Development of a Noninvasive, Laser-Assisted Experimental Model of Corneal Endothelial Cell Loss
Summary
Here, we present a protocol to detach corneal endothelial cells (CEC) from Descemet’s membrane (DM) using a neodymium:YAG (Nd:YAG) laser as an ex vivo disease model for bullous keratopathy (BK).
Abstract
Nd:YAG lasers have been used to perform noninvasive intraocular surgery, such as capsulotomy for several decades now. The incisive effect relies on the optical breakdown at the laser focus. Acoustic shock waves and cavitation bubbles are generated, causing tissue rupture. Bubble sizes and pressure amplitudes vary with pulse energy and position of the focal point. In this study, enucleated porcine eyes were positioned in front of a commercially available Nd:YAG laser. Variable pulse energies as well as different positions of the focal spots posterior to the cornea were tested. Resulting lesions were evaluated by two-photon microscopy and histology to determine the best parameters for an exclusive detachment of corneal endothelial cells (CEC) with minimum collateral damage. The advantages of this method are the precise ablation of CEC, reduced collateral damage, and above all, the non-contact treatment.
Introduction
Transparency of the cornea is essential for the transmission of light to the retina and its photoreceptors1. In this regard, a relative state of dehydration is critical to keep the collagen fibers within the corneal stroma correctly aligned. This homeostasis is maintained by corneal endothelial cells (CEC) located on the Descemet’s membrane (DM)2. The endothelium is the innermost corneal layer. It has an important barrier and pump function, which is crucial for corneal transparency3. In contrast to the epithelium, the endothelium is not able to self-renew4. Therefore, any cell damage caused by disease or trauma stimulates the remaining endothelial cells to enlarge and migrate, to cover resulting defects and to maintain corneal functionality5. However, if the CEC density falls below a critical threshold, decompensation of the endothelium leads to an edema, resulting in blurred vision and discomfort or even severe pain4. Despite the availability of drugs to relieve symptoms, currently the only definitive treatment in these cases is corneal transplantation, which can be performed in the form of a full-thickness graft or a lamellar endothelial transplantation. The latter procedure is available as Descemet's membrane endothelial keratoplasty (DMEK) as well as Descemet's stripping automated endothelial keratoplasty (DSAEK)6. However, the protection of remaining CEC and enhancing their survival could be an alternative target, which needs an adequate disease model to test potential therapeutic drugs.
Current CEC loss disease models focus on the destruction of the endothelium through the injection of toxic agents (e.g., benzalkonium chloride) into the anterior chamber or by mechanical abrasion of the cells using an invasive descemetorhexis technique7,8. While these models are well established, disadvantages such as general inflammatory response and imprecise collateral damage exist. Therefore, these models are more likely to represent final stages of the disease, when the above-mentioned surgical options are inevitable.
With advances in cellular treatment strategies such as stem cells and gene therapy, the application of these cellular therapies could be useful in early stages of CEC loss9. Subsequently, we need a model that represents these earlier stages of the disease more adequately. In this regard, cell culture models have improved over the last decade but are still limited in their validity, as cells in vitro cannot come close to replicating the complex interactions that occur between the different cell types within the cornea10. Therefore, ex vivo and in vivo disease models are still in high demand and improving the existing ones is of utmost interest.
Noninvasive, intraocular surgery by photodisruption using a neodymium:YAG (Nd:YAG) laser has become a routine procedure for ophthalmologists worldwide since its introduction in the late 1970s11. Photodisruption relies on nonlinear light absorption leading to the formation of plasma, generation of acoustic shock waves, and creation of cavitation bubbles, whenever the application site is located in a liquid environment12. In general, these processes contribute to the intended effect of precise tissue cutting. However, they can also be the source of unnecessary collateral damage limiting the local confinement of laser surgery13.
The prediction of resulting mechanical effects has significantly improved through characterization of the shock wave propagation and cavitation course. It is our goal to target CEC with as little damage to surrounding tissue as possible to provide a noninvasive, laser-assisted experimental disease model for the early stages of CEC loss. For this purpose, it is necessary to determine the optimal pulse energies and positions of the focal spots of the laser.
Protocol
All procedures involving animal tissue follow the guidelines of the local Animal Care and Ethics Committee.
1. Preparation of organ culture and laser treatment
- Obtain freshly enucleated porcine eyes from the local abattoir. Keep them cool (4 °C) in Dulbecco's modified Eagle medium (DMEM) with high glucose, supplemented with L-glutamine, sodium pyruvate, penicillin/streptomycin (1%), and porcine serum (10%), henceforth referred to in this article as full medium.
