A Protocol to Acquire the Degenerative Tenocyte from Humans
Summary
In vitro use of degenerative tenocytes is essential when investigating the efficacy of novel treatment on tendinopathy. However, most research studies use only the animal model or a healthy tenocyte. We propose the following protocol to isolate human degenerative tenocytes during surgery.
Abstract
Tendinopathy, a painful condition that develops in response to tendon degeneration, is on the rise in the developed world due to increasing physical activity and longer life expectancy. Despite its increasing prevalence, the underlying pathogenesis still remains unclear, and treatment is generally symptomatic. Recently, numerous therapeutic options, including growth factors, stem cells, and gene therapy, were investigated in hopes of enhancing the healing potency of the degenerative tendon. However, the majority of these research studies were conducted only on animal models or healthy human tenocytes. Despite some studies using pathological tenocytes, to the best of our knowledge there is currently no protocol describing how to obtain human degenerative tenocytes. The aim of this study is to describe a standard protocol for acquiring human degenerative tenocytes. Initially, the tendon tissue was harvested from a patient with lateral epicondylitis during surgery. Then biopsy samples were taken from the extensor carpi radialis brevis tendon corresponding to structural changes observed at the time of surgery. All of the harvested tendons appeared to be dull, gray, friable, and edematous, which made them visually distinct from the healthy ones. Tenocytes were cultured and used for experiments. Meanwhile, half of the harvested tissues were analyzed histologically, and it was shown that they shared the same key features of tendinopathy (angiofibroblastic dysplasia or hyperplasia). A secondary analysis by immunocytochemistry confirmed that the cultured cells were tenocytes with the majority of the cells having positive stains for mohawk and tenomodulin proteins. The qualities of the degenerative nature of tenocytes were then determined by comparing the cells with the healthy control using a proliferation assay or qRT-PCR. The degenerative tenocyte displayed a higher proliferation rate and similar gene expression patterns of tendinopathy that matched previous reports. Overall, this new protocol might provide a useful tool for future studies of tendinopathy.
Introduction
Tendinopathy is a chronic degenerative musculoskeletal condition that develops in various parts of the body. Recently, the number of cases of tendinopathy has increased greatly in the developed world due to growing participation in recreational sports and increased life expectancy1,2. The cause of tendinopathy is considered to be multifactorial and these causes include ischemia, oxygen free radical injuries, an imbalance between vasoconstrictor and vasodilator innervations, internal micro-tears, and changes to neuro-regulation3,4,5,6,7,8. Most treatments for tendinopathy only relieve its symptoms. Moreover, treatments without tissue regeneration require a long time for rehabilitation and achieve a limited response from injured tendons, which imposes a clinical challenge for physicians9.
The incompetence of current treatment options along with the lack of the degenerative tendon's ability to self-heal has lead researchers to take interest in exploring alternative treatment strategies. Recently, new studies reported many promising results for enhancing the healing efficacy of the tendinopathy tendons using growth factors, stem cell based therapy, and gene therapy10,11,12.
Through a literature review, we found that the involved studies may be divided into two categories based on their analysis materials: animal models such as a rat, a mouse, or a rabbit; and human models. With regard to the animal model, currently there are two popular techniques to generate tendinopathy: chemical induction of injury or mechanical overloading the model. However, each animal model was limited in reproducing the complex human tendinopathy pathology13,14.
Most papers using human samples were analyzed histologically or performed the in vitro experiment based on a healthy human tenocyte instead of a degenerative tenocyte15,16,17,18,19,20,21. Only a few papers reported that they used a human degenerative tenocyte, but they did not describe in detail the protocol used to get the degenerative tenocyte from the human22,23. In this context, it should be noted that successful results from either the animal model or the healthy tissue/tenocyte may not necessarily predict human efficacy or efficacious dosing because tendon degeneration is a complicated process and the pathogenesis is still not fully understood.
Collectively, it is necessary to describe the standard protocol for obtaining the degenerative tenocyte from human tissue without causing adverse effects to the donor. This article describes a protocol on how to acquire the human degenerative tenocyte. To validate the protocol, the harvested tissues were analyzed histologically. Then, the cultured cell was confirmed as the degenerative tenocyte by using immunocytochemistry (ICC), a quantitative real time-polymerase chain reaction (qRT-PCR), and a viability assay.
Protocol
The protocol was conducted in accordance with the Declaration of Helsinki and the protocol was approved by the Institutional Review Board at CHA Bundang Medical Center.
1. Degenerative Tendon Tissue Harvest from the Patient
- Diagnose lateral epicondylitis by taking a medical history and using physical exam findings: tenderness over the tendinous origin close to the lateral epicondyle; pain evoked by resisted extension of the wrist joint.
