A Modified Heterotopic Swine Hind Limb Transplant Model for Translational Vascularized Composite Allotransplantation (VCA) Research
Summary
Vascularized Composite Allotransplantations (VCA) have become a clinical reality. However, broad clinical application of VCA is limited by chronic multi-drug immunosuppression. The authors present a reliable and reproducible large animal model to translate novel immunomodulatory strategies that can minimize or potentially eliminate the need of immunosuppression in VCA.
Abstract
Vascularized Composite Allotransplantation (VCA) such as hand and face transplants represent a viable treatment option for complex musculoskeletal trauma and devastating tissue loss. Despite favorable and highly encouraging early and intermediate functional outcomes, rejection of the highly immunogenic skin component of a VCA and potential adverse effects of chronic multi-drug immunosuppression continue to hamper widespread clinical application of VCA. Therefore, research in this novel field needs to focus on translational studies related to unique immunologic features of VCA and to develop novel immunomodulatory strategies for immunomodulation and tolerance induction following VCA without the need for long term immunosuppression.
This article describes a reliable and reproducible translational large animal model of VCA that is comprised of an osteomyocutaneous flap in a MHC-defined swine heterotopic hind limb allotransplantation. Briefly, a well-vascularized skin paddle is identified in the anteromedial thigh region using near infrared laser angiography. The underlying muscles, knee joint, distal femur, and proximal tibia are harvested on a femoral vascular pedicle. This allograft can be considered both a VCA and a vascularized bone marrow transplant with its unique immune privileged features. The graft is transplanted to a subcutaneous abdominal pocket in the recipient animal with a skin component exteriorized to the dorsolateral region for immune monitoring.
Three surgical teams work simultaneously in a well-coordinated manner to reduce anesthesia and ischemia times, thereby improving efficiency of this model and reducing potential confounders in experimental protocols. This model serves as the groundwork for future therapeutic strategies aimed at reducing and potentially eliminating the need for chronic multi-drug immunosuppression in VCA.
Introduction
Vascularized Composite Allotransplantation (VCA) such as hand and face transplants are now a clinical reality with numerous hand and face transplants performed worldwide12. Despite the fact that early and intermediate results are favorable and highly encouraging2, the requirement of chronic multidrug immunosuppression continues to limit its widespread clinical application. The advancements in murine models of VCA including super-microsurgical anastomoses and nonsuture cuff techniques13, 3 have paved the way to a better understanding of alloimmune responses in VCA. Myriads of immunomodulatory protocols have been proposed for clinical applications based on our better understanding of immune mechanisms in VCA but they need to be validated in a large animal model that would be reasonably predictive of their performance in humans7. Based on physiologic and immunologic similarities between human and porcine organ systems6, swine VCA models can be considered reliable and cost-effective alternatives to canine9 and nonhuman primate models1.
This article provides a detailed overview of the methodology used in our MHC-defined swine heterotopic hind limb transplant model, which serves as groundwork for our current and future immunomodulatory strategies aimed at inducing immune tolerance to VCA and hence broadening its clinical application. We utilize well-characterized inbred pigs bred to homozygosity at the swine leukocyte antigen locus specifically for their use in transplant-related research11. We raise a vascularized osteomyocutaneous flap based on femoral vessels. The flap contains intact vascularized bone marrow in the distal femur and proximal tibia. The anteromedial thigh skin is also included in the graft and is exteriorized to the dorsolateral aspect of the recipient animal for immune monitoring of the most immunogenic component of the VCA. Dorsolateral positioning facilitates clinical examination in standing and sitting positions and also keeps the allograft skin relatively clean.
