Isolation and Identification of Limbal Niche Cells
Summary
Here, we present a protocol to isolate and identify the human limbal niche cells.
Abstract
Here we report a standard procedure for the isolation and identification of limbal niche cells (LNCs). Limbus tissue obtained from an eye bank was used for LNCs isolation. The tissue was divided into 12 pieces under aseptic conditions and digested for 18 h at 37 °C in the cell culture incubator using collagenase A to obtain cell clusters with LNCs and limbal epithelial progenitor cells. The cell clusters were further digested for 15 min at 37 °C using 0.25% trypsin-EDTA to obtain single cells and then cultured in modified embryonic stem cell medium (MESCM) on a plastic surface coated with 5% Matrigel. Cells were passaged upon 70% confluence, and LNCs were identified using immunofluorescence, real-time quantitative PCR (qPCR), and flow cytometry. Primary LNCs were isolated and passaged more than 12 times. The proliferation activity of LNCs from P4 to P6 was the highest. LNCs expressed higher stem cell markers than BMMSCs (SCF, Nestin, Rex1, SSEA4, CD73, CD90, MSX1, P75NTR, and PDGFRβ). Furthermore, results showed that P4 LNCs uniformly expressed VIM, CD90, CD105, and PDGFRβ, but not Pan-CK, which could be used as a marker for the identification of LNCs. Flow cytometric analysis showed that approximately 95%, 97%, 92%, and 11% of LNCs expressed CD73, CD90, CD105, and SCF respectively, while they were 68%, 99%, 20%, and 3% in BMMSCs. The standard process for LNC isolation and identification could provide a reliable laboratory basis for the widespread use of LNCs.
Introduction
The incidence of corneal epithelial stem cell deficiency (CESD), also called limbal stem cells deficiency (LSCD)1, and corneal epithelial regeneration (CES) are becoming more and more urgent because of corneal infection and injury. If not properly treated, CESD can lead to blindness that requires corneal transplantation. As a result, CES regeneration is becoming more significant. There is a group of supportive cells called limbal niche cells (LNCs) that provide essential support for CES function. Limbal stromal stem cells were first isolated by Polisetty et al.2 and identified by Xie et al.3 as LNCs which are localized in the limbal epithelium subjacent and stroma of the limbus. LNCs are the key supporting stem cell of the corneal rim and, with the function of bone marrow-derived MSC (BMMSCs), and could be induced to develop into corneal epithelial cells and corneal stromal cells, etc.3,4,5,6,7. Previous studies showed that the stem-cell qualities of LNCs are more primitive than BMMSCs8, which is already widely used in the clinic. LNCs may even become the next viable option after MSC, especially for treating CESD. As important supporting cells for CES, LNCs are also stem cells derived from the "niche" structure of the limbus. LNCs may play a key role in the dedifferentiation of mature corneal epithelial cells (MCEC) to CES9. However, studies on LNCs are still relatively insufficient, and there is no consensus on the terminology, isolation, purification, identification, and characteristics of LNCs. Some researchers have named LNCs limbal biopsy-derived stromal stem cells10, limbal mesenchymal stem cells11, limbal fibroblast stem cells12, and limbal mesenchymal stromal cells13. As the growth characteristics of LNCs have not been described in detail, and because of their promising scientific and clinical applications, and may be one of the most important clinical tools in the future, it is necessary to summarize the isolation, purification, identification, and characteristics of LNCs.
According to a previous study14, LNCs are mainly present at the limbal epithelium subjacent and stroma of the limbus. This protocol includes treating limbus tissue using collagenase A, obtaining a cluster consisting of LEPC and LNCs, and digesting it into single cells with 0.25% trypsin-EDTA (TE). LNCs were then selectively cultured in a modified embryonic stem cell medium (MESCM) to be purified. The protocol reported in this paper is simple and has high efficiency in obtaining human LNCs in large quantities.
The detailed procedure of LNC isolation, culture, and identification was recorded in the video for scientists who are interested in LNC study, and it can be conveniently repeated when needed.
Protocol
Limbus tissue from donors aged between 50 and 60 years was obtained from the Red Cross Eye Bank, Tongji Hospital (Wuhan, China). The protocol was approved by the Tongji Ethics Committee and was conducted in accordance with the Declaration of Helsinki.
1. Isolation
- Obtain limbus tissue from intermediate-term corneal storage medium and operate under aseptic conditions on an ultra-clean workbench.
- Scrape and remove the iris and endothelium around the cornea using a sterile surgical round blade.
- Cut limbus tissue into twelve equally sized pieces with a surgical blade with 1 mm left on both sides of the cornea and sclera.
- Transfer limbus tissues to a 3.5 cm culture plate, add 1 mL of collagenase A (2 mg/mL, in DF-12 medium), to immerse all of the tissues for digestion.
- Put the plate into the 37 °C cell incubator, digest the limbal tissues for 18 h.
NOTE: Follow-up procedures are usually performed on the second day. - Prepare a 5% basement membrane matrix (Matrigel) coated 6-well culture plate.
- Coat 5% basement membrane matrix (dissolved in MESCM [Table 1]) at the bottom of the well.
- Prepare 200 μL and 1 mL tips, one 15-mL centrifugal tube, and one 6-well plate in a sterilized bag.
