Early Weight-Bearing Rehabilitation Protocol After Anterior Cruciate Ligament Reconstruction
Summary
Based on the safety and feasibility, this article presents an early weight-bearing rehabilitation protocol after anterior cruciate ligament reconstruction. The protocol is clear and easy to operate, which is helpful to promote its use in clinical practice and accelerate the functional recovery of patients.
Abstract
Anterior cruciate ligament (ACL) injury is one of the common sports injuries. Anterior cruciate ligament reconstruction (ACLR) is the mainstream treatment for ACL injury, aiming to regain normal anatomical structure and stability of the knee joint and promote the patient’s return to sports. Under the guidance of the concept of enhanced recovery after surgery, early weight-bearing rehabilitation (EWB) is an important factor affecting patient function and quality of life. However, there is no consensus on whether EWB rehabilitation can be performed after ACL surgery.
This study aims to explore the safety and feasibility of EWB after ACL surgery. The study implemented a gradual EWB rehabilitation program in the experimental group, including weight-shifting training, balance training, and gait training on the affected lower limb, and assessed wound healing and stability of the knee joint. The study found that EWB after ACLR is safe and feasible. EWB rehabilitation not only does not pose a negative effect on the patient’s knee pain, swelling, wound healing, and stability, but also helps to improve knee active flexion and quality of life faster and better. The EWB program in this study is simple, safe, and effective, and it provides strong theoretical guidance and practical demonstration for accelerated rehabilitation after ACLR.
Introduction
Enhanced Recovery after Surgery (ERAS) is a concept that promotes the early initiation of postsurgery rehabilitation care units, particularly after orthopedic operations, when conditions are appropriate1. This approach seeks to shift the clinical focus from treating the disease to functional rehabilitation promptly with the goal of reducing hospital stays, minimizing postoperative complications, improving patient prognosis and satisfaction, and enhancing overall rehabilitation outcomes. Since the introduction of ERAS, Chinese orthopedic rehabilitation specialist, Zhou Mouwang, has advocated for the active application of accelerated recovery protocols to further progress perioperative rehabilitation practices within the realm of Chinese orthopedics2. Internationally recognized consensus guidelines have also been established to facilitate enhanced surgical recovery for orthopedic conditions such as joint replacement and spine surgery3. Nonetheless, while considerable advancements have been made in implementing ERAS in recent years, the primary application has been in major operations, such as joint replacement surgeries4. As a result, there is a pressing need to further investigate and expand the application of ERAS within the rehabilitation of other orthopedic conditions.
The anterior cruciate ligament (ACL) plays a pivotal role in maintaining knee joint stability. ACL injuries are among the most prevalent sports-related injuries, with approximately 2 million cases occurring worldwide annually5. Anterior cruciate ligament reconstruction (ACLR) is the mainstream treatment approach, aiming to restore normal knee anatomy and stability, prevent secondary injuries, and enable patients’ return to sport. Rehabilitation following ACL injury has been an active research area. It is widely accepted that post ACLR rehabilitation is integral for optimizing surgical outcomes and facilitating patients’ recovery of sports-related function6,7. However, early weight-bearing (EWB) rehabilitation protocols after ACLR remain understudied, leading to a lack of consensus among clinicians.
The latest research in 2021 supports allowing immediate weight-bearing and full knee range of motion within tolerance after ACL autograft reconstruction surgery7. However, a consensus has not yet been reached in clinical practice. The authoritative British Journal of Sports Medicine published in 2016 also advocates for immediate weight-bearing post ACLR, finding it does not increase knee joint laxity. If gait is proper without increased pain or effusion during/after walking, immediate weight-bearing is considered acceptable6. In contrast, a review in 2022 summarizes that accelerated weight-bearing rehabilitation following ACLR may increase risks of knee joint laxity and bone tunnel widening compared to delayed weight-bearing protocols, advising cautious selection of postoperative regimens8. Additional concerns with EWB include knee pain, swelling, effusion, wound healing, and fall risks after ACLR. Although substantial literature endorses EWB after ACLR, clinical practices still vary. A study in 20209 found that surgeon experience influences post ACLR weight-bearing timelines in France; more experienced surgeons were more likely to favor EWB rehabilitation.
