Assessment of Acute Wound Healing using the Dorsal Subcutaneous Polyvinyl Alcohol Sponge Implantation and Excisional Tail Skin Wound Models.
Summary
Here, two murine wound healing models are described, one designed to assess cellular and cytokine wound healing responses and the other to quantify the rate of wound closure. These methods can be used with complex disease models such as diabetes to determine mechanisms of various aspects of poor wound healing.
Abstract
Wound healing is a complex process that requires the orderly progression of inflammation, granulation tissue formation, fibrosis, and resolution. Murine models provide valuable mechanistic insight into these processes; however, no single model fully addresses all aspects of the wound healing response. Instead, it is ideal to use multiple models to address the different aspects of wound healing. Here, two different methods that address diverse aspects of the wound healing response are described. In the first model, polyvinyl alcohol sponges are subcutaneously implanted along the mouse dorsum. Following sponge retrieval, cells can be isolated by mechanical disruption, and fluids can be extracted by centrifugation, thus allowing for a detailed characterization of cellular and cytokine responses in the acute wound environment. A limitation of this model is the inability to assess the rate of wound closure. For this, a tail skin excision model is utilized. In this model, a 10 mm x 3 mm rectangular piece of tail skin is excised along the dorsal surface, near the base of the tail. This model can be easily photographed for planimetric analysis to determine healing rates and can be excised for histological analysis. Both described methods can be utilized in genetically altered mouse strains, or in conjunction with models of comorbid conditions, such as diabetes, aging, or secondary infection, in order to elucidate wound healing mechanisms.
Introduction
There are many murine model systems available to examine wound healing processes, each possessing specific advantages and limitations1,2. The following methods present two murine wound models, each of which addresses a particular aspect of the wound healing response, and which can be used to identify the cause and effect of perturbations in the response to injury. The process of wound healing occurs in distinct phases. The first phase is inflammatory, characterized by the rapid influx of platelets, neutrophils, and monocytes/macrophages, as well as the production of proinflammatory cytokines and chemokines. Following resolution of inflammation, the environment transitions to a more reparative state with the induction of profibrotic and proangiogenic cytokines and growth factors. Granulation tissue is deposited and neovessels form with the migration of myofibroblasts, fibroblasts, epithelial cells, and endothelial cells. In the final stages, the provisional extracellular matrix is remodeled, and scar formation and wound closure proceeds2,3,4,5,6,7,8.
No single murine model provides a system to study all stages of wound healing2. Here, two surgical wound models are described: one elucidates acute cellular and cytokine wound healing responses, and the other allows for the assessment of wound closure as well as histological analyses. These two methods may be employed in a complementary fashion to assess the effects of a perturbation or comorbidity on different aspects of the wound healing response. The dorsal subcutaneous implantation of polyvinyl alcohol (PVA) sponges is a system that has been used in rodent models for decades to elucidate numerous aspects of cellular and granulation tissue responses9,10,11,12,13,14,15,16,17,18,19,20,21,22,23,24. This approach allows for the retrieval of cytokine-rich wound fluids and cellular infiltrates. In this model, 1 cm x 1 cm x 0.5 cm pieces of PVA sponge are placed into subcutaneous pockets through a 2 cm incision made at the posterior dorsal midline. The incision is closed with surgical clips, and the sponges can be retrieved at later time points for cell and fluid isolation. The cellular and cytokine milieu of isolated sponges reflects the normal stages of acute wound healing up to about 14 days postimplantation. At later time points the model is more advantageous for studying granulation tissue formation and the foreign body response1. With this system, it is possible to isolate >106 cells, which offers a distinct advantage for phenotypic and functional assays and RNA isolation, over isolating cells from other biopsy-based methods1,22,23,25,26.
The rate of wound closure is determined using the tail skin excision model. In this model, as initially described by Falanga et al. and reported by others27,28,29,30, a 1 cm x 0.3 cm full thickness section of tail skin is removed near the base of the tail. The wound area is easily visualized and can be measured over time. Alternatively, tail tissue can be isolated for histological analysis. This approach can be used as an alternative to or in conjunction with the well-established dorsal punch biopsy method. The primary distinctions between these two models are the rate of wound closure, the presence or absence of fur, and the skin structure2,31,32. Tail skin wounds offer a longer timeframe in which to assess wound closure, as it takes approximately 21 days for full closure to occur. This is opposed to unsplinted dorsal punch biopsies, which heal much faster (~7–10 days), primarily by contraction due to the action of the panniculus carnosus. Splinted dorsal punch biopsies heal more slowly and diminish the effects of contractile healing, but rely on the presence of a foreign body to restrict contractile-based mechanisms1,2,27,30,31,33.
The described wound models are informative for understanding normal wound healing processes in the absence of perturbation. While the healing of rodent skin differs in very significant ways from human skin, including loose structure, reliance on contractile healing, and other anatomical differences, the murine system offers certain advantages for mechanistic and screening studies. Foremost among these is the availability of inbred strains and genetic mutants, genetic tractability, and lower cost. Mechanistic insight gained from murine studies can be translated to complex animal models that more closely mimic human skin healing, such as the porcine system2,31.