Ustener et al. introduced one of the first large animal translational models in VCA by transplanting radial forelimb osteomyocutaneous flaps in outbred farm pigs15. The group utilized this model to demonstrate for the first time that acute rejection in VCA which included the highly immunogenic skin component could be delayed and treated with a clinically relevant strategy without significant drug-specific complications and side effects. The favorable results obtained in this study subsequently built a foundational step in designing drug regimens for human reconstructive transplantation. Although these early pig VCA models were well suited for developing protocols to prevent rejection of skin, muscle, bones, nerves and vessels they lacked specialized structures such as articular cartilage and synovial membranes of joints. Subsequent efforts were focused on including the medial digit of the animal, which necessitated full-length cast placement to prevent graft dislodgement14. Although suitable to investigate rejection of all major components of limb transplantation, one of the major limitations of this model was post-transplant ambulatory difficulty due to cast placement. Thus, heterotopic swine limb allotransplantation models, consisting of the tibia, fibula, knee joint, distal femur, surrounding muscle, and a skin paddle, were created to primarily study immunological aspects of VCA while allowing the animal to freely ambulate postoperatively with minimal morbidit 8.
The development of well-characterized SLA-defined inbred pigs through the pioneering work of Dr. David H. Sachs led to a new era of translational VCA research. Utilizing a heterotopic hind limb transplant model in a minor antigen mismatch setting, Mathes et al.10 demonstrated indefinite survival of musculoskeletal components with a short course of cyclosporine treatment. The skin component survival, however, was only prolonged when compared to no treatment controls. The loss of the skin component of the graft was attributed to an isolated and highly vigorous immune response, in particular, to the epidermis. Similarly, using fully mismatched pigs with T-cell depletion, a short course of cyclosporine and cytokine mobilized donor peripheral blood mononuclear cells induced tolerance only to musculoskeletal components and the skin component was still rejected5. This phenomenon, called ‘split tolerance’, brought a paradigm shift in VCA research with a greater focus on the highly immunogenic skin component, which is an integral component of the majority of reconstructive transplants performed to date.
In this modified model, we utilize end-to-end anastomosis by ligating the recipient femoral artery and rotating it cephalad (Figure 1). This not only reduces ischemia time by allowing the use of a conventional coupling device but also decreases the chances of anastomotic failure. We have not observed any ischemic events following ligation of the femoral artery in our recipients indicating that collateral circulation was sufficient to provide vascularity to the native leg. Additionally, in this modified method, the externalized skin component is mobilized based on the underlying perforator vessels and is positioned laterally (Figure 1) in contrast to a ventral groin position in the traditional model10. This allows easy visualization of the graft for immune monitoring in a standing or sitting position of the animal.
Hence, a reliable and reproducible large animal model is essential to investigate tolerance induction strategies towards the skin component of VCA and to develop novel noninvasive immune monitoring strategies for better prediction of graft survival.
Protocol
In this video publication, all animal procedures were conducted in accordance with an animal protocol approved by the Johns Hopkins University Institutional Animal Care and Use Committee (IACUC).
1. Preoperative Planning
- We utilize MHC-defined MGH inbred miniature swine (15-20 kg) in our translational studies for limb allotransplantation wherein one male donor provides limbs for two female recipients (Figure 1). Prior to surgery, donor and recipient animals undergo thorough clinical evaluation by a veterinarian.
- In order to minimize anesthesia and ischemia time, donor and recipient procedures are conducted simultaneously on three operating tables in one dedicated large animal operating room. Teamwork and coordination among surgical teams as well as the veterinary staff are critical for overall success of this procedure. The surgical plan is discussed with the veterinary team in a formal meeting 1-2 weeks prior to the day of surgery.
- A tunneled central venous catheter (7 Fr double lumen Hickman catheter) is placed in an external or internal jugular vein of each recipient animal prior to transplant for immunosuppressive drug level monitoring and intravenous administration of immunosuppressive and/or immunomodulatory drugs. These catheters are placed under direct vision through a venous cut-down technique and tunneled posterior to exit high on the dorsal neck and secured using monofilament nonabsorbable sutures and adhesive bandage wrap around the neck.
- Keep animals NPO (no solid food but are allowed water ad lib) at least 12 hr before surgery.
- On the day of surgery, sedate animals with ketamine 20 mg/kg and xylazine 2 mg/kg IM.
- Place an appropriately sized endotracheal tube and connect it to the anesthesia machine and ventilator (maintained on isoflurane 0.5-3%)
- Place an intravenous catheter in a marginal ear vein and administer weight based 0.9% saline throughout the procedure.