Under the guidance of the ERAS concept, EWB is an important factor affecting patient function and quality of life. However, whether the EWB program could impair wound healing, increase pain and swelling, or impact knee stability remains a key concern for orthopedic and rehabilitation clinicians. In view of the current dilemma of clinicians and inconsistent research results, this study aims to explore the safety and feasibility of EWB after ACLR.
Protocol
This protocol has been approved by the Ethics Committee of Shanghai First People's Hospital (project number: 2022SQ470).
1. Study design
- Ensure that the study is single-blind: researchers will be aware of group assignments but they will not inform participants of their allocation.
- Random grouping: Ensure that the researchers use a random number table and randomly divide the participants into two groups at a 1:1 ratio. The control group (CG) will receive early non-weight-bearing rehabilitation while the experimental group (EG) will receive EWB.
- Power calculation
- Use analysis software to conduct power analysis to obtain the minimum sample size required for statistical results, refer to existing research, and consider study design to define the assumed drop-out rate.
NOTE: The power analysis of this study was based on an independent t-test assuming equal variance. The two-sided significance level was set at an alpha level of 0.05 and a power of 0.8. The results of the power calculation revealed that a total of 34 participants were needed. Considering a drop-out rate of ~10%, we planned to recruit 38 participants.
- Use analysis software to conduct power analysis to obtain the minimum sample size required for statistical results, refer to existing research, and consider study design to define the assumed drop-out rate.
2. Participant recruitment (see Figure 1)
NOTE: The research team selected 38 patients who underwent ACLR at Shanghai First People's Hospital from July 2022 to November 2022 based on the inclusion and exclusion criteria. They were divided into experimental and control groups with 19 participants. General demographic information and clinical indicators, including gender, age, graft type, degree of meniscal repair, pain intensity, and wound healing status, were collected.
- Set the inclusion criteria to patients who had undergone ACLR surgery, patients between the ages of 16 and 55, and those who show good compliance and signed the informed consent form.
- Set the exclusion criteria to be concomitant other bone and joint injuries affecting normal activity; concomitant radioactive or complicated or other unstable meniscal tears; and patients with severe complications such as postoperative fever, poor wound healing, and lower extremity deep vein thrombosis.
3. Rehabilitation treatment plan
- Give patients in both groups the same preoperative and postoperative health education programs.
- Inform the patients about the rehabilitation process, the preparation and use of assistive devices, reasonable expectations, and rehabilitation precautions.
- Perform postoperative assessments, such as pain intensity, edema, and range of motion; formulate personalized rehabilitation plans; and implement rehabilitation programs with the help of the therapist on the day of surgery after the patients regain consciousness.
- Give the same basic bedside rehabilitation programs to the patients in both groups.
- Elevate the affected lower limb as long as possible so that it is at an angle of 30° from the horizontal line.
- Place a cold pack on the affected knee (20 min x 3 times daily, once post rehabilitation).
- Do ankle pump exercises (5 min hourly when the patient is awake).
- Loosen patellar and the surrounding soft tissue. Have the therapist push the patella in four directions, up and down, left and right, and massage the quadriceps and hamstrings.
- Do isometric contraction training of quadriceps (10 sets x 10 repetitions daily).
- Extend and flex the knee joint.
- Perform the activities of daily living training such as dressing, getting in and out of a bed or a chair, and using the toilet under the guidance of the rehabilitation therapist.
- Give EWB training to the EG patients but ensure that CG patients are aware that weight-bearing training is prohibited for 2 weeks after surgery.
NOTE: EWB in this article refers to full weight-bearing training within 2 days after surgery.- EWB-standing training (Figure 2).
- Have a chair, a movable mirror, and an electronic body weightometer in the room. Have the patients wear the knee hinge brace. Set the brace at 0°-30°extension for 2 days after surgery.
- Instruct the patient to stand with or without a walker.
