Fully Endoscopic Mitral Valve Repair with Percutaneous Cannulation of Groin Vessels
Summary
This protocol demonstrates in detail how to perform fully endoscopic mitral valve surgery (EMS) with percutaneous cannulation of the groin vessels, using a percutaneous plug-based vascular closure device. Fundamental steps and useful instructions are described in detail for each step.
Abstract
Endoscopic mitral valve surgery (EMS) has become a standard of care at specialized heart centers, further reducing surgical trauma compared to a traditional minimally invasive, thoracotomy-based approach. Exposure of the groin vessels for the establishment of cardiopulmonary bypass (CPB) via surgical cutdown in minimally invasive surgery (MIS) may result in wound healing disorders or seroma formation. The avoidance of surgical exposure of the groin vessels by using fully percutaneous techniques for the insertion of a CPB cannula with the implementation of vascular pre-closure devices has the potential to reduce these complications and improve clinical results. Herein, we present the utilization of a novel plug based vacsular closure device with a resobable collagen plug and the absence of suture material for closure of the arterial access for CPB in MIS. While this device was initially predominantly used in transcatheter aortic valve implantation (TAVI) procedures, with its safety and feasibility shown, we herein show that it can be used in CPB cannulation, since it is capable of closing arterial access sites up to 25 French (Fr.) in size. This device may be suitable to significantly reduce groin complications in MIS and simplify the establishment of CPB. Here, we describe the fundamental steps of EMS, including percutaneous groin cannulation and decannulation using a vascular closure device.
Introduction
The gold standard for the treatment of primary, degenerative mitral regurgitation (MR) is surgical mitral valve (MV) repair. The efficacy of this approach has been proven in large clinical studies with conclusive long-term data1. Due to a large armamentarium of surgical techniques for MV repair, such as annuloplasty or the insertion of Gore-Tex neochordae, almost all pathologies of the MV are treatable. This includes complex circumstances like Morbus Barlow with prolapse of both MV leaflets, with proven safety and efficacy as well as excellent results up to 20 years2. Furthermore, the majority of isolated MV surgery in Germany is performed via minimally invasive approaches, like a right anterolateral minithoracotomy3. Also, concomitant tricuspid valve (TV) surgery is amenable by minimally invasive access, even in a beating heart fashion4,5.
Surgical cutdown to access groin vessels has traditionally been a routine procedure for the implementation of cardiopulmonary bypass (CPB). However, this approach inherits a certain risk of postoperative wound healing disorders or seroma formation6. The adaption of transcatheter techniques for fully percutaneous insertion of a cannula for the establishment of CPB has been described7,8, and this may reduce possible groin complications. Already used devices for percutaneous vessel closure in endoscopic mitral valve surgery (EMS) include suture-based systems7,8. Recently, a collagen plug-based vascular closure device was introduced for transcatheter heart valve procedures. This large bore closure device can be used for the closure of arterial access sites of up to 25 French (Fr.). Safety and efficacy of the system have previously been demonstrated in a real-world transcatheter aortic valve implantation (TAVI) patient cohort9. The first data of minimally invasive surgery (MIS) of the MV or TV utilizing this system for the closure of the femoral artery showed promising results regarding postoperative groin complications10.
We herein describe the fundamental steps of fully endoscopic mitral valve surgery, including percutaneous groin cannulation and decannulation using a novel vascular closure device. The fully endoscopic approach differs from the MIS non-endoscopic technique in terms of a very small thoracic incision (3-5 cm), avoidance of rib-spreading, and visualization of cardiac structures with an endoscope with no direct view of the heart.
This surgery can be performed on patients with significant heart valve regurgitation or stenosis of atrioventricular heart valves, who are suitable for cardiac surgery. Preoperative diagnostics include transthoracic/transesophageal echocardiography and computed tomography of the chest and iliac vessels in elderly patients or patients with a history of peripheral artery disease.
Protocol
All herein-described procedural steps were performed in accordance with the Institutional Review Board of the University Heart and Vascular Center Hamburg guidelines and after written informed consent was obtained.
1. Fully endoscopic MIS MV repair
- Ensure the patient is under general anesthesia, in a supine position, scrubbed with iodine disinfectant, and draped with a sterile drape.
- Gain thoracic access along the peri-mammillary margin through the fourth intercostal space.
- Achieve distension of the intercostal space using a soft-tissue retractor.
2. Percutaneous cannulation of groin vessels
- Position two cannulas in the femoral artery and vein under transesophageal echocardiogram (TEE) guidance to establish CPB for MIS.
- Perform puncture of the femoral artery using a standard puncture needle and insert a 0.035 mm guidewire under TEE guidance.