- Put the sterilized bag (including tips and centrifugal tube) and a new 6-well plate at -20 °C or -80 °C environment for 20 min. Thaw the basement membrane matrix in the refrigerator at 4 °C.
- Take out the pre-cooled tips, centrifugal tube, and 6-well plate from the -20 °C or -80 °C environment, and then perform the following operations on the ultra-clean workbench.
- Transfer 50 µL 5% basement membrane matrix to 1 mL MESCM using a 200 μL tip, and mix them gently and evenly.
- Transfer 5% basement membrane matrix (dissolved in MESCM) to one well of a 6-well culture plate using the pre-cooled 1 mL tip.
- Shake the 6-well plate gently and horizontally, put the 6-well culture plate in the 37 °C cell incubator for approximately 1 h, and then perform the next step.
- After 18-h digestion, take out collagenase A-digested limbal tissue, only some visible small clusters and undigested scleral tissues will remain.
NOTE: High-magnification microscopy reveals a cluster composed of many densely packed cells (including LNCs). - Use a 200 µL pipette tip to detach the clusters from undigested scleral tissues under the stereomicroscope.
- Transfer the clusters to the 3.5-cm culture plate and immerse them in 0.25% TE, and then place the plate in the cell incubator for 15 min.
- Add 1 mL MESCM with 10% knockout serum to stop cell digestion and gently pipette up and down to resuspend the clusters into individual cells using a 1-mL pipette tip.
- Transfer the cell suspension to a 15-mL centrifugal tube and centrifuge at 200 x g for 5 min.
- Remove the supernatant carefully without disturbing the cell precipitation, and then add 1 mL MESCM to resuspend the cells.
- Pipette up and down 2-3 times until the bottom cell precipitation is evenly suspended in the MESCM using 1 mL pipette tip, and take 20 µL cell suspension for cell counting.
- Transfer the cell suspension to the 5% basement membrane matrix-coated 6-well plate with a 1-mL pipette tip and increase the volume of MESCM to 2.5 mL.
- Gently shake the 6-well plate horizontally to evenly distribute the cells.
- Transfer the cells to the culture incubator after being imaged and recorded. Observe and photograph the cells daily, and change the medium every 3-4 days.
2. Identification of LNC
- Immunofluorescence staining
- Digest the LNCs from the bottom of the plate using 1 mL 0.25% TE for 5 min in the 37°C cell incubator.
- Terminate the digestion by adding 1 mL MESCM (containing knockout serum), centrifuge the cell suspension at 200 x g for 5 min, and aspirate the supernatant carefully.
- Add 1 mL MESCM to resuspend the cells in suspension. Prepare 80 µL cell suspension (4 × 103 cells per slide) for 4 slides (20 µL/slide) and use centrifuge system to deposit cells onto microscope slides as per the manufacturer's instructions.
- Fix cells (adhered to slides in step 3) using 4% paraformaldehyde for about 10 min, and then permeabilize cells on the slides with 0.2% Triton X-100 in PBS for 15 min.
- Block the cells for 1 h with 2% bovine serum albumin (BSA) before incubating them with primary antibodies (Pan-CK [1:1000], Vim [1:100], CD90 [1:100], CD105 [1:200], SCF [1:100], PDGFRβ [1:100]) on a shaker overnight at 4 °C. After the incubation, remove unbound primary antibodies by washing (5 min/wash, 3x) the slides with PBST (PBS + 0.1% Tween 20).
- Incubate the corresponding secondary antibodies (donkey anti-mouse IgG secondary antibody TRITC [1:1000], donkey anti-rabbit IgG FITC [1:500], donkey anti-mouse IgG 488 [1:300], donkey anti-rabbit IgG 594 [1:400]) for 1 h with suitable IgG nonspecific IgG antibodies. Remove the unbound secondary antibody using PBST (5 min/wash, 3x).
- Counterstain the nuclei with 5 µg/mL DAPI (4',6-Diamidino-2-Phenylindole ) and seal the slides.
- Perform fluorescence imaging using a fluorescence microscope (Magnification: 400x; Exposure time: 50 ms).
- Quantitative real-time polymerase chain reaction (qPCR)
- Take RNA Isolation Kit to extract the total RNA as per the manufacturer's instructions.
- Use a high-capacity cDNA Transcription Kit to reverse transcribe 1-2 µg of total RNA to cDNA.
- Perform the reverse transcription (42 °C, 2 min; 50 °C , 85 min) and qPCR ( 95 °C, 5 min; 95 °C, 10 s, 40 cycles) in a 20-μL solution containing cDNA (100 ng), TaqMan Gene Expression Assay Mix (1 μL), universal PCR Master Mix (10 μL) and ddH2O (to 20 µL).
- Use the comparative CT technique (ΔΔCT)4,9 to examine the relative gene expression.
3. Characterization of LNC
- Cell counting (hemocytometer)
- Digest the LNCs from the bottom of the plate using 0.25% TE for 5 min in the 37 °C cell incubator.
- Terminate the digestion by adding 1 mL MESCM (containing knockout serum), centrifuge the cell suspension at 200 x g for 5 min, and aspirate the supernatant carefully.
- Add 1 mL MESCM to resuspend the cells, then take 10 μL cell suspension in a 0.5 mL centrifuge tube. Add an equal volume of 0.4% Trypan blue staining solution.