- Ask the patients to stand with their feet shoulder-width apart. Have the therapist stand on the affected side of the patients and give them verbal instructions (Figure 2A).
- Observe the body posture in a mirror and adjust the posture independently or under the guidance of the therapist (Figure 2B).
- Put the affected leg on the electronic body weightometer while the weight-bearing intensity of the affected leg gradually increases to 25%, 50%, 75%, and 100% of the body weight (Figure 2C,D).
- EWB-balance training (Figure 3).
- Stand on their tiptoes and hold for 5-10 s. Repeat 10x (Figure 3A).
- Stand on one leg with the affected lower limb for 3-5 s and repeat 10x (Figure 3B).
- Ask the patient to stand in a neutral position while pulling on the elastic band with both hands. Have the therapist and the patient pull on the elastic band in opposite directions for 3-5 s and repeat 10x (Figure 3C).
- Ask the patient to stand in a neutral position. Have the therapist move the elastic band around the back of the affected knee and forcefully pull on it. At the same time, ask the patient to try to stay still for 5-10 s; repeat this 10x (Figure 3D).
- EWB-gait training (Figure 4).
- Ask the patient to face the mirror and stand in a neutral position.
- Without moving the affected foot, ask the patient to move the healthy foot backward by one small step, then move it forward by one small step, and repeat 50x (Figure 4A).
- Without moving the healthy foot, ask the patient to move the affected foot backward by one small step, then move it forward by one small step, and repeat 50x (Figure 4B).
- Walk in a straight line for 10 m with small feet and low speed.
NOTE: If the patient can independently do a straight-leg raise without quadriceps lag, the knee hinge brace is adjusted to 0-30° for training with a slight knee bend allowed during gait.
- EWB-standing training (Figure 2).
- Discharge the patients in both groups 1-3 days after surgery. After discharge, ensure that they receive remote home rehabilitation and supervision, with rehabilitation therapists maintaining contact with the patients through messaging and telephone.
- Continue self non-weight-bearing rehabilitation programs during the home phase for the patients in CG.
NOTE: The home-based rehabilitation programs include quadriceps femoris isotonic contraction, knee flexion and extension training, lower limb non-weight-bearing transfer training, and cardiopulmonary function training. - Continue self weight-bearing rehabilitation programs during the home phase for the patients in EG but instruct them to avoid excessive weight-bearing standing and walking during home rehabilitation.
NOTE: If the pain and edema increase during self weight-bearing rehabilitation, ask the patients to stop weight-bearing immediately, rest with limb elevation and ice application, and connect with the rehabilitation therapist for remote advice.
- Continue self non-weight-bearing rehabilitation programs during the home phase for the patients in CG.
4. Outcome assessments
NOTE: The evaluations are completed by rehabilitation therapists on the 2nd, 7th, and 14th day after surgery. The primary outcome measures include wound healing, stability of knee joint, pain, and edema of the knee.
- To assess the safety and feasibility, assess and record the wound healing, anterior drawer test of the knee joint, and sudden knee flexion.
- Observe the progress of wound healing and inflammatory reaction.
NOTE: Neat and dry wound closure without exudate indicates good wound healing; otherwise, it is considered poor wound healing. - Ask the patient to lie on the bed and put the affected feet on the bed. Have the physician perform the anterior drawer test for the knee to observe the stability of the knee joint.
- Ask the patient if sudden knee flexion occurs in the affected lower limb during weight-bearing rehabilitation and record the number of sudden knee flexion.
- Observe the progress of wound healing and inflammatory reaction.
- Pain intensity
- Use the numerical rating scale (NRS)10 from 0 to 10 integers, with higher numbers indicating greater pain intensity.
- Tell patients the method of assessment of pain intensity.
- Ask them to choose an integer to represent their pain intensity.
NOTE: 0 means no pain, 10 means worst pain.
- Degree of knee edema (DKE)
- Ask the patient to lie on the bed.
- Measure 3x with a tape measure around the patella central point for knee circumference and take the average.