- Remove extracellular tissues with scissors and soak the eyes in 5% povidone-iodine ophthalmic solution for 5 min before placing them in sterilized phosphate-buffered saline (PBS) until use.
- Screen eyes for major anterior segment pathologies, such as corneal scarring, edema, and other opacities with a spectral-domain optical coherence tomography device (Table of Materials).
- Position the eyes in front of a slit-lamp unit equipped with a Nd:YAG laser (Table of Materials), which has a wavelength of 1,064 nm and a focal spot diameter of 10 µm in air.
NOTE: For optimal positioning a 3D-printed holding apparatus is used, which was designed to hold the eye firm, without putting too much pressure on it (Figure 1). - Use a magnification of 12x and deflect the illumination to visualize the individual corneal layers.
- Set the pulse energy (e.g., 1.6 mJ) and focus point (e.g., 0.16 mm) for selective ablation of endothelial cells.
- Place a clear cornea paracentesis close to the limbus and inject viscoelastic (Table of Materials) to stabilize the anterior chamber.
- Excise the laser-treated central cornea using an 8 mm trephine.
- Place the excised cornea in a well of a 12-well plate with the endothelial site facing upwards and incubate the specimen in 3 mL of full medium at 37 °C for up to 3 days.
NOTE: Potential cytoprotective agents can be added to the medium during this step.
2. Preparation for histology
- Prepare Sorensen’s buffer with a pH of 7.4 containing 19.6 mL of 133 mM KH2PO4 and 80.4 mL of 133 mM Na2HPO4.
- Remove the medium from the cornea-containing well and fixate the tissue for 20 min at room temperature (RT) using methanol-free paraformaldehyde (4%) in Sorensen’s buffer.
- Place tissue in 20% sucrose in PBS until tissue sinks (1 h) and then in 30% sucrose in PBS overnight at RT. Take care to avoid contact with bubbles and the air surface interface. Embed tissue in optimal cutting temperature (OCT) compound and store at -80 °C.
- Cut sections 10 μm thick using a cryostat at -27 °C.
NOTE: A camel hairbrush is useful to help guide the emerging section over the knife blade. - Transfer the section to a microscope slide by touching the slide to the tissue within 1 min of cutting it to avoid freeze-drying of the tissue. Store the slides at -80 °C.
3. Hematoxylin and eosin (H&E) staining
- Air dry sections for several minutes to remove moisture.
- Stain with filtered 0.1% Mayers hematoxylin for 10 min in a 50 mL tube.
- In a Coplin jar, rinse in cool running ddH2O for 5 min and dip in 0.5% eosin 10x.
- Dip in ddH2O until the eosin stops streaking and then dip in 50% (10x) as well as 70% (10x) EtOH.
- Equilibrate in 95% EtOH (30 s) and 100% EtOH (60 s) before dipping in xylene several times.
- Finally mount and coverslip the specimen before taking images using a light microscope.
Representative Results
Using the procedure presented here, we treated eyes with a Nd:YAG laser, evaluating different pulse energies (1.0−4.6 mJ) and positions of focal points (distance from the posterior surface of the cornea: 0.0−0.2 mm) to find the optimal parameters. Multiple replicates (n = 3) were evaluated for each constellation of the laser parameters (12 x 21).
In addition to the above-mentioned protocol, specimen was analyzed with a two-photon microscope before fixation and H&E staining. The two-photon microscope used a solid-state, mode-locked 80 MHz Ti:sapphire laser with a tuning range of 690−1b040 nm and a mean laser output of >900 mW at 800 nm as light source. It delivered pulses with a width of approximately 150 fs to the sample. Images were taken with a microscope objective (20x/0.95) at a wavelength of 730 nm and 30 mW of laser power.
Two-photon as well as light microscopy images were independently reviewed by 3 reviewers, who were blinded to experimental settings and had to assign the images to three categories: (1) no damage, (2) too much damage, or (3) right amount of damage (Figure 2 and Figure 3). Based on their evaluation a heatmap was calculated (Figure 4). Using this heatmap it is possible to select the right constellation of laser parameters to selectively ablate CEC with minimal damage to surrounding tissue (green). Results show that the focal point of the laser must be at least 0.15 mm behind the corneal endothelium for the lowest pulse energy (1.0 mJ) tested. For pulse energies higher than 2.9 mJ, the longest focal distance tested (0.2 mm) is still too close to the endothelium.
