A Rat Lung Transplantation Model of Warm Ischemia/Reperfusion Injury: Optimizations to Improve Outcomes
Summary
Here, we present optimizations to a rat lung transplantation model that serve to improve outcomes. We provide a size guide for cuffs based on body weight, a measurement strategy to ascertain the 4th intercostal space, and methods of wound closure and BAL (bronchoalveolar lavage) fluid and tissue collection.
Abstract
From our experience with rat lung transplantation, we have found several areas for improvement. Information in the existing literature regarding methods for choosing appropriate cuff sizes for the pulmonary vein (PV), pulmonary artery (PA), or bronchus (Br) are varied, thus making the determination of proper cuff size during rat lung transplantation an exercise of trial and error. By standardizing the cuffing technique to use the smallest effective cuff appropriate for the size of the vessel or bronchus, one can make the transplantation procedure safer, faster, and more successful. Since diameters of the PV, PA, and Br are related to the body weight of the rat, we present a strategy to choosing an appropriate size using a weight-based guide. Since lung volume is also related to body weight, we recommend that this relationship should also be considered when choosing the proper volume of air for donor lung inflation during warm ischemia as well as for the proper volume of PBS to be instilled during bronchoalveolar lavage (BAL) fluid collection. We also describe methods for 4th intercostal space dissection, wound closure, and sample collection from both the native and transplanted lobes.
Introduction
For over three decades, researchers have been modifying and improving rat lung transplantation models so that the data generated are more consistent and more reflective of the actual clinical condition. In our laboratory's time performing this model, we have determined four areas of improvement: cuffing techniques for anastomoses, identification of the recipient's 4th intercostal space, lung inflation and wound closure during the recipient's procedure, and the harvesting of samples for analysis.
Cuffing technique modifications for anastomoses can improve the entire transplantation procedure by shortening handling time of the donor lung1,2,3,4,5,6 and making the anastomosis procedure faster and technically easier for the microsurgeon. While it is critical to use the proper sized cuffs to supply the necessary blood and airflow to the transplanted lung, there is limited guidance regarding how one should choose the size of cuffs for the pulmonary vein (PV), pulmonary artery (PA), or bronchus (Br)5,7,8,9. Since the diameters of the PV, PA, and Br are related to the body weight of the donor and recipient rats, we propose that the cuff size be based on body weight. This report provides a size guide for cuffs based on a rat's body weight (180 g to over 270 g) that serves to optimize blood and air supply to the transplanted lung (Table 1).
While a newer microsurgeon can successfully and easily procure a donor lung during the donor procedure, transplanting the lung during the recipient's procedure is more complicated and is dependent on the microsurgeon's experience. Attempts to find the 4th intercostal space to access the recipient's left lung is one of the more difficult steps that holds some subjectivity and can increase the procedure time. Therefore, we introduce a simple and objective method to assist in the identification of the 4th intercostal space location by using chest measurements and the palpitations of the heart to find the correct area chest wall to dissect4,5,6,10,11,12.
We also propose an improvement to donor lung inflation, which is a potential source of injury to the organ. The donor lung is deflated until reperfusion starts. While suturing the 4th intercostal space, the donor lung is commonly inflated by increasing PEEP from 2 cmH2O to 6 cmH2O. In order to minimize lung injury from overinflation, we propose a technique where three 6-0 nylon sutures are placed around the 4th rib inferior to the 5th rib with simple double knots. When it is time for wound closure, the ends of the three sutures are held with hemostats in both hands, the wound is closed all at once by pulling up on each side, and PEEP is immediately reduced to 2 cmH2O. In this way, the lung is allowed to expand for the shortest time possible10.
At the conclusion of an experiment, the researcher often wants to collect many types of samples for many types of analysis from each transplant. For example, snap frozen tissue, formalin fixed tissue, tissue for wet-to-dry weight ratio to determine pulmonary edema, and bronchoalvelolar lavage (BAL) fluid can all be used to assess how well the transplant went. The traditional method of collecting BAL fluid allows for a mixed pooled sample from both the recipient's native lobes and the donor's transplanted lobe13,14,15. To overcome this, we present a method of clamping the hilar areas that can yield more precise insight into the transplanted and native lungs' condition. Additionally, the volume of PBS used to collect BAL fluid from each side of the lungs is important to consider because BAL fluid contains numerous soluble factors such as cytokines and chemokines that are measured by concentration. Normalizing the volume of the fluid instilled to the estimated volume of lung capacity can help with comparison. With four lobes on the right side and one lobe on the left side, each of the rat's five lobes has a different volume and surface area16. According to a previous study on volume measurement of lung lobes by Backer et al., of the total volume of the whole lung the volume of the right lobes is 63% (4400 mm3) and the left lobe is 37% (2500 mm3). Therefore, we recommend that the volume of PBS used to collect BAL fluid should be calculated as twice the tidal volume (7.2 mL/kg) multiplied by 63% for the right lung and 37% for the left lung. By using this approach, one can better control for variables like body weight and timing10,16.
In all, in this report we will demonstrate a few modifications to the standard experimental model of rat lung transplantation that can make the procedure more efficient and increase the capability of generating more accurate and plentiful data from each experiment.
Protocol
Male Sprague-Dawley rats (180-270 g body weight) were purchased commercially (e.g., Envigo) and were housed under pathogen-free conditions at The Ohio State University Animal Facility. All procedures were humanely performed according to the NIH and the National Research Council's Guide for the Humane Care and Use of Laboratory Animals and with the approval of The Ohio State University Institutional Animal Care and Use Committee (IACUC Protocol # 2012A00000135-R2).
1. Initial setup
- Set up surgical devices.
NOTE: This is a non-survival surgery. If survival surgery is to be performed, sterile instruments and barrier precautions would need to be undertaken.- Turn on the heart rate/oxygen saturation monitoring equipment and warming board to 42 °C.
- Turn on the ventilation and anesthesia machine to pre-warm the isoflurane evaporator.