NOTE: The difference in circumference between the affected and unaffected sides is considered DKE. This study stipulates that a difference of 0-2 cm is mild swelling, 2-4 cm is moderate swelling, and over 4 cm is severe swelling.
- Active knee flexion range of motion (AKROM)
- Ask the patient to lie on the bed and bend the knee to the maximum angle.
- Use a goniometer to measure AKROM 3x and take the average.
NOTE: The knee joint center is the axis of rotation, the femoral shaft is the fixed arm, and the tibial shaft is the moving arm.
- Activities of daily living ability (ADL)
- Ask the patients about their activities of daily living with the Barthel Index11 scale at hospital discharge.
NOTE: The total score is 100 points. Higher scores indicate better ADL: 60 points or more indicate basic self-care ability for daily living.
- Ask the patients about their activities of daily living with the Barthel Index11 scale at hospital discharge.
Representative Results
This study included 38 patients, all of whom completed the 2-week study (CG = 19, PG = 19). There were no significant differences in sex, age, surgical site, graft type, or degree of meniscus repair between the two groups (P > 0.05; see Table 1).
The intensity of pain of patients in EG on postoperative days 2, 7, and 14 was (2.2 ± 1.3), (1.1 ± 0.6), and (0.6 ± 0.5), respectively, indicating a gradual decrease in the intensity of pain. The intensity of pain was (2.5 ± 1.2), (1.5 ± 0.8), and (0.8 ± 0.5) in CG on postoperative days 2, 7, and 14, respectively, also indicating a gradual decrease in pain. DKE in both groups gradually decreased on postoperative days 2, 7, and 14 but there were no significant differences in pain intensity or DKE between the two groups (P > 0.05; see Table 2). All patients had good knee stability during rehabilitation, with good wound healing. None had positive anterior drawer tests, knee giving way, or falls.
AKROM in EG at 2, 7, and 14 days after surgery were (70.5 ± 17.0), (83.4 ± 13.5), and (98.1 ± 13.0), respectively, indicating gradual improvement in AKROM. AKROM in CG was (56.8 ± 13.1), (74.7 ± 12.9), and (87.0 ± 10.6), respectively, also indicating gradual improvement in AKROM. The ADL in EG on postoperative days 2, 7, and 14 were (72.8 ± 8.9), (85.7 ± 5.8), and (94.2 ± 1.9), respectively, indicating that the patients' ability to perform ADL was gradually improving. The ADL in CG were (64.5 ± 9.1), (78.7 ± 6.6), and (89.7 ± 4.6), respectively, indicating the same improvement effect. There were significant differences between the two groups at different time points in AKROM and ADL scores (P < 0.05). The EG had greater flexion angles and ADL scores compared to CG at the same time points (see Table 3).
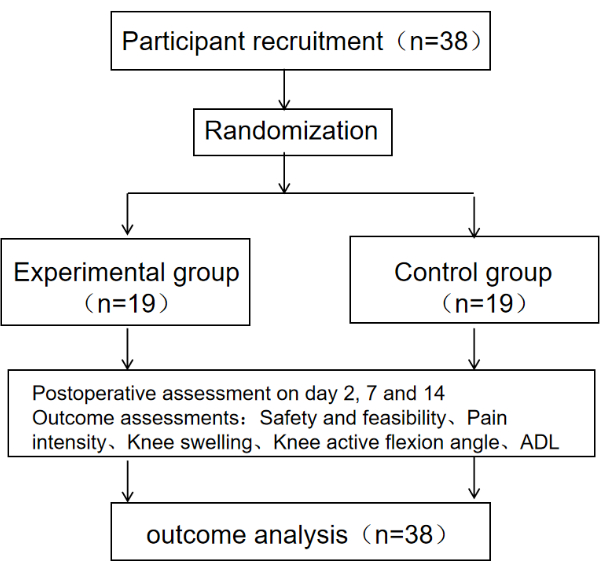
Figure 1: Schematic diagram of the protocol. The schematic diagram of the protocol includes the sample size, grouping, evaluation time, and outcome indicators of the research subjects. Please click here to view a larger version of this figure.