- Place 10 μL stained cell suspension on the counting area of the hemocytometer and cover it with a coverslip for counting.
NOTE: The number of cells in the five middle square areas is defined as "A"; the cell number in 1 mL is calculated as 5A × 104 × 2.
- Examination of LNC and BMMSC markers with flow cytometry15
- Detect the expression of SCF, CD73, CD90, and CD105 in the LNCs and BMMSCs using Flow cytometry15 (2-4 × 106 events/sample, 2,000 cells were obtained from each of the samples, totaling 550,000 cells that were gated simultaneously).
- Collect and stain the cells at 20-30 °C for 15 min in a blocking buffer (3% BSA and 0.05% Tween-20 in PBS) using prelabeled antibodies (SCF [1:50], CD70 [1:50], CD90 [1:50], and CD105 [1:50]) as per the kit instructions.
- Perform fluorescence-activated cell sorting (FACS) analysis using a flow cytometer. In this study, FACS Diva software and FlowJo software were used. For each sample, record 10,000 events and gate and analyze live cells.
Representative Results
Growth of LNC
The LNCs were successfully isolated according to the method of digestion of collagenase A (2 mg/mL) digestion of corneoscleral rim tissue, as described above (Figure 1). Consistent with a previously reported study3, after collagenase A digestion, caterpillar-like clusters were visualized under the microscope (Figure 2). The proportion of spindle cells increased gradually with the cell passage. Spindle-shaped cells could grow on coated 5% basement membrane matrix plates, unlike their counterparts cultivated on plastic without coated basement membrane matrix3. Cells from P1 to P12 exhibited a uniform proliferative rate, with a cell doubling time between 2 and 7 days (Table 2). In this study, LNCs were cultured to the 13 passages, and 34 doublings (Figure 3)3. LNCs were cultured from primary cells (LNC P0); LNC P0 grew slowly and took approximately 12 days. LNCs only needed about 3 days to passage in P1-P8, and the growth rate of LNCs after P9 decreased significantly (Table 2). In terms of cell morphology, LNCs were spindle-shaped, and round in P0. After P3, LNCs were spindle-shaped with the same morphological size (Figure 2). The extent of total expansion was measured as the number of population doubling from P0 to P13 using the following formula: number of cell doubling (NCD) = log10 (y/x) / log102, where y is the final density of cells and x is the initial seeding density of cells3. NCD represents the growth rate of the LNCs (Figure 3A). From the NCD and accumulative-NCD curves (Figure 3B), LNCs took the least time to increase exponentially and grew the fastest from the P3-P5 (Figure 3). After the P5, the cell growth rate decreased significantly, NCD returned to 1.32 in P13, and the growth nearly stopped.
Identification of LNC
After the isolation and culture of LNCs, another important task was identification. LNCs expressed for Vim, CD90, CD105, SCF, and PDGFRβ, but not Pan-CK, according to current relevant studies on LNCs (Figure 4)9. Double immunostaining LNC P4 revealed that these cells were consistently Pan-CK-/Vim+/CD90+/CD105+/SCF+/PDGFR+ (Figure 4). qPCR also revealed decreased Pan-CK expression in the P2 and increased Vim, CD90, CD105, SCF, and PDGFR transcripts in the P3. Transcription levels of Vim, CD90, CD105, SCF, and PDGFR increased dramatically in the P4 compared to the P1 (p < 0.01) (Figure 4)9.
Characteristics of LNC
Further analysis showed that LNCs expressed more embryonic stem cell (ESC) markers (Nestin, Rex1, and SSEA4), mesenchymal stem cell (MSC) markers (CD73, CD90, and CD105), and niche cell (NC) markers (MSX1, P75NTR, and PDGFRβ) (Figure 5)15. Flow cytometry indicated that surface antigen characteristics of MSCs, including CD73, CD90, and CD105, were expressed in both LNCs and BMMSCs15. The percentages of LNCs that expressed CD73, CD90, CD105, and SCF were approximately 95%, 97%, 92%, and 11%, respectively, whereas those of BMMSCs were 68%, 99%, 20%, and 3%, respectively. This shows that LNCs express significantly higher levels of MSC-positive markers CD73, CD105, and the cytokine SCF (p < 0.01) and a similar level of CD90 (p > 0.05) compared to BMMSCs (Figure 6)15.
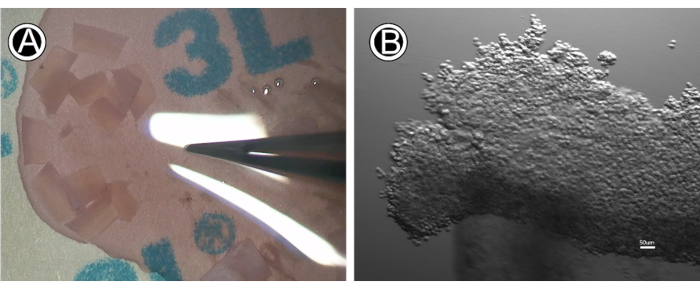
Figure 1: The LNCs isolation process. (A) Corneoscleral rim tissue. (B) Clusters after collagenase A digestion at 37 °C for 18 h. Please click here to view a larger version of this figure.