In addition to examining wound healing responses in the steady state, these models can be combined with comorbid conditions to understand the basis of wound healing defects at the cellular, cytokine, and gross tissue level. It is in this particular setting that the two models can be used in concert to assess the effects of a particular comorbid condition, such as postoperative pneumonia, on both the acute cellular wound healing response and the rate of wound closure30.
Protocol
All animal studies described here were approved by the Brown University Institutional Animal Care and Use Committee and carried out in accordance with the Guide for the Care and Use of Animals of the National Institutes of Health. NOTE: in the video, the surgical drape has been omitted for demonstration purposes.
1. Subcutaneous implantation of PVA sponges
- Use scissors to cut sheets of PVA sponge into 8 mm x 8 mm x 4 mm pieces. Rehydrate the pieces of PVA sponge by submerging them in sterile 1x PBS in a beaker.
- Autoclave the sponges in 1x PBS to sterilize, and cool completely. Store autoclaved sponges in sterile 1x PBS at 4 °C.
- Prior to performing surgical implantation, aliquot the necessary number of sponges into a sterile culture dish under sterile conditions in a laminar flow hood. Store the extra sponges in sterile 1x PBS at 4 °C for future use. Ensure that the sponges swell to 1 cm x 1 cm x 0.5 cm after rehydration. An image of dehydrated PVA sponges is shown in Figure 1A.
NOTE: To maintain the sterility of the surgical site, the PVA sponge implantation procedure requires one individual to handle the mouse and prepare the surgical site, and a second person to perform the implantation. - Anesthetize an 8–12 week-old male C57BL/6J mouse by intraperitoneal injection of 80 mg/kg ketamine. Administer 40 mg/kg of xylazine intraperitoneally for analgesia. Confirm the depth of anesthesia by the loss of a pedal reflex. Prepare the surgical site by removing the hair along the dorsum with clippers. Using sterile gauze, apply povidone-iodine solution to the shave area 2x, followed by 70% ethanol.
- Place the mouse on sterile surgical drapes. Place a heated pad below the surgical drapes to maintain the mouse’s core temperature.
- Wear sterile surgical gloves for performing the surgery. Pull the dorsal skin away from the underlying tissue with forceps, and using sterile surgical scissors, make a 2 cm incision along the dorsal midline approximately 2 cm anterior to the base of the tail. While holding the incision open with sterile forceps, use sterile curved, blunt-tipped surgical scissors to form a subcutaneous pocket along the dorsum in one of the positions indicated in Figure 1B.
- Continue to use forceps to lift the skin away from the underlying tissue. Using sterile surgical scissors, gently squeeze one PVA sponge in the culture dish to remove excess PBS. Pick up the PVA sponge by one corner using sterile surgical scissors and, leading with the corner held by the scissors, place the sponge into the subcutaneous pocket formed in step 1.4.
- Repeat this process 5x, placing a total of six sponges into subcutaneous pockets as shown in Figure 1B.
- Pinch the incised dorsal skin together with sterile forceps and close the incision with two stainless steel wound clips.
- Use a new set of sterile surgical instruments for each mouse. Alternatively, use a bead sterilizer to sterilize instruments between mice.
2. Isolation of fluids from PVA sponges
- To assess the acute wound cytokine milieu, isolate sponges between 1–14 days postimplantation.
- Prepare a fluid collection tube by nesting the barrel of a 5 mL syringe into a 16 mL culture tube.
- Euthanize a mouse with implanted PVA sponges by CO2 asphyxiation followed by cervical dislocation.
- Remove the surgical staples and open the incision with toothed forceps. Use scissors to extend the incision along the dorsal midline.
- Using forceps, extract one sponge from its subcutaneous pocket and transfer it to the prepared syringe barrel, being careful to minimize pressure to the sponge. Disassociate any connective tissue that remains adhered to the surface of the sponge. Use scissors to dissect the sponge from the surrounding tissue if necessary. Repeat the sponge removal process with the remaining sponges. Place the tube containing the sponges on ice.
- To isolate the wound fluid, centrifuge the culture tube containing the 5 mL syringe with the sponges at 700 x g for 10 min.
- After the centrifugation, discard the syringe and the sponges. The wound fluid will have collected in the 16 mL culture tube. A representative image of fluid collected from a day 7 wound is shown in Figure 1D. Transfer the wound fluid to a clean tube for long-term storage at -80 °C.
3. Isolation of cells from PVA sponges
- To assess the acute wound healing cellular milieu, collect sponges between 1–14-days post-sponge implantation. Sponges obtained from a wound 7 days after implantation are shown in Figure 1E.
- Prepare collection medium containing 1x HBSS (+calcium/+magnesium/–phenol red) supplemented with 1% FBS, 1% HEPES, and 1% penicillin-streptomycin.