- Use the following inclusion criteria: over 18 years of age; a history of lateral epicondylitis for a minimum of six months; recalcitrant for non-operative treatment; at least three months have passed since injection of corticosteroid, platelet rich plasma, or botulinum toxin
- Exclude the following: pregnant women; patients with a history of cervical spine disease, elbow arthritis, rheumatologic disease, surgery around elbow, and nerve entrapment syndrome; patients refusing to donate tissue.
- Surgical technique
NOTE: See Figure 124.- After general anesthesia by isoflurane and endotracheal intubation, put the arm on the table and apply a tourniquet. Then apply betadine agent on the whole arm and drape with an aseptic surgical sheet.
- Expose the lateral elbow through a 3–5 cm incision with No. 15 surgical scalpel blade just anteromedial to the lateral epicondyle and proximal to the level of the joint.
- Visually identify the extensor carpi radialis longus (ECRL) and extensor aponeurosis interface and make a splitting incision 2–3 mm in depth between the ECRL and extensor aponeurosis with a No. 15 surgical scalpel blade at the identified interface.
- Extract the ECRL anteriorly, which will bring the pathologic extensor carpi radialis longus brevis (ECRB) origin below into direct view.
- Visually identify the pathologic degenerative tissue by its characteristic dull grayish color and usually edematous and friable tissue.
- After identification, carefully resect all degenerative tissue sharply using No. 15 surgical scalpel and mini-blades.
- Embed the resected tissue (about 1 cm3) into phosphate buffered saline (PBS) immediately and remove all the surrounding tissue except tendon tissue carefully into about 10 mL of PBS as soon as possible.
- In cases with bony exostosis at the lateral epicondyle, remove exostosis using a rongeur and smoothen it with a rasp. Make multiple drill holes (diameter 1.6 mm, about 6–8 holes) in the anterolateral condyle to enhance vascular supply. This is optional.
- Close the wound layer by layer using non-absorbable suture material.
- Healthy control tenocyte
- Obtain healthy tenocytes from the remaining tendon of the auto-hamstring or auto-patella tendon during anterior cruciate ligament reconstruction, and use it as the control for the following experiment25.
NOTE: The number of samples used in this study were three in each group.
- Obtain healthy tenocytes from the remaining tendon of the auto-hamstring or auto-patella tendon during anterior cruciate ligament reconstruction, and use it as the control for the following experiment25.
2. Histology
- Store about half of the harvested tissue in neutral buffered 10% formalin in a chemical fume hood or equivalent.
- Embed the tissue in a paraffin block (4–5 mL) and section it in 4–5 µm sections coronally.
- Stain sections from control and degenerative tendon with Hematoxylin and Eosin stain (H&E) and Alcian blue stain at a pH of 2.5. Perform H&E staining in an automated stain machine as follows.
- Deparaffinize using xylene (3 times, 5 min, respectively).
- Hydrate from graded alcohols to water (100% alcohol, 4 min; 100% alcohol, 3 min; 95% alcohol, 2 min; 70% alcohol, 1 min; water, 2 min).
- Stain in Hematoxylin for 5 min. Wash well in water for 2 min.
- Differentiate in 1% acid alcohol (1% HCl in 70% alcohol) for 3 s. Wash well in water for 3 min.
- Neutralize HCl by dipping in an 0.5% ammonia for 10 s, followed by a 3 min water wash.
- Stain in Eosion for 5 min.
- Dehydrate through alcohols (80% alcohol, 30 s; 95% alcohol, 1 min; 100% alcohol 1 min, 100% alcohol 2 min).
- Clear in xylene (3 times, 2 min, 2 min, and 3 min, respectively).
- Mount with a cover slide.
- Perform immunohistochemitry (IHC) using the Bond Polymer Refine Detection kit according to the manufacturer's instructions with minor modifications.
- After deparaffinization using xylene, perform an antigen retrieval procedure using Bond Epitope Retrieval Solution for 30 min at 100 °C. The Bond Epitope Retrieval Solution contains a citrate based buffer and surfactant (1 L, pH 5.9–6.1).
- Quench endogenous peroxidases by incubating the tissue with hydrogen peroxide for 5 min.
- Incubate the sections for 15 min at an ambient temperature (21-22 °C) with primary antibodies against vascular endothelial growth factor (VEGF) (1:200), tenomodulin (1:200), or mohawk (1:200).
- Perform secondary antibody tagging with a biotin-free polymeric horseradish peroxidase-linker antibody conjugate system.
- Use secondary rabbit anti mouse IgG in 10% (v/v) animal serum in Tris-buffered saline/0.09% 2-Methyl-4-isothiazolin-3-one solution to localize mouse antibodies.
