Identification of Rare Antigen-Specific T Cells from Mouse Lungs with Peptide:Major Histocompatibility Complex Tetramers
Summary
We provide a detailed protocol for isolating and identifying rare antigen-specific T cell populations in mouse lungs through magnetic bead-based T cell enrichment and peptide:major histocompatibility complex (MHC) tetramers.
Abstract
The identification and characterization of antigen-specific T cells during health and disease remains a key to improving our understanding of immune pathophysiology. The technical challenges of tracking antigen-specific T cell populations within the endogenous T cell repertoire have been greatly advanced by the development of peptide:MHC tetramer reagents. These fluorescently labeled soluble multimers of MHC class I or class II molecules complexed to antigenic peptide epitopes bind directly to T cells with corresponding T cell receptor (TCR) specificity and can, therefore, identify antigen-specific T cell populations in their native state without a requirement for a functional response induced by ex vivo stimulation. For exceedingly rare populations, tetramer-bound T cells can be magnetically enriched to increase the sensitivity and reliability of detection.
As the investigation of tissue-resident T cell immunity deepens, there is a pressing need to identify antigen-specific T cells that traffic to and reside in nonlymphoid tissues. In this protocol, we present a detailed set of instructions for the isolation and characterization of antigen-specific T cells present within mouse lungs. This involves the isolation of T cells from digested lung tissue followed by a general T cell magnetic enrichment step and tetramer staining for flow cytometry analysis and sorting. The steps highlighted in this protocol utilize common techniques and readily available reagents, making it accessible for nearly any researcher engaged in mouse T cell immunology, and are highly adaptable for a variety of downstream analyses of any low frequency antigen-specific T cell population residing within the lungs.
Introduction
At the heart of the adaptive immune system lies the ability of a T cell to recognize and respond to a specific antigen. When and where a T cell responds to its cognate antigen determines the balance of infection and autoimmunity, homeostasis and cancer, health and disease1. It follows that the study of T cells in a specific context of immunity should focus on the cells with specificity for a relevant antigen of interest. Among the technological advancements that have greatly enhanced the ability to characterize antigen-specific T cell populations are fluorescently labeled soluble multimers (usually tetramers) of major histocompatibility complex (MHC) class I or class II molecules complexed to antigenic peptide epitopes, better known as "peptide:MHC tetramers"2,3,4,5. By representing the natural ligands of T cell antigen receptors (TCRs), peptide:MHC class I and class II tetramers provide a means to directly identify antigen-specific CD8+ and CD4+ T cells, respectively, within the endogenous repertoire of T cells in the immune system without a requirement for a response to antigen stimulation in an assay. Tetramers represent a more elegant approach to the study of antigen-specific T cells than TCR transgenic T cell adoptive transfer models6, and have been increasingly used to identify foreign and self antigen-specific T cell populations in both experimental mouse models and human disease4,5.
While tetramers can readily identify high-frequency populations of T cells that have expanded in response to antigen stimulation, their use for naive, self antigen-specific, or memory T cells is limited by the very low frequencies of these populations7. Our group and others have developed and popularized tetramer-based magnetic enrichment strategies that increase the sensitivity of detection to enable studies of these cell populations in mouse lymphoid tissues8,9,10,11.
The emergence of tissue-resident T cells in the field has placed a heightened emphasis on developing new ways to investigate T cells in the nonlymphoid space. Like many other mucosal surfaces, T cells in the lungs encounter a range of self and foreign antigens derived from host epithelium, commensal and infectious microbes, and environmental entities, including allergens. Transcriptional analysis of T cells harvested from nonlymphoid tissue (NLT) demonstrates a memory-like phenotype that bears unique tissue-specific fate and function, often directed at trafficking and tissue homeostasis12. Moreover, tissue-resident memory T cells (Trms) tend to be more clonally restricted than those in circulation13. Determining how and why antigens drive T cell residence in NLT is critical to understanding how the immune system protects against infection, maintains tissue homeostasis, and, at times, devolves into autoimmunity. However, there appears to be greater attrition amongst tissue-resident T cells from the lungs compared to other NLT14. Accordingly, the ability to identify and characterize endogenous T cells of the lung with a given antigen-specificity is limited by their inherent rarity.