NOTE: Use a tidal volume (Td) of 7.2 mL/kg, a positive-end expiratory pressure (PEEP) of 2 cmH2O, and a respiratory rate of 80 bpm. - Fill the anesthesia syringe with 10 mL of liquid isoflurane and mount the syringe onto the ventilation and anesthesia machine.
- Turn on the surgical microscope with the height and focus adjusted to the microsurgeon's preferences.
- Turn on the electrocautery device.
- Prepare and lay out surgical tools (Figure 1).
NOTE: All surgical tools were autoclaved at 121 °C for 30 min. - Collect and record body weight of donor and recipient rats.
- Use Table 1 and the rat's body weight to determine the correct gauge of angio-catheter (20, 18, 16 14, or 12 G) to use to make cuffs.
- Prepare cuffs for pulmonary artery (PA), bronchus (Br), and pulmonary vein (PV) using the size guide based on body weight (Table 1 and Figure 2).
- Place angio-catheter sized 20 G, 18 G, 16 G, 14 G, or 12 G (Figure 2A-E) on a sterile surface under the surgical microscope.
- Then use a rib-back surgical blade #11 (Figure 2F) to cut the angio-catheter at a 90° angle to form a 2 mm in length cuff body with a 1 mm X 1 mm tab (width x height) at the top of the cuff body (Figure 2G).
- Store cuffs in sterile saline until ready to use.
- Prepare solutions.
- Prepare a mixture of ketamine and xylazine in a sterile injection vial by adding 1 mL of xylazine (100 mg/mL) to 10 mL ketamine (100 mg/mL).
NOTE: The expiration date for this cocktail is determined using the earliest expiration date of the components used. - Draw into syringes the proper dosage for the rats (0.1 mL of the ketamine/xylazine mixture per 100 g of rat's body weight; e.g., for a 200 g rat, 0.2 mL of ketamine/xylazine mixture would be delivered).
NOTE: This dosage will deliver 91 mg/kg of ketamine and 9.1 mg/kg of xylazine to the rat and should keep a rat sedated for 60-80 min. - Prepare heparin which will be delivered at a dose of 1,000 U/kg.
- Store the saline, PBS, and preservation solution on ice (Table of Materials).
- Prepare a mixture of ketamine and xylazine in a sterile injection vial by adding 1 mL of xylazine (100 mg/mL) to 10 mL ketamine (100 mg/mL).
2. Donor rat preparation
- Induce anesthesia in the donor rat by intraperitoneally injecting the ketamine and xylazine mixture and waiting ~10 min for a surgical plane of anesthesia to develop that can be assessed by lack of response to toe-pinch.
- Shave the incision area using electronic clippers.
- Place the donor rat in a supine position on the surgical warming board and wipe the incision area with a sterile gauze soaked with betadine. Then wipe the area with a 70% isopropyl alcohol swab. Repeat 3 times.
- Make a 3 to 4 cm midline skin incision mid-neck using scissors and carefully dissect out subcutaneous tissues and muscles using forceps (instead of scissors to avoid bleeding).
- For endotracheal intubation, thread 4-0 silk suture around the trachea and insert a 16 G angio-catheter into the trachea. Tie the suture around the trachea tightly with a double knot, and then finish with a single knot to hold the angio-catheter in place.
- Connect the angio-catheter to the ventilator and maintain a surgical plane of anesthesia in the rat with 1-2% of isoflurane.
- Perform a laparo-sternotomy as a combined midline and transverse incision using scissors.
- Inject heparin (1,000 U/kg) with an insulin syringe via the inferior vena cava (IVC) and allow 10 min for systemic circulation.
NOTE: This administration of heparin prevents blood clots in the donor lung. - Dissect the diaphragm carefully by cutting along the thoracic arch, and then expose the thoracic cavity by following the sternum to the neck.
3. Donor lung warm ischemia and procurement
- Euthanize the donor rat by cutting the IVC.
- While lungs are still ventilating, cut both right and left auricles with micro dissecting spring scissors and gravity flush lungs with 20 mL of preservation solution in a syringe hanging at 28 cmH2O by gravity connected to tubing and an 18 G angio-catheter that is introduced directly through the pulmonary artery.
- Disconnect the ventilator from the endotracheal tube and connect it to a 5 mL syringe filled with a proper volume of air based on body weight.
NOTE: Volume of air to inflate lungs can be calculated as with twice of tidal volume (Td = 7.2 mL/kg), e.g., a 200 g rat would have a Td of 1.44 mL and multiplying it by 2 would equal 2.88 mL of air needed to inflate lungs. - Inflate donor's lungs.
- Put a Yasargil clamp on the trachea to keep lungs inflated, and cover the lungs and heart with sterile cotton gauze. Moisturize the gauze with saline, wrap the donor rat with an under pad, and leave on the warming surgery board for 1 h to induce warm ischemia in the lungs (Figure 3).
- After 1 h of warm ischemia, excise the heart-lung block with micro dissecting spring scissors and forceps and place on sterile gauze dampened with ice-cold PBS on a sterile Petri dish on ice.
NOTE: All of the following steps should occur while lungs are on the Petri dish on ice. - Carefully incise pulmonary ligaments with micro dissecting spring scissors to separate the left lung from the esophagus and the post-caval lobe.
- Carefully trim the left lung hilar area with Vannas-Tubingen spring scissor and procure the left PV, PA, and Br.
- Place cuffs on PV, PA, or Br (Figure 4A-C).
- Use a mosquito hemostat to grab the cuff tab.
- Use fine forceps to grab the distal end of the PV, PA, or Br through the appropriate cuff body, evert the extra tissue around the cuff, and secure using 8-0 nylon suture. Use Vannas-Tubingen spring scissors to trim extra tissue and the cuff around the cuff body.
- Keep the donor lung covered with gauze dampened with saline on the Petri dish on ice until it is ready to be transplanted into the recipient rat (Figure 4D).
NOTE: Average cold ischemia time is 84 min ± 11 min S.D.
