Application of Mid-Pancreatectomy with End-to-End Anastomosis in Pancreatic Benign Tumors
Summary
The present protocol describes the application of mid-pancreatectomy combined with end-to-end anastomosis in the surgical treatment of pancreatic benign tumors, which presents a feasible solution for managing such tumors while concurrently preserving pancreatic function.
Abstract
Mid-pancreatectomy combined with end-to-end anastomosis is a surgical procedure used to treat benign pancreatic tumors. It involves removing the tumor from the middle section of the pancreas and connecting the proximal and distal ends through an anastomosis. The traditional surgical approach for resecting the middle segment of the pancreas involves closing the proximal pancreas and creating a Roux-en-Y anastomosis with the jejunum. However, this approach carries a double risk of pancreatic stump fistula and pancreatico enteric anastomotic leak postoperatively. In this paper, a new procedure is described where stent tubes were placed into the proximal and distal sides of the pancreatic ducts after ensuring sufficient freedom from the proximal distal pancreas. The pancreatic parenchyma was then sutured continuously under direct vision to achieve pancreatic end-to-end anastomosis. This procedure helps preserve pancreatic function, reducing the risk of postoperative pancreatic insufficiency. However, due to the complexity and risks involved, thorough evaluation and preparation are necessary before surgery. We carefully assess the patient’s history, serology, and imaging results to determine the feasibility and effectiveness of the procedure. During surgery, we consider the use of a suitable pancreatic duct stent to ensure the flow of pancreatic juice into the intestine through physiological pathways. Our goal is to remove the tumor while preserving as much normal pancreatic tissue as possible for the anastomosis. After the operation, it is crucial to monitor the patient’s pancreatic function, paying close attention to blood glucose levels, drainage fluid volume, and amylase value of the pancreatic anastomosis. During the postoperative follow-up visit, the patient’s pancreatic function was assessed, and there was no significant change in quality of life compared to before the surgery. This indicates that mid-pancreatectomy combined with end-to-end anastomosis is a safe and effective procedure for treating pancreatic benign neoplasms.
Introduction
From a clinical perspective, it is important to note that not all tumors that develop in the pancreas are classified as pancreatic cancers. Pancreatic tumors can be broadly categorized into two main groups: benign tumors of the pancreas and pancreatic malignancies. Benign neoplasms of the pancreas encompass cystadenoma, intraductal papillary mucinous neoplasm, pancreatic hemangioma, and others1. The detection rate of benign pancreatic tumors has been consistently increasing over the years, and surgery remains the most effective treatment option2. However, traditional surgical procedures such as pancreatoduodenectomy or body and tail resection of the pancreas, while ensuring complete tumor removal, often result in the removal of excessive normal pancreatic tissue. This can significantly impact the long-term quality of life for patients, particularly leading to a higher incidence of endocrine and exocrine dysfunction3,4.
In recent years, the field of laparoscopic pancreatic surgery has seen significant advancements due to the rapid development of minimally invasive techniques like laparoscopic surgery and robotic surgery5. This has led to an increase in the number of hospitals performing laparoscopic pancreatic surgery, which has yielded positive outcomes. Among the various surgical methods, laparoscopic mid-pancreatectomy is considered to be the most suitable approach for treating benign or low-grade malignant tumors located in the neck or proximal part of the pancreas6.
The first mid-pancreatectomy was performed in 2003 by the Baca team on a patient with pancreatic cystadenoma7, and since then, this procedure has been adopted worldwide. Compared to other techniques like local enucleation of pancreatic tumor, laparoscopic caudal pancreatectomy, and laparoscopic pancreaticoduodenectomy, mid-pancreatectomy offers the advantage of preserving normal pancreatic parenchyma and reducing the risk of insufficient internal and external pancreatic secretion4,6,8. However, a challenge arises after resecting the middle part of the pancreas, as traditionally, the broken ends of the pancreas were believed to be unable to be anastomosed. To reconstruct the digestive tract, two main methods are employed. The first method involves a single anastomosis, where the distal end of the pancreas is anastomosed with the stomach or jejunum after closing the proximal end. The second method is a double anastomosis, where both the proximal and distal ends of the pancreas are anastomosed with the jejunum in the shape of a Ω. However, these reconstruction techniques pose the risk of pancreatic stump fistula and pancreatic-enterostomy fistula for patients, which can lead to abdominal infection and abdominal bleeding. Overcoming these challenges remains a significant concern for pancreatic surgeons8,9.