- Aliquot 5 mL of HBSS collection medium into a 15 mL conical tube.
- Extract the PVA sponges from euthanized mice as described in 2.2–2.4. Place the sponges into the conical tube containing 5 mL of HBSS collection medium.
- Transfer the sponges and the HBSS collection medium to an 80 mL blender bag by pouring. Hang the blender bag from the hatch of the paddle blender, positioned so that the paddles strike the sponges and media. Adjust the settings of the paddle blender to run on high for 60 s. Press start.
- Transfer the media from the blender bag back to the 15 mL conical tube with a pipette, leaving the sponges behind in the bag. Squeeze the sponges to thoroughly release the media. Adjust the settings of the paddle blender to run for 30 s on high. Add 5 mL of media to the blender bag and repeat the stomaching process 2x for a total of three sponge washes.
- Centrifuge the conical tube at 250 x g for 5 min. A red pellet of cells and red blood cells will be visible at the bottom of the conical tube after centrifugation.
- Discard the supernatant and perform a red blood cell lysis: add 900 μL of dH2O to the cell pellet and pipette to mix. Neutralize with 100 μL of 10x PBS. Add 4 mL of 1x PBS to the tube to fully neutralize the lysis, then centrifuge at 250 x g for 5 min.
NOTE: The lysis step should be brief; leaving the water in contact with the cells for more than 3–5 s could result in lysis of non-red blood cells. - After centrifugation, a white cell pellet containing wound cells devoid of red blood cells will be present at the bottom of the conical tube. Discard the supernatant and resuspend the cell pellet in the desired medium for downstream analyses.
4. Optional flow cytometry analysis of innate leukocytes isolated from PVA sponge wounds
- Resuspend 0.5–1 x 106 wound cells in 25 μL of a 2x solution of blocking antibody containing 10 μg/mL anti-CD16/CD32 FcRγII/III antibody diluted in 1x PBS + 1% BSA.
NOTE: All antibodies should be titrated to determine optimal concentrations for flow cytometry analysis. - Incubate the cells with blocking antibody for 10 min on ice.
- Make a 2x master mix of antibodies containing 2.5 mg/mL of PerCP-eFluor710-Ly6G, 5 mg/mL of FITC-Ly6C, APC-Fire750-CD45.2, APC-R700-Siglec-F, and 10 mg/mL of eFluor660-F4-80 diluted in 1x PBS + 1% BSA. Directly add 25 μL of the antibody cocktail to the cells incubating in blocking antibody.
- Incubate the cells for 20 min on ice, protected from light.
- Wash the cells 2x with 1x PBS.
- Make a master mix of amine-reactive fixable viability dye-eFluor506 diluted 1:1,000 in 1x PBS. Resuspend the cell pellet in 50 μL of the viability dye solution.
NOTE: Serum must be excluded from the fixable viability step, as it will prevent binding of the dye to endogenous proteins. Incubate the cells for 20 min on ice, protected from light. - Wash the cells 2x with 1x PBS. Resuspend the cell pellet in 50 μL of 1% paraformaldehyde.
- Incubate the cells with 1% paraformaldehyde for 15 min on ice, protected from light.
- Wash the cells 1x with 1x PBS and resuspend the pellet in 1x PBS for flow cytometric analysis.
5. Tail skin excision
- Anesthetize an 8–12 week-old male C57BL/6J mouse by intraperitoneal injection of 80 mg/kg of ketamine. Administer 40 mg/kg of xylazine intraperitoneally for analgesia. Confirm the depth of anesthesia by the loss of a pedal reflex.
- Prepare the surgical site on the tail of the anesthetized mouse by using sterile gauze to apply povidone-iodine solution 2x, followed by one application of 70% ethanol.
- Define a 10 mm x 3 mm section on the dorsal surface of the tail, 10 mm from the base of the tail (Figure 1C) using a permanent marker to trace from a premade template.
- Place the anesthetized mouse on sterile surgical drapes.
- Wear sterile surgical gloves to perform the surgical procedures. With a sterile scalpel blade, make a full thickness incision along the right, bottom, and left edges of the wound area.
- Using sterile forceps, peel the excised skin away from the tail, and use sterile surgical scissors to cut away the top edge of the wound area.
- Apply pressure with sterile gauze to stop bleeding.
- Apply a spray barrier film to the wound bed.
- Photograph the wounds from a fixed distance at regular time intervals. Analyze photographs by planimetric analysis to determine wound area measurements. Alternatively, use calipers to obtain wound length and width measurements.
Representative Results
Systemic inflammatory response following PVA sponge implantation
The PVA sponge implantation surgery generated a systemic inflammatory response, as demonstrated by the induction of IL-6 in the plasma 1 day after wounding (Figure 2A). Other proinflammatory cytokines including TNF-α and IL-1β, as well as an array of chemokines including CCL2 and CXCL1 were induced systemically in the first 7 days post-PVA sponge implantation, and have been described elsewhere26,30.