- Use polymer anti-rabbit Poly-HRP-IgG (<25 µg/mL) containing 10% (v/v) animal serum in Tris-buffered saline/0.09% to localize rabbit antibodies.
- Use 3,3'-Diaminobenzidine tetrahydrochloride hydrate in a stabilizer solution to visualize the complex via a brown precipitate.
- Counterstain with <0.1% hematoxylin (blue) to visualize the cell nuclei.
- Observe the slides stained with H&E, Alcian blue stains, and IHC for VEGF, tenomodulin, and mohawk under light microscope and obtain representative microscopic images of each slide under one high power field (400X).
3. Tenocyte Culture
- Tissue preparation
- Prepare the tendon sample by removing all the surrounding tissue thoroughly with micro-scissors and forceps.
- Wash with PBS and mince into small pieces (about 1 mm3 or less).
- Digest tissue for 1 h in 30 mL of Dulbecco's Modified Eagle's Medium (DMEM) supplemented with 30 mg/mL Collagenase II at 37 °C.
- Pass cells through a 100 µm cell strainer.
- Deactivate Collagenase II by adding 1 mL of fetal bovine serum (FBS).
- Centrifuge at 196 x g for 5 min.
- Cell culture
- Seed 3 x 105 cells into a 100 mm dish and culture with DMEM supplemented with 10% FBS and 1% Antibiotic-Antimycotic solution at 37 °C in a 5% CO2 incubator for 1 week.
- Change the culture medium every three days until 80% confluence occurs. Culture both healthy control and degenerative cell samples until passage four and use for experiment.
4. Immunocytochemistry (ICC)
- Transfer 200 µL of cultured cell (2 x 105 cells) to the eight wells of a chamber slide and grow the cells to confluence with the addition of fresh media for 1 day.
- Wash the cells with PBS and fix with 500 µL of 4% formaldehyde per well.
- Incubate the slides with 0.5% Triton X-100 in PBS for 10 min for permeabilization of the membranes.
- Block in PBS with 1% bovine serum albumin and 0.05% TWEEN-20 for mohawk and tenomodulin, respectively.
- Incubate in the dark with mouse anti-mohawk monoclonal antibody (1:100 dilution) and goat anti-tenomodulin antibody (1:100 dilution) at 4 °C overnight.
- Incubate the secondary antibodies (Alexa 555-anti goat (1:200) for tenomodulin; Alexa 488-anti mouse (1:200) for mohawk) in the dark for 1 h at room temperature.
- Mount with 0.5 µL of a fluorescence mounting medium.
- Analyze using a fluorescence microscope (400X).
5. Proliferation Assay
- Measure cell viabilities using water-soluble tetrazolium (WST)-1.
- Seed both healthy and degenerative cells into 96 well plates at a density of 2 x 103 cells per well for 24, 72, and 120 h.
- After incubation, add 10 µL of the 10% WST-1 solution to each well.
- Incubate the plates for 3 h at 37 °C in 5% CO2.
- Measure the optical densities at 450 nm using a microplate reader. Take readings at least three times at all time points for each sample.
- Measure cellular DNA amount using the BrdU assay.
- Seed both healthy and degenerative cell into 96 well plates at a density of 2 x 103 cells per well for 24, 72, and 120 h.
- After incubation, add 10 µL of 10% BrdU solution to each well.
- Incubate the plates for 3 h at 37 °C in 5% CO2.
- Add 100 µL/well of the Fixing/Denaturing Solution (60–70% ethanol, 0.1–0.5% sodium hydroxide) and keep the plate at room temperature for 30 min.
- Add 100 µL/well prepared 1x detection antibody solution and keep the plate at room temperature for 1 h.
- Remove solution and wash plate three times with 1x Wash Buffer.
- Add 100 µL/well prepared 1x HRP-conjugated secondary antibody solution and keep the plate at room temperature for 30 min.
- Remove the solution and wash plate three times with 1x Wash Buffer.
- Add 100 µL of 50% TMB Substrate.
- Incubate for 30 min at room temperature.
- Add 100 µL of STOP Solution.
- Measure the optical densities at 450 nm using a microplate reader.
NOTE: Take readings at least three times at all time points for each sample.
6. Statistical Analysis
- Collect and analyze data using SPSS.
- Depict data by mean ± standard error of mean.
- Use Mann Whitney U test.
- Consider differences statistically significant when the p value is less than 0.05 (p <0.05).