4. Recipient rat preparation
- Induce anesthesia in the recipient rat in the same manner as the donor rat by intraperitoneally injecting the ketamine and xylazine mixture (0.1 mL per 100 g rat) and waiting 10 min for a surgical plane of anesthesia to develop that can be assessed by lack of response to toe-pinch.
- Shave incision area using electronic clippers.
- Place the donor rat in a supine position and wipe the incision area with a sterile gauze soaked with betadine. Then wipe the area with a 70% isopropyl alcohol swab. Repeat 3 times.
- Before the rat is secured to the ventilation machine, draw lines on the rat's chest in preparation for finding the 4th intercostal space.
- Measure the chest from the suprasternal notch to the xiphoid process and draw a line (Figure 5A).
- At the middle of this line, draw a line along the left side of the chest that measures half of the measurement from the suprasternal notch to the xiphoid process (Figure 5A and B).
- Intubate the recipient using a 16 G angio-catheter via visualization using the fiber optic cable connected to an LED light from the endotracheal intubation kit.
- Connect the angio-catheter to the ventilator and maintain a surgical plane of anesthesia with 1-2% isoflurane.
- To find the 4th intercostal space, find the area of the chest wall where a strong palpable cardiac impulse can be felt (Figure 5C, red circle).
- At this location, incise the skin with scissors and the muscle with micro dissecting spring scissors, and use the retractor to open the 4th intercostal space as widely as possible (Figure 5D and E).
NOTE: Use electrical cautery to avoid or stop bleeding during the muscle dissection. - Once the intercostal space is opened widely, carefully dissect the ligaments around the recipient's left lung using Vannas-Tubingen spring scissors and pull the lung out of chest area using sterile cotton swabs and forceps.
- Place sterile gauze around the left lung and hold it with a Dieffenbach bulldog clamp.
- Apply a Yasargil clamp on the left lung hilar area as proximally as possible.
5. Anastomoses
- Pulmonary vein (PV) anastomosis
- Place 7-0 nylon suture around the recipient's PV.
- Incise the recipient's PV using the Vannas-Tubingen spring scissors by transversely cutting the upper and lower segmental veins as distally as possible and flush out blood with 0.2 mL of heparinized saline (1 U/mL) using an insulin syringe.
- Place the donor lung still wrapped with ice-cold wet sterile gauze into the thoracic cavity.
- Insert the donor's cuffed PV into the recipient's PV, and then secure with the prepositioned 7-0 nylon suture (Figure 6).
- Bronchial (Br) anastomosis
- Place 7-0 nylon suture around the recipient's Br.
- Incise the recipient's Br by cutting the upper and lower segmental airways transversely as distally as possible with Vannas-Tubingen spring scissors.
- Insert the donor's cuffed Br into recipient's Br and secure with the prepositioned 7-0 nylon suture (Figure 6).
- Pulmonary artery (PA) anastomosis:
- Place 7-0 nylon suture around the recipient's PA.
- Incise the recipient's PA from its adventitial sheath, incise half of the vessel's circumference with Vannas-Tubingen spring scissors, and then flush out blood in the PA with 0.2 mL heparinized saline (1 U/mL) using an insulin syringe.
- Insert the donor's cuffed PA into the recipient's PA and secure with the prepositioned 7-0 nylon suture (Figure 6).
6. Reperfusion
- Remove the Yasargil clamp on the hilum to allow for reperfusion and ventilation of the transplanted donor lung (Figure 7).
- Dissect out the recipient's native left lung using micro dissecting spring scissors and forceps.
- Carefully reposition the transplanted left lung into the recipient's thorax.
- Close the thoracotomy incision by using 6-0 nylon suture.
- Place three 6-0 nylon sutures with simple double knots around the ribs superior to the 4th rib and inferior to the 5th rib (Figure 8A).
- Use hemostats to gather the three sutures together (Figure 8B).
- Increase the PEEP to 6 cmH2O in the ventilation settings.
- Tie together all three knots at the same time by pulling away to close the wound (Figure 8C).
- Decrease PEEP to 2 cmH2O immediately.
- Close skin with 6-0 nylon suture.
NOTE: Our laboratory studies the acute phase post-transplantation, so the recipient rat in this model is survived for 3 h post-transplantation under ventilation and anesthesia and then samples are collected.
7. Collection of experimental specimens (plasma, lung tissue)
- For control samples, collect the donor's right lobes after the 3 h reperfusion period is initiated.
- Snap-freeze the superior lobe and post-caval lobe for protein or RNA expression analyses, preserve the middle lobe for histology, and use the inferior lobe for wet-to-dry weight ratio (Figure 9A).
- At 10 min before the end of the 3h reperfusion time, prepare to harvest the recipient samples by injecting heparin (1,000 U/kg) with an insulin syringe into the jugular vein.
NOTE: This administration of heparin prevents blood clots in the lungs and allows for a more thorough flushing at the time of procurement. - Plasma collection
- At the end of the 3 h reperfusion period, collect 1 mL of blood with a syringe via the IVC.
- Store on ice and then centrifuge at 2,000 x g for 10 min to harvest plasma.
- Euthanize the recipient rat by cutting the IVC to allow for exsanguination.
- Dissect the diaphragm along the thoracic arch and expose the thoracic cavity by dissecting out the rib cage.
- Collect BAL fluid from the native or transplanted lungs if desired (optional).
NOTE: If wet-to-dry weight ratio or histology is being performed on the lung, BAL fluid collection should not be performed since it can affect results.- Thread 4-0 silk suture around trachea and tie a tight double knot around the trachea and intubation tube to prevent fluid leakage.
- Calculate the amount of ice-cold PBS for BAL fluid collection from the right lobes and left lobe.
NOTE: The volume ratio for the right lung is 63% while the volume ratio for the left lung is 37%16. Therefore, to determine the amount of PBS to instill into each side, the volume should be calculated as twice the tidal volume (Td = 7.2 mL/kg) multiplied by 63% for the right lung and 37% for left lung. - Place a Yasargil clamp on the left lung hilar area (Figure 10A), and, with a syringe connected to the angio-catheter, instill the calculated amount of ice-cold PBS into the right lung (recipient's native lobes) and collect the BAL fluid by pulling up gently on the syringe plunger. Perform twice.