This paper proposes a novel treatment method called laparoscopic mid-pancreatectomy combined with end-to-end anastomosis. The method involves removing the tumor in the middle part of the pancreas and placing stent tubes into the pancreatic duct at both ends of the pancreas. The pancreatic tissue is then continuously sutured to reconstruct the pancreas. The primary objective of this method is to preserve the substance and function of the pancreas while removing the tumor, thereby reducing the risk of postoperative pancreatic fistula, secondary infection, and bleeding10,11. Additionally, it aims to improve surgical safety.
The patient, a 57-year-old male, was admitted to the hospital due to the discovery of a pancreatic mass during a CT scan. The mass was a round cystic structure with low density, measuring approximately 28 mm x 40 mm, and had an unclear boundary. The patient had a history of type II diabetes for 3 years and hepatitis B virus infection for over 10 years. Before the operation, the levels of alpha-fetoprotein (AFP) and carcinoembryonic antigen (CEA) were measured to be 30.53 ng/mL and 5.8 ng/mL, respectively. Laparoscopic mid-pancreatectomy combined with end-to-end anastomosis was performed on June 15, 2022. The postoperative pathology report indicated the presence of a solid cystic mass in the pancreatic tissue, measuring 3.8 cm x 2.5 cm x 2 cm. The mass appeared gray and white, and the cyst contained transparent fluid with a clear boundary (see Figure 1). Postoperative pathology confirmed pancreatic hemangioma. Tumor markers and drainage tube amylase levels showed a decreasing trend after the surgery, and the patient had a successful recovery.
Protocol
The operation is routine and has received ethics approval. This study was permitted by the Ethics Committee of the Six Affiliated Hospital of Sun Yat-sen University. Meanwhile, the informed written consent was obtained from the patient. Its research contents and methods meet the medical ethics norms and requirements.
1. Patient selection
- Use the following inclusion criteria: benign pancreatic tumors, including hemangioma, benign neuroendocrine tumor, serous or mucinous cystadenoma, solid pseudopapilloma, and non-invasive intraductal myxoma.
- Use the following exclusion criteria: pancreatic malignant tumors, atrophy of the tail of the pancreatic body, diffuse inflammation of the pancreas, and vascular variation.
2. Preoperative preparation, operative position, and anesthesia
- Ask the patient to consume a low in fat, salt, and sugar diet 1 day before the surgical operation and then abstain from eating food and drinking water at least 8 h prior to the surgery.
- Place the patient in a supine position with the head elevated and slightly tilted to the left. The surgery was performed using a dual primary knife mode.
NOTE: In the dual primary knife mode, two skilled and experienced surgeons alternate between the roles of surgeon and assistant as needed, aiming to improve efficiency and quality. - Perform endotracheal intubation and give general anesthesia. Judge the anesthetic effect according to the patient's post-anesthesia and intraoperative conditions, such as complete anesthesia block, no additional drugs during operation, and stable vital signs.
3. Surgical technique
- Make a vertical incision 2 cm above the right side of the navel and establish pneumoperitoneum with a Veress needle. Insert a 12 mm trocar and introduce the laparoscope after establishing pneumoperitoneum.
- Place five trocars in the following positions: a 12 mm trocar in the supraumbilical region for observation, a 5 mm trocar in the right anterior axillary line, a 12 mm trocar under the costal margin of the right midclavicular line, a 5 mm trocar horizontally 2 cm below the xiphoid process, and a 12 mm trocar horizontally 2 cm at the supraumbilical level (see Figure 2).
- Explorate carefully the intraperitoneal organs and peritoneal surface to reveal a mass above the pancreas, protruding from the surface of the pancreas and measuring approximately 3cm x 3 cm.
- Use an ultrasonic knife to separate abdominal adhesions and excise a portion of omental tissue.