Representative Results
Histological analyses revealed that the harvested tissue from lateral epicondylitis had the characteristics of a tendinopathic tendon.H&E section of tendinopathy degenerative tendon revealed a disorganized collagen bundle with a loss of polarity and fine straight, strongly packed parallel fiber structures. Histological signs suggestive of degeneration such as higher cellularity and enlarged nuclei without the typical spindle shape were common in samples. Additionally, collagen bundles of the degenerated tendon were relatively weak eosin stained by H&E but were positively stained by Alcian blue indicating increased proteoglycans and glycosaminoglycans substance.
In all cases, blood vessels were increased in number and aggregates occupying spaces embedded between fibers were compared to normal slit-like blood vessels. In the IHC staining, cells of degenerated tendons showed cytoplasmic granular positive reaction to VEGF in comparison to the negative reaction of control ones. Collectively, these findings confirmed that the harvested tissues from lateral epicondylitis were degenerative tissues and suitable for the degenerative tenocyte culture (see Figure 2).
The cultured cells were confirmed as tenocytes by ICC and the harvested tissues were confirmed by IHC as tendon tissue. Most of the cultured cells and cells in tendon tissue showed a positive stain for the representative tenocyte markers known as mohawk (green) proteins and tenomodulin (red) proteins with an elongated appearance under microscopy (see Figure 3). Also, the harvested tissues had the positive staining for mohawk proteins and tenomodulin proteins immunohistochemically (see Supplementary Figure 1). These suggested that the harvested tissues were composed by the tendon tissue.
Cultured tenocytes from the harvested tissue of lateral epicondylitis had the characteristic features that correspond to tendinopathy. Both degenerative and healthy tenocytes were cultured for 4 days under the same condition. At each time point, the proliferation rate was measured by BrdU assay and WST-1 assay. The results showed that the proliferation rate of the degenerative cells was significantly higher compared to the controls as previously reported (p <0.05) (see Figure 4A).
Five genes which are known to be up-regulated in the degenerative tendon were analyzed by qRT-PCR. Expressions of the genes, COL3A1, ACTA2, TAC1 (SP), TAC receptor 1, and PTGS2 (COX2) were increased more significantly in the cultured cells from the degenerative tendon than in the cells from the healthy ones. The relative expressions for all genes are shown in Figure 4B and Supplemental Figure 2.
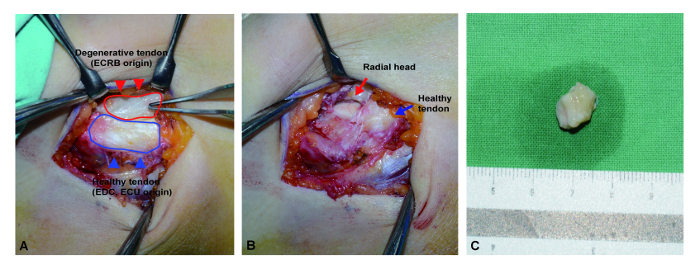
Figure 1: Surgical photo of degenerative tendon harvest. (A) After skin incision and dissection, the pathologic degenerative tissue on the common extensor origin was exposed, showing a characteristic dull-grayish color with edematous change (red line). Conversely, the general appearance of normal tendon tissue was shiny and firm with a slightly grayish tone (black line). (B) All identified degenerative tissues were resected sharply and then the radial head bone was exposed. (C) All resected tissues were embedded into the phosphate buffered saline immediately and the surrounding non-tendinous tissue was carefully dissected as soon as possible. ECRB: extensor carpi radialis brevis. EDC: extensor digitorum communis. ECU: extensor carpi ulnaris. Please click here to view a larger version of this figure.
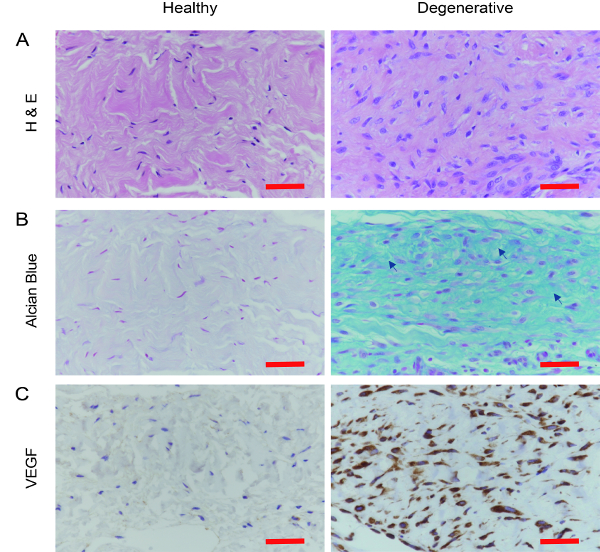
Figure 2: Confirmation of degenerative tendon histologically. (A) In the H & E staining, degenerative samples from the lateral epicondylitis had disorganized collagen bundles with loss of polarity and increased cell number compared to the healthy control. (B). Alcian blue staining showed that the degenerative tendon had increased ground substance consisting of proteoglycans and glycosaminoglycans with several mucoid patches and vacuoles between fibers (Arrow). (C). Additionally, VEGF immunohistochemistry demonstrated increased staining in vessel formation in degenerative tendon samples compared to the control samples. VEGF: Vascular endothelial growth factor. Scale bar = 50 µm. Please click here to view a larger version of this figure.