NOTE: One should expect 70-80% recovery of instilled fluid. - Remove the Yasargil clamp on the left lung and place the clamp on the right lung hilar area (Figure 10B).
- Collect BAL fluid from transplanted left lobe in the same way as it was collected for the right lobes, and then remove the clamp on right lung hilar area.
- Cut the right and left auricles with micro dissecting spring scissors and flush lungs by gravity through the PA using an 18 G angio-catheter attached to tubing and a syringe with 20 mL of pre-chilled preservation solution hanging at 28 cmH2O.
- Collect samples from the recipient's lung.
- Snap-freeze the superior lobe and post-caval lobe for protein or RNA expression analyses, preserve the middle lobe for histology, and use the inferior lobe for wet-to-dry weight ratio) (Figure 9A).
- Divide the left transplanted left lobe into three parts: the upper region collected for snap-frozen, the middle region for histology, and the lower region for wet-to-dry weight ratio (Figure 9B).
Representative Results
In order to measure pulmonary edema, the wet-to-dry weight ratio was calculated. The donor's native lobe, the transplanted lobe, and the recipient's native lobe were collected as described in the protocol and weighed immediately for wet weight, dried at 60 °C for 48 h, and then weighed again for the dry weight. An increased wet-to-dry weight ratio would be indicative of pulmonary edema. Our results indicate that the transplanted lobe did have a significant increase in wet-to-dry weight ratio compared to the donor's or recipient's native lobe (p=0.0050, n=6/group; Figure 11).
| Angio-catheter size for cuffs | |||
| Rat Body Weight (g) | PA | Br | PV |
| 180-200 | 20 G | 18 G | 16 G |
| 200-230 | 18 G | 16 G | 14 G |
| 230-250 | 18 G | 14 G | 14 G |
| 250-270 | 18 G | 14 G | 12 – 14 G |
| Over 270 | 16 G | 14 G | 12 G |
Table 1. Size Guide for Cuffs. The size of the pulmonary artery (PA), bronchus (Br), or pulmonary vein (PV) is related to body weight. Depending on the body weight and which type of cuff you are making, the recommended angio-catheter size is given.
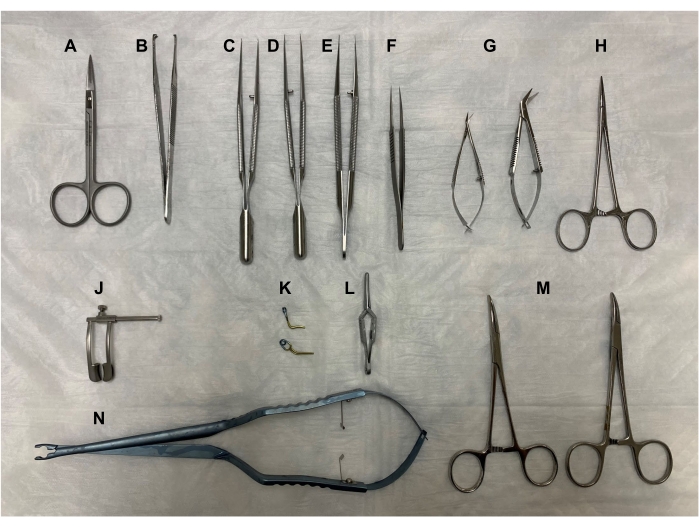
Figure 1. Surgical tools. (A) Fine scissors, (B) forceps, (C-E) microsurgical forceps, (F) Dumont #5 fine forceps, (G) Vannas-Tubingen spring scissors and Castroviejo micro dissecting scissors, (H) Halsted-mosquito hemostat, (J) retractor, (K) Yasargil clamps, (L) Dieffenbach bulldog clamp, (M) curved hemostats, and (N) Yasargil clamp applicator. All tools should be autoclaved at 121 °C for 30 min. Please click here to view a larger version of this figure.
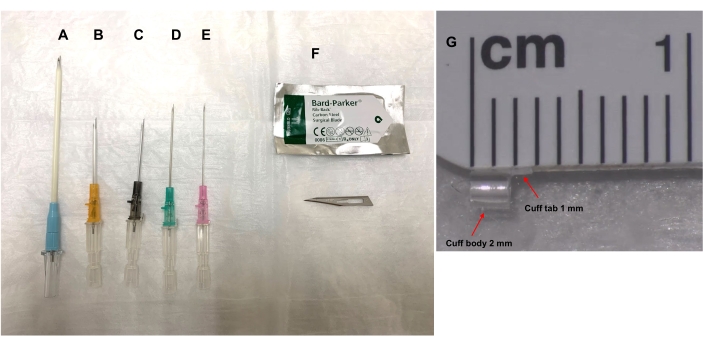
Figure 2. Cuff preparation with various sizes of angio-catheter and rib-back surgical blade #11. The size of the angio-catheter chosen for the cuff is determined by the cuff size guide (Table 1) that takes into account the rat's body weight and whether the cuff is for the pulmonary artery (PA), bronchus (Br), or pulmonary vein (PV). The angio-catheters (A) 20 G, (B) 18 G, (C) 16 G, (D) 14 G, or (E) 12 G are cut with a (F) rib-back surgical blade #11 as described in the protocol, and stored in saline until needed. (G) The cuff body length is 2 mm and a 1 mm X 1 mm tab (width x height) is left at the top of the cuff body for handling of the cuff body. Please click here to view a larger version of this figure.