Figure 2: Early weight-bearing standing training. (A–D) The methods and steps of weight-bearing standing. Please click here to view a larger version of this figure.
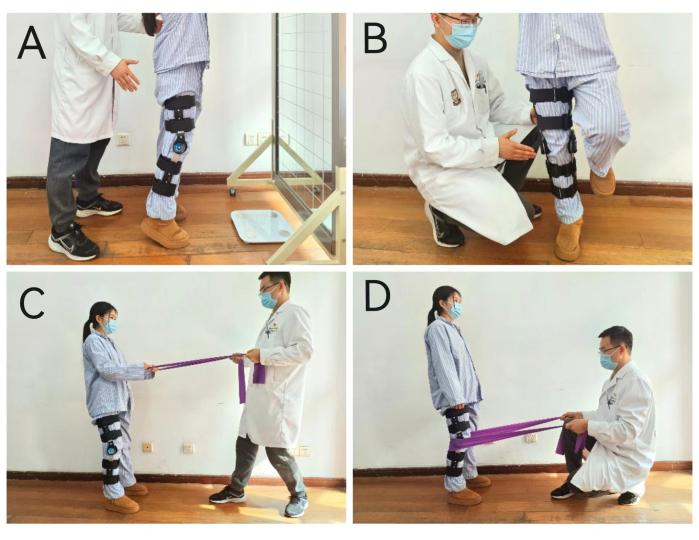
Figure 3: Early weight-bearing balance training. (A–D) Four different methods of balance training. Please click here to view a larger version of this figure.
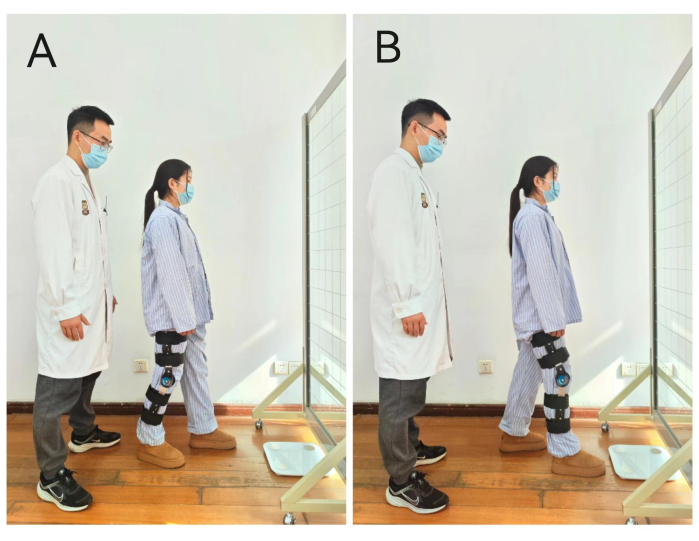
Figure 4: Early weight-bearing gait training. (A,B) Gait training methods with different foot support. Please click here to view a larger version of this figure.
| EG (n=19) | CG (n=19) | P-value | |
| Sex (M/F) | 16/3 | 14/5 | 0.426a |
| Age (years) | 29.8 ± 9.4 | 33.5 ± 7.3 | 0.224b |
| Affected limb (L/R) | 9/10 | 11/8 | 0.516a |
| Graft type (ALL/ARL) | 9/10 | 4/15 | 0.087a |
| Meniscus repair (N/M) | 11/8 | 10/9 | 0.744a |
Table 1: Basic characteristics. This table shows the sample size, gender, age, surgical site, graft type, and meniscus repair degree of the two groups. Data are presented as mean ± SD. Abbreviations: EG = Experimental group; CG = Control group; M = male; F = female; L = left; R = right; ALL =autologous ligament; ARL =artificial ligament; N = no repair; M = mild repair; Superscript a = χ2 test; "b" = t-test.