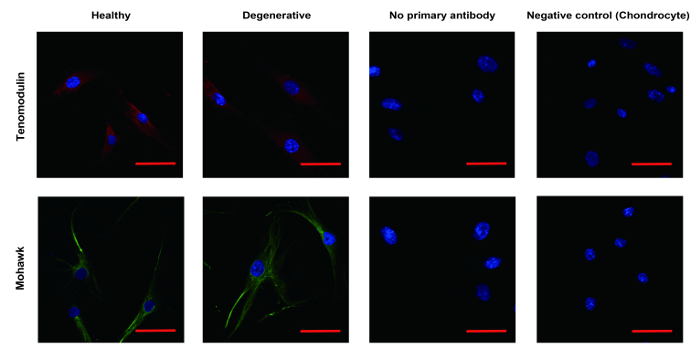
Figure 3: Identification of tenocyte by ICC. The cultured cells and cells in tendon tissue were confirmed as tenocyte by ICC. Most of the cells showed positive stain for the representative tenocyte marker, including mohawk (green) and tenomodulin (red) with elongated appearance under microscopy. Chondrocyte was used as the negative control. ICC: Immunocytochemistry. Scale bar = 50 µm. Please click here to view a larger version of this figure.
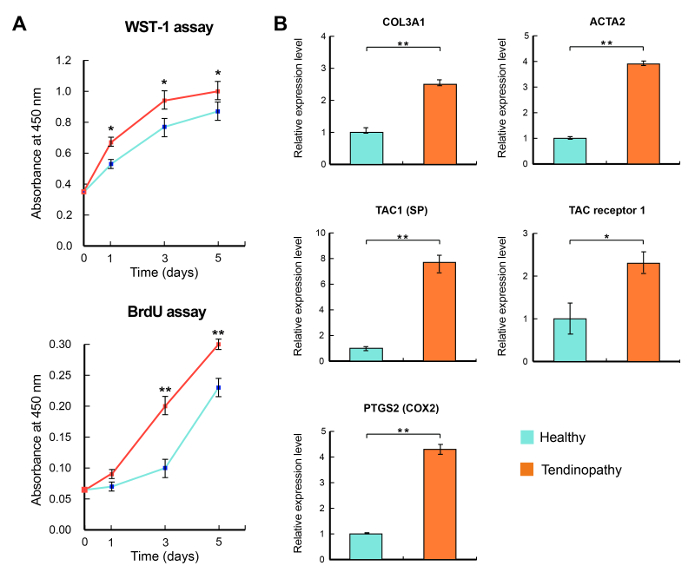
Figure 4: Characteristics of degenerative tenocyte. (A, B) Degenerative tenocytes (red) had a higher proliferation rate with a notable increase in cellularity. (C) Five genes that are known to be related in the development of tendinopathy were significantly elevated in the degenerative tenocytes. Gene expression levels were normalized against GAPDH. *: mean <0.05, **: mean <0.01, respectively. SP: substance P. Please click here to view a larger version of this figure.
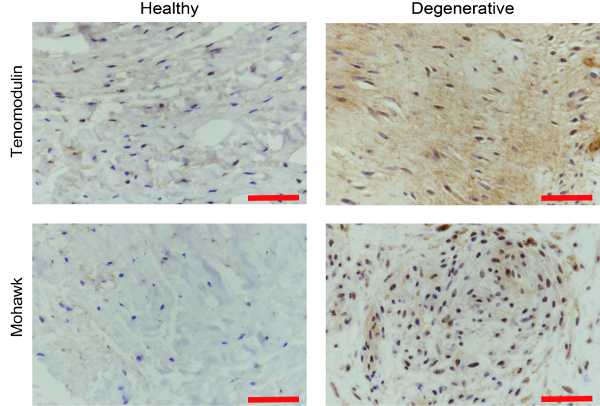
Supplementary Figure 1: Histological confirmation of the harvested tissue as the tendon tissue. The harvested tissue was also analyzed by IHC for mohawk and tenomodulin to determine whether the harvested tissue had the adequate characteristics of tendon tissue. IHC: Immunohistochemistry. Scale bar = 50 µm. Please click here to view a larger version of this figure.