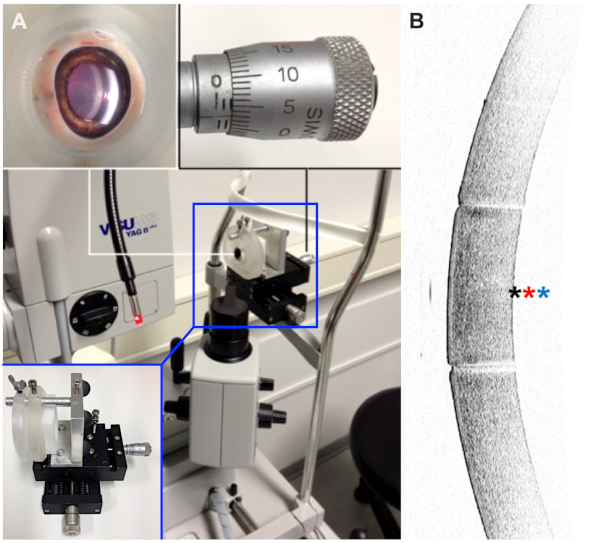
Figure 1: Experimental setup. (A) Eyes were fixed in a partially 3D-printed holding apparatus, which allowed precise alignment with respect to the laser beam. (B) Before laser treatment, the tissue was evaluated with an anterior segment optical coherence tomography device to check for major anterior segment pathologies. Positions of focal laser points are indicated with exemplary for 0.0 mm (black asterisk), 0.1 mm (red asterisk), and 0.2 mm (blue asterisk). Please click here to view a larger version of this figure.
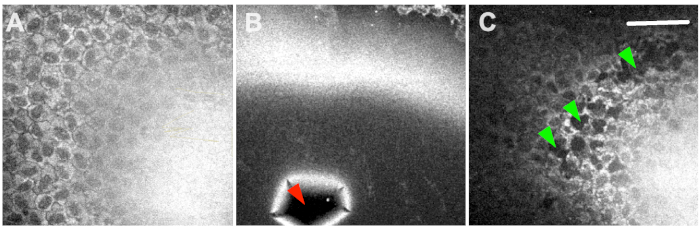
Figure 2: Two-photon microscopy. Results ranged from no damage at all (A), extensive collateral damage (B) to selective ablation of endothelial cells (C). The red arrowhead shows a ruptured Descemet’s membrane, and green arrowheads indicate selective ablation of CEC-clusters. Scale bar = 100 µm. Please click here to view a larger version of this figure.
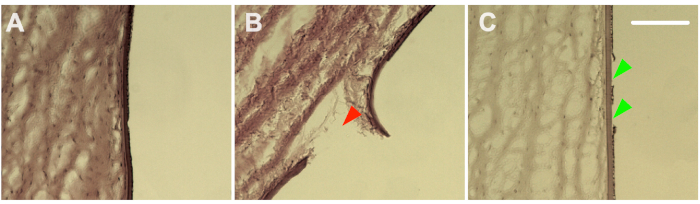
Figure 3: Histology. Hematoxylin and eosin staining confirmed the damage range from no damage at all (A), extensive collateral damage (B) to selective ablation of endothelial cells (C). The red arrowhead shows a ruptured Descemet’s membrane, and green arrowheads indicate selective ablation of CEC-clusters. Scale bar = 100 µm. Please click here to view a larger version of this figure.
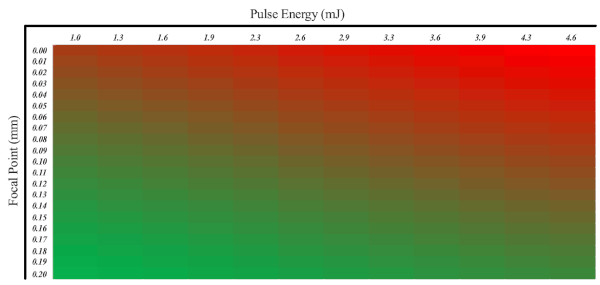
Figure 4: A heatmap showing the probability of selective CEC damage. In this regard, the pulse energy as well as the position of the Nd:YAG laser focal point must be taken into account. Excessive damage is shown in red, and the desired portion of damage is shown in green. Please click here to view a larger version of this figure.
Discussion
The results of this pilot study indicate that a Nd:YAG laser can be used to selectively ablate corneal endothelial cells when appropriate parameters for energy dose and focus point position are chosen.