Figure 2: P0 to P13 LNCs cultured on 5% basement membrane matrix coated 6-well plate in MESCM. (Bar = 50 µm). Please click here to view a larger version of this figure.
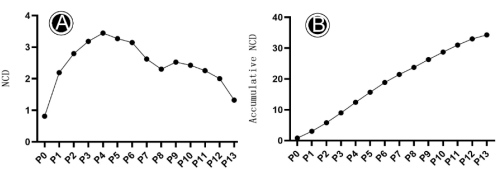
Figure 3: The growth pattern of LNCs from P0-P13. (A) The NCD of LNCs from P0-P13; (B) The cumulative NCD of LNCs from P0-P13. Please click here to view a larger version of this figure.
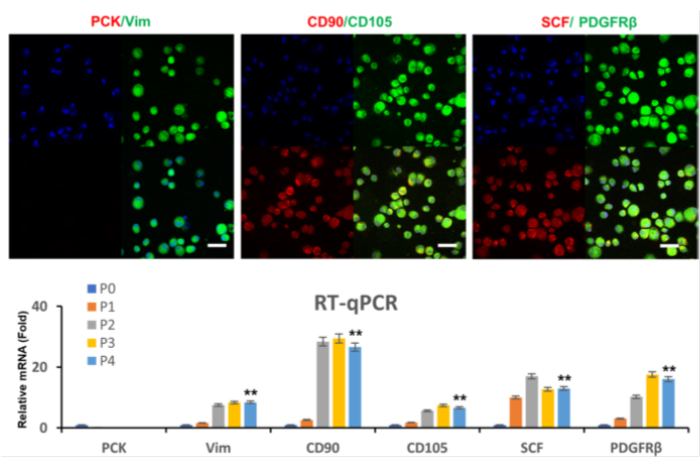
Figure 4: Immunofluorescence and qPCR. Immunofluorescence and qPCR revealed that LNCs uniformly expressed Vim, CD90, CD105, SCF, and PDGFRβ, but not Pan-CK. This figure has been reproduced with permission from Zhu et al.9. Please click here to view a larger version of this figure.
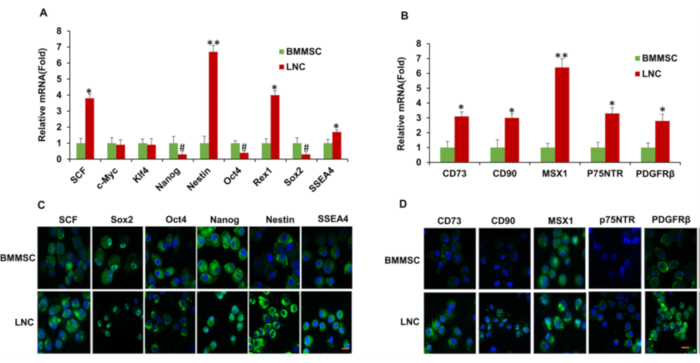
Figure 5: LNCs express more ESC, MSC, and NC markers than BMMSCs. P4 LNCs and P4 BMMSCs were subjected to qPCR for transcription expression of ESC markers (A), MSC and neural crest markers (B) (n = 3, *P < 0.05, #P < 0.05, and **p < 0.01 respectively). Immunostaining of ESC markers (C) and MSC, NC markers (D), with nuclear counterstain by Hoechst 33342. Scale bars = 25 µm. This figure has been reproduced with permission from Li et al.15. Please click here to view a larger version of this figure.
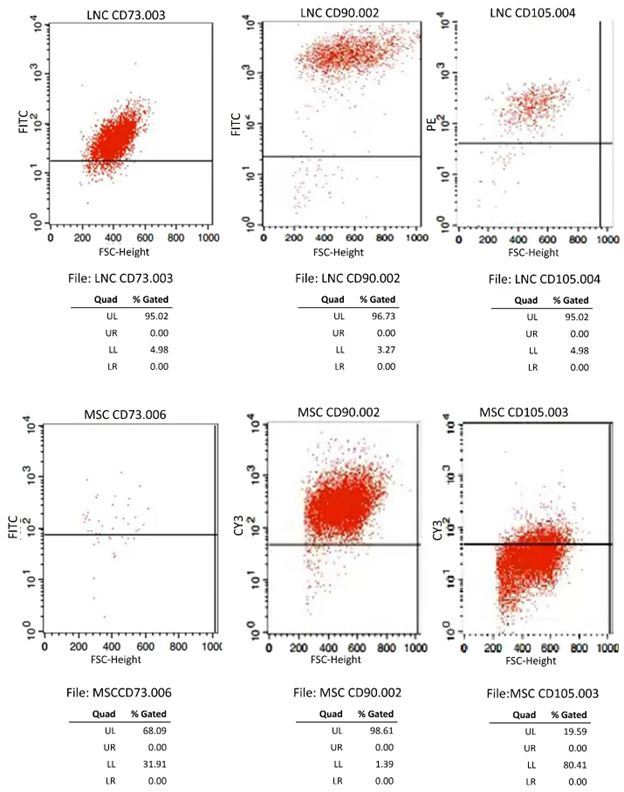
Figure 6: Fluorescence-activated cell sorting of P4 LNCs and BMMSCs (A-F). Fluorescence-activated cell sorting (FACS) analysis of MSC markers including CD73, CD90, and CD105 (n=3). This figure has been reproduced with permission from Li et al.15. Please click here to view a larger version of this figure.