- Use an ultrasonic knife to free the greater curvature side tissues of the gastroepiploic artery, suspend the greater curvature of the stomach using clamps (see Table of Materials), and expose the pancreas.
- Following intraoperative B-ultrasound localization, use an ultrasonic scalpel to cut off 1 cm of normal pancreatic tissue from the edge of the pancreatic mass near the neck of the pancreas.
- Use an ultrasonic knife to free the splenic artery and vein at the upper posterior of the pancreas. Then, free the connective tissue between the tail and body of the pancreas and the splenic vessels (see Figure 3).
- Resect completely the pancreatic mass using an ultrasonic scalpel and remove the normal pancreatic tissue 1 cm proximal to the margin of the pancreatic mass.
- Place the stent tubes into the proximal and distal sides of the pancreas within the pancreatic ducts (see Figure 4).
NOTE: The diameter and length of the stent tubes in the pancreatic duct were 2 mm and 6 cm, respectively. (see Table of Materials). - Suture the pancreatic tissue continuously using 4-0 priline (see Figure 5; see Table of Materials) and make an extended incision 2 cm below the navel to remove the pancreatic mass.
- Rinse the abdominal cavity with saline to check for any bleeding points and place a drain above and below the pancreatic anastomosis, respectively. Finally, suture the incision (see Figure 2), and the operation is concluded.
4. Postoperative nursing and monitoring
- Perform ECG monitoring and low-flow oxygen after the operation.
- Give the patient a semi-liquid diet and instruct the patient to turn over and exercise in bed on the 1st day after the operation.
- Provide hepatoprotective, anti-inflammatory, hemostatic, analgesic, albumin, and acid suppression treatment.
- Monitor amylase changes in the drainage tube at the 1st, 3rd, 4th, and 5th day after operation.
Representative Results
The operation was completed within 1.5 h, and there was a minimal intraoperative bleeding volume of 50 mL, without the need for a blood transfusion. The dissociation of splenic arteriovenous during the surgery was sufficient to provide effective protection for preserving the pancreatic tail and spleen. The gap left after central pancreatectomy is 1.7 mm. There were no short-term complications, and the patient's postoperative recovery was successful. The duration of the hospital stay was 20 days, and the postoperative hospital stay was 10 days. The drain amylase levels decreased from 29300 U/L on postoperative day 1 to 58.39 U/L on postoperative day 5. Venous blood was collected from the patient. The level of CEA in blood decreased from 5.8 ng/mL preoperatively to 2.28 ng/mL postoperatively. Additionally, the level of AFP decreased from 30.53 ng/mL preoperatively to 7.66 ng/mL postoperatively (see Table 1). Preoperative images and postoperative images can be seen in Figure 6.
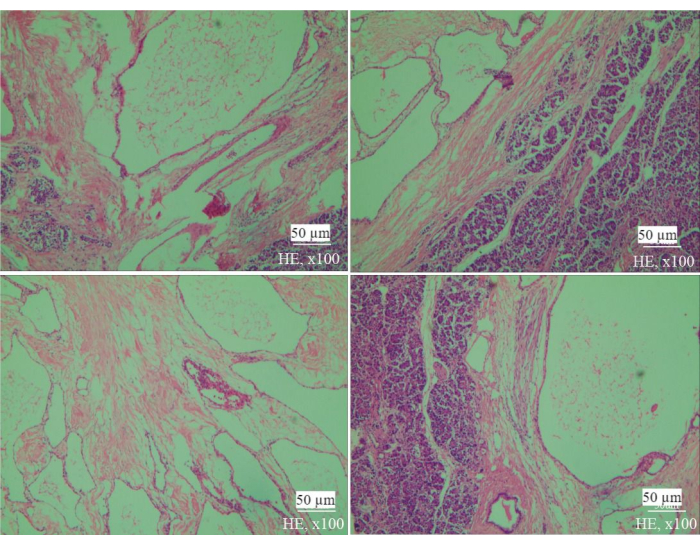
Figure 1: Tumor pathology. The results are from HE staining at 100x. Please click here to view a larger version of this figure.