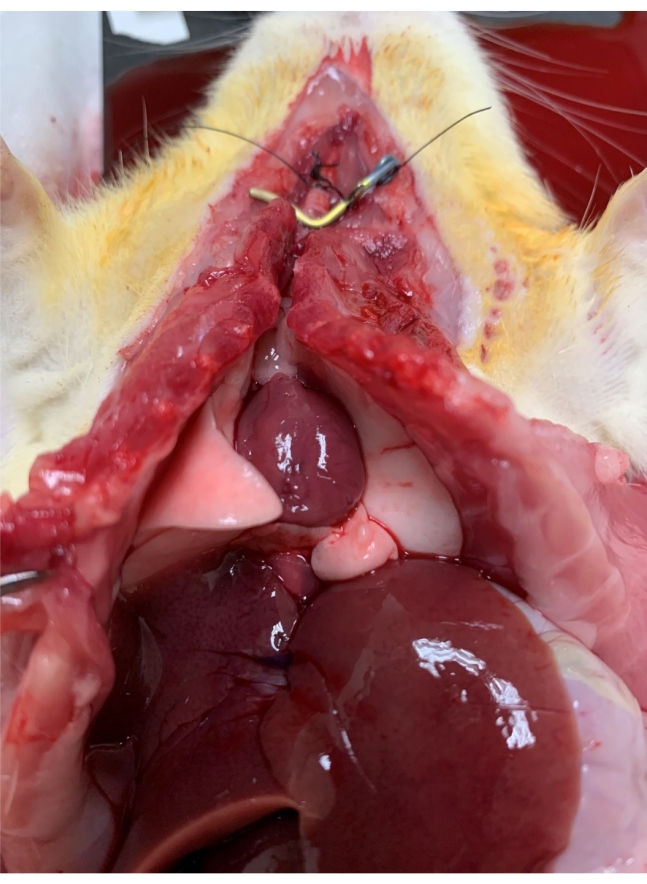
Figure 3. Warm ischemia. Lungs are flushed with the preservation solution through the pulmonary artery, inflated with twice the tidal volume of air, and then wrapped with an under pad and kept on the surgery warming board to keep the rat at normal body temperature for 1 h. Please click here to view a larger version of this figure.
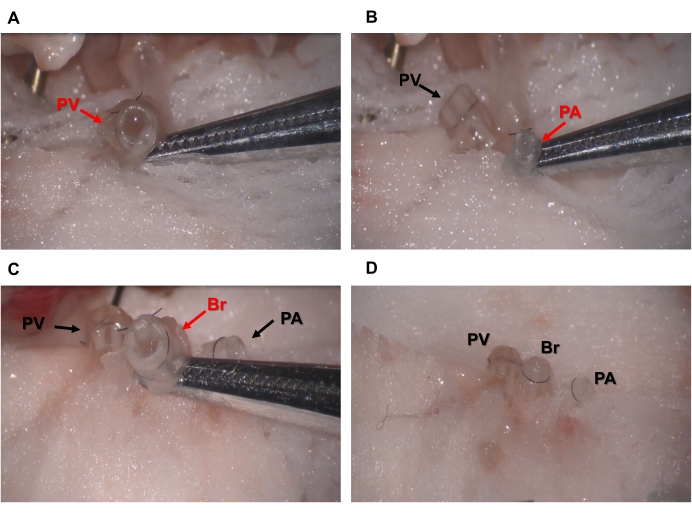
Figure 4. Cuffing of donor lung PV, PA, and Br. (A) Pulmonary vein, PV (B) pulmonary artery, PA, or (C) bronchus, Br, is inserted through a properly sized cuff, everted, secured with 8-0 nylon suture, and (D) then stored on sterile gauze dampened with ice-cold saline on a sterile Petri dish on ice. Please click here to view a larger version of this figure.
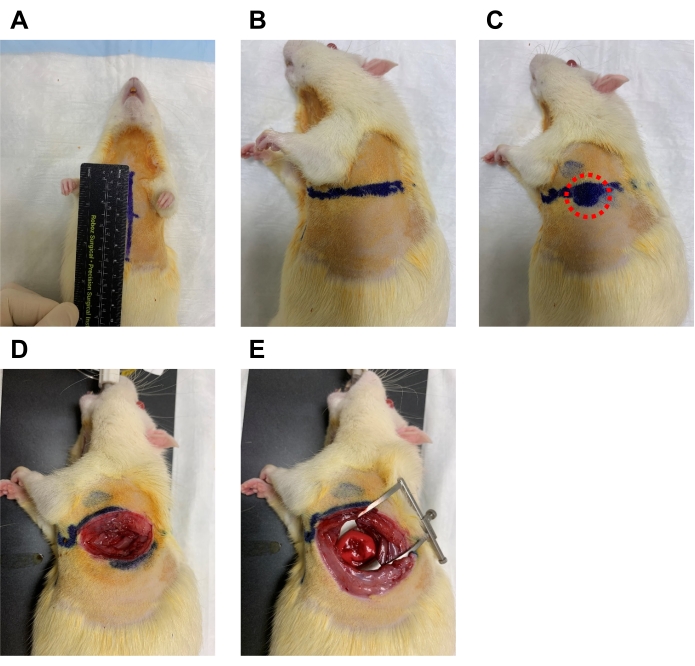
Figure 5. Measuring and dissecting at the 4th intercostal space. (A) The recipient rat is laid supine, and the chest is measured from the suprasternal notch to the xiphoid process and a line is drawn. (B) At the midpoint of this line, another line to the left side is drawn at half the length. (C) Along this line, the microsurgeon should feel for an area where the cardiac impulse is strongest to ensure the proper location of the 4th intercostal space (red circle). (D) The skin and muscle are then dissected with fine scissors. (E) The retractor is then used to open the space widely. Please click here to view a larger version of this figure.