| G | NRS | DKE | ||||||||||
| Day 2 | Day 7 | Day 14 | Day 2 | Day 7 | Day 14 | |||||||
| Mil | Mod | Sev | Mil | Mod | Sev | Mil | Mod | Sev | ||||
| EG | 2.2±1.3 | 1.1±0.6 | 0.6±0.5 | 4 | 11 | 4 | 9 | 9 | 1 | 12 | 6 | 1 |
| CG | 2.5±1.2 | 1.5±0.8 | 0.8±0.5 | 3 | 10 | 6 | 8 | 10 | 1 | 15 | 3 | 1 |
| P-value | 0.850b | 0.059b | 0.198b | 0.744b | 0.946b | 0.513b | ||||||
Table 2: Pain intensity and degree of knee edema in two groups. This table records the intensity of pain and knee joint edema degree of the two groups at different time points. Data are presented as mean ± SD. Abbreviations: DKE = Degree of knee edema; EG = Experimental group; CG = Control group; Mil = Mild; Mod = Moderate; Sev = Severe; "b" = t-test.
| G | AKROM (degree) | BI | ||||
| Day 2 | Day 7 | Day 14 | Day 2 | Day 7 | Day 14 | |
| EG | 70.5±17.0 | 83.4±13.5 | 98.1±13.0 | 72.8±8.9 | 85.7±5.8 | 94.2±1.9 |
| CG | 56.8±13.1 | 74.7±12.9 | 87.0±10.6 | 64.5±9.1 | 78.7±6.6 | 89.7±4.6 |
| P-value | 0.009b | 0.049b | 0.006b | 0.008b | 0.001b | 0.001b |
Table 3: Active knee flexion range of motion and daily living ability score of two groups after surgery. This table shows the angle of active knee flexion and daily living ability scores of the two groups at different time points. Data are presented as mean ± SD. Abbreviations: AKROM = Active knee flexion range of motion; BI = Barthel index; EG = Experimental group; CG = Control group.
Discussion
This study protocol contains details of the EWB rehabilitation after ACLR. Its process is clear and not complicated, and because only simple rehabilitation equipment is needed for the implementation of the EWB rehabilitation program, it is clinically feasible and convenient. In addition, safety is an important consideration in this study protocol. The EWB rehabilitation program not only adds protective measures to prevent iatrogenic sports injury but also follows the step-by-step principle. Therefore, the results of this study show that the EWB rehabilitation program within 2 weeks after ACLR does not increase knee pain and edema and helps improve the active knee flexion angle and the ability for daily living of patients, demonstrating its safety and effectiveness.
In this study, there were no significant differences in pain intensity, knee swelling, or wound healing at 2, 7, and 14 days after surgery between EG and CG (Table 2). The pain intensity was mild in both groups, indicating that EWB after ACLR did not cause additional pain for the patients, exacerbate wound swelling, or affect wound healing. On the one hand, this may be related to postoperative analgesia measures. On the other hand, it is also related to scientific and standardized weight-bearing rehabilitation regimens. The EWB rehabilitation regimen in this study emphasizes full knee extension during weight-bearing standing and walking as much as possible within 2 weeks after surgery and allows activity within 30° of knee flexion when sensation is good. During walking, patients were required to concentrate attention, enhance overall exertion of the affected lower limb, activate the quadriceps as much as possible, improve knee stability, reduce traction and excessive stimulation on the wound caused by instability, and avoid aggravating the inflammatory response. Moreover, ACLR is a minimally invasive surgery with little trauma and good wound suturing. As patients are generally young with strong healing abilities, theoretically, EWB after surgery will not cause more trauma.
This study comprehensively assessed knee stability after ACLR through the anterior drawer test and sudden knee flexion during rehabilitation. No patients had positive anterior drawer tests or reported sudden knee flexion, suggesting that EWB rehabilitation after surgery is safe and feasible. Knee stability after ACLR is critical for graft safety. Classic previous studies show that the integrity and stability of the knee joint are maintained by the passive and active structures surrounding it. The ACL is considered the primary restraint to anterior tibial translation (ATT). Excessive ATT may place the ACL graft at risk of injury12.