- Administer pre-emptive analgesia (buprenorphine 0.02 mg/kg IV).
- Administer prophylactic antibiotic (cefazolin 20-25 mg/kg IV) prior to the initial incision to both donor and recipient animals.
- Use sterile technique in all procedures for both recipients and donors. This includes the use of autoclaved or gas sterilized instruments, masks, head caps, sterile surgical gowns and sterile gloves. Shave the area of the incision with a clipper and disinfect with alternating Betadine solution and alcohol.
Intraoperative Monitoring:
- After induction and intubation, maintain anesthesia with an inhalation mixture 0.5-3% isoflurane in oxygen.
- Monitor heart rate, pulse oximetry, ECG, end-tidal CO2 and rectal temperature continuously and record every 15 min.
- Prevent hypothermia with a Bair Hugger warm forced-air blanket.
Osteomyocutaneous Limb Allograft Harvest from Donor Pig:
- Place the donor animal in a supine position on the operating table and drape in a sterile manner.
- Use near-infra red laser angiography to identify perforator vessels to the anteromedial skin. Inject indocyanine green at approximately 0.06 mg/kg diluted in 2-5 ml of normal saline through peripheral vascular access. Approximately 10 sec later, perform 30 sec-2 min of near infrared recordings. Use the video from these recordings to identify perforators. Based on perforators, mark an area of skin (approximately 100 cm2) for monitoring.
- Use a scalpel to make a groin skin incision in continuity with markings for the skin paddle (Figure 2).
- Identify femoral vessels and isolate them distally to the level of the suprageniculate branches and proximally to the level of the inguinal ligament.
- Dissect the skin and subcutaneous tissue while preserving the area of the skin paddle. Suture the edges of the skin to underlying muscles to avoid contraction during flap harvest.
- Perform an osteotomy just above the tarsus using a reciprocating saw (Electric Pen Drive, Synthes, West Chester PA).
- Divide the muscles in the proximal thigh using electrocautery.
- Divide the femur at mid-shaft leaving an osteomyocutaneous flap on a vascular pedicle. The flap contains the skin paddle, underlying thigh muscles, knee joint, distal femur and proximal tibia which includes intact vascularized bone marrow with its unique immunologic features.
- Use bone wax to achieve hemostasis in the marrow spaces. Smooth bone edges using ronjeurs in preparation for the recipient.
- Keep the graft perfused on its vascular pedicle until the recipient’s femoral vessels are prepared (Figure 3).
- Once the recipient dissection is complete, ligate the donor femoral vessels as proximal as possible and infuse the graft with histidine-tryptophan-ketoglutarate (HTK, Custodiol, Newtown PA) prior to transplantation.
NOTE: The donor limb is transplanted on the contralateral side of the recipient i.e. the left donor limb for the right side of the recipient and the right donor limb for the left side of the recipient). - Euthanize the donor pig immediately after harvesting the second hind limb using 100 mg/kg IV sodium pentobarbital. Death is confirmed by the veterinary staff per established protocol.
4. Recipient Procedure (Hind Limb Allotransplantation)
- Start the recipient induction and intubation immediately after the initial donor incision to allow preparation of recipient vessels while the donor limb is being harvested. This eliminates unnecessary wait time and reduces the total anesthesia time for the donor and recipients.
- Position the animal supine with a 30° rotation on the operating side to allow exposure of the dorsolateral side.
- Make a groin incision and expose the femoral vessels; isolate them distally to the level of the suprageniculate branches and proximally to the level of the inguinal ligament.
- Create a subcutaneous pocket from the groin to the dorsolateral abdominal wall for the graft inset (Figure 4).
- Ligate the donor vessels and flush the graft with HTK.
- Perform the graft inset in an inverted manner: Have the skin paddle facing dorsolateral to allow easy immune monitoring in a standing position and the cut ends of the femoral vessels facing caudally to allow end-to-end vascular anastomoses without any tension on the vessels (Figure 5).