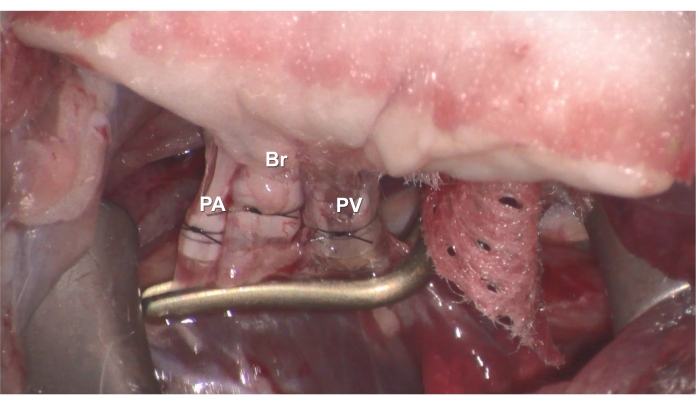
Figure 6. Anastomosis. The donor's cuffed (A) PV (B) Br, or (C) PA is inserted into the recipient's PV, Br, or PA, and then secured with 7-0 nylon suture. Please click here to view a larger version of this figure.
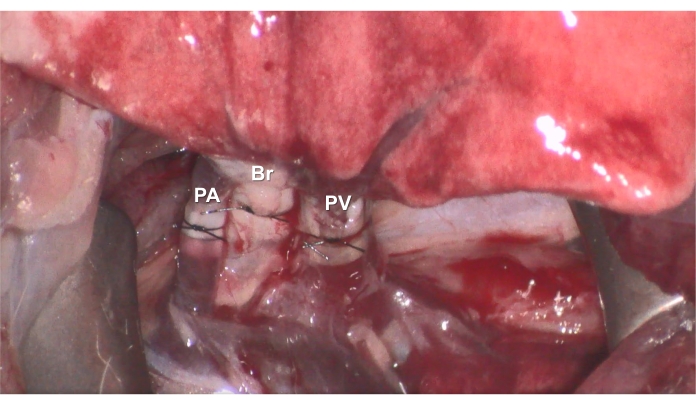
Figure 7. Reperfusion. After the anastomoses are complete, reperfusion can be started by removing the clamp, and the recipient rat is survived for 3 h under ventilation and anesthesia. Please click here to view a larger version of this figure.
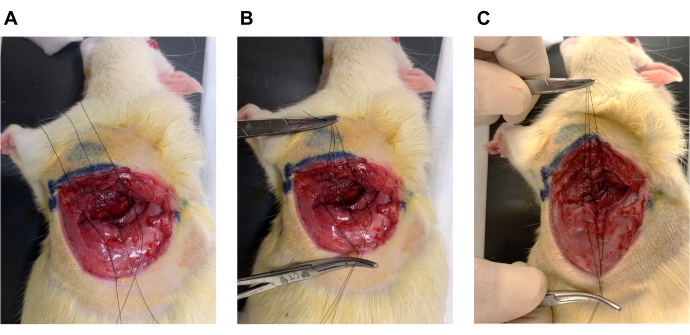
Figure 8. Wound closure. (A) Three 6-0 nylon sutures with simple double knots are placed around the ribs superior to the 4th rib and inferior to the 5th rib. (B) Use hemostats in both hands to gather the three sutures together and increase the PEEP to 6 cmH2O in the ventilation settings. (C) Tie together all three knots at the same time by pulling up and away to close the wound, decrease PEEP to 2 cmH2O immediately, and close skin with 6-0 nylon suture. Please click here to view a larger version of this figure.
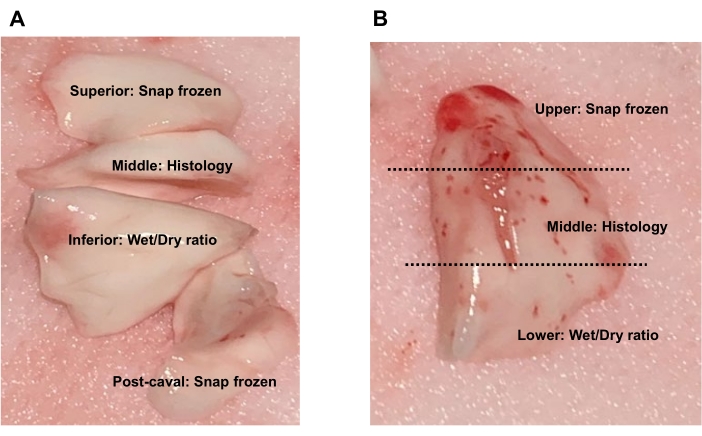
Figure 9. Lung tissue collection. (A) For the donor's or recipient's native lobes, the superior lobe and post-caval lobe can be snap frozen for protein or RNA expression analyses, the middle lobe can be preserved for histology, and the inferior lobe can be used for wet-to-dry weight ratio. (B) For the transplanted lobe, collect the upper region for snap frozen, middle region for histology, or lower region for wet-to-dry weight ratio. Please click here to view a larger version of this figure.
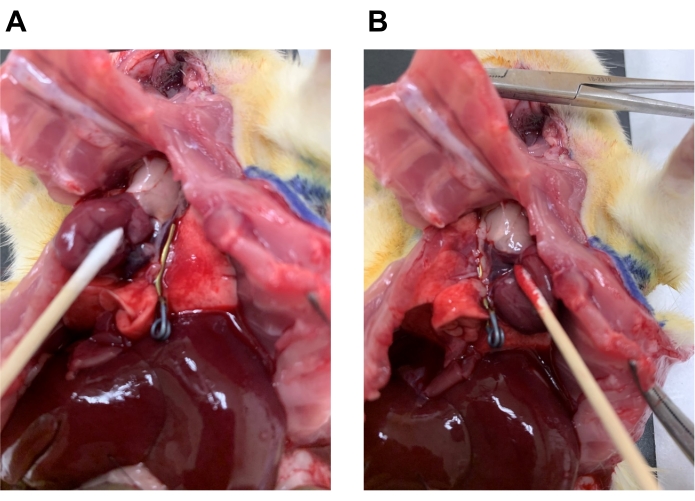
Figure 10. Application of the clamp for selective BAL fluid collection. To avoid a pooled sample, BAL fluid can be collected from either the right (native) or left (transplanted) lung. (A) The left lung hilar area can be clamped to collect BAL fluid from the right lobes. (B) The right lung hilar area can be clamped to collect BAL fluid from the left lobe. Please click here to view a larger version of this figure.