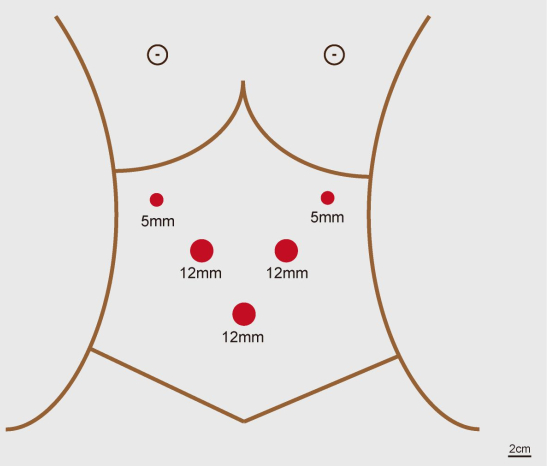
Figure 2: The layout of trocars. In total, there were 5 trocars, including 1 observation hole and 4 operation holes. Please click here to view a larger version of this figure.
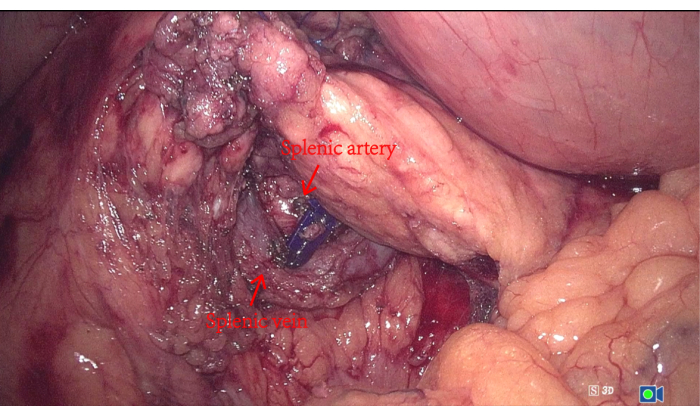
Figure 3: Free splenic artery and splenic vein. To free the splenic artery and vein at the upper posterior of the pancreas. Please click here to view a larger version of this figure.
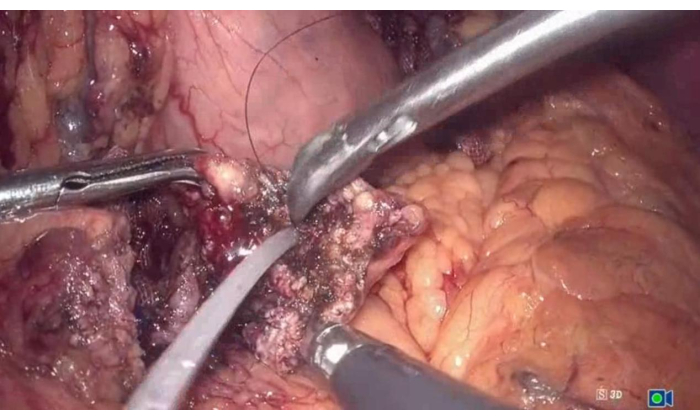
Figure 4: Placement of the pancreatic duct stent. Place the stent tubes into the proximal and distal sides of the pancreas within the pancreatic ducts. Please click here to view a larger version of this figure.
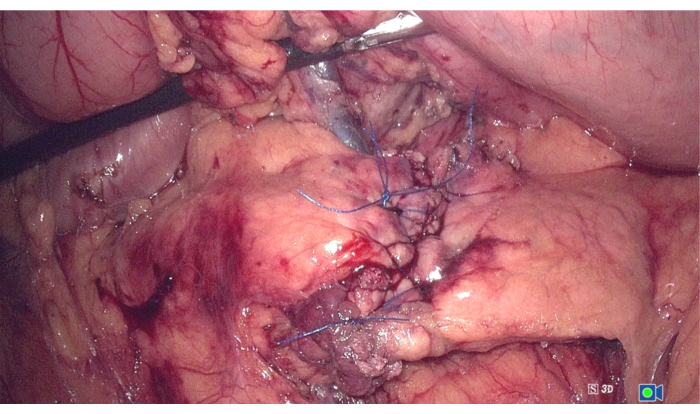
Figure 5: Pancreatic end-to-end anastomosis. Suture the pancreatic tissue continuously using 4-0 priline for end-to-end anastomosis. Please click here to view a larger version of this figure.