Isolation of cells and fluids from PVA sponge wounds
The primary advantage of the PVA sponge wound model is the ability to recover enough cells for phenotypic and functional analyses of the acute cellular wound healing response. The number of cells that can be recovered from PVA sponge wounds increases over time, from approximately 2 x 106 cells per six sponges on wound day 1 x 106 to 8 x 106 cells on wound day 7 (Figure 2B). The cell number continues to increase beyond day 7. It is not recommended to continue this model beyond ~14 days because the sponges become fully encapsulated by collagen and the system transitions from modeling an acute wound healing response to modeling a foreign body granuloma1,22,23,25,26. Neutrophils, monocytes, and macrophages were the primary cellular infiltrate in PVA sponge wounds. Neutrophils predominated the wound cellular milieu one day after wounding, as assessed by flow cytometric analysis (Figure 2C). Monocytes and monocyte-derived macrophages accumulated within 3 days post-sponge implantation, and the three cell populations increased in number over time (Figure 2C). A representative flow cytometry gating strategy to identify neutrophil, monocyte, and macrophage populations is shown in Figure 2D. After excluding cell doublets using FSC-H and SSC-H parameters (Figure 2D, i and ii), non-viable cells were excluded using an amine-reactive fixable viability dye (shown here) or a nucleic acid dye (e.g., sytox or propidium iodide) (Figure 2D, iii). Residual cellular debris not removed by the prior gating steps was then excluded using FSC-A and SSC-A parameters (Figure 2D, iv). Hematopoietic cells comprised the majority of PVA sponge wound cells and were identified by CD45 expression (Figure 2D, v). Neutrophils were identified as Ly6G+Siglec-F– (Figure 2D, vi). Siglec-F+ cells were primarily eosinophils (Figure 2D, vii). Gating on Ly6G–Siglec-F– cells, monocytes/macrophages were identified as F4/80+ cells (Figure 2D, viii). F4/80+ cells could be further fractionated by Ly6C expression to distinguish Ly6Chi inflammatory monocytes (Figure 2D, ix) and Ly6Clow monocyte-derived macrophages (Figure 2D, x)26.
The ability to measure cytokines and other wound soluble factors is another advantage to the PVA sponge wound model. It is possible to extract up to 100 μL of fluid per sponge. Extracted fluids are suitable for a variety of downstream assays. The detection of cytokines and chemokines in early and late wound fluids by ELISA or bead-based multiplex immunoassays have been reported elsewhere26,30. It is possible to obtain both cells and fluids from the same wound. To do this, it is recommended to isolate three sponges from one side of the dorsal midline for cell isolation and 3 sponges from the opposite side of the dorsal midline for fluid extraction.
Assessment of wound closure using the tail skin excision model
The excisional tail skin model provides an alternative to the dorsal skin punch biopsy method to study slow wound closure in firm skin lacking dense fur. Example images of tail skin wounds at 1, 7, and 15 days post-excision are shown in Figure 3A. Wound closure could be quantified by measuring the area of the wound bed over time. The day 7 and day 15 wound bed areas were approximately 70% and 35%, respectively, of the day 1 wound area (Figure 3B). Full wound closure required approximately 28 days. The tail skin wound could also be observed in cross section by histological analysis. Figure 3C and Figure 3D show representative images of H&E and Masson’s Trichrome-stained tail cross sections, respectively. The lateral margins of the excised skin are indicated by arrowheads on the dorsal surface of the tail.
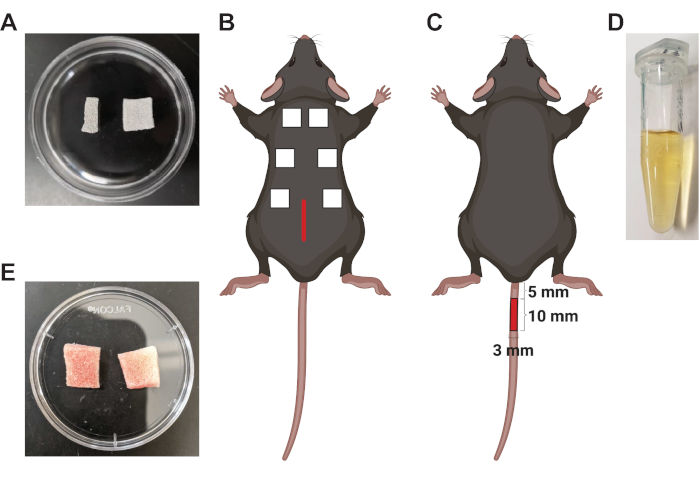
Figure 1: Schematic of murine wound healing models. (A) Side (left) and top (right) view of dehydrated PVA sponges measuring 8 mm x 8 mm x 0.4 mm. (B) Illustration of a mouse demonstrating the placement of the dorsal midline incision (central red line) and six 1 cm x 1 cm x 0.5 cm PVA sponges in subcutaneous pockets. (C) Schematic demonstrating the size and placement of an excisional skin wound (10 mm x 3 mm red rectangle) on the dorsal surface of the tail. (D) Wound fluid isolated from three sponges that were retrieved from the subcutaneous space 7 days after implantation. (E) The appearance of sponges retrieved from the wound 7 days after implantation. Please click here to view a larger version of this figure.