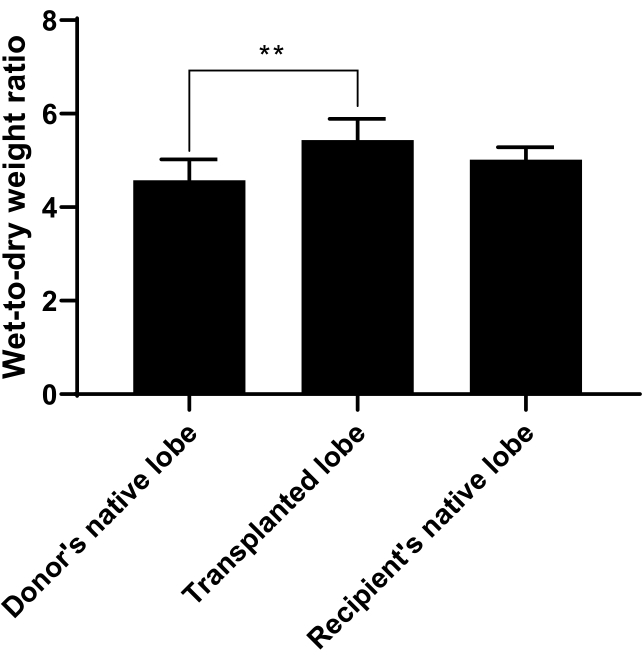
Figure 11. Wet-to-Dry Weight Ratio. Wet-to-dry weight ratio was calculated to measure pulmonary edema and can be used to indicate how well the transplant went. The donor's native lobe, the transplanted lobe, or recipient's native lobe was collected as described in the protocol and weighed immediately for wet weight, dried at 60 °C for 48 h, and then weighed again for the dry weight. A ratio of wet weight to dry weight was taken. The ratio for the transplanted lobe was significantly increased compared to the donor or recipient's native lobes. n=6 rats/group and bars represent mean ± SD. Statistical analysis was performed by using ANOVA with Tukey's post-hoc analysis. ** p<0.01. Please click here to view a larger version of this figure.
Discussion
In this report, we have intervened at several critical steps in a rat lung transplantation protocol to optimize the procedure. While various cuffing techniques for rat lung transplantation has been reported1,2,3,4,5,6,7,8,9,15, the process can still be subjective and hard for microsurgeons to apply. We have emphasized that the proper size of cuffs for PV and PA to provide blood or Br to provide air into the transplanted lung should be used, and we have provided a more objective way to determine optimal cuff size based on the rat's body weight. To more consistently induce warm ischemia of the lungs, we have given recommendations of lung inflation, clamping, and how to keep the rat warm during the 1 h warm ischemia time. During the recipient's procedure, it can be difficult to locate the 4th intercostal space. We have recommended that one can more accurately locate this position by employing a method of measurement and feeling for cardiac impulse. At the time of reperfusion, to better close the wound, we also showed a technique of handling sutures and adjusting PEEP that can more quickly close the wound and prevent overinflation and injury of the lung. Finally, we have presented strategies for tissue and BAL fluid collection that allow for a more objective harvesting of samples that can be compared across experiments and different body weights.
The most significant limitation of the described techniques is the rather steep learning curve of the transplant operation in general. The learning curve is one that can be reduced with consistent surgical practice and from reviewing troubleshooting techniques in the literature. Another limitation is that this model studies the acute phase of IRI and transplantation where biochemical changes are first occurring, which is the focus of our laboratory. Future studies should test bronchial and vascular patency at longer timelines post-transplantation.
Overall, a viable small animal transplant model is critical for evaluating therapeutic interventions for transplantation and ischemia-reperfusion injury (IRI). The rat lung transplantation model, in particular, is useful as an adjunct to studying small animal ex vivo lung perfusion (EVLP)17. It is also a more viable alternative to murine lung transplantation, because the larger anatomic size allows the researcher to obtain sufficient tissue for more in-depth analyses18. Additionally, the model is essential for determining the viability of donor lung allografts after therapeutic intervention with novel small molecule and protein therapeutics19,20,21,22 either to the donor, to the donor organ through EVLP17, or to the recipient and provides a powerful avenue to gather in vivo data.The optimizations that we describe in this report are important for microsurgeons who aim to lessen their learning curve and to remove some subjectivity. By utilizing a standardized lung cuffing size algorithm, the surgical approach can be streamlined and more objective. At the conclusion of the transplant reperfusion period, the described structured approach to BAL fluid and tissue collection also provides responsible use of animals and efficient use of the microsurgeon's time by maximizing the impact of data collected per experiment.
Declarações
The authors have nothing to disclose.
Acknowledgements
None.