Some studies13 show that partial weight bearing starts 1-2 weeks after ACLR, with full weight bearing even later. However, other studies believe that allowing immediate or even full weight bearing after ACLR does not affect knee stability and helps prevent complications14,15. Therefore, whether immediate weight-bearing rehabilitation after surgery leads to excessive anterior tibial translation, increasing graft tension and causing graft elongation, poor tendon-bone healing, and enlarged bone tunnels, has become a focus of debate. One study on healthy subjects found that in non-weight bearing conditions, knee flexion of 20° leads to increased ATT with increased quadriceps load, especially with sudden load increases, which may cause sudden rises in ACL tension16. Another important study on ACL-deficient subjects found that in 20° of knee flexion during weight-bearing, the degree of ATT was unrelated to the amount of weight borne, and ATT was minimal and significantly less than during the Lachman test and non-weight bearing17. EWB in this study emphasizes isometric contractions and weight-shifting exercises in full knee extension after surgery. One study18 also found that ATT during side-to-side and anterior-posterior weight-shifting exercises 2 weeks after ACLR did not differ from healthy controls. Although weight-shifting training started 2 weeks after surgery in that study compared to 1-2 days in this study, considering the incorporation process of autografts and allografts, graft strength is generally greatest at initial implantation19. Thus, there are reasons to believe that EWB in this study is less likely to cause excessive anterior tibial translation and graft elongation.
This study also found that EWB after ACLR increased patients’ AKROM and improved the quality of life (Table 3). The increased postoperative AKROM may be related to earlier activation of lower limb flexors and inhibition of antagonist muscle tension and spasms with EWB20. Weight-bearing activities also increased fluid flow, promoting joint fluid secretion and absorption, facilitating sliding between joint surfaces, and reducing blocking sensation during knee flexion21. The increased AKROM allows patients to choose more positions, improving convenience in daily life. Earlier out-of-bed weight-bearing rehabilitation increased patients’ activity area, enhancing recovery confidence, and reducing depression or anxiety caused by prolonged bed rest. This is also helpful in improving patients’ enthusiasm for participating in rehabilitation.
However, this study lacked a quantitative assessment of knee stability and long-term follow-up. Future studies should aim to increase sample size, lengthen follow-up duration, objectively quantify knee stability through instrumentation, and explore the effects of EWB rehabilitation on patients’ mid-to-long term knee joint stability. In summary, under ERAS guidance, EWB rehabilitation protocol after ACLR appears safe and feasible, which can help accelerate the functional recovery of patients and improve rehabilitation efficiency.
Disclosures
The authors have nothing to disclose.
Acknowledgements
This research was supported by two grants from the research project grant from Shanghai First People's Hospital (grant number: SYYG20221007) and the Medical Innovation Research Special Project in the Science and Technology Innovation Action Plan of the Shanghai Science and Technology Committee (grant number: 22Y11912100).
Materials
| Elastic band | JOINFIT | 10722038422 | |
| Electronic body weightometer | China's Xiaomi Technology (W0LONOW) | 100021480693 | |
| Movable mirror | Guangzhou Compaq Medical Equipment Co. LTD | 10073735389717 | |
| SPSS 21.0 | statistical analysis |
References
- Kehlet, H. Multimodal approach to control postoperative pathophysiology and rehabilitation. Br J Anaesth. 78 (5), 606-617 (1997).
- Zhou, M. W., Li, T. Jiji kaizhan jiasu kangfu waike gongzuo,cujin woguo guke weishouqi kangfu de fazhan[To carry out the work of accelerating rehabilitation surgery actively and promote the development of perioperative rehabilitation of orthopedics in our country]. Zhongguo kangfu yixue zazhi. 35 (7), 769-770 (2020).
- Yun, S. C., Tae, W. K., Moon, J. C., Seung, B. K., Chong, B. C. Enhanced recovery after surgery for major orthopedic surgery: a narrative review. Knee Surg Relat Res. 34 (1), 8 (2022).
- Bertrand, D., et al. 34;Consensus statement for perioperative care in lumbar spinal fusion: Enhanced Recovery After Surgery (ERAS®) Society recommendations". Spine J. 21 (5), 729-752 (2021).