- If available, use a vascular coupling device (Synovis, St Paul MN) for venous anastomoses (size 2.5-3.5 is suitable for 10-20 kg animals). This significantly reduces ischemia time when compared to conventional methods.
- Perform arterial anastomoses using a conventional suture technique with 9-0 suture (Synovis, St Paul MN)
- After vascular patency is confirmed, secure the graft in place with 3-0 PDS sutures (Figure 5). The muscles of the graft are sutured to the abdominal wall muscles. The graft muscles should not be sutured to the recipient thigh muscles since it can be deleterious when the animal moves around the cage.
- Exteriorize the skin paddle on the dorsolateral side for immune monitoring (Figure 6) and suture it to the adjacent skin using 3-0 Vicryl subcutaneous sutures and 4-0 monofilament absorbable interrupted skin sutures.
- Close the groin skin in layers using 3-0 Vicryl subcutaneous sutures and 4-0 monofilament absorbable interrupted skin sutures.
- Place a 50-100 mcg/hr fentanyl patch for post-operative analgesia.
- After hind limb allograft transplantation, return the animal to its pen once awake and breathing comfortably on its own.
Representative Results
Twenty-four SLA-defined swine heterotopic hind limb transplants were performed using our modified technique with a mean ischemia time of 78 min (Range: 62-94 min). Graft inset and dorsolateral skin paddle positioning were achieved without difficulty in all animals. Near infrared laser angiography showed excellent graft perfusion in all recipients. The initial twelve venous anastomoses were performed using conventional suture techniques while the last twelve venous anastomoses were performed using a vascular coupling device. One animal with the conventional suture technique required a reanastomosis when a venous thrombus was identified immediately post-procedure. No complications were observed in any anastomoses performed with the coupling device. Recipient animals received a short course (30 days) of tacrolimus monotherapy with or without donor bone marrow (BM) infusion and co-stimulatory blockade. Tacrolimus dosing was adjusted to achieve target levels of 10-15 ng/ml. The short course tacrolimus only and untreated animals served as controls. The co-stimulation blockade based immunomodulatory protocol resulted in over 6 month survival post-transplant. There was no evidence of GVHD in any recipient. All long-term survivors (beyond 150 days post-transplant) had viable vascularized bone marrow at the time of euthanasia which demonstrates reliability of this model for investigating unique immunologic features of the bone marrow component of VCA (Figure 7).
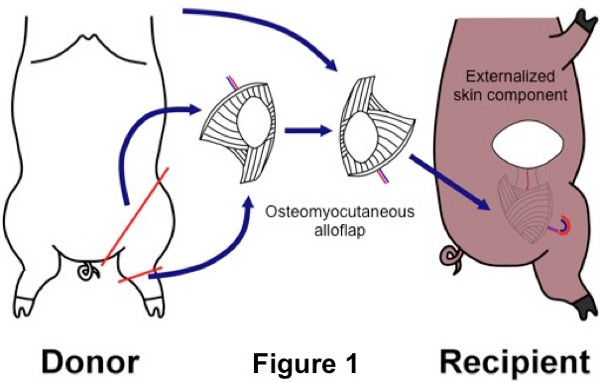
Figure 1. Schematic diagram of a swine heterotopic hind limb transplant. An osteomyocutaneous flap is harvested from the donor hind limb and transplanted to a subcutaneous pocket along the abdominal wall of the recipient.
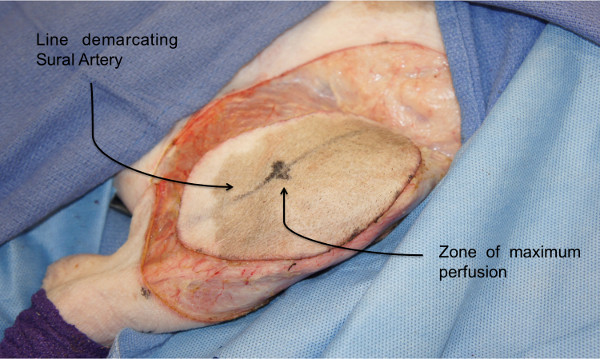
Figure 2: Osteomyocutaneous flap harvest: Donor skin paddle. Perforator zones in the anterolateral thigh are identified using laser angiography to demarcate the skin paddle of the osteomyocutaneous flap.