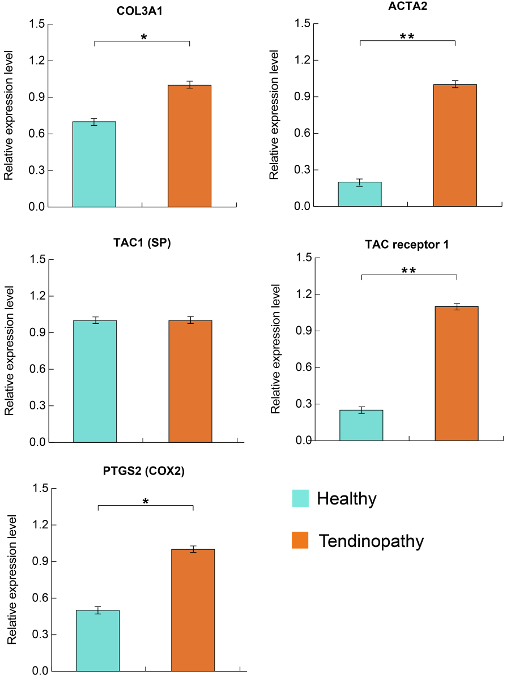
Supplementary Figure 2: Expression of tendinopathy related genes in tenocyte. The transcripts of five genes normalized by actin expression were significantly elevated in the degenerative tenocytes and have similar trends to Figure 4. Gene expression levels were normalized against actin with a mean < 0.05 and < 0.01, respectively. SP: substance P. Please click here to view a larger version of this figure.
Discussion
A number of previous studies have reported how to create chronic tendinopathic animal models using different procedures such as collagenase or kartogenin injection, treadmill running, and more26,27. Although numerous studies showed promising therapeutic effects based on these animal models, experiments using the human degenerative tenocyte would be crucial in the field of tendinopathy in order to reproduce the efficacy of treatment. In this article, we established a protocol to successfully harvest and culture human degenerative tenocytes consistently. Both harvested tendon tissue and the cultured tenocyte showed the common characteristics of the degenerative tendon and tenocyte7,28.
In our experience, for the successful tissue harvest, it is essential to comprehend the morphological changes frequently associated with degenerative tendon and to accurately delineate that area during surgery. Degenerative tissue is typically grey or brown in color and the tissue is thin, fragile, and disorganized with loose texture. The inclusion and exclusion criteria of the protocol should be strictly kept with careful evaluation of previous treatments before harvest.
Tissue size is also important for a successful cell culture. We recommend harvesting more than 1 cm3. Usually, as long as all of the degenerative area is removed, the amount of collected tissue would be enough for the cell culture. Lastly, we did not use tenocytes over passage six in all experiments. Until passage six, we believe that the cultured cells still had the characteristics of degeneration.
Our protocol has several advantages. These advantages include no harm to the patient since the degenerative tissue was supposed to be removed during surgery, efficiency since the amount of tissue required is enough for the experiment, highly ethical due to no violation of healthy tissues, reproducibility in that pathological tissues from humans can be readily obtained during surgery, and, lastly, ease of application once surgical techniques become familiar.
However, we acknowledge that our experiment has several limitations. First, we cannot completely exclude the remnant effect of previous corticosteroid or platelet rich plasma injection even though we included only patients who had passed at least three months from receiving any previous treatment. In addition, in this protocol, we only harvested the ECRB tendon and used it to culture degenerative tenocytes since the ECRB tendon is a common tendinopathy site for surgery along with Achilles and rotator cuff tendons. Further studies should be carried out with a larger sample size focusing on any differences between various tendinopathy sites.
In conclusion, this validated protocol for acquiring human degenerative tenocytes will be a useful tool for future investigations in tendon biology and for testing novel therapeutic interventions.
Disclosures
The authors have nothing to disclose.
Acknowledgements
This research was supported by a grant from the Korea Health Technology R&D Project through the Korea Health Industry Development Institute (KHIDI), which was funded by the Ministry of Health & Welfare, Republic of Korea (grant number: HI16C1559).