As the endothelial function is important for corneal transparency and safeguarding the cornea from stromal edema, models of endothelial dysfunction play an important role in the development of anti-edematous drugs or surgical procedures. There are several established in vitro models for mimicking the in vivo situation10,14,15, but as generally known, in vitro models cannot completely imitate the influences of enzymes and cytokines or the effect of cell-cell-interaction. In contrast, this newly developed ex vivo model of endothelial cell loss offers the possibility to monitor different states of the disease and corneal decompensation in the natural environment.
As the cornea in our model is excised with a trephine after the laser procedure, the physiology of the cornea changes and similar to the in vitro situation, regional interactions are significantly hampered. However, the local interface remains intact and especially the cellular communication to other cells within the cornea persists. Our study revealed that under these circumstances the cornea maintains its function for three days in culture, which offers sufficient time to observe and evaluate potential therapeutic agents. On the other hand, longtime healing processes cannot be investigated.
In our model, we used porcine eyes as larger quantities of those can be easily obtained. Furthermore, porcine eyes mimic human eyes very well. In contrast to rabbits that are regularly used for experiment, porcine eyes have a Bowman’s membrane. Nevertheless, the corneal thickness of the porcine eye differs considerably from the human eye. In particular, the porcine stroma is much thicker and there is no difference between central and peripheral thickness in porcine corneas16. It must also be considered that human CEC do not have any healing capability while this regenerative feature is reported in some animals, such as pigs and rabbits17,18. Our study did not focus on wound healing processes, but this difference should be kept in mind when translating results. As the wound healing of animal CEC does not exceed four days, it might still be observed in our cultured tissues even if they last only for three days.
Comparing our experimental setup with previous studies, the applied energy levels were similar19. Instead of focusing only on the endothelium, different locations of focal points were evaluated. Therefore, the main difference of our setup to earlier studies is its potential to induce specific endothelial damage without damaging either DM or stromal tissue. Accurate monitoring of energy dose and focus position enables selective CEC ablation without causing shock wave damage to other parts of the cornea. Also, we have not noticed stromal or subepithelial edema directly after laser treatment20.
A previous study showed that temperatures of ~40 °C can lead to CEC damage21. We did not measure the induced temperature, but it might be of interest for further studies. Moreover, the effect of different types of laser systems should be evaluated. Earlier studies showed a difference between laser induced circumscribed CEC damage and other CEC injuries19,22. This might also limit the comparability to human tissue and diseases because laser induced damage seems to be followed by different disease development processes. Interestingly, the wound healing after laser application stopped at the burned DM in earlier studies19. The source of injury might be less important if the DM remains intact.
Higher energy levels can pose a higher risk of extended injury22. Our results show that using higher energy levels (<2.9 mJ) for selective CEC damage requires a tighter focus range. While the damage to CEC was mechanically applied in previous studies17, laser-induced damage used here has a more precise dosing of the lesion and can be easily used in in vivo studies.
It should be noted that only a small number of eyes have been treated and examined according to this protocol. As mentioned above, there might be interindividual differences in the response to the laser treatment as well as differences between the corneas of different animal species. Since CEC damage can be produced at different focal positions, certain thresholds should not be exceeded to avoid extended damage.
Finally, the lesions generated in this study were placed in the central part. An earlier study of porcine eyes showed accelerated wound healing in the corneal periphery, which might be due to its proximity to limbal stem cells17 as the corneal thickness in porcine eyes does not differ between regions. It should be evaluated in future studies whether laser parameters should be adjusted when switching from the center of the cornea to the periphery.
In conclusion, our study introduces a noninvasive model for further investigations on CEC dysfunction. Limitations of ex vivo or in vivo studies in terms of usage of animal instead of human tissue remain and must be considered when interpreting the results.
Disclosures
The authors have nothing to disclose.
Acknowledgements
We thank Christine Örün and Jan A. M. Sochurek for their help with experimental methods.
Materials
| BARRON VACUUM TREPHINE | Katena | K20-2058 | |
| Cryostat | Leica | CM 3050S | |
| Dulbecco’s Modified Eagle’s Medium – high glucose | PAA | E-15009 | |
| Eye holder | Self | N/A | |
| Inverted Microscope | Leica | DMI 6000 B | |
| KH2PO4 | Merck | 529568 | |
| Na2HPO4 | Merck | 1065860500 | |
| Nd:YAG laser | Zeiss Meditec | visuLAS YAG II plus | |
| OCT Tissue Tek | Sakura Finetechnical | 4583 | |
| Penicillin-Streptomycin | Sigma-Aldrich | P4333 | |
| Phosphate Buffered Saline (PBS) | Gibco | 10010056 | |
| Porcine serum | Sigma-Aldrich | 12736C | |
| Spectral-domain optical coherence tomograph | Heidelberg Engineering | Spectralis | |
| Tissue culture plate 12-well | Sarstedt | 833921 | |
| Two-Photon Microscope | JenLab | DermaInspect | |
| Viscoelastic | OmniVision | Methocel |
References
- DelMonte, D. W., Kim, T. Anatomy and physiology of the cornea. Journal of Cataract and Refractive Surgery. 37 (3), 588-598 (2011).