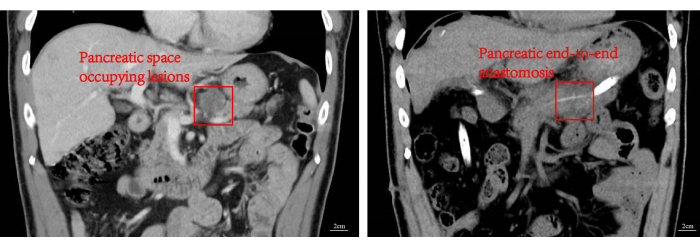
Figure 6: Preoperative images and postoperative images. Preoperative and postoperative CT coronal view imaging. Please click here to view a larger version of this figure.
| Items | Results |
| Operation time (min) | 90 |
| Intraoperative bleeding volume (mL) | 50 |
| Blood transfusion volume (mL) | 0 |
| Gap left after operation (mm) | 1.7 |
| Postoperative complication | None |
| Duration of hospital stay (day) | 20 |
| Postoperative hospital stay (day) | 10 |
| Drain amylase levels on POD1 (U/L) | 29300 |
| Drain amylase levels on POD5 (U/L) | 58.39 |
| Level of CEA preoperatively (ng/mL) | 5.8 |
| Level of CEA postoperatively (ng/mL) | 2.28 |
| Level of AFP preoperatively (ng/mL) | 30.53 |
| Level of AFP postoperatively (ng/mL) | 7.66 |
Table 1: Relevant outcomes of the patient. Abbreviations: POD = postoperative day; CEA = carcinoembryonic antigen; AFP = alpha-fetoprotein.
Discussion
The pancreas, an important digestive organ in the human body, has several important secretory functions. Therefore, in pancreatic surgery, attention needs to be paid to the preservation of pancreatic parenchyma and its function. With the rising detection rate of benign pancreatic tumors and low-grade malignancies, various procedures have been developed to preserve function, including local enucleation of the pancreas, mid-pancreatectomy, and pancreatic head resection with preservation of the duodenum12,13. Compared to previous pancreatoduodenectomy or the body and tail of the pancreas, these function-preserving pancreatic surgeries aim to ensure radical tumor resection while minimizing the removal of normal pancreatic tissue. However, it is important to note that these procedures may increase the risk of postoperative pancreatic fistula due to potential leakage from the pancreatic stump12,13,14.
The mid-pancreatectomy described in this case was first reported by Ehrhardt in 190814. In a patient with gastric cancer complicated by a pancreatic tumor, gastrectomy and segmental pancreatectomy were performed, and the two pancreatic stumps were directly anastomosed. The healing process occurred naturally through drainage. Mid-pancreatectomy, as a surgical procedure to preserve pancreatic parenchyma and function, reduces the risk of postoperative pancreatic exocrine and endocrine insufficiency and has been adopted to treat benign or low-grade tumors in the neck and proximal body of the pancreas. However, there is evidence suggesting that patients who underwent mid-pancreatectomy were associated with a higher risk of pancreatic fistula because the tumors of these patients were mostly benign or borderline, and the pancreatic parenchyma is soft15. Therefore, proper management of the pancreatic stump is crucial to prevent postoperative pancreatic fistula. The key point of mid-pancreatectomy is the treatment of the pancreatic stump and the selection of a suitable digestive tract to rebuild. One approach is to use an anastomotic technique. Traditionally, after a mid-pancreatic resection, it was believed that an anastomosis between the ends of the pancreas was not possible. As a result, the classic surgical approach involved closing the proximal pancreas and creating a Roux-en-Y anastomosis between the distal pancreas and the jejunum. However, this approach carries the risk of both pancreatic stump fistula and pancreatico-enteric anastomotic leakage. Additionally, intraperitoneal infection and hemorrhage secondary to pancreatic fistula pose significant challenges for pancreatic surgeons. It has been reported that Sun et al., using endo-stent drainage of the pancreatico jejunal bridge after mid-pancreatic resection by silicon tube drainage of the secretions from the pancreas into the jejunum, confirmed that this method could lower the rate of pancreatic fistula than conventional pancreatico jejunostomy or pancreatico gastric anastomosis16. In this paper, we challenge the traditional view by proposing the use of a supporting duct of the pancreatic duct followed by an end-to-end anastomosis after mid-pancreatic resection. This prevents the anastomosis of the pancreas with the digestive tract, ensuring that the pancreatic juice does not come into contact with the digestive fluid and remains inactive. As a result, the risk of pancreatic fistula bleeding is reduced to some extent. After the surgery, it is important to maintain the patency of the drainage tube and provide symptomatic support treatment, such as enzyme inhibition and nutrition. Although pancreatic fistula may still occur, the risk of bleeding and infection is greatly reduced due to the inactivation of pancreatic juice by digestive fluids.