- Determine the depth of the initial puncture using a puncture-locating dilator, which is inserted over the wire. This detects puncture depth by outlet backflow/the stop of backflow.
- Define the depth at skin level, which is defined by the visible stop of backflow of the measuring tool.
NOTE: For the later release of the vessel closure device, deployment depth is defined as the puncture depth at skin level plus 1 cm. - Place the arterial cannula (sizes vary according to body surface area) over the wire and connect it to CBP.
- Puncture the femoral vein medial to the artery in the same manner (step 2.2) and after insertion of the venous cannula connects to the CBP.
3. MV repair
- Insert the 3D-HD camera over the thoracic incision.
- Open the pericardium above the right site phrenic nerve using diathermy.
- Place a transthoracic Chitwood aortic clamp through a small incision for cross-clamping of the aorta under the induced ventricular fibrillation.
- Arrest the heart with antegrade Del-Nido cardioplegia and moderate hypothermia of 32 °C, which is established and maintained by the heart and lung machine. The effectiveness of cardioplegia is documented by an electrocardiogram.
- Open the left atrium with scissors and lift the left atrial roof with a dynamic retractor.
- Expose the MV and inspect the pathology, by prolapse of the posterior mitral leaflet in this case.
- Determine the size for the correct annuloplasty ring and neochordae via an annuloplasty measuring tool and a caliper for the length of native chordae.
- Resuspend the posterior mitral leaflet (PML). Implant the annuloplasty ring by implanting the neochordae at the respective papillary muscle and placing circumferential annulus sutures.
- Secure the neochordae to the papillary muscle, pass twice through the free margin of the posterior leaflet, and knot down.
- Place circumferential sutures around the annulus and then put the sutures through the annuloplasty ring, which is taken down onto the annulus via the sutures.
- Close the left atrium with a polypropylene, non-absorbable 4-0 suture; remove the aortic cross-clamp.
- Close the thoracic access and perform CBP weaning.
4. Decannulation and vascular closure
- Remove the venous cannula using a Z-suture technique at the cannula entrance site and tie down the suture after pulling out of the cannula.
- For closure of the femoral artery, use the collagen plug-based closure device.
- Clamp the arterial cannula, puncture the cannula, and insert a wire under TEE guidance.
- Retract the cannula over the wire by holding the wire in place to ensure a safe wire position in the descending aorta.
- Insert the closure system sheath fully over the wire and remove the dilator.
- Insert the closure device over the integrated insertion tool and slowly remove the whole system at a steady 45° angle under constant retraction force to the measured depth.
- Observe markings on the sheath, adjust the deployment depth, and rotate the lever for toggle release.
- Retract the system further from the femoral artery until tension appears and the indicator field appears yellow/green.
- Advance the lock advancement tool until a click is heard; the puncture is now sealed via an extravascular collagen plug.
- When hemostasis is obtained, remove the guide wire, cut the lead suture, and close the skin with a single suture.
- Apply a pressure bandage for 6 h.
NOTE: This is the end of the surgery.
Representative Results
In a preliminary patient cohort undergoing EMS and using this novel vascular closure device at our center, promising results were documented11. This cohort included 35 patients, with the most common accompanying diseases being arterial hypertension (10/35, 28.6%) and atrial fibrillation (9/35, 25.7%). Valve failure mechanisms included primary, degenerative MR (30/35, 85.7%), secondary, functional MR (3/35, 8.6%), and endocarditis (2/35, 5.7%). Concomitant procedures in MV MIS MV were tricuspid valve repair (6/35, 17.1%), ablation for atrial fibrillation (AF) (6/35, 17.1%), and left atrial appendage closure (8/35, 22.9%). For cannulation of the femoral artery, a 19 Fr. Cannula was most frequently utilized (25/35, 71.4%), followed by 21 Fr. cannula (9/35, 25.7) and a 17 Fr. cannula in one case. Isolated femoral vein cannulation was common (22/35, 62.9 %). In 13 patients, additional venous drainage was established via the jugular vein (13/35, 37.1%). With the commercial device presented in this protocol, success with immediate hemostasis was achieved in 34/35 cases (97.1%). In one patient, pull trough of the collagen plug occurred due to toggle release at the wrong height. Here, surgical cutdown was conducted and direct suturing of the femoral artery with immediate hemostasis was performed.
A 30 day follow-up presented no cases of death, stroke, myocardial infarction, or kidney injury. Permanent pacemaker implantation due to atrioventricular block was necessary in one case. A wound healing disorder occurred in one patient. Major bleeding, access site complications, or access site-related transfusion were not documented during the 30 day follow-up (see Table 1).