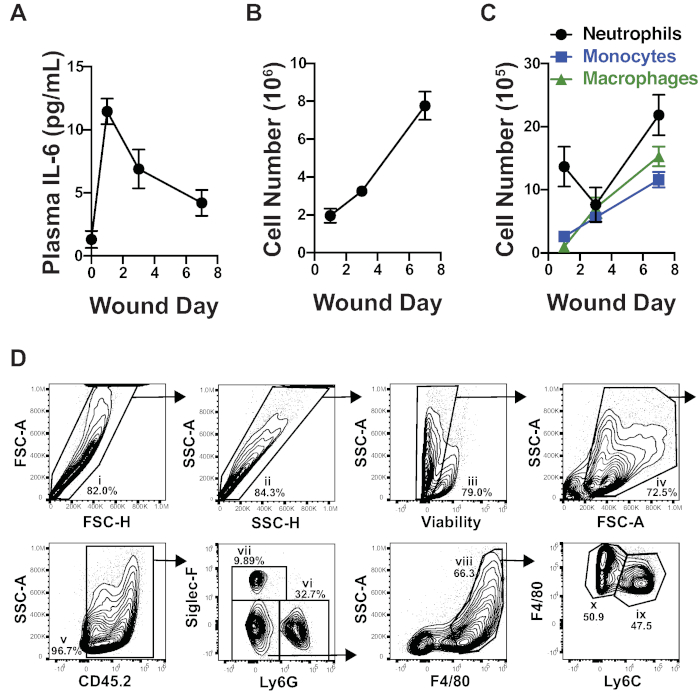
Figure 2: The systemic and cellular response to PVA sponge implantation. (A) A time course of IL-6 levels in the plasma demonstrates that PVA sponge implantation induced a systemic inflammatory response. The concentration of IL-6 was measured using a multiplex bead-based immunoassay. (B) The number of cells isolated from PVA sponges wound increased over time. (C) A time course demonstrates the accumulation of neutrophils, monocytes, and monocyte-derived macrophages in PVA sponge wounds over time. (D) A representative gating strategy of cells isolated from PVA sponge wounds demonstrates how to identify leukocyte subsets by flow cytometric analysis. Gates are defined as follows: (i and ii) doublet exclusion, (iii) dead cell exclusion using an amine-reactive fixable viability dye, (iv) debris exclusion by FSC-A and SSC-A, (v) CD45+ hematopoietic cells, (vi) Ly6G+ neutrophils, (vii) Siglec-F+ eosinophils, (viii) Ly6G–Siglec-F– F4/80+ monocytes/macrophages, (ix) F4/80+Ly6Chi monocytes, and (x) F4/80+Ly6Clow macrophages. Gates were placed according to fluorescence-minus one (FMO) controls. The data shown in A–C are the mean ± SEM, n = 6–10 mice per group in (A), n = 8–9 mice in (B), and n = 6–8 mice in (C). All data are combined from 2–3 independent experiments. Please click here to view a larger version of this figure.
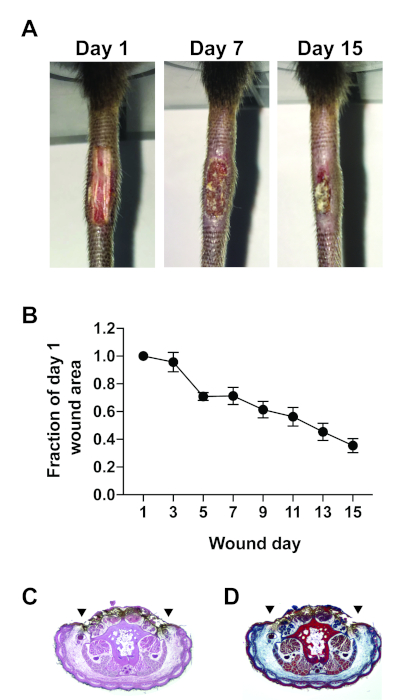
Figure 3: Assessment of excisional tail skin wound healing. (A) Representative photographs of excisional tail skin wounds taken 1, 7, and 15 days post-wounding. (B) The rate of closure of excisional tail skin wounds. Wounds were photographed every other day. Image processing software was used to trace the wound bed margins and calculate the wound area at indicated time points. The wound area is presented as a fraction of the wound area measured on day 1. Representative images of tail cross sections that were paraffin-embedded, sectioned, and stained with (C) H&E or (D) Masson’s Trichrome. The wound was located on the dorsal surface of the tail cross section; lateral wound margins are indicated by arrowheads. The data shown in (B) are the mean ± SEM, n = 8 mice per group. Data are combined from two independent experiments. Please click here to view a larger version of this figure.
