Improvement of Higher Education Personnel of Brazil (CAPES- #1800789).
Materials
| Bluetooth speaker | JBL | – | Used to time all protocol and signal the 30 s of each subset |
| Chair | – | – | Used on assessments |
| Clipboard | Tilibra | – | Used to support documents |
| Crepe Tape of 2cm | Dexter | – | Used to create the agility ladder on the floor |
| Measuring Tape | Stakley | – | Used to measure assessments distance |
| Pen | Bic | – | Used to note data |
| Saucer Cone | Kipsta | – | Used on assessments |
| Stowatch | Vollo | – | Used to time assessments results |
| Sulfite Paper | Chamex | – | used to write all data |
Referências
- Álvarez-García, J., Durán-Sánchez, A., Del Río-Rama, M. C., García-Vélez, D. F. Active ageing: Mapping of scientific coverage. International Journal of Environmental Research and Public Health. 15 (12), E2727 (2018).
- Weil, A. Aging And Health. Health Affairs. 34 (1), 6 (2018).
- Sheppard, J., Young, W. Agility literature review: Classifications, training and testing. Journal of Sports Sciences. 24 (9), 919-932 (2006).
- Paul, D. J., Gabbett, T. J., Nassis, G. P. Agility in Team Sports: Testing, Training and Factors Affecting Performance. Sports Medicine. 46 (3), 421-442 (2016).
- Okubo, Y., Schoene, D., Lord, S. R. Step training improves reaction time, gait and balance and reduces falls in older people: A systematic review and meta-analysis. British Journal of Sports Medicine. 51 (7), 586-593 (2017).
- Liu-Ambrose, T., et al. Resistance and Agility Training Reduce Fall Risk in Women Aged 75 to 85 with Low Bone Mass: A 6-Month Randomized, Controlled Trial. Journal of the American Geriatrics Society. 52 (5), 657-665 (2004).
- Liu-Ambrose, T., Khan, K. M., Eng, J. J., Lord, S. R., McKay, H. A. Balance confidence improves with resistance or agility training: Increase is not correlated with objective changes in fall risk and physical abilities. Gerontology. 50 (6), 373-382 (2004).
- Donath, L., van Dieën, J., Faude, O. Exercise-Based Fall Prevention in the Elderly: What About Agility?. Sports Medicine. 46 (2), 143-149 (2016).
- Diamond, A. Executive Functions. Annual Review of Clinical Psychology. 64 (1), 135-168 (2014).
- Shigematsu, R., et al. Square-Stepping Exercise and Fall Risk Factors in Older Adults: A Single-Blind, Randomized Controlled Trial. Journals of Gerontology Series A Biological Sciences & Medical Sciences. 63 (1), 76-82 (2008).
- Teixeira, C. V. L., et al. Effect of square-stepping exercise and basic exercises on functional fitness of older adults. Geriatrics and Gerontology International. 13 (4), 842-848 (2013).
- Ng, R., Cheung, C. W., Kim Wai Sum, R. Effects of 6-week agility ladder drills during recess intervention on dynamic balance performance. Journal of Physical Education and Sport. 17 (1), 306-311 (2017).
- Pawar, S. B., Pradeep, B. Effect of ladder drills training in female kabaddi players. International Journal of Physical Education, Sports and Health. 180 (2), 180-184 (2018).
- Raya, M. A., et al. Comparison of three agility tests with male servicemembers: Edgren Side Step Test, T-Test, and Illinois Agility Test. Journal of Rehabilitation Research and Development. 50 (7), 951-960 (2013).
- Buatois, S., et al. Five times sit to stand test is a predictor of recurrent falls in healthy community-living subjects aged 65 and older. Journal of the American Geriatrics Society. 56 (8), 1575-1577 (2008).
- Podsiadlo, D., Richardson, S. The Timed “Up & Go”: A Test of Basic Functional Mobility for Frail Elderly Persons. Journal of the American Geriatrics Society. 39 (2), 142-148 (1991).
- Yamada, M., et al. Prevalence of sarcopenia in community-dwelling Japanese older adults. Journal of the American Medical Directors Association. 14 (12), 911-915 (2013).
- Briggs, R. C., Gossman, M. R., Birch, R., Drews, J. E., Shaddeau, S. A. Balance performance among noninstitutionalized elderly women. Physical Therapy. 69 (9), 748-756 (1989).
- Yamada, M., Tanaka, B., Nagai, K., Aoyama, T., Ichihashi, N. Rhythmic stepping exercise under cognitive conditions improves fall risk factors in community-dwelling older adults: Preliminary results of a cluster-randomized controlled trial. Aging & Mental Health. 15 (5), 647-653 (2011).
- Reid, K. F., Fielding, R. A. Skeletal muscle power: A critical determinant of physical functioning in older adults. Exercise and Sport Sciences Reviews. 40 (1), 4-12 (2012).
- Bouaziz, W., et al. Health benefits of multicomponent training programmes in seniors: a systematic review. International Journal of Clinical Practice. 70 (7), 520-536 (2016).