These results confirm that the described method of EMS is safe and effective for MV repair even in complex pathologies. The closure device is simple, easy to use, and provides immediate hemostasis, and therefore, has the potential to further simplify EMS and reduce groin wound healing disorders/seroma formation and potential durations of hospital stay.
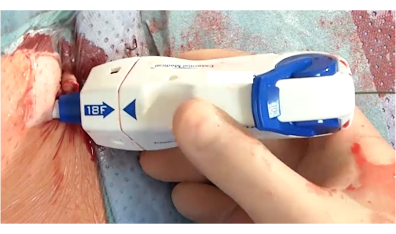
Figure 1: Collagen plug-based vascular closure device in the femoral artery. The device is fully inserted before closure of the femoral artery. The next steps include retrieval, adjustment of deployment depth, and advancing of the lock advancement tool. Please click here to view a larger version of this figure.
| Study group (n = 35) | ||
| All-cause mortality (30 days), % (n) | 0.0 (0) | |
| Stroke, % (n) | 0.0 (0) | |
| Wound healing disorder (thoracotomy), % (n) | 2.9 (1) | |
| Intensive care unit stay, days | 1.6±0.9 | |
| Hospital stay, days | 11.2±5.1 | |
| Bleeding, major/life threatening, % (n) | 0.0 (0) | |
| Access site complications, % (n) | 0.0 (0) | |
| Access site related transfusion, % (n) | 0.0 (0) | |
Table 1: Clinical outcome at 30 days after minimally invasive heart valve surgery using a collagen plug-based large bore closure device.
Discussion
The application of vascular closure devices for arterial CPB cannulation is a transcatheter technique that has the potential to improve outcomes in cardiac surgery is. Application of this technique in cardiac surgery procedures, and especially EMS valve surgery, has been adopted in specialized centers over recent years to avoid surgical cutdown and the exposure of groin vessels. ProStar and ProGlide systems are the most commonly used devices7,12. In a series of 300 patients who underwent MV MIS surgery with application of the ProStar device for arterial CPB cannulation, no postoperative bleeding complications were observed. However, in 1.6% of patients, bleeding events caused by the closure device were seen, retroperitoneal bleeding was seen in 0.6% of cases, and in 2.0% of patients, bleeding events necessitating surgical cutdown were observed. Similar results for the ProStar device have been reported by other authors7,12. For the ProGlide device, only small series of applications in EMS are documented13. The ProGlide device success rate is 92% to 95% in aortic procedures14,15.
In our first experience using this novel device, excellent results were documented, with a device success rate of 97.1%. In one patient, pull trough of the collagen plug occurred due to toggle release at the wrong height. Therefore, documentation of puncture depth is of paramount importance. When the initial puncture depth is not remembered, de novo determination of the puncture depth can be achieved after the puncture and removal of the arterial cannula. In cases of device failure, surgical cutdown can be conducted, and direct suturing of the femoral artery can be performed. In this case, manual compression of the femoral artery proximal to the puncture site is necessary for surgical cutdown. The device success rate is excellent and suggests ease of application, even when physicians are unfamiliar with the commercial system used in our protocol. Further advantages include the absence of suture material and the remaining extravascular stainless-steel lock, indicating the position of vessel entry in cases of re-interventions subsequent to later vessel complications. Although earlier studies suggest higher rates of vessel complications with this percutaneous device compared to surgical cutdown16, our series presented no postoperative vascular complications in terms of bleeding, wound healing disorders/seroma formation, or pseudoaneurysms. This is comparable to a previous study17, indicating that the described technique may simplify EMS. However, the results differ in TAVI, most likely due to application of the device in older patients with smaller and more calcified vessels18,19.
The treated patient cohort in this protocol presented with non-calcified vessels. Therefore, the results may differ in calcified vessels, as seen in TAVI procedures. Furthermore, no patient was randomized to a specific treatment, therefore hidden confounders may be apparent.
Declarações
The authors have nothing to disclose.
Acknowledgements
N.A.
Materials
| 30° camera head | Aesculap Einstein Vision | PV 632 | |
| 3D-HD camera | Aesculap Einstein Vision | PV 630 | |
| Annuloplasty ring | Edwards | 93381 | |
| Aortic clamp | Cardio Vision | CV 195.10 | |
| Aterial Cannula | Medtronic | 96570-121 | |
| Femoral Cannula | Metronic | 96670-125 | |
| Full HD 3D Monitor | Aesculap Einstein Vision | PV 646 | |
| Giude wire | Merit Medica | 6678-71 | |
| Heart valve retractor set | Cardio Vision | CV 100.00 | |
| LED light source | Aesculap Einstein Vision | OP 950 | |
| Manta | Teleflex Medical Inc. | 2115 | |
| Neo chordae | Serag Wiesner | MCL14A | |
| Soft Tissue Retractor | Cardio Vision | Cv100/80 | |
| Stative table arm for endoscopes | Cardio Vision | CV 281.73 | |
| Stative table arm for instruments | Cardio Vision | CV 281.72 | |
| Suture for fixing Loops | Gore-Tex Suture | 4N02 |
Referências
- David, T. E., Ivanov, J., Armstrong, S., Rakowski, H. Late outcomes of mitral valve repair for floppy valves: Implications for asymptomatic patients. The Journal of Thoracic and Cardiovascular Surgery. 125 (5), 1143-1152 (2003).