To sum up, the placement of a pancreatic duct stent after a mid-pancreatic resection for end-to-end anastomotic reconstruction is feasible for a benign neoplasm of the pancreas. In this case, the patient had a successful recovery. The critical steps of the protocol involve performing rigorous surgical dissection and excision to ensure maximum preservation of healthy pancreatic tissue. It is crucial to have precise surgical skills and experience to achieve end-to-end anastomosis using the placement of a pancreatic duct stent. In addition, close monitoring and management are essential after the surgery, along with timely intervention if needed, to minimize the risk of complications. Our technique is based on existing mid-pancreatectomy but with some significant modifications, including the placement of a pancreatic duct stent for end-to-end anastomosis, to improve pancreatic function preservation and reduce the risk of complications. This procedure not only helps preserve pancreatic function but also avoids injury to other organs and eliminates the need for devascularization during digestive tract reconstruction. It significantly enhances the safety of the procedure, accelerates patient recovery, reduces complications, and shortens hospital stay. However, there are some limitations to the protocol since our study involved only one case, and pancreatic end-to-end anastomosis is not widely available; further evidence is needed to establish the advantages of combining middle pancreatic resection with end-to-end anastomosis.
Disclosures
The authors have nothing to disclose.
Acknowledgements
This work was supported by grants from the Project of Guangdong clinical medical research center of digestive diseases (2020B1111170004), National Key Clinical Discipline and the program of Guangdong Provincial Clinical Research Center for Digestive Diseases.
Materials
| abdominal instrument button | Johnson & Johnson | ||
| abdominal instrument cap | Johnson & Johnson | ||
| abdominal instrument collar | Johnson & Johnson | ||
| abdominal instrument connector | Johnson & Johnson | ||
| Absorbable ligature clip | Sichuan Guona Technology Co., LTD | 230716 | |
| barbs | Johnson & Johnson | ||
| blade | Johnson & Johnson | ||
| blood pad | Johnson & Johnson | ||
| Cloth towel forceps | Johnson & Johnson | ||
| disposable drainage tube | Johnson & Johnson | 412280 | 6 cm x 2 mm |
| Electric knife head | Johnson & Johnson | ||
| forceps | Johnson & Johnson | ||
| hilt | Johnson & Johnson | ||
| holding flask | Johnson & Johnson | ||
| intestinal forceps | Johnson & Johnson | ||
| laparoscope | Johnson & Johnson | ||
| laparoscopic instruments | Johnson & Johnson | ||
| Ligating clip | Teleflex Medical | 73H2300118 | |
| long curved forceps | Johnson & Johnson | ||
| medium curved forceps | Johnson & Johnson | ||
| Nail clamp | Ethicon,USA | 584C82 | |
| needle holders | Johnson & Johnson | ||
| ovoid forceps | Johnson & Johnson | ||
| Paraffin oil | Johnson & Johnson | ||
| purse string forceps | Johnson & Johnson | ||
| right angled forceps | Johnson & Johnson | ||
| right angled forceps | Johnson & Johnson | ||
| scissors | Johnson & Johnson | ||
| Siphonhead | Johnson & Johnson | ||
| Small cup | Johnson & Johnson | ||
| small curved forceps | Johnson & Johnson | ||
| Sonotome keyhole | Johnson & Johnson | ||
| steel ruler | Johnson & Johnson | ||
| Straight forceps | Johnson & Johnson | ||
| Suction needle plate | Johnson & Johnson | ||
| Suture needle | Johnson & Johnson | Vcp397H | |
| Syringe | Johnson & Johnson | ||
| syringe needle | Johnson & Johnson | ||
| tissue forceps | Johnson & Johnson | ||
| trocar(XCEL) | Ethicon Endo-Surgery | 695C71 | |
| Ultrasonic knife spacers | Johnson & Johnson | ||
| ultrasound knife | Johnson & Johnson | ||
| yarn ball | Johnson & Johnson |
References
- Yoon, J. G., et al. Pancreatic cystic neoplasms: A review of current recommendations for surveillance and management. Abdominal Radiol. 46 (8), 3946-3962 (2021).