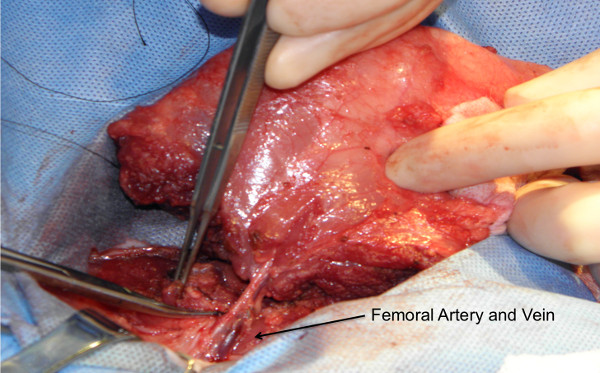
Figure 3: Osteomyocutaneous flap harvest: Graft on its vascular pedicle. Flap consisting of the distal femur, knee joint, proximal tibia, fibula, thigh muscles and skin paddle is harvested on a femoral vascular pedicle.
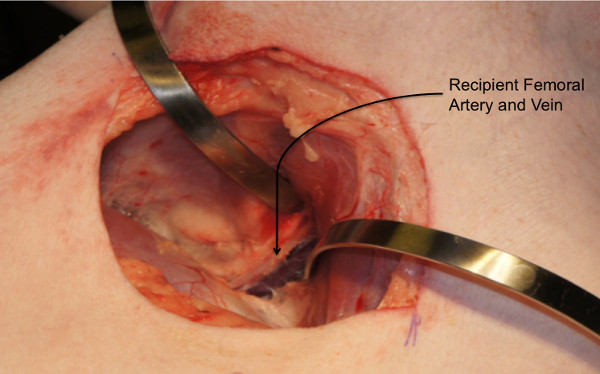
Figure 4: Recipient procedure: Creation of a subcutaneous abdominal pocket. Subcutaneous dissection is carried out to create an abdominal wall pocket extending from the groin to the dorsolateral abdominal wall.
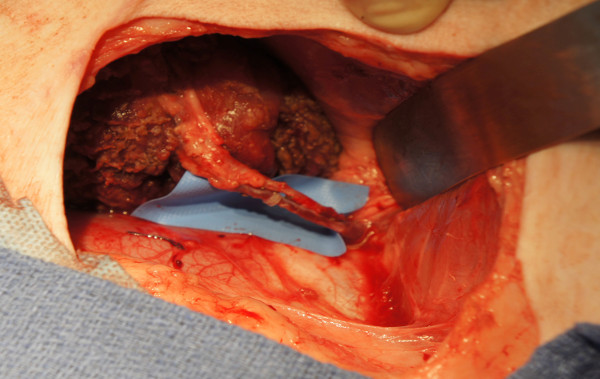
Figure 5: Recipient procedure: Graft inset and reperfusion following microvascular anastomosis. End-to-end femoral vessel anastomosis is performed after flap inset. The donor limb is used for the contralateral side of the recipient (i.e. the left donor limb for the right side of the recipient and the right donor limb for the left side of the recipient).
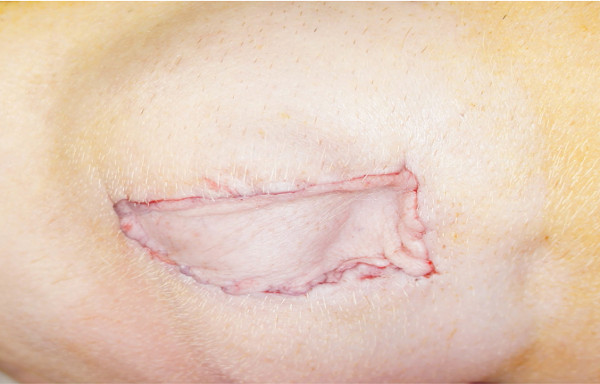
Figure 6: Skin component exteriorized to dorsolateral position for immune monitoring. During inset, the flap is positioned in a way that the skin paddle faces the dorsolateral abdominal wall where it is sutured to the recipient skin. This position allows easy monitoring of the flap.