By combining the use of magnetic bead-based cell enrichment techniques and peptide:MHC tetramer staining, we have succeeded in detecting expanded but rare self antigen-specific T cells in mouse lungs15,16. Here, we present a detailed description of a protocol that we have optimized to reliably isolate and characterize any rare antigen-specific T cell population present in mouse lungs (Figure 1). This protocol incorporates an in vivo antibody staining step to distinguish tissue-resident from vascular T cells17 followed by two different methods for lung tissue processing to accommodate resource availability. This is then followed by a general T cell magnetic enrichment step, tetramer staining, and analysis by flow cytometry. Cell viability and tetramer staining is further enhanced in this protocol by the addition of aminoguanidine, which blocks inducible nitric oxide synthase (iNOS)-mediated T cell activation-induced apoptosis18 and Dasatinib which limits TCR downregulation19. The steps highlighted in this protocol utilize common techniques and readily available reagents, making it accessible for nearly any researcher engaged in mouse T cell immunology and is highly adaptable for a variety of downstream analyses. Although naive T cells are not likely to be found in the lungs, we believe this protocol will be particularly helpful for the study of self antigen-specific T cells and Trms in the lungs.
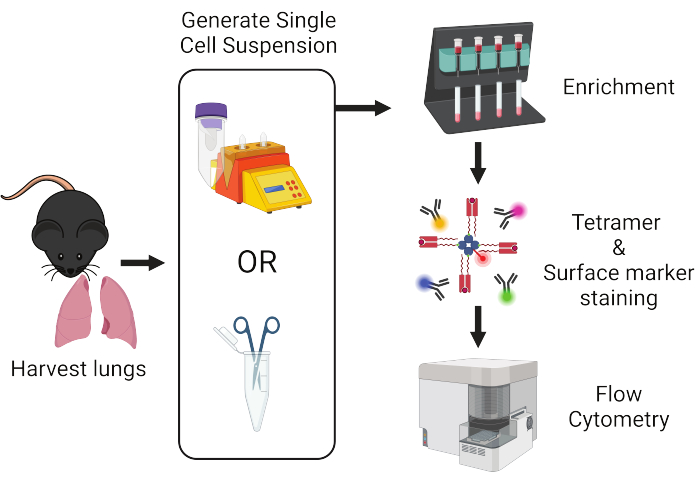
Figure 1: Overview of protocol workflow. Lungs are harvested from mice and dissociated into single cells. Samples are subsequently enriched for T cells prior to staining with peptide:MHC tetramers and fluorescently-labeled antibodies for flow cytometric analysis. Please click here to view a larger version of this figure.
Protocol
Representative Results
Discussion
Prior characterizations of antigen-specific T cells from the lungs have benefitted from the robust numbers of antigen-specific T cells that expand following an acute priming event such as intranasal immunization or infection20,21,22. However, rarer T cell populations in the lungs, such as self antigen-specific T cells or tissue-resident memory T cells, are difficult to detect without some form of sample enrichment for the T cell…
Disclosures
The authors have nothing to disclose.
Acknowledgements
We thank L. Kuhn for technical assistance with tissue processing and tetramer production. This work was funded by the National Institutes of Health (R01 AI107020 and P01 AI165072 to J.J.M., T32 AI007512 to D.S.S.), the Massachusetts Consortium on Pathogen Readiness (J.J.M), and the Massachusetts General Hospital Executive Committee on Research (J.J.M.).