Materials
| Scalpel | Kisanbio | KS-Q0306-15 | No. 15 |
| Mini-blade | Beaver | 374769 | |
| Dulbecco's modified Eagle's medium (DMEM) | Gibco | 11995065 | |
| Collagenase Ⅱ | Sigma-Aldrich | C6885 | |
| PBS | Gibco | 14190250 | |
| fetal bovine serum (FBS) | Gibco | 16000044 | |
| 50 mM ascorbic acid-2-phosphate | Sigma-Aldrich | A5960 | |
| Antibiotic-Antimycotic solution | Gibco | 15240062 | |
| 4% formaldehyde | Bio-solution | BP031 | |
| Triton X-100 | Sigma-Aldrich | X100-100ml | |
| BSA | Rdtech | C0082 | |
| TWEEN 20 | Sigma-Aldrich | P9416-100ml | |
| MKX (C-5) | Santa cruz biotechnology | sc-515878 | |
| Tenomodulin (N-14) | Santa cruz biotechnology | sc-49325 | |
| Fluorescence Mounting Medium | DAKO | S3023 | |
| DAPI (4',6-Diamidino-2-Phenylindole, Dihydrochloride) | Thermo Fisher Scientific | D1306 | |
| WST-1 | Dojindo Molecular Technologies | CK04 | |
| BrdU Cell Proliferation Assay Kit | Cell Signaling Technology | #6813 | |
| TRIzol Reagent | Invitrogen | 15596018 | |
| iScript cDNA Synthesis Kit | Bio-Rad | 170-8891 | |
| TaqMan Gene Expression Master Mix | Applied Biosystems | 4369016 | |
| GAPDH | Thermo Fisher Scientific | Hs02786624_g1 | |
| COL3A1 | Thermo Fisher Scientific | Hs00943809_m1 | |
| ACTA2 | Thermo Fisher Scientific | Hs00426835_g1 | |
| TAC1 | Thermo Fisher Scientific | Hs00243225_m1 | |
| TACR1 | Thermo Fisher Scientific | Hs00185530_m1 | |
| PTGS2 | Thermo Fisher Scientific | Hs00153133_m1 | |
| ACTB | Thermo Fisher Scientific | Hs99999903_m1 | |
| Cell Strainers (100 µm) | Corning | 352360 | |
| 100mm culture dish | Thermo Fisher Scientific | 8188207 | |
| 8-well Chamber Slide | Thermo Fisher Scientific | 154534 | |
| 96 Well Clear Flat Bottom Polystyrene TC-Treated Microplates | Corning | 3596 | |
| Nikon Eclipse 50i Microscope | Nikon | ||
| VERSA max microplate reader | Molecular Devices | ||
| CFX96 Real-Time PCR Detection System | Bio-Rad | ||
| Formalin solution, neutral buffered, 10% | Sigma-Aldrich | HT501128 | |
| Paraffins | Leica Biosystems | 3801340 | |
| Ethanol | JUNSEI CHEMICAL | 90303-2185 | |
| Hematoxylin | DAKO | CS70030-2 | |
| Eosin | DAKO | CS70130-2 | |
| Alcian blue | DAKO | AR16011-2 | |
| Citric acid | Sigma-Aldrich | 251275 | |
| Xylene | JUNSEI CHEMICAL | 25165-0430 | |
| Endogenous peroxidases | DAKO | S200380-2 | |
| Canada balsam | JUNSEI CHEMICAL | 23255-1210 | |
| Microtome Blade | FEATHER | A35 | |
| Slide glass | SUPERIOR | 1000612 | |
| Cover glass | Marienfeld-Superior | 101050 | |
| VEGF | Santa cruz biotechnology | sc-7269 | |
| SPSS Software | IBM | Ver. 18.0 | |
| Multi-purpose Centrifuge | LABOGENE | 1248R |
References
- Ackermann, P. W., Renstrom, P. Tendinopathy in sport. Sports Health. 4 (3), 193-201 (2012).
- Maffulli, N., Wong, J., Almekinders, L. C. Types and epidemiology of tendinopathy. Clinical Sports Medicine. 22 (4), 675-692 (2003).
- Lui, P. P., Chan, L. S., Fu, S. C., Chan, K. M. Expression of sensory neuropeptides in tendon is associated with failed healing and activity-related tendon pain in collagenase-induced tendon injury. American Journal of Sports Medicine. 38 (4), 757-764 (2010).
- Han, S. H., et al. Effects of corticosteroid on the expressions of neuropeptide and cytokine mRNA and on tenocyte viability in lateral epicondylitis. Journal of Inflammation (London). 9 (1), 40 (2012).
- Uchio, Y., et al. Expression of neuropeptides and cytokines at the extensor carpi radialis brevis muscle origin. Journal of Shoulder and Elbow Surgery. 11 (6), 570-575 (2002).
- Lieber, R. L., Loren, G. J., Friden, J. In vivo measurement of human wrist extensor muscle sarcomere length changes. Journal of Neurophysiology. 71 (3), 874-881 (1994).
- Regan, W., Wold, L. E., Coonrad, R., Morrey, B. F. Microscopic histopathology of chronic refractory lateral epicondylitis. American Journal of Sports Medicine. 20 (6), 746-749 (1992).
- Sharma, P., Maffulli, N. Tendon injury and tendinopathy: healing and repair. Journal of Bone and Joint Surgery American volume. 87 (1), 187-202 (2005).