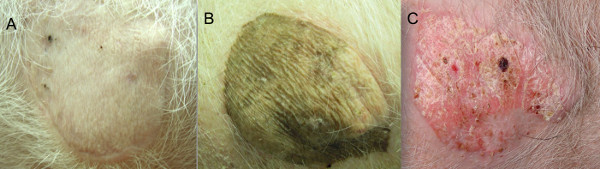
Figure 7: Representative images from transplanted animals: (A) Long term survivor (>150 days) with no clinical evidence of rejection. (B) Long term survivor (>150 days) with no clinical evidence of rejection. The allograft was obtained from a donor with dark color skin. Both (A) and (B) received co-stimulation blockade (CTLA4Ig) based immunomodulatory therapy. (C) Negative control (short-term tacrolimus therapy only) with de-epithelialization and advanced rejection as soon as tacrolimus was withdrawn (Day 30).
Discussion
Historically, the heterotopic hind limb transplant protocol included exteriorization of a skin paddle to the ventral abdominal wall and the vessels were anastomosed in an end-to-side manner (Hettiarachty 2004). However, in our modified method, an inverted flap insetting and end-to-end anastomoses bring the skin paddle more laterally and hence facilitates immune monitoring in a standing position of the animal. The identification of the sural artery and the zones of maximum perfusion using near infrared laser angiography further improves the reliability of the skin paddle.
In our modified technique, we perform end-to-end anastomosis between the femoral vessels to minimize technical failures related to microvascular anastomosis. End-to-end anastomosis also enabled us to use a vascular coupling device (Synovis St. Paul MN) for venous anastomosis, which further decreased warm ischemia time. In our experience, ischemia time was more predictable with the use of a coupling device and since variation in ischemia time is directly correlated with immunologic outcome, this modification improved the reliability of this model. However, the use of a coupling device results in additional material costs but is still considered cost-effective based on the overall cost of the procedure and the avoidance of potential complications.
Our heterotopic hind limb transplants instantly produced circulating donor-derived bone marrow cells as evidenced by male donor derived SRY quantitative PCR analysis. Additionally, the viability of the bone marrow component of the allograft in our longterm survivors was confirmed using immunohistochemistry. This further improves reliability of our model as an investigative tool for unique immune privileged features of vascularized bone marrow, which is a key component of certain reconstructive transplants. This osteomyocutaneous flap also contains the knee joint with articular cartilage and a synovial membrane and serve as a reliable model to assess rejection of these specialized structures.
Despite the fact that this model seems to be ideal for translational studies investigating immunologic aspects of VCA and its components including skin, muscle, nerves, vessels and joints it still does not allow for the assessment of a functional outcome. Once the immunologic barrier is overcome, further modifications and/or additional translational models can be performed to investigate therapeutic strategies aimed at improving motor and sensory function of VCA.
Utilizing this model, our group demonstrated that high-dose bone marrow cell infusion combined with co-stimulatory blockade optimized induction therapy, reduced maintenance immunosuppression, and indefinitely prolonged graft survival16. Such targeted immunomodulatory protocols that combine bone marrow cell-based strategies and biologics might facilitate immune tolerance and eliminate the need for multidrug immunosuppression to maintain graft survival after VCA.
Disclosures
The authors have nothing to disclose.
Acknowledgements
We would like to acknowledge the following individuals for their contribution to this project: Kakali Sarkar, PhD, Joani Christensen, BS, Kate Buretta, BS, Nance Yuan, BS, William Lehao, MD, Johanna Grahammer, Georg Furtmüller, MD, Erin Rada MD, Mohammed Al-Rakan MD, Karim Sarhane MD, Saami Khalifian, BS, Mao Qi, MD, and Angelo Leto Barone MD, VCA Laboratory, Department of Plastic and Reconstructive Surgery, Johns Hopkins University School of Medicine, Janis Taube, MD, Mark Fischer, MD, Departments of Dermatology and Pathology, Johns Hopkins University School of Medicine, Sue Eller, Minimally Invasive Surgery Training Center, Johns Hopkins University School of Medicine and Cheng-Hung Lin, MD Chang Gung Memorial Hospital, Linkou, Taiwan.