- Kromrey, M. L., et al. Prospective study on the incidence, prevalence and 5-year pancreatic-related mortality of pancreatic cysts in a population-based study. Gut. 67 (1), 138-145 (2018).
- Falconi, M., et al. Pancreatic insufficiency after different resections for benign tumours. The British J Surg. 95 (1), 85-91 (2008).
- Fujii, T., et al. Comparison of pancreatic head resection with segmental duodenectomy and pylorus-preserving pancreatoduodenectomy for benign and low-grade malignant neoplasms of the pancreatic head. Pancreas. 40 (8), 1258-1263 (2011).
- Wang, M., et al. Practice patterns and perioperative outcomes of laparoscopic pancreaticoduodenectomy in China. Ann Surg. 273 (1), 145-153 (2021).
- Müller, M., et al. Middle segmental pancreatic resection: An option to treat benign pancreatic body lesions. Ann Surg. 244 (6), 918-920 (2006).
- Baca, I., Bokan, I. Laparoscopic segmental pancreas resection and pancreatic cystadenoma. Chirurg. 74 (10), 961-965 (2003).
- Addeo, P., Julliard, O., Imperiale, A., Goichot, B., Bachellier, P. Middle-segment preserving pancreatectomy for multifocal neuroendocrine pancreatic tumors. Surg Oncol. 35, 466-467 (2020).
- Wakabayashi, T., et al. Robotic central pancreatectomy for well-differentiated neuroendocrine tumor: Parenchymal-sparing procedure. Ann Surg Oncol. 26 (7), 2121 (2019).
- Liu, G., et al. Case report: Treatment of intraductal papillary mucinous neoplasms located in middle-segment pancreas with end-to-end anastomosis reconstruction after laparoscopic central pancreatectomy surgery through a pigtail-tube-stent placement of the pancreatic duct. Front Surg. 9, 937682 (2022).
- Yang, F., et al. Central pancreatectomy with external drainage of monolayer pancreaticojejunostomy for prevention of postoperative pancreatic fistula: A retrospective cohort study. Int J Surg. 51, 104-108 (2018).
- Wang, X., et al. Enucleation of pancreatic solid pseudopapillary neoplasm: Short-term and long-term outcomes from a 7-year large single-center experience. Eur J Surg Oncol. 44 (5), 644-650 (2018).
- Siech, M., Mattfeldt, T., Schlosser, W., Beger, H. Duodenum-preserving pancreatic head resection in patients with benign and borderline tumors of the pancreatic head. Langenbeck’s Arch Surg. 385 (3), 229-233 (2000).
- Iacono, C., Ruzzenente, A., Bortolasi, L., Guglielmi, A. Central pancreatectomy: The dagradi serio iacono operation. Evolution of a surgical technique from the pioneers to the robotic approach. World J Gastroenterol. 20 (42), 15674-15681 (2014).
- Wang, P., et al. Diagnosis and treatment of solid-pseudopapillary tumors of the pancreas: A single institution experience with 97 cases. Pancreatology. 18 (4), 415-419 (2018).
- Sun, D., et al. Pancreaticojejunal bridge stent internal drainage as a safe reconstruction technique after middle segmental pancreatic resection. Chinese ed J. 131 (11), 1367-1368 (2018).