| Reagent | Concentration of stock solution | Volume | Final concentration | Storage Environment |
| DME/F-12 1:1(1×) | Basic medium | 180 mL | 90% | 4 °C |
| KnockOutTMSR | – | 20 mL | 10% | -20 °C |
| Serum Replacement for ESCs/iPSCs | ||||
| Recominant Human Leukemia Inhibitory Factor (Lif) | 50 µg/mL | 40 µL | 10 ng/mL | -80 °C |
| Recombinant Human FGF-basic | 100 µg/mL | 8 µL | 4 ng/mL | -80 °C |
| ITS (insulin, transferrin, sodium selenite) | 500 μg/mL insulin | 2 mL | 5 μg/mL insulin | -20 °C |
| 500 μg/mL transferrin | 5 μg/mL transferrin | |||
| 500 ng/Ml sodium selenite | 5 ng/mL sodium selenite | |||
| Gentamicin | 25 µg/mL | 2 mL | 50 µg/mL | 4 °C |
| Amphotericin B | 2500 µg/mL | 100 µL | 1.25 µg/mL | 4 °C |
Table 1: MESCM formulation.
| Passage | Seeding Density (× 105 cells/cm2) | Final density (× 105cells/cm2) | Culture time (days) | Number of Cell Doublings (NCD) | Accumulative NCD |
| P0 | 0.22 | 0.385714 | 12 | 0.810029 | 0.810029 |
| P1 | 0.08 | 0.365714 | 4 | 2.192645 | 3.002674 |
| P2 | 0.051429 | 0.357143 | 3 | 2.795859 | 5.798533 |
| P3 | 0.037143 | 0.337143 | 2 | 3.182203 | 8.980737 |
| P4 | 0.028571 | 0.311429 | 6 | 3.446256 | 12.42699 |
| P5 | 0.04 | 0.385714 | 3 | 3.269461 | 15.69645 |
| P6 | 0.054286 | 0.48 | 4 | 3.14439 | 18.84084 |
| P7 | 0.057143 | 0.351429 | 3 | 2.620586 | 21.46143 |
| P8 | 0.08 | 0.394286 | 3 | 2.30117 | 23.7626 |
| P9 | 0.06 | 0.345714 | 6 | 2.526546 | 26.28915 |
| P10 | 0.022857 | 0.122857 | 7 | 2.426265 | 28.71541 |
| P11 | 0.025714 | 0.122857 | 5 | 2.25634 | 30.97175 |
| P12 | 0.028571 | 0.114286 | 5 | 2 | 32.97175 |
| P13 | 0.045714 | 0.114286 | 10 | 1.321928 | 34.29368 |
Table 2: Serial Passages of the LNC on plastic.
Discussion
Corneal transparency is typically maintained by regular arrangement and distribution of small fibers (25-30 nm in diameter) in the corneal stroma, which is crucial for normal vision acuity16. There are 253 million visually impaired people worldwide, 36 million of whom are blind17. The world health organization (WHO) considers corneal blindness one of the most serious hazards to human eyesight, accounting for 5.1% of all blindness worldwide16. Corneal epithelium defect with normal CES can heal quickly without leaving a scar18. It is estimated that more than 12.7 million patients worldwide require corneal transplants due to moderate to severe vision loss19; 30% of the cornea transplantation failure was caused by CESD20. However, because of the shortage of cornea donation in most countries worldwide, only one out of seventy cornea-blind patients could eventually receive corneal transplantation21. Currently, corneal epithelial stem cell transplantation (CEST) can be used to treat CESD22. Patients with monocular CESD can obtain CES from healthy eyes for CEST. However, for patients with bilateral CESD, only allogeneic CES can be obtained for treatment. Immune rejection remains the main reason for the failure of allogeneic CEST. A promising method to reduce the therapeutic treatment for CESD is to find a cell that can effectively replace autogenous CES or encourage the differentiation of other autogenous cells from other places to become CES. In vitro differentiation of autologous cells into CES is also becoming popular, including BMMSC23, oral mucosal epithelial cells (OMEC)24, dental pulp stem cells (DPSC)19, human fibroblast-derived-induced pluripotent stem cells (iPSC)25, and adipose stem cells (ASC)26. Rohaina et al.23found that BMMSCs cultured on amniotic membranes for 10 days could differentiate into corneal epithelial cells and that CK3 and p63 expression increased significantly after the induction of differentiation. In 2020, O'Callaghan et al.24induced the differentiation of oral mucosal epithelial cells into corneal epithelial cells using a new culture system, and successfully used it for treating CESD using a 3D tissue structure (RAFT) as a support for oral mucosal epithelial cell culture with human oral mucosal fibroblasts as trophoblasts. Additionally, DPSC differentiates successfully into corneal stromal and epithelial cells. By upregulating the expression of K3, K12, and CD90, DPSC can prevent corneal conjunctival invasion. Another study used DPSC as amniotic cell sheets piggybacked onto the corneal surface in a rabbit CESD model. The results showed that the DPSC group had cleaner corneas and less angiogenesis than the control group27. Hayashi et al.28achieved differentiation using fibroblast-derived iPSC that could be induced in PAX6(+) and K12(+) corneal epithelial cells after 12 weeks. iPSC effectively develops into corneal epithelial cells, activates K12, and suppresses NANOG25. Zeppieri et al.26 discovered that ASCs could differentiate into corneal epithelial cells to cure mouse CESD and enhance corneal epithelial wound healing in a laser-induced animal model.