- David, T. E., David, C. M., Lafreniere-Roula, M., Manlhiot, C. Long-term outcomes of chordal replacement with expanded polytetrafluoroethylene sutures to repair mitral leaflet prolapse. The Journal of Thoracic and Cardiovascular Surgery. 160 (2), 385-394 (2020).
- Beckmann, A., Meyer, R., Lewandowski, J., Markewitz, A., Harringer, W. German heart surgery report 2018: the annual updated registry of the German Society for Thoracic and Cardiovascular Surgery. The Thoracic and Cardiovascular Surgeon. 67 (5), 331-344 (2019).
- Abdelbar, A., et al. Endoscopic tricuspid valve surgery is a safe and effective option. Innovations. 15 (1), 66-73 (2020).
- Pfannmueller, B., Misfeld, M., Davierwala, P., Weiss, S., Borger, M. A. Concomitant tricuspid valve repair during minimally invasive mitral valve repair. The Thoracic and Cardiovascular Surgeon. 68 (6), 486-491 (2020).
- Ko, K., et al. Minimally invasive mitral valve surgery: a systematic safety analysis. Open Heart. 7 (2), e001393 (2020).
- Pozzi, M., et al. Total percutaneous femoral vessels cannulation for minimally invasive mitral valve surgery. Annals of Cardiothoracic Surgery. 2 (6), 739-743 (2013).
- Kim, J., Yoo, J. S. Totally endoscopic mitral valve repair using a three-dimensional endoscope system: initial clinical experience in Korea. Journal of Thoracic Disease. 12 (3), 705-711 (2020).
- Kroon, H. G., et al. Dedicated plug based closure for large bore access-The MARVEL prospective registry. Catheterization and Cardiovascular Interventions. 97 (6), 1270-1278 (2021).
- Van Praet, K. M., et al. The MANTA vascular closure device for percutaneous femoral vessel cannulation in minimally invasive surgical mitral valve repair. Innovations. 15 (6), 568-571 (2020).
- Otto, C. M., et al. ACC/AHA guideline for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Journal of the American College of Cardiology. 77 (4), 450-500 (2020).
- Vergnat, M., Finet, G., Rioufol, G., Obadia, J. F. Percutaneous femoral artery access with Prostar device for innovative mitral and aortic interventions. European Journal of Cardiothoracic Surgery. 39 (4), 600-602 (2011).
- Ramponi, F., Yan, T. D., Vallely, M. P., Wilson, M. K. Total percutaneous cardiopulmonary bypass with Perclose ProGlide. Interactive Cardiovascular and Thoracic Surgery. 13 (1), 86-88 (2011).
- Sahin, A. A., et al. Comparison between PeRcutanEous and surgical femoral aCcess for endovascuLar aOrtic repair in patientS with typE III aortic Dissection (PRECLOSE Trial). Vascular. 29 (4), 616-623 (2020).
- Malkawi, A. H., Hinchliffe, R. J., Holt, P. J., Loftus, I. M., Thompson, M. M. Percutaneous access for endovascular aneurysm repair: a systematic review. European Journal of Vascular and Endovascular Surgery. 39 (6), 676-682 (2010).
- Kastengren, M., et al. Percutaneous vascular closure device in minimally invasive mitral valve surgery. The Annals of Thoracic Surgery. 110 (1), 85-91 (2020).
- Ahmad, A. E., et al. First experiences with MANTA vascular closure device in minimally invasive valve surgery. The Thoracic and Cardiovascular Surgeon. 69 (5), 455-460 (2021).
- Wood, D. A., et al. Pivotal clinical study to evaluate the safety and effectiveness of the MANTA percutaneous vascular closure device. Circulation. Cardiovascular Interventions. 12 (7), e007258 (2019).
- De Palma, R., Settergren, M., Rück, A., Linder, R., Saleh, N. Impact of percutaneous femoral arteriotomy closure using the MANTATM device on vascular and bleeding complications after transcatheter aortic valve replacement. Catheterization and Cardiovascular Interventions. 92 (5), 954-961 (2018).