Funding source: Armed Forces Institute of Regenerative Medicine (DoD W81XWH-08- 2-0032)
Materials
| Name of the Reagent | Company | Catalogue Number | Comments (optional) |
| REAGENTS | |||
| HTK | Custodial | N/A | |
| EQUIPMENT | |||
| Electric Pen Drive | Synthes, Westchester PA | 05.001.011 | Reciprocating saw |
| Vascular Coupling device | Synovis, Newtown PA | 21003B |
References
- Barth, R. N., Rodriguez, E. D., Mundinger, G. S., et al. Vascularized bone marrow-based immunosuppression inhibits rejection of vascularized composite allografts in nonhuman primates. Am. J. Transplant. 11 (7), 1407-1416 (2011).
- Brandacher, G., Gorantla, V. S., Schneeberger, S., et al. Hand/Forearm transplantation using a novel cell-based immunomodulatory protocol-experience with five patients. Am. J. Transplant. 11, 190 (2011).
- Brandacher, G., Grahammer, J., Sucher, R., Lee, W. P. Animal models for basic and translational research in reconstructive transplantation. Birth Defects Res. C Embryo Today. 96 (1), 39-50 (2012).
- Brandacher, G., Lee, W. P. Hand transplantation. Hand Clin. 27, xiii-xiv (2011).
- Hettiaratchy, S., Mendely, E., Randolph, M. A., et al. Tolerance to composite tissue allografts across a major histocompatibility barrier in miniature swine. Transplantation. 27, 514-521 (2004).
- Ibrahim, Z., Busch, J., Awwad, M., et al. Selected physiologic compatibilities and incompatibilities between human and porcine organ systems. Xenotransplantation. 13 (6), 488-499 (2005).
- Kirk, A. D. Crossing the bridge: large animal models in translational transplantation research. Immunol. Rev. 19, 176-196 (2003).
- Lee, W. P., Rubin, J. P., Cober, S., et al. Use of swine model in transplantation of vascularized skeletal tissue allografts. Transplant Proc. 30, 2743-2745 (1998).
- Mathes, D. W., Hwang, B., Graves, S. S., et al. Tolerance to vascularized composite allografts in canine mixed hematopoietic chimeras. Transplantation. 92 (12), 1301-1308 (2011).
- Mathes, D. W., Randolph, M. A., Solari, M. G., et al. Split tolerance to a composite tissue allotransplant in a swine model. Transplantation. 75 (1), 25-31 (2003).
- Mezrich, J. D., Haller, G. W., Arn, J. S., et al. Histocompatible miniature swine: an inbred largeanimal model. Transplantation. 75 (6), 904-907 (2003).
- Petruzzo, P., Lanzetta, M., Dubernard, J. M., et al. The International Registry on Hand and Composite Tissue Transplantation. Transplantation. 90, 1590-1594 (2010).
- Sucher, R., Lin, C., Zanoun, R., et al. Mouse hind limb transplantation: a new composite tissue allotransplantation model using nonsuture supermicrosurgery. Transplantation. 90, 1374-1380 (2010).
- Ustüner, E. T., Majzob, R. K., Ren, X., et al. Swine composite tissue allotransplant model for preclinical hand transplant studies. Microsurgery. 20, 400-406 (2000).
- Ustüner, E. T., Zdichavsky, M., Ren, X., et al. Long-term composite tissue allograft survival in a porcine model with cyclosporine/mycophenolate mofetil therapy. Transplantation. 661, 581-587 (1998).
- Wachtman, G. S., Wimmers, E. G., Gorantla, V. S., et al. Biologicals and donor bone marrow cells for targeted immunomodulation in vascularized composite allotransplantation: a translational trial in swine. Transplant Proc. 43, 3541-3544 (2011).