LNCs localize in the limbal niche, where CES are protected and supported, and have many characteristics similar to MSCs. LNCs were first isolated by Polisetty et al.2 and first named by Xie et al.3. According to recent studies, LNCs are more fundamental stem cells than MSCs and can easily differentiate into adipocytes, chondrocytes, and osteocytes4,29. Compared to the commonly used BMMSCs, LNCs show greater stem cell characteristics (higher expression of CD73, CD105, PDGFR, SCF, etc.) (Figure 5)30. LNCs can successfully treat rabbits with CESD caused by corneal alkali burns by promoting the repair of the corneal epithelium and stroma15. The reduced expression of fibronectin (FN), connective tissue growth factor (CTGF), and secreted protein acidic and cysteine rich (SPARC) in corneal fibroblasts suggest LNCs secretion enhances wound healing and reduces fibrosis7.
In a 3D microenvironment, what is interesting is that LNCs may reunite with MCECs, stimulating the latter cells to restore stem cell properties9. LNCs effectively accelerate CES growth31 and prevents corneal scarring10. However, the quantity of LNCs is limited; studies have indicated it represents only approximately 3% of the total number of limbal stromal cells in the bovine cornea32, with significant expression of keratan sulfate, keratocan, and ALDH3A133. They may be less than 1% in human corneas33.
In this protocol, previous methods of isolating, purifying, and identifying LNCs were repeated3,14,34. After 18 h of treatment of human limbus tissue with collagenase A (2 mg/mL), LNCs were isolated. P0 LNC developed slowly and exhibited various cell morphologies, including spindle-shaped LNCs, polygonal others, and visible spherical MCEC (Figure 2, P0). Previous studies have shown that LNCs are spindle-shaped cells that attach to the bottom of the culture surface with homogeneous morphology14. At the same time, MCECs are round29, which is consistent with the morphology of the cells cultured in this protocol. In addition, P0 LNCs grew slowly to the cells growing full approximately 70%-80% of cell density in approximately 12 days. P1-P12 LNC proliferated substantially faster and, in 3-6 days, practically covered the entire culture plate. Following P1, spindle-shaped LNCs adnexal cells significantly outnumbered round MCEC and polygonal cells.
It is clear from the NCD values in Table 2 and Figure 3 that the LNCs P0 had the lowest NCD (0.810) and that cell passage occurred over 12 days. However, after the P1, the growth of LNCs accelerated dramatically, and the growth rate peaked at 3.44 in the P4. After the P6, the growth rate of the LNCs were substantially reduced (Figure 3). The LNCs growth rate and activity of the P4 were substantially the highest in terms of the LNCs growth pattern, consistent with earlier findings indicating that the P4-P6 LNCs growth activity is the best9. However, this method has certain limitations, the number of LNC P0 varies greatly according to the donor's age and the time of death. Therefore, when the donor tissue is younger and fresher, more P0 LNC can be isolated. The most important factor in mimicking the microenvironment of CES in vitro is the need for universal niche factors, such as a laminamine-rich extracellular matrix35.
In conclusion, LNCs play a crucial role in supporting corneal epithelial stem cells and maintaining the stemness of CES, including self-renewal and differentiation into mature cornea epithelial cells. LNC could be expected to be an innovative cell tool for treating patients with CESD9,15.
Disclosures
The authors have nothing to disclose.