Materials
| 100 mm cell strainer | Fisher Scientific | 22-363-549 | |
| 10x PBS without Ca++ or Mg++ | Corning | 46-013-CM | |
| 1x PBS without Ca++ or Mg++ | Corning | 21-031-CV | |
| AccuCheck Counting Beads | Invitrogen | PCB100 | |
| Aminoguanidine Hemisulfate Salt | Sigma-Aldrich | A7009 | |
| CD90.2 microbeads, mouse | Miltenyi | 130-121-278 | |
| Cell separation magnet (MidiMACS Separator) | Miltenyi | 130-042-302 | Holds single LS column |
| Cell separation magnet (QuadroMACS Separator) | Miltenyi | 130-090-976 | Holds 4 LS columns |
| Dasatinib | Sigma-Aldrich | CDS023389 | |
| DNase I | Roche | 10104159001 | |
| Eagle’s Ham’s Amino Acids medium | Sigma-Aldrich | C5572 | |
| gentleMACS | Miltenyi | 130-093-235 | Automated tissue dissociator |
| gentleMACS C Tubes | Miltenyi | 130-093-237 | Automated tissue dissociator tubes |
| Hank's Balanced Salt Solution with Ca++ or Mg++ | Corning | 21-020-CM | |
| HEPES | Gibco | 15630080 | |
| Ketamine | Vedco | NDC 50989-996-06 | |
| Liberase TM | Roche | 5401119001 | |
| Pacific Blue anti-mouse CD45 antibody (Clone: 30-F11) | Biolegend | 103126 | |
| Paramagnetic cell separation columns (LS Columns) | Miltenyi | 130-042-401 | Comes with plunger |
| Purified anti mouse CD16/32 antibody (Clone: 93) | Biolegend | 101302 | |
| RPMI 1640 medium without L-glutamine | Corning | 15-040-CM | |
| Sodium Chloride 0.9% (Normal Saline) | Cytiva | Z1376 | |
| Xylazine | Pivetal | NDC 466066-750-02 |
References
- Sun, L., Su, Y., Jiao, A., Wang, X., Zhang, B. T cells in health and disease. Signal Transduct Target Ther. 8 (1), 235 (2023).
- Altman, J. D., et al. Phenotypic analysis of antigen-specific T lymphocytes. Science. 274 (5284), 94-96 (1996).
- Crawford, F., Kozono, H., White, J., Marrack, P., Kappler, J. Detection of antigen-specific T cells with multivalent soluble class II MHC covalent peptide complexes. Immunity. 8 (6), 675-682 (1998).
- Nepom, G. T., et al. HLA class II tetramers: tools for direct analysis of antigen-specific CD4 + T cells. Arthritis Rheum. 46 (1), 5-12 (2002).
- Davis, M. M., Altman, J. D., Newell, E. W. Interrogating the repertoire: broadening the scope of peptide-MHC multimer analysis. Nat Rev Immunol. 11 (8), 551-558 (2011).
- Moon, J. J., et al. Tracking epitope-specific T cells. Nat Protoc. 4 (4), 565-581 (2009).
- Jenkins, M. K., Moon, J. J. The role of naive T cell precursor frequency and recruitment in dictating immune response magnitude. J Immunol. 188 (9), 4135-4140 (2012).
- Moon, J. J., et al. Naive CD4(+) T cell frequency varies for different epitopes and predicts repertoire diversity and response magnitude. Immunity. 27 (2), 203-213 (2007).
- Obar, J. J., Khanna, K. M., Lefrancois, L. Endogenous naive CD8+ T cell precursor frequency regulates primary and memory responses to infection. Immunity. 28 (6), 859-869 (2008).
- Kotturi, M. F., et al. Naive precursor frequencies and MHC binding rather than the degree of epitope diversity shape CD8+ T cell immunodominance. J Immunol. 181 (3), 2124-2133 (2008).
- Legoux, F. P., Moon, J. J. Peptide:MHC tetramer-based enrichment of epitope-specific T cells. J Vis Exp. 68, 4420 (2012).