- Renstrom, P. A. Eight clinical conundrums relating to anterior cruciate ligament (ACL) injury in sport:recent evidence and a personal reflection. Br J Sports Med. 47 (6), 367-372 (2013).
- Nicky, V. M., et al. Evidence-based clinical practice update: practice guidelines for anterior cruciate ligament rehabilitation based on a systematic review and multidisciplinary consensus. Br J Sports Med. 50 (24), 1506-1515 (2016).
- Kaycee, E. G., et al. Anterior cruciate ligament reconstruction recovery and rehabilitation: a systematic review. J Bone Joint Surg Am. 104 (8), 739-754 (2022).
- Fan, Z. Y., et al. Delayed versus accelerated weight-bearing rehabilitation protocol following anterior cruciate ligament reconstruction: a systematic review and meta-analysis. J Rehabil Med. 54, (2022).
- Hasan, B. S., et al. Early postoperative practices following anterior cruciate ligament reconstruction in France. Orthop Traumatol Surg Res. 107, 103065 (2021).
- Marianne, J. H., et al. Studies comparing numerical rating scales, verbal rating scales, and visual analogue scales for assessment of pain intensity in adults: a systematic literature review. J Pain Symptom Manage. 41 (6), 1073-1093 (2011).
- Collin, C., Wade, D. T., Davies, S., Horne, V. The Barthel ADL Index: a reliability study. Int Disabil Stud. 10 (2), 61-63 (1988).
- Butler, D. L., Noyes, F. R., Grood, E. S. Ligamentous restraints to anterior-posterior drawer in the human knee. A biomechanical study. J Bone Joint Surg Am. 62 (2), 259-270 (1980).
- Zhang, L., Xu, J. W., Huang, L., Tao, G., Liao, M. Quanshen zhendong jiehe yundong xunlian dui qianjiaocha rendai chongjian shuhou huanzhe zaoqi kangfu de yingxiang [Effects of whole-body vibration combined with exercise training on early rehabilitation of patients after anterior cruciate ligament reconstruction surgery]. Zhonghua wuli yixue yu kangfu zazhi. 43 (2), 158-161 (2021).
- Jonas, I., Eva, F., Sveinbjörn, B., Bengt, I. E., Jon, K. Early active extension after anterior cruciate ligament reconstruction does not result in increased laxity of the knee. Knee Surg Sports Traumatol Arthrosc. 14 (11), 1108-1115 (2006).
- Riccardo, D., Nicola, U., Fabrizio, D. F. Quadrupled semitendinosus anterior cruciate ligament reconstruction without the use of tourniquet and minimal instrumentation: the "Double D" technique. Arthrosc Tech. 12 (9), e1589-e1593 (2023).
- Schmitz, R. J., Kim, H., Shultz, S. J. Effect of axial load on anterior tibial translation when transitioning from non-weight bearing to weight bearing. Clin Biomech. 25 (1), 77-82 (2010).
- Yack, H. J., Riley, L. M., Whieldon, T. R. Anterior tibial translation during progressive loading of the ACL-deficient knee during weight-bearing and nonweight-bearing isometric exercise. J Orthop Sports Phys Ther. 20 (5), 247-253 (1994).
- Joanna, K. Tibial translation in exercises used early in rehabilitation after anterior cruciate ligament reconstruction exercises to achieve weight-bearing. Knee. 13 (6), 460-463 (2006).
- Steven, C., Peter, V., Ramses, F., Johan, B. The "ligamentization" process in anterior cruciate ligament reconstruction:what happens to the human graft? A systematic review of the literature. Am J Sports Med. 39 (11), 2476-2483 (2011).
- Gabriel, D. A., Kamen, G., Frost, G. Neural adaptations to resistive exercise: mechanisms and recommendations for training practices. Sports Med. 36 (2), 133-149 (2006).
- Jakobsen, T. L., Husted, H., Kehlet, H., Bandholm, T. Progressive strength training (10RM) commenced immediately after fast-track total knee arthroplasty:is it feasible. Disabil Rehabil. 34 (12), 1034-1040 (2012).