Acknowledgements
Thanks to Wei Wang, Lingjuan Xu, and Rong Liu for the guidance on this work, Yongyao Tan, Bihui Jin, Chunxiu You, and Li Guigang for providing some of the material, Guanyu Su for writing the manuscript, Xiao Zhou, Yihong Xiong, and Huatao Xie for correcting the manuscript, and Guigang Li for his full guidance. This study was supported by the National Natural Science Foundation of China (No. 82070936, 81470606, 81570819), Hubei Province health and family planning scientific research project (No. WJ2017M073), Top Ten Translational Medical Research Projects from Tongji Hospital (No.2016ZHYX20), Training Project of Young medical Pioneers in Wuhan City (No.2015whzqnyxggrc10), Global Talents Recruitment Program (G2022154028L), National Health Commission of Hubei Province project In 2022(WJ2021ZH0005), and Subject Construction Foundation of Finance Department of Hubei In 2022(42000022815T000000102)
Materials
| 4',6-Diamidino-2-Phenylindole | ThermoFisher | D1306 | 5μg/mL |
| Amphotericin B | Sigma | V900919 | 1.25 μg/mL |
| Anti-CD73 | Abcam | ab202122 | 1:50 |
| Bovine Serum Albumin | MERCK | A1933 | – |
| CD105 | Proteintech | 67075-1-Ig | 1:200 |
| CD105 | Abcam | ab114052 | 1:50 |
| CD90 | Proteintech | 66766-1-Ig | 1:100 |
| CD90 | Abcam | ab307736 | 1:50 |
| Cell Incubator | Shanghai Lishen | K1119K4644 | HF90(HT) |
| Centrifuge system | StatSpin | StatSpin CytoFuge 12 | – |
| Collagenase A | Roche | 10103578001 | 2 mg/mL |
| Confocal microscope | Zeiss | LSM700 | – |
| Culture plate | virya | 3500356 | 35 mm |
| DME/F-12 1:1 (1x) | cytiva | SH30023.01 | 90% |
| Donkey anti-Mouse IgG (H+L) Secondary Antibody | ThermoFisher | A16016 | 1:1000 |
| Donkey anti-rabbit IgG (H+L) Secondary Antibody | ThermoFisher | 31568 | 1:1000 |
| FACS Diva sofware | BD Biosciences | Tree Star | – |
| Flow Cytometer | BD Biosciences | Becton Dickinson LSRII | – |
| Fluorescence microscope | olympus | cx31 | |
| Gentamicin | Sigma | G1914 | 50 μg/mL |
| Hemocytometer | MERCK | Z359629 | Bright-Line |
| High-capacity cDNA Transcription Kit | ThermoFisher | 4374966 | |
| Inverted phase-contrast microscope | UOP | DSZ2000X | |
| ITS (insulin, transferrin, sodium selenite) | Sigma | I3146 | 5 μg/mL insulin, 5 μg/mL transferrin, 5 ng/mL sodium selenite |
| KnockOut SR Serum Replacement for ESCs/iPSCs | gibco | 10828-028 | 10% |
| Matrigel | BioCoat | 356234 | – |
| Pan-CK | Abcam | ab7753 | 1:1000 |
| Paraformaldehyde | NoninBio | NBS0135 | 4.00% |
| Paraformaldehyde | MKBio | MM-1505 | 4% |
| PDGFRβ | Abclonal | A1444 | 1:100 |
| Real-time fluorescence quantitative PCR instrument | Applied Biosystems | Step One Plus | – |
| Recombinant Human FGF-basic | Peprotech | 100-18B | 4 ng/mL |
| Recominant Human Leukemia Inhibitory Factor(Lif) | Peprotech | 300-05 | 10 ng/mL |
| RNeasy Mini RNA Isolation Kit | Qiagen | 74104 | – |
| SCF | Bioss | bs-0545R | 1:100 |
| SCF | Abcam | ab52603 | 1:50 |
| Stereomicroscope | ZEISS | SteREO Discovery. V8 | |
| Sterile surgical round blade | Careforde | 29500 | size 10 |
| TaqMan Gene Expression Assay Mix | Applied Biosystems | 4448489 | |
| Triton X-100 | MERCK | X100 | 0.20% |
| Trypan blue | ThermoFisher | 15250061 | 0.40% |
| Trypsin-EDTA | Genview | GP3108 | 0.25% |
| Tween 20 | MERCK | P9416 | – |
| Ultra Clean Bench | LaiTe | LT20200705 | SW-CJ-IFDG |
| Universal PCR Master Mix | Applied Biosystems | 4304437 | |
| Vim | Abcam | ab92547 | 1:100 |
References
- Le, Q., Xu, J., Deng, S. X. The diagnosis of limbal stem cell deficiency. Ocular Surface. 16 (1), 58-69 (2018).
- Polisetty, N., Fatima, A., Madhira, S. L., Sangwan, V. S., Vemuganti, G. K. Mesenchymal cells from limbal stroma of human eye. Molecular Vision. 14, 431-442 (2008).
- Xie, H. T., Chen, S. Y., Li, G. G., Tseng, S. C. Isolation and expansion of human limbal stromal niche cells. Investigative Ophthalmology & Visual Science. 53 (1), 279-286 (2012).
- Li, G. G., Zhu, Y. T., Xie, H. T., Chen, S. Y., Tseng, S. C. Mesenchymal stem cells derived from human limbal niche cells. Investigative Ophthalmology & Visual Science. 53 (9), 5686-5697 (2012).
- Li, G. G., Chen, S. Y., Xie, H. T., Zhu, Y. T., Tseng, S. C. Angiogenesis potential of human limbal stromal niche cells. Investigative Ophthalmology & Visual Science. 53 (7), 3357-3367 (2012).
- Hu, W., Zhang, Y., Tighe, S., Zhu, Y. T., Li, G. G. A new isolation method of human lacrimal canaliculus epithelial stem cells by maintaining close association with their niche cells. International Journal of Medical Sciences. 15 (12), 1260-1267 (2018).
- Kumar, A., Xu, Y., Yang, E., Du, Y. Stemness and regenerative potential of corneal stromal stem cells and their secretome after long-term storage: Implications for ocular regeneration. Investigative Ophthalmology & Visual Science. 59 (8), 3728-3738 (2018).
- Xiao, Y. T., Qu, J. Y., Xie, H. T., Zhang, M. C., Zhao, X. Y. A comparison of methods for isolation of limbal niche cells: Maintenance of limbal epithelial stem/progenitor cells. Investigative Ophthalmology & Visual Science. 61 (14), 16 (2020).
- Zhu, H., et al. Limbal niche cells and three-dimensional matrigel-induced dedifferentiation of mature corneal epithelial cells. Investigative Ophthalmology & Visual Science. 63 (5), 1 (2022).