- Szabo, P. A., Miron, M., Farber, D. L. Location, location, location: Tissue resident memory T cells in mice and humans. Sci Immunol. 4 (34), eaas9673 (2019).
- Poon, M. M. L., et al. Tissue adaptation and clonal segregation of human memory T cells in barrier sites. Nat Immunol. 24 (2), 309-319 (2023).
- Wakim, M. Z. M., Zheng, L. M. Tissue resident memory T cells in the respiratory tract. Mucosal Immunol. 15 (3), 379-388 (2022).
- Legoux, F. P., et al. CD4+ T cell tolerance to tissue-restricted self antigens is mediated by antigen-specific regulatory T Cells rather than deletion. Immunity. 43 (5), 896-908 (2015).
- Shin, D. S., et al. Lung injury induces a polarized immune response by self-antigen-specific CD4(+) Foxp3(+) regulatory T cells. Cell Rep. 42 (8), 112839 (2023).
- Anderson, K. G., et al. Intravascular staining for discrimination of vascular and tissue leukocytes. Nat Protoc. 9 (1), 209-222 (2014).
- Vig, M., et al. Inducible nitric oxide synthase in T cells regulates T cell death and immune memory. J Clin Invest. 113 (12), 1734-1742 (2004).
- Lissina, A., et al. Protein kinase inhibitors substantially improve the physical detection of T-cells with peptide-MHC tetramers. J Immunol Methods. 340 (1), 11-24 (2009).
- Hogan, R. J., et al. Protection from respiratory virus infections can be mediated by antigen-specific CD4(+) T cells that persist in the lungs. J Exp Med. 193 (8), 981-986 (2001).
- Hogan, R. J., et al. Activated antigen-specific CD8+ T cells persist in the lungs following recovery from respiratory virus infections. J Immunol. 166 (3), 1813-1822 (2001).
- Zhao, J., et al. Airway memory CD4(+) T cells mediate protective immunity against emerging respiratory coronaviruses. Immunity. 44 (6), 1379-1391 (2016).
- Hondowicz, B. D., et al. Interleukin-2-dependent allergen-specific tissue-resident memory cells drive asthma. Immunity. 44 (1), 155-166 (2016).
- Jungblut, M., Oeltze, K., Zehnter, I., Hasselmann, D., Bosio, A. Standardized preparation of single-cell suspensions from mouse lung tissue using the gentleMACS Dissociator. J Vis Exp. 29, 1266 (2009).
- Faustino, L. D., et al. Interleukin-33 activates regulatory T cells to suppress innate gammadelta T cell responses in the lung. Nat Immunol. 21 (11), 1371-1383 (2020).
- Atif, S. M., Gibbings, S. L., Jakubzick, C. V. Isolation and identification of interstitial macrophages from the lungs using different digestion enzymes and staining strategies. Methods Mol Biol. 1784, 69-76 (2018).
- Pape, K. A., Taylor, J. J., Maul, R. W., Gearhart, P. J., Jenkins, M. K. Different B cell populations mediate early and late memory during an endogenous immune response. Science. 331 (6021), 1203-1207 (2011).
- Naeher, D., et al. A constant affinity threshold for T cell tolerance. J Exp Med. 204 (11), 2553-2559 (2007).
- Moon, J. J., et al. Quantitative impact of thymic selection on Foxp3+ and Foxp3- subsets of self-peptide/MHC class II-specific CD4+ T cells. Proc Natl Acad Sci U S A. 108 (35), 14602-14607 (2011).
- Koehli, S., Naeher, D., Galati-Fournier, V., Zehn, D., Palmer, E. Optimal T-cell receptor affinity for inducing autoimmunity. Proc Natl Acad Sci U S A. 111 (48), 17248-17253 (2014).
- Zhang, Z., Legoux, F. P., Vaughan, S. W., Moon, J. J. Opposing peripheral fates of tissue-restricted self antigen-specific conventional and regulatory CD4(+) T cells. Eur J Immunol. 50 (1), 63-72 (2020).

.