- Lui, P. P. Stem cell technology for tendon regeneration: current status, challenges, and future research directions. Stem Cells Cloning. 8, 163-174 (2015).
- Dahlgren, L. A., van der Meulen, M. C., Bertram, J. E., Starrak, G. S., Nixon, A. J. Insulin-like growth factor-I improves cellular and molecular aspects of healing in a collagenase-induced model of flexor tendinitis. Journal of Orthopedic Research. 20 (5), 910-919 (2002).
- Schnabel, L. V., et al. Mesenchymal stem cells and insulin-like growth factor-I gene-enhanced mesenchymal stem cells improve structural aspects of healing in equine flexor digitorum superficialis tendons. Journal of Orthopedic Research. 27 (10), 1392-1398 (2009).
- Durgam, S. S., Stewart, A. A., Sivaguru, M., Wagoner Johnson, A. J., Stewart, M. C. Tendon-derived progenitor cells improve healing of collagenase-induced flexor tendinitis. Journal of Orthopedic Research. 34 (12), 2162-2171 (2016).
- Titan, A., Andarawis-Puri, N. Tendinopathy: Investigating the Intersection of Clinical and Animal Research to Identify Progress and Hurdles in the Field. Journal of Bone and Joint Surgery Review. 4 (10), (2016).
- Dirks, R. C., Warden, S. J. Models for the study of tendinopathy. Journal of Musculoskeletal Neuronal Interaction. 11 (2), 141-149 (2011).
- de Mos, M., et al. Can platelet-rich plasma enhance tendon repair? A cell culture study. American Journal of Sports Medicine. 36 (6), 1171-1178 (2008).
- Scherb, M. B., Han, S. H., Courneya, J. P., Guyton, G. P., Schon, L. C. Effect of bupivacaine on cultured tenocytes. Orthopedics. 32 (1), 26 (2009).
- Wong, M. W., et al. Effect of dexamethasone on cultured human tenocytes and its reversibility by platelet-derived growth factor. Journal of Bone and Joint Surgery American Volume. 85 (10), 1914-1920 (2003).
- Tempfer, H., et al. Effects of crystalline glucocorticoid triamcinolone acetonide on cultered human supraspinatus tendon cells. Acta Orthopaedics. 80 (3), 357-362 (2009).
- Menon, A., et al. New insights in extracellular matrix remodeling and collagen turnover related pathways in cultured human tenocytes after ciprofloxacin administration. Muscles Ligaments Tendons J. 3 (3), 122-131 (2013).
- Backman, L. J., Fong, G., Andersson, G., Scott, A., Danielson, P. Substance P is a mechanoresponsive, autocrine regulator of human tenocyte proliferation. PLoS One. 6 (11), 27209 (2011).
- Backman, L. J., Eriksson, D. E., Danielson, P. Substance P reduces TNF-alpha-induced apoptosis in human tenocytes through NK-1 receptor stimulation. Britich Journal of Sports Medicine. 48 (19), 1414-1420 (2014).
- Rolf, C. G., Fu, B. S., Pau, A., Wang, W., Chan, B. Increased cell proliferation and associated expression of PDGFRbeta causing hypercellularity in patellar tendinosis. Rheumatology (Oxford). 40 (3), 256-261 (2001).
- Hoppe, S., et al. Tenocytes of chronic rotator cuff tendon tears can be stimulated by platelet-released growth factors. Journal of Shoulder and Elbow Surgery. 22 (3), 340-349 (2013).
- Schipper, O. N., Dunn, J. H., Ochiai, D. H., Donovan, J. S., Nirschl, R. P. Nirschl surgical technique for concomitant lateral and medial elbow tendinosis: a retrospective review of 53 elbows with a mean follow-up of 11.7 years. American Journal of Sports Medicine. 39 (5), 972-976 (2011).
- Cook, J. L., Feller, J. A., Bonar, S. F., Khan, K. M. Abnormal tenocyte morphology is more prevalent than collagen disruption in asymptomatic athletes’ patellar tendons. Journal of Orthopedic Research. 22 (2), 334-338 (2004).
- Yuan, T., et al. Creating an Animal Model of Tendinopathy by Inducing Chondrogenic Differentiation with Kartogenin. PLoS One. 11 (2), 0148557 (2016).
- Lui, P. P., Maffulli, N., Rolf, C., Smith, R. K. What are the validated animal models for tendinopathy. Scandinavian Journal of Medical Scientific Sports. 21 (1), 3-17 (2011).
- Wilhelm, A. Lateral epicondylitis review and current concepts. Journal of Hand Surgery American Volume. 34 (7), 1359-1360 (2009).