- Basu, S., et al. Human limbal biopsy-derived stromal stem cells prevent corneal scarring. Science Translational Medicine. 6 (266), 266ra172 (2014).
- Acar, U., et al. Effect of allogeneic limbal mesenchymal stem cell therapy in corneal healing: role of administration route. Ophthalmic Research. 53 (2), 82-89 (2015).
- Katikireddy, K. R., Dana, R., Jurkunas, U. V. Differentiation potential of limbal fibroblasts and bone marrow mesenchymal stem cells to corneal epithelial cells. Stem Cells. 32 (3), 717-729 (2014).
- Polisetti, N., Sharaf, L., Reinhard, T., Schlunck, G. Isolation and ex vivo expansion of limbal mesenchymal stromal cells. Bio-Protocols. 12 (14), e4471 (2022).
- Xie, H. T., Chen, S. Y., Li, G. G., Tseng, S. C. Limbal epithelial stem/progenitor cells attract stromal niche cells by SDF-1/CXCR4 signaling to prevent differentiation. Stem Cells. 29 (11), 1874-1885 (2011).
- Li, G., et al. Human limbal niche cells are a powerful regenerative source for the prevention of limbal stem cell deficiency in a rabbit model. Scientific Reports. 8, 6566 (2018).
- Kumar, A., Yun, H., Funderburgh, M. L., Du, Y. Regenerative therapy for the cornea. Progress In Retinal and Eye Research. 87, 101011 (2022).
- Pineda, R. . World Corneal Blindness. Foundations of Corneal Disease. , 299-305 (2020).
- Zieske, J. D., Guimarães, S. R., Hutcheon, A. E. Kinetics of keratocyte proliferation in response to epithelial debridement. Experimental Eye Research. 72 (1), 33-39 (2001).
- Resnikoff, S., et al. Global data on visual impairment in the year 2002. Bulletin of the World Health Organization. 82 (11), 844-851 (2004).
- Tan, Y., et al. Limbal bio-engineered tissue employing 3D nanofiber-aerogel scaffold to facilitate LSCs growth and migration. Macromolecular Bioscience. 22 (5), e2100441 (2022).
- Aghamirsalim, M., et al. 3D printed hydrogels for ocular wound healing. Biomedicines. 10 (7), 1562 (2022).
- Sasamoto, Y., Ksander, B. R., Frank, M. H., Frank, N. Y. Repairing the corneal epithelium using limbal stem cells or alternative cell-based therapies. Expert Opinion on Biological Therapy. 18 (5), 505-513 (2018).
- Rohaina, C. M., et al. Reconstruction of limbal stem cell deficient corneal surface with induced human bone marrow mesenchymal stem cells on amniotic membrane. Translational Research. 163 (3), 200-210 (2014).
- O’Callaghan, A. R., Dziasko, M. A., Sheth-Shah, R., Lewis, M. P., Daniels, J. T. J. A. B. Oral mucosa tissue equivalents for the treatment of limbal stem cell deficiency. Advanced Biosystems. 4 (7), e1900265 (2020).
- Yu, D., Chen, M., Sun, X., Ge, J. Differentiation of mouse induced pluripotent stem cells into corneal epithelial-like cells. Cell Biology International. 37 (1), 87-94 (2013).
- Zeppieri, M., et al. Adipose-derived stem cells for corneal wound healing after laser-induced corneal lesions in mice. Journal of Clinical Medicine. 6 (12), 115 (2017).
- Kumar, A., Kumar, V., Rattan, V., Jha, V., Bhattacharyya, S. Secretome cues modulate the neurogenic potential of bone marrow and dental stem cells. Molecular Neurobiology. 54 (6), 4672-4682 (2017).
- Hayashi, R., et al. Coordinated generation of multiple ocular-like cell lineages and fabrication of functional corneal epithelial cell sheets from human iPS cells. Nature Protocols. 12 (4), 683-696 (2017).
- Guo, P., et al. Limbal niche cells are a potent resource of adult mesenchymal progenitors. Journal of Cellular and Molecular Medicine. 22 (7), 3315-3322 (2018).
- Wang, W., et al. Differential gene expression between limbal niche progenitors and bone marrow derived mesenchymal stem cells. International Journal of Medical Sciences. 17 (4), 549-557 (2020).
- González, S., Deng, S. X. Presence of native limbal stromal cells increases the expansion efficiency of limbal stem/progenitor cells in culture. Experimental Eye Research. 116, 169-176 (2013).
- Funderburgh, M. L., Du, Y., Mann, M. M., SundarRaj, N., Funderburgh, J. L. PAX6 expression identifies progenitor cells for corneal keratocytes. FASEB Journal. 19 (10), 1371-1373 (2005).
- Funderburgh, J. L., Funderburgh, M. L., Du, Y. Stem cells in the limbal stroma. Ocular Surface. 14 (2), 113-120 (2016).
- Chen, S. Y., Hayashida, Y., Chen, M. Y., Xie, H. T., Tseng, S. C. A new isolation method of human limbal progenitor cells by maintaining close association with their niche cells. Tissue Engineering. Part C, Methods. 17 (5), 537-548 (2011).
- Sato, T., Clevers, H. SnapShot: Growing organoids from stem cells. Cell. 161 (7), 1700-1701 (2015).