Discussion
This article describes two tractable murine wound models that allow for the assessment of the acute wound healing response. The first method involves the surgical implantation of PVA sponges in the dorsal subcutaneous space. This approach offers a distinct advantage over biopsy-based wound models for studying the cellular wound healing response due to the large number of cells and quantity of wound fluids obtained from the isolated sponges. For the successful execution of this procedure, maintaining a sterile surgical field by thoroughly cleaning the skin around the incision is imperative, as translocation of bacteria into the wound will significantly alter the course of healing. Using the cell isolation method described here, it is possible to isolate at least 1–10 x 106 cells from the PVA sponges, depending on the time of sponge extraction. The majority of cells isolated from PVA sponge wounds are viable (Figure 2D). However, because it is possible for dead cells to constitute up to ~20% of isolated wound cells after mechanical disruption, it is highly recommended to use a viability stain when proceeding with flow cytometry-based analyses. Cells isolated from PVA sponge wounds are primarily of hematopoietic origin as determined by CD45 positivity (Figure 2D). The rapid accumulation of neutrophils followed by monocytes and macrophages is consistent with the acute stages of wound repair3,4,34,35,36,37,38. Isolated cells are suitable for downstream analyses including immunophenotyping, cell sorting, culturing, RNA extraction, and a variety of functional assays.
The PVA sponge wound model also allows for the isolation of fluids, which is ideal for assessing cytokine and growth factor responses in the acute wound environment. PVA sponge fluids are suitable for testing by ELISA, bead-based multiplex immunoassay, and protein quantitation, among others. Previous studies have demonstrated through cytokine and growth factor measurement that the early wound environment is inflammatory in nature, with rapid induction of IL-6, TNF-α, and IL-1β from days 1–3. The wound environment then transitions to a reparative state with the later induction of pro-angiogenic and pro-fibrotic growth factors, including VEGF and TGF-β22,23,25,26,30.
While the PVA sponge implantation model is advantageous for studying acute wound cellular and cytokine responses, one of its limitations is the inability to measure the rate or degree of healing. Measurement of this aspect of wound healing may be required when assessing the effects of a comorbid condition on various aspects of the wound healing response30. For this metric, biopsy-based methods are preferred. Here, the tail skin excision model is presented. In this model, a full thickness section of tail skin is excised from the dorsal surface of the tail. Again, maintaining a sterile surgical field is important to avoid inoculating the wound bed. The use of a spray barrier film or other wound covering is also recommended to avoid later wound infection. Older male mice or aggressive strains require solo housing to avoid disruption of the wound. A particular advantage of the tail as a site for studying wound healing is that it relies more on re-epithelialization for closure, as described by others27,32,33. In addition to measuring the wound bed area and performing histological analyses, others have reported its use in assessing the efficacy of topical interventions in modulating the healing processes33.
Each of the wound models described in these methods offer distinct advantages for understanding wound repair processes in the steady state and in the presence of comorbidities. Due to the wide availability of genetically altered strains of inbred mice, it is also possible to manipulate the wound healing responses to answer mechanistic questions about the process. Furthermore, these systems can be implemented in murine models of conditions associated with poor wound healing including diabetes, aging, secondary infection, and others30,36,39,40. The mechanistic insights gained from murine studies may then provide the basis for studying wound healing in higher order animal models. Together, the PVA sponge implantation and excisional tail skin wound models provide tractable and versatile systems to elucidate wound healing processes under steady state and pathological conditions.
Divulgations
The authors have nothing to disclose.
Acknowledgements
The authors would like to thank Kevin Carlson of the Brown University Flow Cytometry and Sorting Facility for consultation and assistance with flow cytometry experiments. Images in Figure 1B and C were created with BioRender. Kayla Lee and Gregory Serpa are thanked for their photographic assistance. This work was supported by grants from the following: Defense Advanced Research Projects Agency (DARPA) YFAA15 D15AP00100, Dean’s Areas of Emerging New Science Award (Brown University), National Heart Lung and Blood Institute (NHLBI) 1R01HL126887-01A1, National Institute of Environmental Science (NIES) T32-ES7272 (Training in Environmental Pathology), and the Brown University Research Seed Award.