- Edelhauser, H. F. The balance between corneal transparency and edema: the Proctor Lecture. Investigative Ophthalmology & Visual Science. 47 (5), 1754-1767 (2006).
- Tuft, S. J., Coster, D. J. The corneal endothelium. Eye. 4, 389-424 (1990).
- Bourne, W. M. Biology of the corneal endothelium in health and disease. Eye. 17, 912-918 (2003).
- He, Z., et al. 3D map of the human corneal endothelial cell. Scientific Reports. 6, 29047 (2016).
- Gain, P., et al. Global Survey of Corneal Transplantation and Eye Banking. JAMA Ophthalmology. 134 (2), 167-173 (2016).
- Schwartzkopff, J., Bredow, L., Mahlenbrey, S., Boehringer, D., Reinhard, T. Regeneration of corneal endothelium following complete endothelial cell loss in rat keratoplasty. Molecular Vision. 16, 2368-2375 (2010).
- Bredow, L., Schwartzkopff, J., Reinhard, T. Regeneration of corneal endothelial cells following keratoplasty in rats with bullous keratopathy. Molecular Vision. 20, 683-690 (2014).
- Bartakova, A., Kunzevitzky, N. J., Goldberg, J. L. Regenerative Cell Therapy for Corneal Endothelium. Current Ophthalmology Reports. 2 (3), 81-90 (2014).
- Zhao, B., et al. Development of a three-dimensional organ culture model for corneal wound healing and corneal transplantation. Investigative Ophthalmology & Visual Science. 47 (7), 2840-2846 (2006).
- Aron-Rosa, D., Aron, J. J., Griesemann, M., Thyzel, R. Use of the neodymium-YAG laser to open the posterior capsule after lens implant surgery: a preliminary report. Journal – American Intra-Ocular Implant Society. 6 (4), 352-354 (1980).
- Vogel, A., Hentschel, W., Holzfuss, J., Lauterborn, W. Cavitation bubble dynamics and acoustic transient generation in ocular surgery with pulsed neodymium: YAG lasers. Ophthalmology. 93 (10), 1259-1269 (1986).
- Vogel, A., Schweiger, P., Frieser, A., Asiyo, M. N., Birngruber, R. Intraocular Nd:YAG laser surgery: laser-tissue interaction, damage range, and reduction of collateral effects. IEEE Journal of Quantum Electronics. 26 (12), 2240-2260 (1990).
- Zhu, Q., Zhu, Y., Tighe, S., Liu, Y., Hu, M. Engineering of Human Corneal Endothelial Cells In Vitro. International Journal of Medical Sciences. 16 (4), 507-512 (2019).
- Li, Z., et al. Nicotinamide inhibits corneal endothelial mesenchymal transition and accelerates wound healing. Experimental Eye Research. 184, 227-233 (2019).
- Pescina, S., et al. Development of a convenient ex vivo model for the study of the transcorneal permeation of drugs: histological and permeability evaluation. Journal of Pharmaceutical Sciences. 104 (1), 63-71 (2015).
- Smeringaiova, I., et al. Endothelial Wound Repair of the Organ-Cultured Porcine Corneas. Current Eye Research. 43 (7), 856-865 (2018).
- Yamashita, K., et al. A Rabbit Corneal Endothelial Dysfunction Model Using Endothelial-Mesenchymal Transformed Cells. Scientific Reports. 8 (1), 16868 (2018).
- Schubert, H. D., Trokel, S. Endothelial repair following Nd:YAG laser injury. Investigative Ophthalmology & Visual Science. 25 (8), 971-976 (1984).
- Zhang, W., et al. Rabbit Model of Corneal Endothelial Injury Established Using the Nd: YAG Laser. Cornea. 36 (10), 1274-1281 (2017).
- McCally, R. L., Bonney-Ray, J., de la Cruz, Z., Green, W. R. Corneal endothelial injury thresholds for exposures to 1.54 micro m radiation. Health Physics. 92 (3), 205-211 (2007).
- Nash, J. P., Wickham, M. G., Binder, P. S. Corneal damage following focal laser intervention. Experimental Eye Research. 26 (6), 641-650 (1978).