Materials
| 12 Gauge angio-catheter | BD | 382277 | |
| 14 Gauge angio-catheter | B. Braun | 4251717-02 | |
| 16 Gauge angio-catheter | B. Braun | 4252586-02 | |
| 18 Gauge angio-catheter | B. Braun | 4251679-02 | |
| 20 Gauge angio-catheter | B. Braun | 4252527-02 | |
| 4-0 silk suture | Surgical Specialties Corp. | SP116 | |
| 6-0 nylon suture | AD Surgical | S-N618R13 | |
| 7-0 nylon suture | AD Surgical | S-N718SP13 | |
| 8-0 nylon suture | AD Surgical | XXS-N807T6 | |
| Betadine Spray | Avrio Health L.P | UPC 367618160039 | |
| Clippers | VWR | MSPP-023326 | |
| Castroviejo micro dissecting spring scissors | Roboz Surgical Instrument Co | RS-5668 | |
| Dumont #5 – Fine Forceps | Fine Science Tools | 11254-20 | |
| Electrocautery | Macan | MV-7A | |
| Endotracheal intubation kit | Kent Scientific | ETI-MSE | |
| Forceps | Fine Science Tools | 11027-12 | |
| Halsted-mosquito hemostat | Roboz Surgical Instrument Co | RS-7112 | |
| Heparin | Fresnius Medical Care | C504701 | |
| Insulin syringe | Life Technologies | B328446 | |
| Isoflurane | Piramal Critical Care | NDC 66794-017-25 | |
| Isopropyl Alcohol Swabs | BD | 326895 | |
| Ketamine | Hikma Pharmaceuticals PLC | NDC 0413-9505-10 | |
| Dieffenbach Bulldog Clamp | World Precision Instruments | WPI14117 | |
| Needle holder/Forceps, Curved | Micrins | MI1542 | |
| Needle holder/Forceps, Straight | Micrins | MI1540 | |
| Perfadex Plus (Organ Preservation Solution) | XVIVO Perfusion AB | REF# 19950 | |
| PhysioSuite | Kent Scientific | PS-MSTAT-RT | Used to check SpO2 and heartbeat |
| Retractor | Roboz Surgical Instrument Co | RS-6560 | |
| Saline | PP Pharmaceuticals LLC | NDC 63323-186-10 | |
| Scissors | Fine Science Tools | 14090-11 | |
| SomnoSuite Small Animal Anesthesia System | Kent Scientific | SS-MVG-Module | |
| Sterile Cotton Gauze Pad | Fisherbrand | 22-415-469 | |
| Surgical Microscope | Leica | M500-N w/ OHS | |
| Syringe 5mL | BD | 309646 | |
| Vannas-Tubingen Spring Scissors | Fine Science Tools | 15008-08 | |
| Xylazine | Korn Pharmaceuticals Corp | NDC 59399-110-20 | |
| Yasargil Clamp | Aesculap, Inc | FT351T | Used to clamp bronchus |
| Yasargil Clamp | Aesculap, Inc | FT261T | Used to clamp hilum |
| Yasargil Clamp Applicator | Aesculap, Inc | FT484T |
Referências
- Mizuta, T., Kawaguchi, A., Nakahara, K., Kawashima, Y. Simplified rat lung transplantation using a cuff technique. Journal of Thoracic and Cardiovascular Surgery. 97 (4), 578-581 (1989).
- Zhai, W., et al. Simplified rat lung transplantation by using a modified cuff technique. Journal of Investigative Surgery. 21 (1), 33-37 (2008).
- Goto, T., et al. Simplified rat lung transplantation using a new cuff technique. Annals of Thoracic Surgery. 93 (6), 2078-2080 (2012).
- Guo, H., et al. Improvements of surgical techniques in a rat model of an orthotopic single lung transplant. European Journal of Medical Research. 18, 1 (2013).
- Tian, D., Shiiya, H., Sato, M., Nakajima, J. Rat lung transplantation model: modifications of the cuff technique. Annals of Translational Medicine. 8 (6), 407 (2020).
- Rajab, T. K. Anastomotic techniques for rat lung transplantation. World Journal of Transplantation. 8 (2), 38-43 (2018).
- Reis, A., Giaid, A., Serrick, C., Shennib, H. Improved outcome of rat lung transplantation with modification of the nonsuture external cuff technique. Journal of Heart and Lung Transplantation. 14 (2), 274-279 (1995).
- Sugimoto, R., et al. Experimental orthotopic lung transplantation model in rats with cold storage. Surgery Today. 39 (7), 641-645 (2009).
- Santana Rodriguez, N., et al. Technical modifications of the orthotopic lung transplantation model in rats with brain-dead donors. Archivos de Bronconeumología. 47 (10), 488-494 (2011).
- Gielis, J. F., et al. A murine model of lung ischemia and reperfusion injury: tricks of the trade. Journal of Surgical Research. 194 (2), 659-666 (2015).
- Rajab, T. K. Techniques for lung transplantation in the rat. Experimental Lung Research. 45 (9-10), 267-274 (2019).
- Iskender, I., et al. Effects of Warm Versus Cold Ischemic Donor Lung Preservation on the Underlying Mechanisms of Injuries During Ischemia and Reperfusion. Transplantation. 102 (5), 760-768 (2018).
- Lin, X., et al. Five-year update on the mouse model of orthotopic lung transplantation: Scientific uses, tricks of the trade, and tips for success. Journal of Thoracic Disease. 4 (3), 247-258 (2012).
- Song, J. A., et al. Standardization of bronchoalveolar lavage method based on suction frequency number and lavage fraction number using rats. Toxicological Research. 26 (3), 203-208 (2010).
- Chang, J. E., Kim, H. J., Yi, E., Jheon, S., Kim, K. Reduction of ischemia-reperfusion injury in a rat lung transplantation model by low-concentration GV1001. European Journal of Cardio-Thoracic Surgery. 50 (5), 972-979 (2016).
- De Backer, J. W., et al. Study of the variability in upper and lower airway morphology in Sprague-Dawley rats using modern micro-CT scan-based segmentation techniques. Anatomical Record. 292 (5), 720-727 (2009).
- Nelson, K., et al. Method of isolated ex vivo lung perfusion in a rat model: lessons learned from developing a rat EVLP program. Journal of Visualized Experiments. (96), e52309 (2015).
- Suzuki, H., Fan, L., Wilkes, D. S. Development of obliterative bronchiolitis in a murine model of orthotopic lung transplantation. Journal of Visualized Experiments. (65), e3947 (2012).
- Jia, Y., et al. Treatment of acute lung injury by targeting MG53-mediated cell membrane repair. Nature Communications. 5, 4387 (2014).
- Kim, J. L., et al. Pegylated-Catalase Is Protective in Lung Ischemic Injury and Oxidative Stress. Annals of Thoracic Surgery. , (2020).
- Beal, E. W., et al. D-Ala(2), D-Leu(5)] Enkephalin Improves Liver Preservation During Normothermic Ex Vivo Perfusion. Journal of Surgical Research. 241 (2), 323-335 (2019).
- Akateh, C., et al. Intrahepatic Delivery of Pegylated Catalase Is Protective in a Rat Ischemia/Reperfusion Injury Model. Journal of Surgical Research. 238, 152-163 (2019).