Materials
| 10x Phosphate Buffered Saline | Fisher Scientific | BP3991 | |
| 15 mL centrifuge tubes, Olympus | Genesee | 28-103 | |
| 1x HBSS (+Calcium, +Magnesium, –Phenol Red) | ThermoFisher Scientific | 14025076 | |
| 5ml Syringe | BD | 309646 | |
| Anti-mouse CD45.2-APC Fire750 | BioLegend | 109852 | Clone 104 |
| Anti-mouse F4/80-eFluor660 | ThermoFisher Scientific | 50-4801-82 | Clone BM8 |
| Anti-mouse Ly6C-FITC | BD Biosciences | 553104 | Clone AL-21 |
| Anti-mouse Ly6G-PerCP-eFluor710 | ThermoFisher Scientific | 46-9668-82 | Clone 1A8-Ly6g |
| Anti-mouse Siglec-F-APC-R700 | BD Biosciences | 565183 | Clone E50-2440 |
| Autoclip Stainless Steel Wound Clip Applier | Braintree Scientific | NC9021392 | |
| Autoclip Stainless Steel Wound Clips, 9mm | Braintree Scientific | NC9334081 | |
| Blender Bag, 80mL | Fisher Scientific | 14258201 | |
| Culture Tube, 16mL, 17×100 | Genesee Scientific | 21-130 | |
| Fetal Bovine Serum – Standard | ThermoFisher Scientific | 10437028 | |
| Fixable Viability Dye eFluor506 | ThermoFisher Scientific | 65-0866-14 | |
| Hepes Solution, 1M | Genesee Scientific | 25-534 | |
| ImageJ Software | NIH | ||
| Penicillin-Streptomycin (5000 U/mL) | ThermoFisher Scientific | 15070-063 | |
| Polyvinyl alcohol sponge – large pore size | Ivalon/PVA Unlimited | www.sponge-pva.com | |
| Povidone-iodine solution, 10% | Fisher Scientific | 3955-16 | |
| Spray barrier film, Cavilon | 3M | 3346E | |
| Stomacher 80 Biomaster, 110V | Seward | 0080/000/AJ |
References
- Gottrup, F., Agren, M. S., Karlsmark, T. Models for use in wound healing research: a survey focusing on in vitro and in vivo adult soft tissue. Wound Repair and Regeneration: Official Publication of the Wound Healing Society [and] the European Tissue Repair Society. 8 (2), 83-96 (2000).
- Elliot, S., Wikramanayake, T. C., Jozic, I., Tomic-Canic, M. A Modeling Conundrum: Murine for Cutaneous Wound Healing. Journal of Investigative Dermatology. 138 (4), 736-740 (2018).
- Eming, S. A., Martin, P., Tomic-Canic, M. Wound repair and regeneration: Mechanisms, signaling, and translation. Science Translational Medicine. 6 (265), (2014).
- Huber-Lang, M., Lambris, J. D., Ward, P. A. Innate immune responses to trauma. Nature Immunology. 19 (4), 327-341 (2018).
- Novak, M. L., Koh, T. J. Phenotypic Transitions of Macrophages Orchestrate Tissue Repair. The American Journal of Pathology. 183 (5), 1352-1363 (2013).
- Martins-Green, M., Petreaca, M., Wang, L. Chemokines and Their Receptors Are Key Players in the Orchestra That Regulates Wound Healing. Advances in Wound Care. 2 (7), 327-347 (2013).
- Guerrero-Juarez, C. F., et al. Single-cell analysis reveals fibroblast heterogeneity and myeloid-derived adipocyte progenitors in murine skin wounds. Nature Communications. 10 (1), 650 (2019).
- Shook, B. A., et al. Myofibroblast proliferation and heterogeneity are supported by macrophages during skin repair. Science. 362 (6417), 2971 (2018).
- Davidson, J. M., et al. Accelerated wound repair, cell proliferation, and collagen accumulation are produced by a cartilage-derived growth factor. The Journal of Cell Biology. 100 (4), 1219-1227 (1985).
- Buckley, A., Davidson, J. M., Kamerath, C. D., Wolt, T. B., Woodward, S. C. Sustained release of epidermal growth factor accelerates wound repair. Proceedings of the National Academy of Sciences. 82 (21), 7340-7344 (1985).
- Peterson, J. M., Barbul, A., Breslin, R. J., Wasserkrug, H. L., Efron, G. Significance of T-lymphocytes in wound healing. Surgery. 102 (2), 300-305 (1987).
- Efron, J. E., Frankel, H. L., Lazarou, S. A., Wasserkrug, H. L., Barbul, A. Wound healing and T-lymphocytes. Journal of Surgical Research. 48 (5), 460-463 (1990).
- Schäffer, M. R., Tantry, U., Thornton, F. J., Barbul, A. Inhibition of nitric oxide synthesis in wounds: pharmacology and effect on accumulation of collagen in wounds in mice. The European Journal of Surgery = Acta Chirurgica. 165 (3), 262-267 (1999).
- Opalenik, S. R., Davidson, J. M. Fibroblast differentiation of bone marrow-derived cells during wound repair. FASEB Journal: Official Publication of the Federation of American Societies for Experimental Biology. 19 (11), 1561-1563 (2005).
- Järveläinen, H., et al. A role for decorin in cutaneous wound healing and angiogenesis. Wound Repair and Regeneration: Official Publication of the Wound Healing Society [and] the European Tissue Repair Society. 14 (4), 443-452 (2006).
- Luckett, L. R., Gallucci, R. M. Interleukin-6 (IL-6) modulates migration and matrix metalloproteinase function in dermal fibroblasts from IL-6KO mice. The British Journal of Dermatology. 156 (6), 1163-1171 (2007).
- Daniel, T., et al. Regulation of the postburn wound inflammatory response by gammadelta T-cells. Shock. 28 (3), 278-283 (2007).
- MacLauchlan, S., et al. Macrophage fusion, giant cell formation, and the foreign body response require matrix metalloproteinase 9. Journal of Leukocyte Biology. 85 (4), 617-626 (2009).
- Schwacha, M. G., Thobe, B. M., Daniel, T., Hubbard, W. J. Impact of thermal injury on wound infiltration and the dermal inflammatory response. Journal of Surgical Research. 158 (1), 112-120 (2010).
- Ganesh, K., et al. Prostaglandin E2 Induces Oncostatin M Expression in Human Chronic Wound Macrophages through Axl Receptor Tyrosine Kinase Pathway. The Journal of Immunology. 189 (5), 2563-2573 (2012).
- Deskins, D. L., et al. Human mesenchymal stromal cells: identifying assays to predict potency for therapeutic selection. Stem Cells Translational Medicine. 2 (2), 151-158 (2013).
- Daley, J. M., Brancato, S. K., Thomay, A. A., Reichner, J. S., Albina, J. E. The phenotype of murine wound macrophages. Journal of Leukocyte Biology. 87 (1), 59-67 (2010).
- Thomay, A. A., et al. Disruption of Interleukin-1 Signaling Improves the Quality of Wound Healing. The American Journal of Pathology. 174 (6), 2129-2136 (2009).
- Brancato, S. K., et al. Toll-like receptor 4 signaling regulates the acute local inflammatory response to injury and the fibrosis/neovascularization of sterile wounds. Wound Repair and Regeneration: Official Publication of the Wound Healing Society [and] the European Tissue Repair Society. 21 (4), 624-633 (2013).
- Daley, J. M., et al. Modulation of macrophage phenotype by soluble product(s) released from neutrophils. Journal of Immunology. 174 (4), 2265-2272 (2005).
- Crane, M. J., et al. The monocyte to macrophage transition in the murine sterile wound. PloS One. 9 (1), 86660 (2014).
- Falanga, V., et al. Full-thickness wounding of the mouse tail as a model for delayed wound healing: accelerated wound closure in Smad3 knock-out mice. Wound Repair and Regeneration. 12 (3), 320-326 (2004).
- Li, J., et al. Molecular mechanisms underlying skeletal growth arrest by cutaneous scarring. Bone. 66, 223-231 (2014).
- Zhou, S., et al. A Novel Model for Cutaneous Wound Healing and Scarring in the Rat. Plastic and Reconstructive Surgery. 143 (2), 468-477 (2019).
- Crane, M. J., et al. Pulmonary influenza A virus infection leads to suppression of the innate immune response to dermal injury. PLOS Pathogens. 14 (8), 1007212 (2018).
- Grada, A., Mervis, J., Falanga, V. Research Techniques Made Simple: Animal Models Healing. Journal of Investigative Dermatology. 138 (10), 2095-2105 (2018).
- Rittié, L. Cellular mechanisms of skin repair in humans and other mammals. Journal of Cell Communication and Signaling. 10 (2), 103-120 (2016).
- Falanga, V., et al. Autologous Bone Marrow-Derived Cultured Mesenchymal Stem Cells Delivered in a Fibrin Spray Accelerate Healing in Murine and Human Cutaneous Wounds. Tissue Engineering. 13 (6), 1299-1312 (2007).
- Lucas, T., et al. Differential Roles of Macrophages in Diverse Phases of Skin Repair. The Journal of Immunology. 184 (7), 3964-3977 (2010).
- Wang, J., et al. Visualizing the function and fate of neutrophils in sterile injury and repair. Science. 358 (6359), 111-116 (2017).
- Mirza, R. E., Koh, T. J. Contributions of cell subsets to cytokine production during normal and impaired wound healing. Cytokine. , 1-4 (2014).
- Mirza, R., DiPietro, L. A., Koh, T. J. Selective and Specific Macrophage Ablation Is Detrimental to Wound Healing in Mice. The American Journal of Pathology. 175 (6), 2454-2462 (2010).
- DiPietro, L. A., Burdick, M., Low, Q. E., Kunkel, S. L., Strieter, R. M. MIP-1alpha as a critical macrophage chemoattractant in murine wound repair. Journal of Clinical Investigation. 101 (8), 1693-1698 (1998).
- Wetzler, C., Kämpfer, H., Stallmeyer, B., Pfeilschifter, J., Frank, S. Large and Sustained Induction of Chemokines during Impaired Wound Healing in the Genetically Diabetic Mouse: Prolonged Persistence of Neutrophils and Macrophages during the Late Phase of Repair. Journal of Investigative Dermatology. 115 (2), 245-253 (2000).
- Kim, D. J., Mustoe, T., Clark, R. A. Cutaneous wound healing in aging small mammals: a systematic review. Wound Repair and Regeneration. 23 (3), 318-339 (2015).

